Obstetrics and Gynaecology Cases - Reviews
Left Vaginal Obstruction and Complex Left Uterine Horn Communication in a 12 Year Old Female
Barry E. Perlman*, Amy S. Dhesi, Gerson Weiss
Department of Obstetrics, Gynecology and Women's Health, Rutgers - New Jersey Medical School, Newark, United States of America
*Corresponding author:
Barry E. Perlman DO, Department of Obstetrics, Gynecology and Women's Health, Rutgers - New Jersey Medical School, MSB E-506, 185 South Orange Avenue, Newark, NJ 07101-1709, United States of America, Tel: 732 233 0997, E-mail: Perlman.barry@gmail.com
Obstet Gynecol Cases Rev, OGCR-2-064, (Volume 2, Issue 5), Case Report; ISSN: 2377-9004
Received: September 01, 2015 | Accepted: October 27, 2015 | Published: October 29, 2015
Citation: Perlman BE, Dhesi AS, Weiss G (2015) Left Vaginal Obstruction and Complex Left Uterine Horn Communication in a 12 Year Old Female. Obstet Gynecol Cases Rev 2:064. 10.23937/2377-9004/1410064
Copyright: © 2015 Perlman BE, et al This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Obstructive Mullerian duct anomalies are an infrequently encountered clinical problem. The use of imaging and surgical exploration allowed for diagnosis and treatment of symptoms of a complex obstructive mullerian anomaly. We present a case of a 12 year old female with a history of intermittent lower abdominal pain and absent left kidney who was found to have an obstructed left vagina and complex left uterine horn communications resulting in hematocolpos, hematometra, and endometriosis.
Key words
Mullerian duct anomalies, hematocolpos, obstructed vagina, uterine horn communication
Introduction
Obstructive Mullerian duct anomalies are an infrequently encountered clinical problem, occurring at an estimated incidence between 0.16% to 10% of all women [1]. Patients with obstructive anomalies often present in adolescence with progressively worsening pain. Developmental abnormalities during organogenesis, fusion, or septal resorption of the mullerian ducts can lead to varying anomalies as described by the American Society for Reproductive Medicine [2]. Despite a comprehensive classification system, not all cases will fall into one of these categories. We present a case of a 12-year-old female patient with two uterine horns, one midline cervix extending from the right horn, communications between the left horn to the cervix and to a partially obstructed vagina, resulting in significant hematocolpos with pain. Noninvasive techniques of ultrasound, magnetic resonance imaging (MRI), and intravenous pyelogram were initially attempted to establish her anatomic abnormalities, but ultimately, surgical exploration was needed for diagnosis of her complex anatomy and for treatment of her pain.
Case
A 12-year-old virginal female initially presented to the emergency room with several days of worsening abdominal pain. She reported a six-month history of intermittent left lower abdominal pain, and menarche had occurred three months prior to presentation. She has a history of absent left kidney.
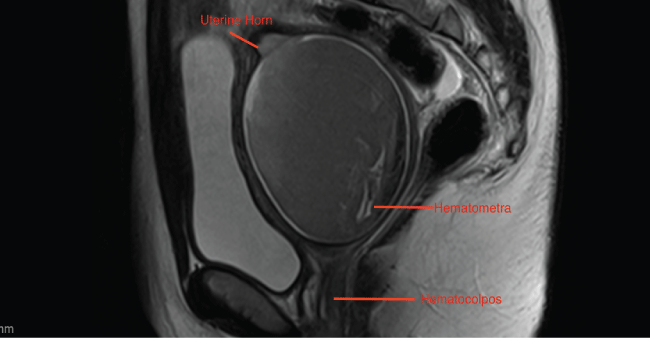
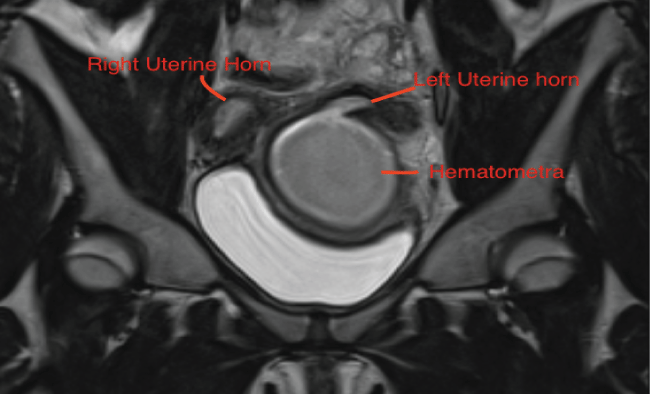
Abdominal ultrasound confirmed absent left kidney. Transabdominal pelvic sonogram revealed two prominent uterine cornua with an endometrial thickness of 3 mm in each horn. The right cornu measured 11.4 × 2.0 × 3.6 cm and the left cornu measured 10.4 × 2.8 × 4.1 cm. A 7 cm mass in the endocervical canal, concerning for hematocolpos, represented an occlusion extending to the left vagina (Figure 1).
