Obstetrics and Gynaecology Cases - Reviews
The Case of 11w+ 2d Fetal Heart Rate Positive Unruptured Cervical Pregnancy
Önder Sakin*, Bülent Kars, ‚lke Tanir and Ömer Talip Turhan
Dr. Lutfi Kirdar Kartal Education and Research Hospital, Department of Obstetrics & Gynecology, Turkey
*Corresponding author: Onder Sakin, Dr. Lutfi Kirdar Kartal Education and Research Hospital, Department of Obstetrics & Gynecology, Kaptan Arif Caddesi Altin Apt. no: 56/8, Erenköy, Ìstanbul, Turkey, Tel: +90 (505) 8110031, Fax: +90 (216) 411 54 76, E-mail: sakin-onder@hotmail.com
Obstet Gynecol Cases Rev, OGCR-2-055, (Volume 2, Issue 4), Case Report; ISSN: 2377-9004
Received: June 08, 2015 | Accepted: August 02, 2015 | Published: August 05, 2015
Citation: Sakin O, Kars B, Tanir I, Turhan OT (2015) The Case of 11w+ 2d Fetal Heart Rate Positive Unruptured Cervical Pregnancy. Obstet Gynecol Cases Rev 2:055. 10.23937/2377-9004/1410055
Copyright: © 2015 Sakin O, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aim: The treatment of cervical pregnancy which is one of the rarest forms of ectopic pregnancy is one of the cases difficult decisions need to be taken. Many years ago when hysterectomy was the only treatment and in case of late treatment decision, 50% of maternal mortality was seen, which results in a change of status with the shape of the high-risk pregnancies' extremely minimal invasive treatment may be possible Moreover, the patient fertility will be preserved and hysterectomy and the negative situations accordingly will stay away.
Case: Patient admitted to our emergency department with vaginal bleeding and CRL 11 + 2 weeks with positive fetal cardiac activity was diagnosed cervical ectopic pregnancy and a total of 75 mg of methotrexate via transabdominal approach and intracardiac ultrasound-guided intralesional application was made. At the end of 3rd month complete regression was achieved.
Conclusion: Successful treatment with systemic and intralesional methotrexate in the treatment of ectopic pregnancy has been reported in recent years.
As is known, systemic methotrexate treatment success in particular from 10 weeks of pregnancy and pregnancies with fetal cardiac activity decreases or sometimes no answer can be received. Therefore, in our case, the treatment of intralesional and intracardiac methotrexate is primarily applied and definite success has been achieved.
Although, each case in their own separate and private; in cervical pregnancies more than 10 weeks and with fetal cardiac activity, we propose intracardiac and intralesional methotrexate therapy to be applied as a form of primary treatment.
Background
Cervical ectopic pregnancy is one of the rarest forms of ectopic pregnancies [1]. Cervical ectopic pregnancy is a condition that is very rare, but dangerous for life. Years ago, the only treatment for these cases was hysterectomy and the cases resulted with maternal mortality by 50 percent, thanks to new treatments that are applied today, it is possible to encounter this situation [2]. Still, despite all the innovations the management of cervical ectopic pregnancy often leads to morbidity [3].
Predisposing factors are dilatation curettage and cesarean section which cause endometrial damage. It may lead to severe bleeding and life threatening situations. It may be diagnosed with transvaginal ultrasound [4]. Magnetic resonance imaging is another method for early diagnosis. When necessary; it can be utilized by both.
Today, thanks to the use of ultrasound in the last two decades with precise b-hCG measurement ectopic pregnancies including cervical pregnancy can be recognized in early weeks; this lead to conservative approach modalities being discovered [5].
Selected appropriate cases of cervical pregnancy methotrexate and misoprostol can be a good alternative to surgical treatment [1]. While local and systemic methotrexate injection of a single dose or series of methotrexate and leucovorin injection regimens can be applied; mifepristone and local potassium chloride are other methods in the treatment [3]. Especially methotrexate is the most preferred treatment [6].
As surgical procedures; curettage and tamponade, internal iliac artery ligation, angiographic uterine artery embolization, carboplast intracervical injection may be other appropriate methods [7].
Each case must be evaluated separately and in their case the special treatment should be applied. We also aimed to discuss this rare and special situation that we have encountered in our clinic in light of updated information accompanied by literature.
Case
The examination of 30-year-old patient who was admitted to our obstetrics and gynecology emergency clinic with light vaginal bleeding; 11 + 2 weeks of cervical pregnancy was determined. This was the patient's first pregnancy.
There was no abortion procedure, cervical initiative process, operation history or uterine initiative process in patient's background. There was no history of smoking, alcohol, cocaine or drug abuse. There was no inspection of any property in the abdominal and systemic examination. And there were no other complaints except than mild bleeding.
