Obstetrics and Gynaecology Cases - Reviews
The Anesthetic Approach for a 27-Week Pregnant Woman Undergoing Endoscopic Sinus Surgery
Nilay Boztas*, Sevda Ozkardesler, Mert Akan and Mine Sari
Department of Anesthesiology and Reanimation, Dokuz Eylul University, Turkey
*Corresponding author: Nilay Boztas, MD, Medical Faculty, Department of Anesthesiology and Reanimation, Dokuz Eylul University, Izmir, Turkey, Tel: +90 505 2242752, Fax: +90 232 4122846, E-mail: nilayboztas@hotmail.com
Obstet Gynecol Cases Rev, OGCR-3-095, (Volume 3, Issue 5), Case Report; ISSN: 2377-9004
Received: June 21, 2016 | Accepted: August 29, 2016 | Published: September 02, 2016
Citation: Boztas N, Ozkardesler S, Akan M, Sari M (2016) The Anesthetic Approach for a 27-Week Pregnant Woman Undergoing Endoscopic Sinus Surgery. Obstet Gynecol Cases Rev 3:095. 10.23937/2377-9004/1410095
Copyright: © 2016 Boztas N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In pregnancy non-obstetric surgery involves many significant difficulties for the anesthetist. The majority of these procedures are non-elective and some are life-threatening. This report explains the preoperative preparation and general anesthetic method for a 27-week pregnant woman with osteofibrotic mass narrowing the left optic canal causing rapidly advancing loss of vision.
Introduction
In developed countries, the incidence of non-obstetric surgery during pregnancy is about 1-2% [1]. The most common reasons for surgery in pregnancy are appendicitis, cholecystitis, ovarian torsion, trauma and maternal malignant pathologies. Studies have reported that of non-obstetric surgeries during pregnancy, 42% are in the first trimester, 35% are in the second trimester and 23% are in the third trimester [2].
This case report presents the anesthetic approach for a 27-week pregnant woman undergoing endoscopic sinus surgery for complaint of rapidly advancing loss of vision due to left optic mass. We aimed to recall the anesthetic methods for non-obstetric surgery on the basis of this case.
Case Report
A 27-week pregnant, 22-year old female, 65 kg weight, 1.60 cm height, and body mass index (BMI): 25 with physical situation American Society of Anesthesiologists (ASA) IIE. About two years previously a biopsy was taken from a mass in the left optic canal and osteofibrotic lesion was diagnosed. The complaints were headache, orbital and retro-orbital pain of two years ago to perform a biopsy. The patient applied with loss of vision in the left eye for 1-2 weeks and complaint of headache. Due to the mass narrowing the optic canal on the left side and causing advancing loss of vision, semi-emergency endoscopic sinus surgery was planned by the Ear, Nose, and Throat (ENT) department (Figure 1). In order to share our experience of this situation as a scientific article, the required consent was obtained from the patient.
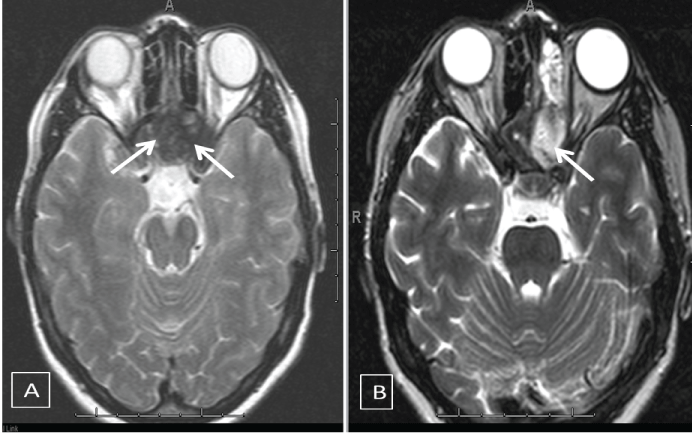
.
Figure 1A: T1-weighted axial MR image revealing low signal lesions both sites that fill the back ethmoid and sphenoid sinuses (arrows);
B: T1-weighted axial postoperative MR image revealing lesion was resected and monitored the cavity is filled with liquid (arrow).
