Obstetrics and Gynaecology Cases - Reviews
Successful Treatment of A Primary Cervical Diffuse Large B-Cell Lymphoma with Rituximab-CHOP Immunochemotherapy
Díaz-de la Noval B*, Hernández-Gutiérrez A, Zapardiel I, De Santiago-García J, Diestro-Tejeda MD
Department of Gynecology and Obstetrics, Gynecology Oncology Unit, La Paz University Hospital, Madrid-Spain
*Corresponding author: Díaz-De La Noval B, Department of Gynecology and Obstetrics, Gynecology Oncology Unit, La Paz University Hospital, Paseo de la Castellana 261, 28046- Madrid, Madrid-Spain, Tel: 34616306566, E-mail: begodelanoval@gmail.com
Obstet Gynecol Cases Rev, OGCR-3-085, (Volume 3, Issue 3), Case Report; ISSN: 2377-9004
Received: December 20, 2015 | Accepted: April 23, 2016 | Published: May 02, 2016
Citation: De la Noval B, Hernández A, Zapardiel I, De Santiago J, Diestro MD (2016) Successful Treatment of A Primary Cervical Diffuse Large B-Cell Lymphoma with Rituximab-CHOP Immunochemotherapy. Obstet Gynecol Cases Rev 3:085. 10.23937/2377-9004/1410085
Copyright: © 2016 De la Noval, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Primary Large B-cell extranodal lymphoma of the cervix is a very rare disease and can present with bilateral hydronephrosis from obstruction by the tumor mass. Because of the rarity of this tumor the diagnosis and therapy are often difficult and delaying.
Objective: The aim is to provide an updated review of the literature and report a recent case in our institution.
Case report: We describe a 46-year-old healthy woman with primary extranodal Non-Hodgkin's diffuse large B-cell lymphoma of the uterine cervix Ann Arbor stage IIEA IPI 1. She presented an acute renal failure and severe ureterohydronephrosis successfully treated with 6 courses of chemotherapy based on Rituximab plus Cyclophosphamide, Doxorubicin, Vincristine and Prednisone (R-CHOP) with no major side effects.
Discussion: Symptoms are usually non-specific and the diagnosis is difficult to reach. Diffuse Large B-cell lymphoma is the most common histology type of extranodal non-Hodgkin's lymphoma. Therapy is still under discussion but chemotherapy with R-CHOP or CHOP-like regimens are preferred with a better prognosis and high overall survival.
To conclude, in case of a young woman with a big well defined uterine cervical mass, bilateral ureteral entrapment and an uncertain Pap or biopsy tests, the presence of a lymphoma should be considered. Biopsy and immuno phenotypical evaluation are essential for diagnosis.
Keywords
Non-hodgkin's lymphoma, Diffuse large B-cell lymphoma, Primary cervical large B-cell extranodal lymphoma, Treatment of lymphoma
Abbreviations
DLBCL: Diffuse Large B-Cell Lymphoma; IPI: International Prognostic Index; R-CHOP: Rituximab plus Cyclophosphamide, Doxorubicin, Vincristine and Prednisone; NHL: Non-Hodgkin's Lymphoma; CT: Computed Tomography; PET: Positron Emission Tomography; FDG: 18-Fluodeoxyglucose; SCC: Squamous Cell Carcinoma antigen; FIGO: International Federation of Gynecology and Obstetrics; GCB: Germinal Center B-cell phenotype; R-ACVBP: Rituximab plus Doxorubicin, Cyclophosphamide, Vindesine, Bleomycin and Prednisone; R-EPOCH: Rituximab plus Etoposide, Prednisolone, Oncovin, Cyclophosphamide and Hydroxydaunorubicin.
