Obstetrics and Gynaecology Cases - Reviews
A Rare Case of Acute Pseudo-Meigs' Syndrome Presenting with Pleural Effusion and Ascites and a Ruptured Leiomyoma and Hemorrhagic Shock
Matthew Cowan1, Janine Crantz2, Stephanie Welsh2, William Nahhas2 and Steven R Lindheim2*
1Department of Obstetrics and Gynecology, Franciscan St. James Health Systems, Olympia Fields, Illinois, USA
2Department of Obstetrics and Gynecology, Wright State University, Boonshoft School of Medicine, Dayton, Ohio, USA
*Corresponding author: Steven R Lindheim, MD, Department of Obstetrics and Gynecology, Franciscan St. James Health Systems, Olympia Fields, 128 Apple Street, Suite 3800 Weber CHE, Dayton, OH, USA, 45409, Tel: (937) 208-2301, Fax: (937) 222-7255, E-mail: steven.lindheim@wright.edu
Obstet Gynecol Cases Rev, OGCR-3-070, (Volume 3, Issue 1), Case Report; ISSN: 2377-9004
Received: September 15, 2015 | Accepted: January 25, 2016 | Published: January 28, 2016
Citation: Cowan M, Crantz J, Welsh S, Nahhas W, Lindheim SR (2016) A Rare Case of Acute Pseudo-Meigs' Syndrome Presenting with Pleural Effusion and Ascites and a Ruptured.
Leiomyoma and Hemorrhagic Shock. Obstet Gynecol Cases Rev 3:070. 10.23937/2377-9004/1410070
Copyright: © 2016 Cowan M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Meigs' Syndrome is classically described as a triad of benign solid ovarian tumor with the gross appearance of a fibroma (either a fibroma, thecoma, or granulosa cell tumor) accompanied with ascites and pleural effusion [1]. In contrast, pseudo-Meigs' Syndrome presents with ascites and pleural effusion but with any other pelvic mass [2], including mature teratomas, struma ovarii, and leiomyomata of the ovary, fallopian tube, or uterus [3]. While leiomyomata are the most common benign tumors of the uterus, they are rarely implicated in pseudo-Meigs' Syndrome or intraperitoneal hemorrhage. We present a case of a uterine leiomyoma presenting with both of these serious and rare complications.
Case Report
A 56-year-old Gravida 1, Para 0 female presented to the emergency department by ambulance after acute onset of sharp abdominal pain followed by a pre-syncopal episode. While driving home from a massage, she experienced a sudden acute onset of abdominal pain and light-headedness. She managed to steer her car to the shoulder of the highway, but she side-swiped a concrete median at low speed. Alert and awake, she was able to call for ambulance assistance.
Her past medical history was only significant for increasing abdominal girth. She had not seen a physician for medical care for about ten years, but was otherwise is good health. On further questioning, she did note recent progressive shortness of breath, but ascribed it to a lack of conditioning and exercise. Her gynecologic history was significant for a fibroid uterus.
On initial exam, she was ill-appearing, diaphoretic, and displayed discomfort taking deep breaths. Her BMI was 32 kg/m2, pulse was 107 beats per minute, blood pressure 67 mmHg systolic and 44 mmHg diastolic, with respirations of 16 breaths per minute. Her abdomen was significantly distended, moderately tender, but without rebound or guarding.
Her hemodynamic status responded well to crystalloid fluid resuscitation and she was cross-matched in preparation for packed red blood cell transfusion. Initial hemoglobin was 11.2 grams per deciliter, hematocrit 35%, platelets 267,000 per milliliter, International Normalized Ratio (INR) 1.1. Because of the acute onset of her symptoms and hypotension, an immediate computed tomography (CT) scan with intravenous contrast was done in the emergency department to investigate for possible ruptured abdominal aortic aneurysm. Imaging revealed a large heterogeneous pelvic mass associated with the uterus and surrounding intraperitoneal hematoma (Figure 1A). From the radiologist's interpretation, there was suspicion of active blood extravasation from the ovarian vessels, and there was fluid demonstrated around the liver and spleen (Figure 1B). Additionally, there was a large right-sided pleural effusion without any radiographic signs of chest trauma (Figure 1C).