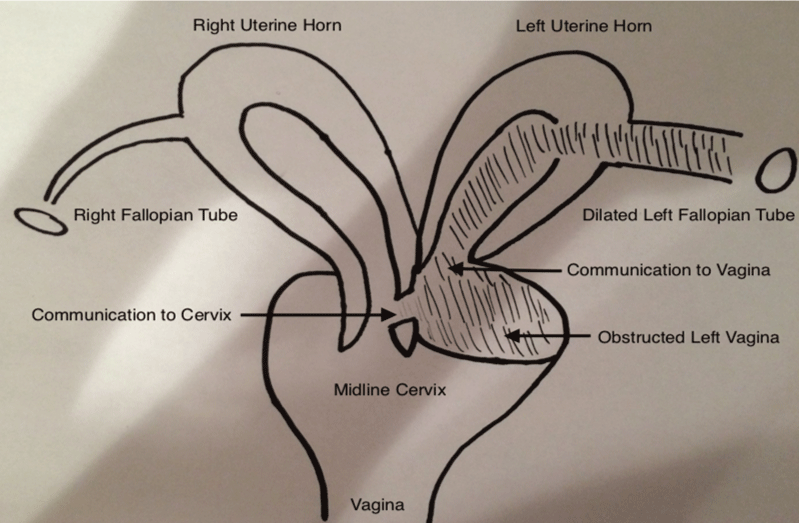
.
Figure 1: Diagram of left vaginal obstruction and complex left uterine horn communication
View Figure 1
She underwent further imaging with two MRI studies that were mutually inconclusive and inconsistent in regards to her pelvic anatomy. An intravenous pyelogram demonstrated a solitary right kidney with a normal right renal collecting system and a single ureter extending toward the bladder.
Based on presenting factors and inconclusive imaging, the decision was made to surgically explore the pelvic anatomy for diagnosis and treatment of her symptoms. Prior to surgery, the patient was placed on continuous combined oral contraceptive pills to suppress menstrual cycles. Pelvic examination under anesthesia revealed a single midline cervix with a normal right vaginal lateral wall and a significant bulge adjacent to the cervix in the left fornix (Figure 2 and Figure 3).
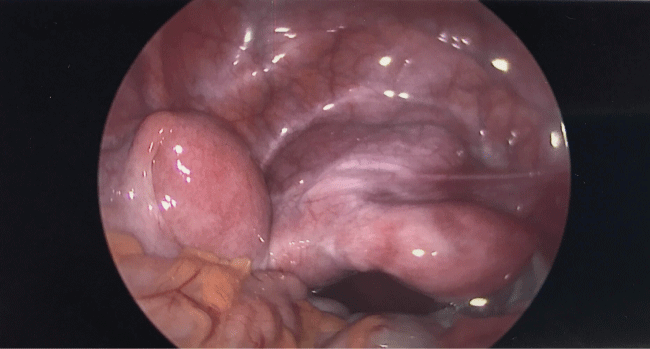
Under direct visualization with laparoscopy, two distinct uterine horns were visualized. The right horn and right fallopian tube appeared normal. The left horn appeared elongated and larger with a dilated left fallopian tube. Normal appearing, post-pubertal ovaries were seen bilaterally. The left fallopian tube was noted to be blocked and had adhesions to the uterus, the left pelvic sidewall, and the large bowel (Figure 4). These adhesions were lysed. Endometriotic implants were present along the serosa of the left uterine horn and were fulgurated.
Subsequently, hysteroscopy was performed. At time of hysteroscopy, the dilators were easily inserted with the curve to the right. The hysteroscope was inserted through a midline cervix, which centered into a normal right uterine cavity. No damage from the dilators or hysteroscope was noted. The right tubal ostium was visualized and appeared normal. When the hysteroscope was placed in the cervical canal, a communication was observed from the left uterine horn into the cervix with drainage of blood into the cervical canal (Figure 5).

.
Figure 5: Hysteroscopic imaging of Communication from Left Uterine Horn into Midline Cervix
View Figure 5
Attention was turned to the vaginal bulge in the left fornix. A 2 cm incision was made in the out-pouching of vaginal tissue, exposing old blood and mucus. The vaginal space was copiously irrigated and marsupialized. Inspection of the left side of the vagina revealed no visible left cervix as well as no obvious communication from the previously obstructed left vaginal fornix to the midline cervix or to the left uterine horn.
Postoperative imaging with MRI demonstrated two uterine horns with collapsed endometrial cavities and resolution of hematocolpos. Bleeding occurred through a single midline cervical os.