Introduction
The incidence of Non-Hodgkin's Lymphoma (NHL) has been increasing in recent decades, prevalence of extranodal-NHL is about 30 to 50% of all NHL patients. Primary Large B-cell extranodal lymphoma of the cervix is a very rare disease, 0.008% of all cervical tumors. The Diffuse large B-cell lymphoma (DLBCL) is the most common extranodal lymphoid neoplasm in around 25% of all NHL [1]. DLBCL has an aggressive course with a rapidly growing mass. The gastrointestinal tract and the skin are the most common sites, but almost any organ may be affected. Primary lymphomas of the female reproductive are less than 1% of extranodal NHL and < 0.5% of gynaecological cancers. Primary pelvic NHL sites include the ovary, uterus, cervix, vagina, vulva and regional lymph nodes, with the cervix being the most common.Because of the rarity of this tumor the diagnosis and therapy are often difficult [2].
Case Report
In February 2015, a 46-year-old woman developed an obstructive acute renal failure and severe ureterohydronephrosis. Since last year she had recurrent urinary tract infections, hematuria and pain in the left flank, suspecting urolithiasis. She did not referred pelvic pain but little persistent vaginal spotting and dyspareunia since two months. No relevant personal history except smoking and autoimmune thyroiditis outstanding total thyroidectomy for papillary thyroid carcinoma. An ultrasound showed a small right kidney and moderate left hydronephrosis with no litiasis. Uro-CT scan revealed a cervical mass. Serum creatinine level was 5.63 mg/dl and pyelogram displayed a severe bilateral ureterohydronephrosis with a distal stop. Considering a secondary obstructive acute renal failure and severe hydroureter, the patient required a double nefrostomy (Figure 1).
.
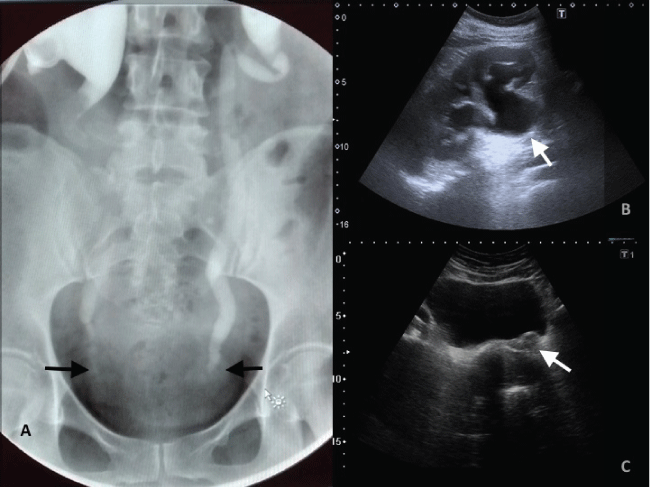
Figure 1: Pyelogram.
(A) Severe bilateral hydronephrosis with a distal stop in both sides. Abdominal echography: severe dilatation of the renal pelvis with cortical thinning in left kidney;
(B,C) High vascularised 6 cm cervical mass that expands to the posterior wall of the bladder trigone and traps both ureters. Uterus and adnexae appeared normal.
View Figure 1
Gynecological evaluation reported a 6 cm-bulky endophytic cervical mass that expands to the upper third of the vagina and both parametrium, left almost to the pelvic wall, no inguinal lymphadenopathy and uterus and adnexae appeared normal. PET-TC showed left iliac lymph nodes without retroperitoneal invasion (Figure 2). Tumor markers altered were SCC 2.1 ng/ml and β2-μglobulin 5.5 mg/dl. Pap test and cervical biopsy were negative, but suspicion was a clinical locally advancedcervical carcinoma at least FIGO stage IIIB, so we performed a conization and deep biopsies to ensure the diagnosis. Histological examination showed a diffuse infiltration of medium to large sized mononuclear cells with a typical fusiform ones around vascular structures but not infiltrating. Inmunohistochemical staining was CD20, CD45, BCL6 and CD30 positive, 50% Ki67, with CK-AE1/AE3, CD15, AML, CD68, BCL2, CD10, MUM1, CD5 and C-MYC negative. Hans's Algorithm suggested a Germinal Center B-cell Lymphoma (GCB). Further staging has not revealed any other localization of disease.
.