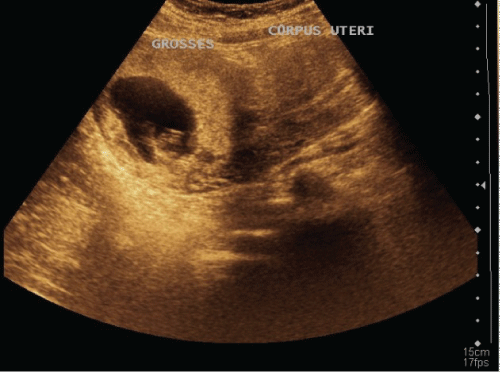
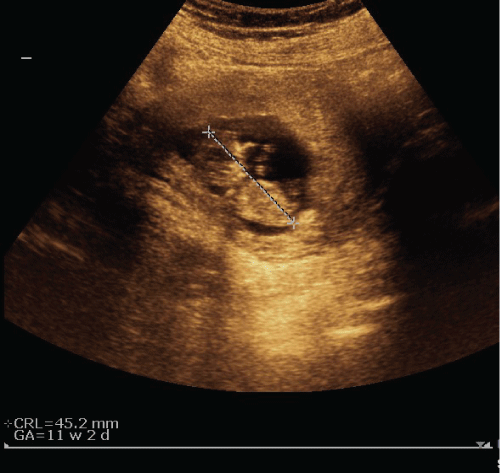
Pregnancy was evaluated by transvaginal ultrasound and abdominal ultrasound. Gestational sac boundaries are natural; an abnormal placental property is not monitored. CRL 11 + 2 weeks, fetal cardiac activity was seen as positive.
Isthmical pregnancy differential diagnosis was made with transvaginal ultrasound. Cervical internal os and external os were seen around the gestational sac. And behind solid cervical tissue was not observed.
Any feature was not seen in laboratory tests including liver enzymes, renal function tests, complete blood count and some other biochemical tests. (WBC 6.0x103/mcL, hemoglobin 11.9g/dl, Hct %35.6 and platelets 189x103/mcL).
Intralesional methotrexate therapy was planned after the patient's routine assays were evaluated. Transabdominal route is preferred for the operation. Abdominal ultrasound-guided methotrexate 25mg up into the fetal heart with 22G needle was given. Then, the needle is passed into the sac and 50mg methotrexate was injected after the liquid was aspirated. Process was terminated uncomplicated.
Patient follow-up was taken in service. Fetal cardiac activity was terminated after the first day of operation. After serial ultrasound follow-up patient was discharged on 3rd day. Patient was invited to the ultrasound control 3 day and 7 day intervals. The first week beta -hCG levels were followed at intervals of 3 days. After that; first month monitored at 5-7 days intervals. It was then followed at 10 days intervals until it was negative. And ultrasound examination was also performed on each control visit. We paid attention to the weekly level of beta -hCG falls by 15%. Gestational sac has collapsed on the 14th day. Full resolution was confirmed by beta -hCG and transvaginal utrasound at the end of the 3rd month (Figure 1-4).
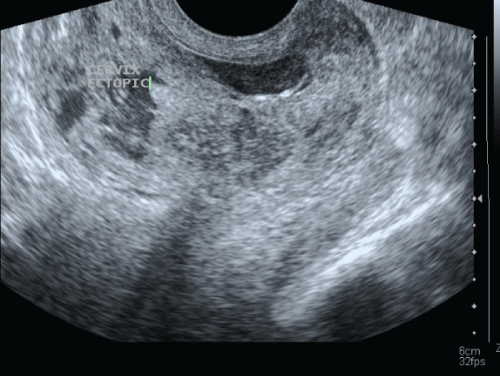
.
Figure 3: Ultrasound examination after 14 days from intralesional methotrexate therapy
View Figure 3
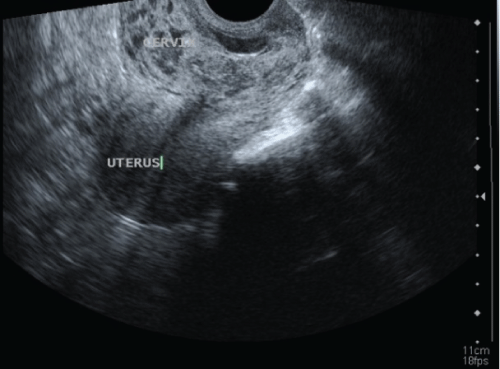
.
Figure 4: Ultrasound examination after 2 months from intralesional methotrexate therapy
View Figure 4
Discussion
In the selected appropriate cases of cervical pregnancy methotrexate and misoprostol can be a good alternative to surgical treatment [1]. Local and systemic injection of a single dose methotrexate or series of methotrexate + leucovorin regimens can be applied. Systemic methotrexate followed by curettage can be a choice. On the other hand, mifepristone and local potassium chloride are other used treatment methods [3].
