Obstetrics and Gynaecology Cases - Reviews
Uterine Arteriovenous Malformations and its Imitators: Is there a Role for Hysteroscopy?
Christopher M Tarney*, Saioa Torrealday and Jason Parker
Department of Obstetrics and Gynecology, Womack Army Medical Center, Fort Bragg, NC, USA
*Corresponding author: Christopher M Tarney, Department of Obstetrics and Gynecology, Womack Army Medical Center, 2817 Reilly Road, Fort Bragg, NC 28307, USA, Tel: 908-419-5046, Fax: 910-907-2903, E-mail: christopher.tarney@us.army.mil
Obstet Gynecol Cases Rev, OGCR-2-068, (Volume 2, Issue 6), Case Report; ISSN: 2377-9004
Received: October 26, 2015 | Accepted: December 24, 2015 | Published: December 28, 2015
Citation: Tarney CM, Torrealday S, Parker J (2015) Uterine Arteriovenous Malformations and its Imitators: Is there a Role for Hysteroscopy?. Obstet Gynecol Cases Rev 2:068. 10.23937/2377-9004/1410068
Copyright: © 2015 Tarney CM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Uterine arteriovenous malformation (AVM) is an uncommon vascular disease, which can be a life-threatening condition. Treatment recommendations include embolization versus hysterectomy.
Case: A 26 year-old gravida 6 para 2042 presented three months after an early pregnancy loss with persistent vaginal bleeding.
Ultrasonography and angiography demonstrated a hypervascular intrauterine mass consistent with an AVM. Hysteroscopy demonstrated an intracavitary mass with increased vascularity which, upon resection and pathology evaluation, was confirmed to be retained products of conception (RPOC).
Conclusion: AVMs are a rare condition in which angiography has classically been the gold standard modality to clinch the challenging diagnosis. Since there are several conditions which mimic the presentation of AVMs, hysteroscopy can be a useful tool in the diagnosis, which can influence treatment decisions.
Teaching points: 1. Angiography is considered the gold standard for definitive diagnosis of uterine AVMs; however, many diagnoses present in a similar fashion, which often makes treatment decisions dangerous.
2. In case of persistently elevated hCG levels that suggest retained products of conception, and contradicting digital subtraction angiography evidence for AVM, hysteroscopy may play a valuable role in differentiating between these two entities.
Introduction
Uterine arteriovenous malformations (AVMs) are an uncommon vascular disease occurring in women during the reproductive years, which can lead to life-threatening vaginal bleeding. The prevalence of AVMs is unknown with less than 100 case reports described in the literature [1]. Uterine AVMs may be congenital or acquired; risk factors for the latter include early pregnancy loss, pregnancy termination, and instrumentation of the uterus, cervical or endometrial cancer, endometritis, and trophoblastic disease [2]. Hysterectomy was traditionally the treatment of choice for uterine AVMs, but angiographic embolization is an alternative solution for women who desire uterine preservation [1]. Embolization of uterine AVMs, however, is not without risk, and its long-term effects on fertility and future pregnancies remain unknown [3].
Uterine AVMs were initially diagnosed by laparotomy or upon inspection of the uterus after hysterectomy, but there are now multiple radiologic techniques to diagnose uterine AVMs [4]. Gray-scale and color Doppler ultrasonography, or magnetic resonance angiography, provide non-invasive methods for the initial diagnosis of a hypervascular uterine mass. However, the gold standard for the diagnosis of a uterine AVM remains angiography [1,4-7]. We present a case of a patient with a hypervascular mass seen on color Doppler ultrasonography on imaging after an early pregnancy loss, and angiography suggesting uterine AVM. Hysteroscopic evaluation was performed to help characterize the lesion and plan the appropriate course of action. In our case, the patient's pathology demonstrated necrotic retained products of conception; thus highlighting the important role hysteroscopy can play prior to undergoing established treatment methods that have significant impact on future fertility.
Case
A 26 year-old gravida 6 para 2042 presented to the emergency room with a three month history of continuous vaginal bleeding after experiencing an early pregnancy loss. Ultrasonography during the previous pregnancy was notable for a single, intrauterine gestational sac with measurements consistent with 6 2/7 weeks gestation with no identifiable fetal pole or yolk sac. Her obstetric history was notable for one term vaginal delivery followed by three early pregnancy losses, one of which required suction dilation and curettage for uterine evacuation. Prior to her most recent early pregnancy loss, she had an uncomplicated term vaginal delivery. Otherwise, the patient's history was unremarkable for any other uterine instrumentation or pathology.