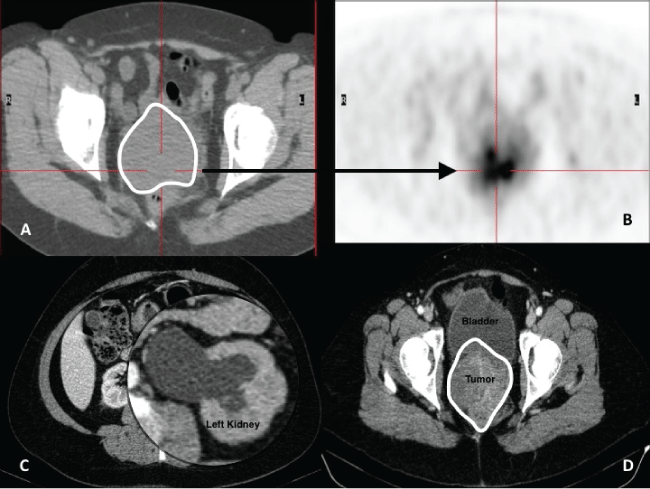
Figure 2: (A,B) PET described an intense FDG avid mass in the uterine cervix, well defined;
(C,D) CT at diagnosis:large Bulky mass involving the whole cervix and reaching the posterior wall of the bladder with bilateral ureteral obstruction and severe hydronephrosis, most on the left side.
View Figure 2
Final diagnosis was a primary high grade extranodal DLBCL type GCB, Ann Arbor stage IIEA1. The age-adjusted International Prognostic Index (IPI) was 1.
She was successfully treated with 6 courses of chemotherapy based in Rituximab plus Cyclophosphamide, Doxorubicin, Vincristine and Prednisone (R-CHOP), standard protocol, with no major side effects. Maintains right ureteral catheter with loss of function in the left kidney. Actually free of disease.
Discussion
DLBCL is the most common extranodal NHL neoplasm (30-58%). Median age of onset described in DLBCL is 40 years old, earlier than median age of NHL (60-65 years old). Folliclular Lymphomais the second most common subtype of lymphoma and represents about 20% to 25% of cases of NHL, others are B-cell small lymphocytic, lymphoma, mantle-cell lymphoma, follicular centre-cell lymphomas, and marginal zone B-cell lymphomas (including MALT lymphomas) amounted to 17%, 12.8%, 4.3%, and 2.1%, respectively [3].
Symptoms are usually non-specific and include abnormal vaginal bleeding as the most common (70%) but it often presents with bilateral ureterohydronephrosis, other symptoms are perineal discomfort (40%), persistent vaginal discharge (20%), abdominal pain or asymptomatic. B symptoms of NHL were rarely seen [4].
The diagnosis may be difficult to reach, and usually requires histological review and immunohistochemical evaluation. Pap is typically negative so colposcopy and a deep biopsy are essential to establish the diagnosis. That is because these tumors arise from cervical stroma, and the overlying squamous epithelial is preserved, at least initially [2].
CT body scan is commonly the study of choice for detection and staging of NHL. Staging also includes a bone marrow biopsy and PET-TC imaging [3].
Immunohistochemistry is necessary to determine the type and subtype of lymphoma. Hans's Algorithm uses the expression of CD20, CD10, BCL6 y MUM1, in our case CD20 positive, CD10 negative, BCL6 positive and MUM-1 negative suggested a germinal center B-type (GCB) DLBCL [4,5]. Lactate deshydrogenase (LDH) is a good prognostic marker of Diffuse Large B-cell Lymphoma, but in our case LDH was not requested because a lymphoma was not first suspected, subsequent tests during and after treatment had normal levels.
The differential diagnosis is usually done with small-cell neuroendocrine carcinoma, undifferentiated cervical carcinoma and adenocarcinoma of the cervix [1].
Staging is performed according to the Ann Arbor System, with stages I and II being most common. Stage I with involvement of a single lymph node area or location, and stage II with two or more lymph node areas or extranodal territory affected in the same side of the diaphragm. Extranodal NHL is represented with an "E". Adding an "A" to the stage denotes the absence of constitutional symptoms, the presence is denoted by adding a "B" to the stage.
