Obstetrics and Gynaecology Cases - Reviews
Cyst of Canal of Nuck: Our Experience
Juan Piazze1,5*, Ettore Palma2, Francesco Recchia3,5, Valerio D'Orazi4, Daniela Romanzi5, Michele Rosselli5,7, Massimo Bratta5,8 and Silvio Rea5,6
1ASL Frosinone (Poliambulatorio di Ceprano-Ospedale SS Trinità di Sora), Fondazione Carlo Ferri, Monterotondo, Rome, Italy
2Department of Gynecological Obstetrics and Urologic Sciences, Sapienza University, Rome, Italy
3Ospedale Civile di Avezzano, Fondazione Carlo Ferri, Monterotondo, Rome, Italy
4Department of General Microsurgery and Hand Surgery, Fabia Mater Hospital, Rome, Italy
5Fondazione Carlo Ferri, Monterotondo, Rome, Italy
6Chirurgia Oncologica, Università degli Studi de L'Aquila, Fondazione Carlo Ferri, Monterotondo, Rome, Italy
7Unità operativa di Oncologia , Ospedale Civile di Frascati, Rome, Italy
8Ospedale Civile di Rieti, Rome, Italy
*Corresponding author: Dr. Juan Piazze, ASL Frosinone (Poliambulatorio di Ceprano-Ospedale SS Trinità di Sora), Fondazione Carlo Ferri, Monterotondo, Rome, E-mail: cloudpia@me.com
Obstet Gynecol Cases Rev, OGCR-3-097, (Volume 3, Issue 5), Case Series; ISSN: 2377-9004
Received: March 21, 2016 | Accepted: September 21, 2016 | Published: October 01, 2016
Citation: Piazze J, Palma E, Recchia F, D'Orazi V, Romanzi D, et al. (2016) Cyst of Canal of Nuck: Our Experience. Obstet Gynecol Cases Rev 3:097. 10.23937/2377-9004/1410097
Copyright: © 2016 Piazze J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report two cases of a cyst of the canal of Nuck in which sonography showed a tubular cystic structure characterized by internal septum localized within the inguinal canal. Unfortunately, Magnetic resonance (MRI) examination was not performed in the first case, however in the second case, MRI demonstrated that the mass suggested an hydrocele of the Canal of Nuck. Both cases were solved satisfactorily and confirmed cysts of canal of Nuck by means of laparoscopic technique.
Keywords
Canal of Nuck, Hydrocele, Magnetic resonance, Ultrasound
Introduction
Hydrocele of the canal Nuck is a rare cause of inguinal swelling in women, and it occurs due to a patent processus vaginalis. Ultrasound and MRI findings are described to be useful linked to a good anamnesis in patients with suspected inguinal hernia [1,2].
In women, a round ligament is attached to the uterus close to the origin of the fallopian tubes, and the extension of the parietal peritoneum follows the round ligament as it passes to the inguinal canal through the internal ring. The processus vaginalis in the female fetus usually closes and disappears long before birth. Evagination of the parietal peritoneum along with the round ligament of the uterus through the inguinal ring into the inguinal canal forms the canal of Nuck. Although complete obliteration of the canal of Nuck usually occurs, partial patency with peritoneal communication, allowing only fluid collection, can result in a hydrocele of the canal of Nuck. The hydrocele may present as a painless and elastic soft swelling in the inguinal region and labium majus. If the hydrocele of the canal of Nuck communicates into the peritoneal space, it often mimics an inguinal hernia in female patients because of its changeable mass. We present two cases that solved satisfactorily by means of laparoscopic totally extraperitoneal (TEP) approach.