View Figure 1
Preanesthetic assessment found; clear consciousness, cooperative, oriented patient with no pathology found on cardiovascular and respiratory system examination. Airway evaluation determined mallampati score of 1. Preoperative tests: Hb 11.1, Htc 33.6, WBC 12,200, Na+ 139, K+ 4.1, glucose 80, Cr 0.5, sedimentation 52, ECG and coagulation test normal. Due to the possibility of premature birth, before surgery 2 doses of Betamethasone intravenous (iv) were administered at 12 hour intervals to ensure maturation of the baby's lungs and then 48 hours waiting was allowed. For thromboembolism prophylaxis, a single dose of 0.4 mL subcutan (sc) enoxaparin was administered the night before surgery. One hour before surgery, iv ranitidine was administered.
The patient was monitored with ECG DII lead and pulse oxymetry, noninvasive and invasive blood pressure, capnography, urine and axillary temperature with two venal (18 Gauge, 20 Gauge) and left radial artery cannula (20 Gauge) inserted. To reduce aorto-caval pressure, and to shift the uterus to the left, a pillow was placed under the right hip. With a mask, 100% oxygen (O2) was administered for 3 min for preoxygenation, 6 mg/kg iv thiopental was titrated and after loss of consciousness the Sellick Maneuver was applied. After intravenous 1 mg/kg rocuronium, 60 s waiting ensued and then the patient was intubated with number 7 cuff endotracheal tube. For prophylaxis 1 g iv cefazolin was administered. Anesthesia maintenance was ensured with 50% O2/air, 1.5% sevoflurane and 1 μg/kg/hr fentanyl infusion. Mechanical ventilation was applied in volume control mode with 30-35 mmHg ETCO2. During the operation no additional neuromuscular blocker was administered. In the operating room, an obstetrician monitored cardiotocography and continuous fetal heart rate (FHR). In the preoperative period FHR was 150/min, while during surgery FHR was 135/min. Arterial blood gas analysis was within normal physiological limits. The surgery lasted two hours, during the operation the patient's hemodynamics were stable and 1000 mL isotonic and 500 mL isolate-S was administered. Total urine output was above 2 ml/kg. Intraoperative blood sugar was 94 mg/dL. At the end of surgery the patient was fully conscious, placed in lateral position and moved to the recovery unit. With stable hemodynamics the patient was monitored for two hours and then sent to the ward. On the postoperative first day, the patient was observed to be stable in the ward. Preoperative vision degree was 2/10 which improved to 7/10 on the postoperative second day. With all complaints resolving, the patient was discharged on the 3rd day postoperative.
Discussion
The primary aim of emergency surgery is to protect the life of the mother [3]. The decision for surgery should be made by the anesthetist, surgeon and obstetrician together.
During surgery due to the possibility of emergency cesarean, iv steroids were administered 48 hours before surgery for development of the fetus' lungs. Reduction in venous return to the heart from the growing uterus causes edema in lower extremities and increased risk of thromboembolism. The incidence of thromboembolic complications is 5 times increased in pregnancy so prophylaxis is required [2]. For thromboembolism prophylaxis our case was administered sc 0.4 mL enoxaparin the night before surgery.
During preanesthetic assessment, consultation with obstetric and neonatal units should be requested before surgery. Gestational age should be estimated, the probabilities of miscarriage or premature birth should be calculated and these possibilities discussed with the patient. For premedication, aspiration prophylaxis (ranitidine, metaclopramide) should be administered from the beginning of the second trimester.
From the 2nd trimester on, especially, lower esophageal sphincter pressure reduces linked to progesterone and intra abdominal pressure increases [4]. As a result rapid serial induction should be administered. NSAI (non-steroid antiinflamatuar) medications should be avoided as early closure of the ductus arteriosus may occur. Many studies have reported that surgery in pregnancy does not cause an increase in incidence of congenital anomalies; however the risk of abortus, low birth weight and premature birth are high [3].
From the 6-7th week of pregnancy, cardiac, hemodynamic, respiratory and metabolic alterations are observed. In pregnancy the per minute ventilation and oxygen consumption (20%) increase, while oxygen reserves reduce Functional residual capacity (FRC) and Residual Volume (RV) reduce and linked to this more rapid desaturation is observed. Due to the stimulating effect of progesterone on respiration, hyperventilation and mild respiratory alkalosis are observed. During surgery, Partial arterial carbon dioxyde pressure (PaCO2) should be kept within normal limits. The increase in soft tissue mass in the neck and laryngeal edema may cause difficulty with ventilation and intubation. As a result a smaller diameter tracheal tube should be used. Difficult intubation equipment should be ready and waiting [2]. With normal airway examination, no difficulty was experienced during intubation of our case.