At diagnosis, 30% cervical NHL have an early stage (I or II) and 30-40% have extranodal involvement. Between 20-30% of patients have bone marrow involvement, and 5-10% of patients have central nervous system infiltration at the relapse or progression [6].
The international prognostic index (IPI) is considered the most reliable and reproducible prognostic model to quantify the prognosis of NHL. IPI combines five clinical parameters easily measured (tumor stage, serum lactate dehydrogenase level, number of extranodal disease sites, age and performance status) and classified into four risk groups (low 0-1, medium-low 2, intermediate-high 3 and high 4-5). Low risk group has a predicted 4-year progression-free survival and overall survival of 94% [6], our patient had a low IPI value.
The DLBCL has an aggressive course but potentially curable. Therapy is still under discussion; actually, R-CHOP is the most preferred chemotherapy regimen [7]. 70-80% of complete remission with 6 cycles of R-CHOP in stages I and II of Ann Arbor is obtained. Although there are other more intensive regimens as R-ACVBP or R-EPOCH, but with worse adverse effects. In our patient, due to renal failure,these intensive chemotherapy schemes were not advised; also, intensive regimens are prefered for poor-prognosis aggressive Non-Hodgkin Lymphoma.
Radiotherapy is considered for residual lesions, large bulky tumors (> 10 cm) or incomplete response. Radical surgery should be avoided [1]. The overall survival rate for patients with lymphoma of the cervix, vagina, and endometrium is 89%, with a relapse-free survival rate of 70%. The 5-year survival of patients with GCB lymphoma was higher [4].
In conclusion, although Primary Large Bcell extranodal lymphoma of cervix is a rare disease and the squamous cell carcinoma is the most common type of malignancy,in case of a young woman with a quickly developed bulky uterine cervical mass, bilateral hydronephrosis and an uncertain Pap or biopsy tests, the presence of a lymphoma should be considered. Given the aggressiveness of the tumor, a quick diagnosis is necessary. Histological and immunophenotypical evaluation are essential for diagnosis. First line therapy is chemotherapy with good results.
Ethical Statement
The authors declare that they have no competing interests. Written consent was obtained for publication.
References
-
Mandato VD, Palermo R, Falbo A, Capodanno I, Capodanno F, et al. (2014) Primary Diffuse Large B-cell Lymphoma of the uterus: case report and review. Anticancer Res 34: 4377-4390.
-
Bellevicine, Zabatta A, Malapelle U, Vetrani A, Troncone G (2014) Diffuse large B-cell extranodal lymphoma of the uterine cervix: an incidental pap smear finding with histological and immunohistochemical correlation. Diagn Cytopathol 42: 644-646.
-
Novotny S, Ellis T, Stephens J (2011) Primary B-cell lymphoma of the cervix presenting with bilateral hydronephrosis. Obstet gynecol 117: 444-446.
-
Ahmad AK, Hui P, Litkouhi B, Azodi M, Rutherford T, et al. (2014) Institutional review of primary non-hodgkin lymphoma of the female genital tract: a 33-year experience. Int J Gynecol Cancer 24: 1250-1255.
-
Campo E, Swerdlow SH, Harris NL, Pileri S, Stein H, et al. (2011) The 2008 WHO classification of lymphoid neoplasms and beyond: evolving concepts and practical applications. Blood 117: 5019-5032.
-
Cao XX, Li J, Zhang W, Duan MH, Shen T, et al. (2014) Patients with primary diffuse large B-cell lymphoma of female genital tract have high risk of central nervous system relapse. Ann Hematol 93: 1001-1005.
-
Egyed M, Kollar B, Prievara FT, Viski A, Bajzik G, et al. (2007) Successful treatment of a primary uterine B-cell lymphoma with rituximab-chop immunochemotherapy. Haematologica 92: e26-e27.