Cases
Case 1
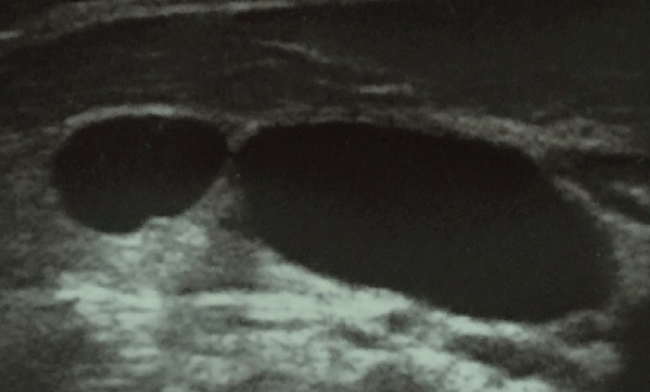
A 45-year-old woman was referred to our department for a suspicious left sliding inguinal hernia evident only two months before. There was no history of abdominal pain or bowel dysfunction. The palpable mass could be repositioned manually. She showed a simple cystic left inguinal hypoechogenic lesion as evaluated by inguinal high resolution ultrasound by means of a linear probe, with net margins and with hyperechogenic linear tracts, negative to color Doppler signals (Figure 1). Transvaginal examination did not show any ultrasound detected alteration. Unfortunately MRI was not performed since after our consult she was evaluated by a general surgeon who decided for immediate intervention for a suspected inguinal hernia that was performed in laparoscopy. She presented to our Institution three months after intervention for control examination. She referred to have been operated under laparacoscopic TEP Inguinal Hernia repair, to be in good clinical conditions and that from histological examination of the lesion, the suspected inguinal hernia turned into a hydrocele of the canal of Nuck.
Case 2
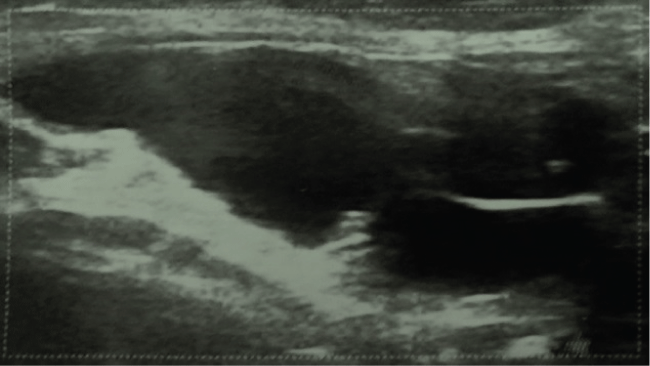
A 38-year-old woman presented to our Institution for a suspicious right sliding inguinal hernia. She had complained of reducible swelling in her right groin for about three years. She noticed a slight increase in the size of the swelling after childbirth. There was no history of abdominal pain or bowel dysfunction. The palpable mass could be repositioned manually and became clinically evident only three months before our clinical examination. Ultrasonographic examination by linear probe revealed the mass to be hypoechoic and homogeneous without solid components. Color Doppler was negative and it measured 13 × 36 mm at inguinal ultrasound. The lesion appeared to be in contact with the right ovary connected at its base with the parietal peritoneum as detected by successive transvaginal examination (Figure 2 and Figure 3). MRI showed Sagittal T2-weighted MR image linked to a fluid-intensity tumor led to the inguinal canal. Enhanced T2-weighted MRI revealed no solid component within the cystic tumor in contact with the ovary.
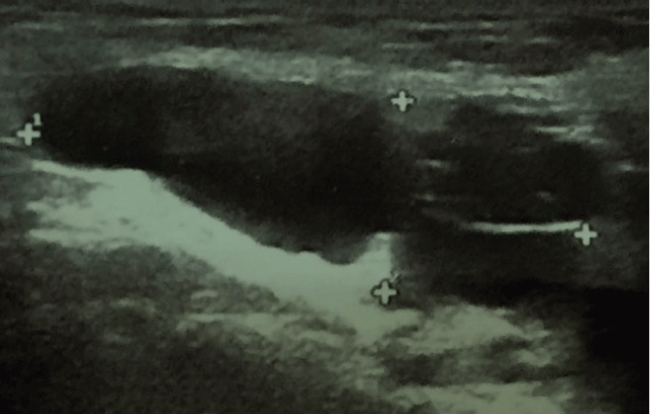
.
Figure 3 Dimension reported in right inguinal canal lesion in patient 2 (13 × 36 mm).
View Figure 3
We suggested laparoscopic TEP excision of the hydrocele and repair of the inguinal hernia [3]. Pathological findings revealed that the resected wall of the hydrocele was lined with a single layer of mesothelial cells and consisted of fibrous components without solid components. The patient was discharged uneventfully on the 3rd postoperative day.
The surgical interventions were performed at the "Fabia Mater Hospital", for diagnosis we used a high resolution ultrasound machine (Esaote MyLab 70 XVision, Italy) by means of a variable band linear and endocavitary probes (5-11 Mhz); the MRI apparatus was an Ingenia 3.0 T (The Netherlands). Histological techniques included ultramicrotome section and acid/basic automatic sample colorant treatment.