Due to signs of hemorrhagic shock on presentation, the decision was made to proceed to the operating room emergently. Prior to entering the operating room, repeat blood draw revealed hemoglobin had fallen to 9.3 grams per deciliter, hematocrit 27.2% and platelets 138,000 per milliliter. With fluid replacement, the patient's heart rate rose to 112 beats per minute.
A right pleurocentesis was initially performed draining 1650 cubic centimeters of serosanguineous pleural fluid. An exploratory laparotomy was performed with a midline incision. Initial abdominal survey revealed congealed blood in the pelvis layered under transudative ascitic fluid, totaling approximately 2500 milliliters. The pelvic mass was a complex of leiomyomata measuring 23 centimeters × 12 centimeters × 10 centimeters attached by a relatively narrow stalk to the uterine fundus. It also had loose parasitic adhesions to the small bowel. A degenerating cystic fibroid near the superior pole of the mass, approximately 8 centimeters in diameter, had ruptured, was actively bleeding, and was filled with hemorrhagic material. Both ovaries were atrophic with no active bleeding from the ovarian vessels as suspected on CT and there was no sign of metastatic disease in the peritoneum (Figure 1D). A supracervical hysterectomy with bilateral salpingoophorectomy was performed given her body mass index and significant intraperitoneal blood loss. The surgery proceeded uneventfully and intra-operative blood loss was minimal compared to pre-existing blood. Total blood and ascitic fluid volume removed from the abdomen was 3800 milliliters. Additionally, 1650 milliliters of pleural fluid was drained in the operating room. Six units of packed red blood cells and two units of fresh frozen plasma were transfused intraoperatively.
.
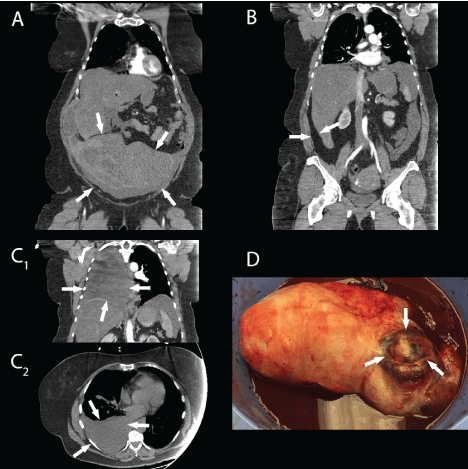
Figure 1: A: Uterine mass on Computer Tomography with IV contrast (arrows); B: Ascites can be seen displacing the liver medially (arrows); C1,2: Right-sided pleural effusion in coronal and transverse planes (arrows); D: Resected Pelvic Mass in a 12-inch basin with the ruptured cavity at the superior pole (arrows).
View Figure 1
Her post-operative recovery was uneventful with complete resolution of her symptoms as well as her pleural effusion on chest X-ray. She was discharged home on post-operative day 3. Pathologic examination of the specimen revealed benign leiomyomata, adenomyosis, unremarkable endometrium, ovaries and tubes. Cytology from the pleural fluid revealed mesothelioma cells and mixed inflammatory cells with the absence of malignant cells; peritoneal fluid was extravascular fluid of low protein content without malignancy or blood clot.