As we know this can be a life-threatening condition and may require hysterectomy to save the patient's life. And this operation is usually a total hysterectomy. Also it can be done in elective conditions or urgent conditions. But for the treatment of abnormal bleedings; uterine tamponade, Foley's catheter to cervix, vaginal packing, ligation of uterine arteries, embolization of uterine arteries and bilateral hypogastric artery ligation can be made either. Which one we prefer changes to the state of the patient [3].
There is not a strict criterion for the treatment of cervical pregnancy. Therefore, our approach to work is limited to a small number of cases.
Medical therapy, minimally invasive therapies and surgical treatments can be used in appropriate group of patients. Clinical success is indicated by different techniques in many different publications.
Šijanović et al. evaluated a patient with failed intraamniotic methotrexate treatment, added hysteroscopic resection and became successful. As a result, they told that a combination of some methods can be used together for satisfactory results [8].
Duvan et al. have applied the treatment of methotrexate (with single-dose systemic; 50mg dose/square) and misoprostol (vaginal 400μg/day) to patient with 6w+3d pregnancy with an existing fetal heart rate and specified that in selected suitable alive cervical pregnancy cases methotrexate and misoprostol is a good alternative treatment to surgical treatment [1].
Fylstr DL treated 13 cases of cervical pregnancy with suction curettage and balloon tamponade and ended up with successful results [9].
Headley A showed that uterine artery embolization which is less invasive can be made before the surgery in order to avoid hysterectomy in cases where methotrexate is contraindicated [10].
In this case we encountered in our obstetrics and gynecology emergency clinic, we gave priority to this form of treatment rather than systemic methotrexate because of the advanced cervical ectopic pregnancy week and the presence of fetal cardiac activity. We thought it would be, with high risk of bleeding in surgical procedures due to advanced pregnancy week and did intralesional and intracardiac methotrexate applications. We had a successful outcome with this treatment.
Currently the treatment of cervical ectopic pregnancy in the first step is methotrexate therapy and additional methods are needed when it is contraindicated or failed.
Conclusion
Successful treatment with systemic and intralesional methotrexate in the treatment of ectopic pregnancy has been reported in recent years.
As is known, systemic methotrexate treatment success is decreasing and sometimes no answer can be received in particular from 10 weeks of pregnancy and pregnancies with fetal cardiac activity. Therefore in our case, the treatment of intralesional and intracardiac methotrexate is primarily applied and definite success has been achieved.
Although, in each case their own separate and private; we propose intralesional and intracardiac methotrexate therapy can be applied as a form of primary treatment in 10 weeks and above cervical pregnancy with fetal cardiac activity.
References
-
Samal SK, Rathod S (2015) Cervical ectopic pregnancy. J Nat Sci Biol Med 6: 257-260.
-
Río de la Loza Cava L, Moyers Arévalo JA (2012) Ectopic cervical pregnancy, when conservative treatment fails. Case report and literature review. Ginecol Obstet Mex 80: 668-672.
-
Adabi K, Nekuie S, Rezaeei Z, Rahimi-Sharbaf F, Banifatemi S, et al. (2013) Conservative management of cervical ectopic pregnancy: systemic methotrexate followed by curettage. Arch Gynecol Obstet 288: 687-689.
-
Plascencia Moncayo N, Hernández Mde L, Guadarrama Sánchez R, Guerra Becerra L, Salmón Vélez JF, et al. (2008) Cervical pregnancy. Three cases. Ginecol Obstet Mex 76: 744-748.
-
Saeng-anan U, Sreshthaputra O, Sukpan K, Tongsong T (2013) Cervical pregnancy with massive bleeding after treatment with methotrexate. BMJ Case Rep 2013.
-
Hosni MM, Herath RP, Mumtaz R (2014) Diagnostic and therapeutic dilemmas of cervical ectopic pregnancy. Obstet Gynecol Surv 69: 261-276.
-
Rafal RB, Kosovsky PA, Markisz JA (1990) MR appearance of cervical pregnancy. J Comput Assist Tomogr 14: 482-484.
-
Sijanovic S, Vidosavljevic D, Topolovec Z, Milostic-Srb A, Mrcela M (2014) Management of cervical ectopic pregnancy after unsuccesful methotrexate treatment. Iran J Reprod Med 12: 285-288.
-
Fylstra DL (2014) Cervical pregnancy: 13 cases treated with suction curettage and balloon tamponade. Am J Obstet Gynecol 210: 581.
-
Headley A (2014) Management of cervical ectopic pregnancy with uterine artery embolization: a case report. J Reprod Med 59: 425-428.