Postoperatively, the patient resumed continuous oral contraceptive pills to suppress future growth of endometriosis. She reported significant improvement in pain. During the postoperative visit a repeat vaginal exam was performed and a single midline cervix was once again palpated. Further anatomic evaluation was delayed until she patient is older and more accepting of additional exams.
Discussion
The urinary and genital systems both arise from a common ridge of mesoderm along the dorsal body wall, and both rely on normal development of the mesonephric system [3]. The ureters, renal calices, and collecting tubules are formed from the ureteral bud, which arises from the mesonephric ducts, which also induce formation of the kidneys [4]. Hence, abnormal differentiation of the mesonephric and paramesonephric ducts may also be associated with anomalies of the kidneys. Renal anomalies occur in 29% of mullerian abnormalities and are often ipsilateral to the side of obstruction, if present [5]. While described in the literature, these complex urinary and genital system malformations are rare. Often these abnormalities are undiagnosed or misdiagnosed resulting in improper management.
Renal agenesis and concurrent obstruction of the vagina are twice as likely to occur on the right as on the left side of the body [6]. This case is unique as the patient had a history of a congenital absent left kidney and was later found to have an obstruction of the left vagina. The incidence of left-sided renal and vaginal abnormalities, as seen in our patient, is a rare occurrence based on a literature review.
Furthermore, the communications involving the left uterine horn were found to be remarkably complex and likely of two separate origins. The communication between the left uterine horn and the cervix was visualized on hysteroscopy. An additional communication between the left uterine horn and left occluded vaginal fornix was not seen after marsupialization, but we suspect a small communication must be present given existing hematocolpos. The communications between the left uterine horn into the cervix and into the left vagina may have formed as a consequence of left uterine and fallopian tube obstruction and resulting pressure due to accumulation of blood. Hematocolpos, hematometra, and endometriosis as seen in this patient are likely outcomes of outflow tract obstruction. In the case of our patient, her symptoms were likely due to the left uterine horn obstruction, left vaginal obstruction, and left fallopian tube obstruction.
With newer imaging technology, early preoperative diagnosis is often possible. MRI is now considered the imaging of choice given high accuracy, but with a high degree of concordance between 3D ultrasound and MRI in the diagnosis of uterine malformations, this may change [7-9].
The continued use of history, physical exam and imaging has allowed for the diagnosis and surgical plan to be made in many patients. However, in our case, MRI was not an effective tool in diagnosis. Surgical evaluation was necessary to determine the anatomy and thus, the treatment plan. Surgical exploration and marsupialization of vaginal tissue provided the patient with resolution of hematocolpos and its associated pain. As she approaches concerns about future reproductive function, we recommend evaluation with hysterosalpingography to further delineate uterine horns, cervix, and the complex communications involving the left uterine horn to the cervix and to the vagina.
References
-
Byrne J, Nussbaum-Blask A, Taylor WS, Rubin A, Hill M, et al. (2000) Prevalence of Mullerian duct anomalies detected at ultrasound. Am J Med Genet 94: 9-12.
-
(1988) The American Fertility Society classifications of adnexal adhesions, distal tubal obstruction, tubal occlusions secondary to tubal ligation, tubal pregnancies, Mullerian anomalies and intrauterine adhesions. Fertil and Steril 49: 944-955.
-
Moore KL, Persaud TV (1998) The urogenital system: the development of the genital system. In: The developing human: clinically oriented embryology. 6th ed. Pa: Saunders, Philadelphia: 303.
-
Speroff L, Glass RH, Kase NG (1978) Development of the mullerian system. In: Mitchell C, eds. Clinical gynecologic endocrinology and infertility. Baltimore, Md: Williams & Wilkins, Lippincott: 124.
-
Li S, Qayyum A, Coakley FV, Hricak H (2000) Association of renal agenesis and mullerian duct anomalies. J Comput Assist Tomogr 24: 829-834.
-
Vercellini P, Daguati R, Somigliana E, Vigano P, Lanzani A, et al. (2007) Asymmetric lateral distribution of obstructed hemivagina and renal agenesis in women with uterus didelphys: institutional case series and systematic literature review. Fertil Steril 87: 719-724.
-
Troiano RN, McCarthy SM (2004) Mullerian duct anomalies: imaging and clinical issues. Radiology 233: 19-34.
-
Chandler TM, Machan LS, Cooperberg PL, Harris AC, Chang SD (2009) Mullerian duct anomalies: from diagnosis to intervention. Br J Radiol 82: 1034-1042.
-
Pellerito JS, McCarthy SM, Doyle MB, Glickman MG, DeCherney AH (1992) Diagnosis of uterine anomalies: relative accuracy of MR imaging, endovaginal sonography, and hysterosalpingography. Radiology 183: 795-800.