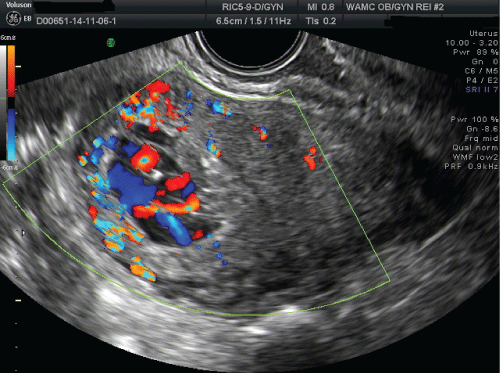
Upon presentation, the patient's serum quantitative hCG was 34.1 mIU/mL and ultrasonography showed a complex cystic fluid-filled mass measuring 2.5 × 1.6 × 2.3 cm with internal vascular flow (Figure 1). The following week repeat serum quantitative hCG was 34.4 mIU/mL and a three-dimensional color Doppler sonography showed a hypervascular endometrial lesion with turbulent flow (Figure 2). The differential diagnosis consisted of retained products of conception from the previous early pregnancy loss, uterine AVM, gynecologic malignancy, gestational trophoblastic disease, and hemangioma.
.
Figure 1: Color-Doppler sonography showing hypervascular cystic mass within the endometrial cavity.
View Figure 1
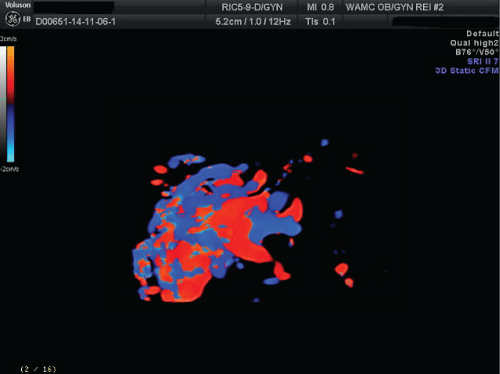
.
Figure 2: Hypervascular uterine mass on three-dimensional color-Doppler sonography.
View Figure 2
The patient underwent angiography to further evaluate the uterine mass. Angiography revealed a prominent hypervascular mass measuring 7.0 × 6.2 × 6.2 cm with early venous filling consistent with AVM. A repeat serum quantitative hCG remained unchanged at 34.4 mIU/mL and her qualitative urine hCG was negative. The reference laboratory threshold for a positive urine qualitative hCG is a serum quantitative hCG of at least 20.0 mIU/mL; therefore, the addition of the urine testing suggested a possible heterophilic antibody.
The patient's history of continuous vaginal bleeding for three months following her pregnancy loss, the presence of a hypervascular uterine mass, and the persistent positive quantitative serum hCG were consistent with likely retained products of conception. However, the urine hCG testing was negative suggesting the possibility of a heterophilic antibody. Furthermore, angiography demonstrated findings consistent with a uterine arteriovenous malformation. Given these findings, we proceeded with hysteroscopy to further evaluate the uterine mass. Operative findings were notable for a large intracavitary mass with increased vascularity. Given an inability to entirely visualize the lesion, we proceeded with laparotomy in which a transfundal incision was performed to remove the endometrial mass that measured 5.2 × 1.2 × 1.4 cm. There were no intraoperative or postoperative complications associated with the surgery. The total estimated blood loss was 100 mL. Pathology demonstrated necrotic immature chorionic villi consistent with retained products of conception.
Discussion
Uterine AVMs are rare vascular lesions that present with heavy vaginal bleeding usually in the reproductive age. Although this condition is rare, uterine AVMs have been associated with life-threatening bleeding that may result in hysterectomy. Other conditions which present with vaginal bleeding and may have ultrasound findings similar to an AVM include retained products of conception, hypervascular polyp, leiomyoma, hemangioma, or gestational trophoblastic disease.