Discussion
Hydrocele of the canal of Nuck is an unusual diagnosis. In the literature, only a few cases of cysts of the canal of Nuck are described as internal incomplete septae within a cyst demonstrated by ultrasonography and MRI [2-4]. It seems remarkable that most of the cases reported in the literature were diagnosed at surgery performed for suspicious inguinal hernia. It was reported that high-resolution sonography can identify the nature of groin [3,5-7]. The recommended treatment is excision of the hydrocele and closure of the enlarged inguinal ring [8]. This is usually performed through the inguinal canal by an anterior approach. In the present case, the laparoscopic approach was useful for diagnosis and treatment.
If swelling in the inguinal region and labium majus is recognized in the adult female, fine-needle aspiration can be helpful to assist in making an accurate diagnosis. Normally this peritoneal evagination undergoes obliteration soon after birth in both sexes. Clinically a cyst of the canal of Nuck appears as a fluctuant irreducible mass causing mild pain or a painless lump in the inguinal region. In one third of patients an associated inguinal hernia is present, so diagnosis can be difficult [9]. A cyst of the canal of Nuck is different from an inguinal hernia sac as there is no omental and intestinal contents within the cystic mass. The differential diagnosis list includes also enlarged lymph nodes and soft tissue tumors (e.g. lipomas, leiomyomas and endometriosis of the round ligament). Sonography is an easily applied and highly accurate imaging modality. A tubular or oval anechoic lesion in the inguinal area or labium majus is observed. Differential diagnosis with abcess or solid mass is mainly suggested by manual evaluation, patient's conditions and high temperature.
In both cases described, basically the patients arrived to our evaluation with a palpable mass that could be repositioned manually, no excessive pain. They showed a simple cystic inguinal hypoechogenic lesion as evaluated by inguinal high resolution ultrasound by means of a linear probe, with net margins and with hyperechogenic linear tracts, negative to color Doppler signals; transvaginal examination suggested a connection with a homolateral adnexial involvement in the second case, while the first patient presented an apparent normal transvaginal examination.
The value of MRI is extremely helpful in this condition, representing the demonstration of an abdominal connection of the simple inguinal cyst, with classical hypointense on T1-weighted images and hyperintense on T2-weighted images. Use of the TEP approach can provide surgeons with information on the origin and type of hydrocele of the canal of Nuck [4,8,9]. Furthermore, an incision of the peritoneum for excision of hydrocele, which would avoid the bowel adhesion, is not necessary.
Conclusion
Ultrasonography and MR are the imaging modalities of choice for evaluating a cyst of the canal of Nuck. Laparoscopic totally extraperitoneal technique solves satisfactorily the inguinal swelling.
References
-
Jagdale R, Agrawal S, Chhabra S, Jewan SY (2012) Hydrocele of the canal of Nuck: value of radiological diagnosis. J Radiol Case Rep 6: 18-22.
-
Yigit H, Tuncbilek I, Fitoz S, Yigit N, Kosar U, et al. (2006) Cyst of the canal of Nuck with demonstration of the proximal canal: the role of the compression technique in sonographic diagnosis. J Ultrasound Med 25: 123-125.
-
Bunting D, Szczebiot L, Cota A (2013) Laparoscopic hernia repair--when is a hernia not a hernia? JSLS 17: 654-656.
-
Ozel A, Kirdar O, Halefoglu AM, Erturk SM, Karpat Z, et al. (2009) Cysts of the canal of Nuck: ultrasound and magnetic resonance imaging findings. J Ultrasound 12: 125-127.
-
Safak AA, Erdogmus B, Yazici B, Gokgoz AT (2007) Hydrocele of the canal of Nuck: sonographic and MRI appearances. J Clin Ultrasound 35: 531-532.
-
Shadbolt CL, Heinze SB, Dietrich RB (2001) Imaging of groin masses: inguinal anatomy and pathologic conditions revisited. Radiographics 21: S261-271.
-
Gaeta M, Minutoli F, Mileto A, Racchiusa S, Donato R, et al. (2010) Nuck canal endometriosis: MR imaging findings and clinical features. Abdom Imaging 35: 737-741.
-
Yen CF, Wang CJ, Lin SL, Chang PC, Lee CL, et al. (2001) Laparoscopic closure of patent canal of Nuck for female indirect inguinal hernia. J Am Assoc Gynecol Laparosc 8: 143-146.
-
Huang CS, Luo CC, Chao HC, Chu SM, Yu YJ, et al. (2003) The presentation of asymptomatic palpable movable mass in female inguinal hernia. Eur J Pediatr 162: 493-495.