Discussion
Meigs' Syndrome and pseudo-Meigs' Syndrome are very rare conditions. Meigs' Syndrome is present in approximately 1% of all ovarian fibroma, thecoma, and granulosa cell tumors. Specifically in ovarian fibromas, ascites and pleural effusion have been described in 10-15% and 1% of cases, respectively [4]. The incidence of pseudo-Meigs' Syndrome is even lower and is rarely associated with benign leiomyomata, which was first reported by Authur in 1909 [5]. Since, an additional 33 cases have been reported in the literature (MEDLINE search terms: pseudo-Meigs' and leiomyoma, leiomyoma and ascites). Likewise, hemorrhage from uterine leiomyomata is also a rare occurrence, of which 52 cases have been reported in the literature (MEDLINE search terms: leiomyoma intraperitoneal hemorrhage).
Paracentesis and thoracentesis can be performed for symptomatic relief in either syndrome, but treatment is focused on surgical removal of the tumor. The retrospective diagnosis can be made when the ascites and pleural effusions resolve and do not re-accumulate.
Our case is unusual in that the patient presented in acute distress from leiomyoma rupture as well as pleural effusion. These two overlapping rarities confounded the diagnosis initially. While it is difficult to differentiate ascites in the setting of hemoperitoneum, we can assume our patient did have the triad of pseudo-Meigs' Syndrome prior to the rupture of the leiomyoma because of the cytology of the peritoneal fluid, and her pleural effusion.
The pathophysiology of the ascites and pleural effusion in Meigs' or pseudo-Meigs' Syndrome is not fully understood. It is believed that the ascitic fluid may be transudative or exudative, and the amount of fluid often correlates with the size of the tumor. It has been postulated that interstitial edema accumulates in the mass itself due to limited venous and lymphatic return channels in relation to a large amount of arterial blood flow. This interstitial edema can cause a transudative ascites [6,7], hence the amount of fluid often correlates with the size of the tumor. Another plausible mechanism of ascites may be direct transudate from surrounding lymphatics or vessels due to tumor compression or tumor torsion [8,9]. The pleural effusion likely is transferred via lymphatic channels from the peritoneum across the diaphragm and often is on the right side [6,10]. Serosanguineous and hemorrhagic effusions have been reported both with benign and malignant pathology and are thought to be related to pleural inflammation [11].
Others have suggested that there is an increase in vascular endothelial growth factor (VEGF) and interleukin 6 (IL-6) which is known to cause vascular hyperpermeability [12] and may be involved in the clinical manifestations. A case of pseudo-Meigs' Syndrome has been described where increased VEGF production from the ovaries was noted [7]. This is comparable to the elevated IL-6 in ovarian hyperstimulation, which can have similar presentations with massive ascites and pleural effusions [13]. In another case of pseudo-Meigs' Syndrome caused by a metastatic ovarian mass of colorectal origin, removal of the mass resulted in decreased serum VEGF levels and resolution of the patient's pleural effusions and ascites [6]. Interestingly, the VEGF was found to be expressed from the oviducts but not from the tumor itself in this case.
Hemorrhagic shock associated with leiomyomata is usually due to rupture of a vessel traversing the surface of a large subserosal leiomyoma. In the case of a large fibroid, the feeding vessels can be quite massive and their walls attenuated. An increase in intra-abdominal pressure, trauma, pregnancy, or menstruation has been postulated to increase congestion and subsequent rupture of these vessels [14]. Other cases have been described wherein trauma causes damage to the tumor itself, leading to hemorrhage [15], while still others have described rupture of a degenerating cystic leiomyoma as cause of hemorrhage [16]. In our case, the cystic leiomyoma cavity was filled with congealed blood, leading us to believe the hemorrhage originated from a disrupted vessel within the wall of the leiomyoma.
While these syndromes should be considered in women with the triad of pelvic mass, ascites and pleural effusion, they can mimic the presentation of much more serious malignant tumors. In a hemodynamically stable patient, cancer antigen 125 (CA-125) measurements may be done, however in our case given the acute presentation, this was not done. Furthermore, this may further cloud the diagnosis, as CA-125 can be elevated in many types of intra-abdominal benign pathology [17].