The diagnosis of a uterine AVM is challenging due to the obscurity of the condition and its similarity to other benign hypervascular lesions. The various imaging modalities used to screen for a uterine AVM include gray-scale sonography, color Doppler sonography, and magnetic resonance angiography. Recently, there have been an increasing number of reports regarding uterine vascular lesions. This may not necessarily be due to a true rise in the incidence of uterine AVMs, but rather the improvement in color Doppler sonography [6]. However, there is consensus that angiography is the gold standard for diagnosing uterine AVMs [6,7].
Hysterectomy has been the definitive treatment of choice for uterine AVMs, especially for women who presented with life threatening vaginal bleeding. However, uterine artery embolization is now an attractive alternative for women desiring future fertility. There is limited information on pregnancy after uterine artery embolization, with concerns regarding abnormal placentation. Therefore, uterine artery embolization should be used cautiously for women who desire fertility [8]. More importantly, a high clinical suspicion must be used to carefully manage women presenting with persistent vaginal bleeding in the setting of a hypervascular mass on sonography after experiencing an early pregnancy loss. The most common cause for these findings is retained products of conception, which can be managed with uterine curettage or operative hysteroscopy to evacuate the uterus. Nevertheless, in the presence of a true uterine AVM, the risk of hemorrhage can lead to significant morbidity and mortality.
Our case illustrates the importance of carefully reviewing a patient's history and radiologic findings prior to offering treatment, which can impact the patient's reproductive future. The patient's history, timing of presentation, and elevated serum quantitative hCG were consistent with the fact that the hypervascular mass, initially seen on sonography, was likely secondary to retained products of conception. However, given the plateau of the serum quantitative hCG and negative urine qualitative testing (suggesting possible heterophilic antibody), angiography was obtained for further clarification. Angiography demonstrated the classic findings of a uterine AVM. In efforts to accurately determine whether the uterine lesion was in fact retained product of conception or an AVM, hysteroscopy was performed to better characterize the uterine lesion. Hysteroscopy demonstrated a large, hypervascular, intracavitary mass, suspicious for retained products of conception. The information provided by visualizing the lesion was paramount to determining that the lesion was retained products of conception and not an AVM making the decision to proceed with resection of the mass via laparotomy. This case suggests that angiography has limitations in its ability to firmly diagnose a uterine AVM since there are many other conditions that are great imitators of classic AVM findings. For patients who present with a hypervascular uterine mass, imaging suspicious for a uterine AVM, and a desire for future fertility, hysteroscopy should be considered as an additional diagnostic modality, and possible treatment option.
Financial Disclosure
No funding or financial support was received for this work.
Disclaimer
The opinions or assertions contained herein are the private views of the authors and are not to be construed as the official policy of the Department of the Army, Department of Defense, or the U.S. Government.
References
-
Hashim H, Nawawi O (2013) Uterine arteriovenous malformation. Malays J Med Sci 20: 76-80.
-
Ichikawa Y, Nakauchi T, Sato T, Oki A, Tsunoda H, et al. (2003) Ultrasound diagnosis of uterine arteriovenous fistula associated with placental site trophoblastic tumor. Ultrasound Obstet Gynecol 21: 606-608.
-
Memsta M, Homer H (2012) Complications associated with uterine artery embolization for fibroids. Obstetrics and Gynecology International 2012: 1-5.
-
Grivell RM, Reid KM, Mellor A (2005) Uterine arteriovenous malformations: a review of the current literature. Obstet Gynecol Surv 60: 761-767.
-
Ranjha K, Nabil N, Khalid KN, Rana A, Tariq N (2014) Uterine arteriovenous malformation. JSOGP 4: 170-173.
-
Mungen E (2003) Vascular abnormalities of the uterus: have we recently over-diagnosed them? Ultrasound Obstet Gynecol 21: 529-531.
-
Castro-Aragon I, Aragon I, Urcuyo R, Abbott J, Levine D (2004) Conservative management of a uterine arteriovenous malformation diagnosed in pregnancy. J Ultrasound Med 23: 1101-1104.
-
American College of Obstetricians and Gynecologists (2008) ACOG practice bulletin. Alternatives to hysterectomy in the management of leiomyomas. Obstet Gynecol 112: 387-400.