Though there is no optimal anesthetic technique for non-obstetric surgery in pregnancy, as the maternal airway should be protected and exposure of the fetus to general anesthesia medications prevented, regional anesthesia should be chosen. Of anesthetic agents propofol, barbiturate, opioids, neuromuscular blockers and local anesthetics are said to be reliable. At clinical concentrations, they are not teratogenic [2]. The sensitivity to volatile agents is increased in pregnancy, so Minimum Alveolar Concentration (MAC) values should be 30% lower. Since the introduction of sugammadex it is an alternative to the use of rocuronium [4]. In animal studies N2O was reported to be teratogenic [5]. At low dose, thiopental is the most common agent used for rapid serial induction in pregnancy [6]. Propofol is becoming increasingly popular in use and is not teratogenous in animal experiments [7].
Lengthened maternal hypoxia may reduce uteroplacental vasoconstriction and uteroplacental perfusion causing fetal hypoxemia, acidosis and death [8].
Maternal fluid volume and blood pressure have critical importance [3]. Plasma volume and cardiac output increase 40-50%, with htc reducing 20% linked to dilution. Blood pressure may fall secondary to vasodilatation developing linked to progesterone. Aortocaval compression is generally a major danger from the 20th week, suppressing uterine blood flow and causing supine hypotension syndrome [2]. To prevent this situation during surgery the lateral position should be used. We placed a pillow under the right hip of our patient aiming to reduce aortocaval pressure. Maintenance of maternal and uteroplacental (fetal) perfusion is directly linked to maternal systemic arterial pressure; both cardiac output and systemic vascular resistance should be protected. In our case to ensure sufficient placental perfusion, systolic blood pressure was kept above 100 mmHg.
During surgery the patient was warmed with a Bair-Hugger and body temperature was held at around 36.5°C. During surgery fetal heart rate (from 24-26 weeks) should be routinely monitored by an obstetrician. A reduction in FHR may be related more too fetal hypoxemia and acidosis [9]. In our case during surgery FHR was monitored by an obstetrician and no pathology was observed.
Conclusion
In this case we aimed to present the anesthetic management of a 27-week pregnant woman undergoing endoscopic sinus surgery for left optic mass causing rapidly advancing vision loss. These types of cases require a multidisciplinary approach involving anesthetist, surgeon and obstetrician and need complex perioperative anesthesia management.
References
-
Crowhurst JA (2002) Anaesthesia for non obstetric surgery during pregnancy. Acta Anaesthesiol Belg 53: 295-297.
-
Reitman E, Flood P (2011) Anaesthetic considerations for non-obstetric surgery during pregnancy. Br J Anaesth 107: i72-78.
-
Walton NKD, Melachuri KV (2006) Anaesthesia for non-obstetric surgery during pregnancy. Critical care & pain 6: 83-85.
-
Nejdlova M, Johnson T (2012) Anaesthesia for non-obstetric procedures during pregnancy. Critical care & pain 12: 203-206.
-
Fujinaga M, Baden JM (1994) Methionine prevents nitrous oxide-induced teratogenicity in rat embryos grown in culture. Anesthesiology 81: 184-189.
-
Gin T, Mainland P, Chan MT, Short TG (1997) Decreased thiopental requirements in early pregnancy. Anesthesiology 86: 73-78.
-
Higuchi H, Adachi Y, Arimura S, Kanno M, Satoh T (2001) Early pregnancy does not reduce the C50 of propofol for loss of consciousness. Anesth Analg 93: 1565-1569.
-
Dilts PV Jr, Brinkman CR 3rd, Kirschbaum TH, Assali NS (1969) Uterine and systemic hemodynamic interrelationships and their response to hypoxia. Am J Obstet Gynecol 103: 138-157.
-
Kuczkowski KM (2004) Nonobstetric surgery during pregnancy: what are the risks of anesthesia? Obstet Gynecol Surv 59: 52-56.