Conclusion
Although pseudo-Meigs' Syndrome is very rare, this case study is a reminder that benign leiomyoma can cause significant sequela if not addressed. The life-threatening complications encountered in this case mimic behaviors and complications of malignant neoplasms, thus a broad differential diagnosis is necessary for surgical planning.
References
-
Meigs JV (1954) Fibroma of the ovary with ascites and hydrothorax; Meigs' syndrome. Am J Obstet Gynecol 67: 962-985.
-
Meigs JV (1954) Pelvic tumors other than fibromas of the ovary with ascites and hydrothorax. Obstet Gynecol 3: 471-486.
-
Williamson JG, Patel D, Menzies DN (1972) Leiomyomata of the uterus associated with ascites and hydrothorax. J Obstet Gynaecol Br Commonw 79: 273-280.
-
Saha S, Robertson M (2012) Meigs' and Pseudo-Meigs' Syndrome. AJUM 15: 29-31.
-
Dunn JS Jr, Anderson CD, Method MW, Brost BC (1998) Hydropic degenerating leiomyoma presenting as pseudo-Meigs syndrome with elevated CA 125. Obstet Gynecol 92: 648-649.
-
Okuchi Y, Nagayama S, Mori Y, Kawamura J, Matsumoto S, et al. (2010) VEGF hypersecretion as a plausible mechanism for pseudo-meigs' syndrome in advanced colorectal cancer. Jpn J Clin Oncol 40: 476-481.
-
Yonehara Y, Yanazume S, Kamio M, Togami S, Tasaki T, et al. (2014) Concentrated ascites re-infusion therapy for pseudo-Meigs' syndrome complicated by massive ascites in large pedunculated uterine leiomyoma. J Obstet Gynaecol Res 40: 1944-1949.
-
Terada S, Suzuki N, Uchide K, Akasofu K (1992) Uterine leiomyoma associated with ascites and hydrothorax. Gynecol Obstet Invest 33: 54-58.
-
Kazanov L, Ander DS, Enriquez E, Jaggi FM (1998) Pseudo-Meigs' Syndrome. Am J Emerg Med 16: 404-405.
-
Oguma T, Yamasaki N, Nakanishi K, Kinoshita D, Mitsuhashi T, et al. (2014) Pseudo-Meigs' syndrome associated with hydropic degenerating uterine leiomyoma: a case report. J Obstet Gynaecol Res 40: 1137-1140.
-
Kumar S, Verma SK, Singh R, Prasad R (2009) Hemorrhagic pleural effusion secondary to sarcoidosis: A brief review. Ann Thorac Med 4: 27-31.
-
Kraft A, Weindel K, Ochs A, Marth C, Zmija J, et al. (1999) Vascular endothelial growth factor in the sera and effusions of patients with malignant and nonmalignant disease. Cancer 85: 178-187.
-
Rizk B, Aboulghar M, Smitz J, Ron-El R (1997) The role of vascular endothelial growth factor and interleukins in the pathogenesis of severe ovarian hyperstimulation syndrome. Hum Reprod Update 3: 255-266.
-
Akahira J, Ito K, Nakamura R, Jajima A (1998) Massive intraperitoneal hemorrhage and hypovolemic shock due to rupture of a coronary vessel of a uterine leiomyoma: a report of two cases. Tohoku J Exp Med 185: 217-222.
-
Estrade-Huchon S, Bouhanna P, Limot O, Fauconnier A, Bader G (2010) Severe life-threatening hemoperitoneum from posttraumatic avulsion of a pedunculated uterine leiomyoma. J Minim Invasive Gynecol 17: 651-652.
-
Takai H, Tani H, Matsushita H (2013) Rupture of a degenerated uterine fibroid as a cause of acute abdomen: a case report. J Reprod Med 58: 72-74.
-
Moss EL, Hollingworth J, Reynolds TM (2005) The role of CA125 in clinical practice. J Clin Pathol 58:308-312.





