Journal of Obesity and Weight-loss Medication
Overweight/Obesity and Cardiovascular Risk in the Eastern Morocco
El Bakkay Sellam* and Abdellatif Bour
Department of Biology, University Ibn Tofail, Kenitra, Morocco
*Corresponding author:
El Bakkay Sellam, Department of Biology, Faculty of Sciences, Team Food and Nutrition Transition (ETAN), Biological Testing Laboratory, University Ibn Tofail, BP 133, Kenitra 14000, Morocco, E-mail: Sellam79@gmail.com
J Obes Weight-Loss Medic,
JOWM-1-009, (Volume 1, Issue 2),
Review Article
Received: November 10, 2015: Accepted: December 01, 2015: Published: December 05, 2015
Citation: Sellam EB, Bour A (2015) Overweight/Obesity and Cardiovascular Risk in the Eastern Morocco. J Obes Weight-Loss Medic 1:009
Copyright: © 2015 Sellam EB, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective:The aim of our study was to estimate the prevalence of overweight/obesity and abdominal obesity in the prefecture of Oujda-Angad and to study and assess the risk of chronic diseases including CVD risk.
Material and Methods:Epidemiological Study Transversal on 624 women of childbearing age healthy and not pregnant. The study was conducted in prefecture of Oujda-Angad. Data on socioeconomic and demographic level were collected using a questionnaire. Anthropometric measurements were determined according to the WHO standards. Medical tests were performed in a laboratory accredited private analysis in Oujda. The data were processed using SPSS.
Results:The mean age of the women surveyed was 31.47 ± 7.87 years. Women aged 30-39 years were the most reported (43.10%). The mean of body mass index (BMI) was 27.72 ± 5.91 kg/m2. The BMI values indicate that the prevalence of obesity among women surveyed is 30.61% and the prevalence of overweight was 38.78%. Our results show that the most affected age groups are 30-39 and 40-49. The prevalence of abdominal obesity affects 79.10% of women. Hypertension is the highest risk factor in our sample (33.5% of women), more than 22% of women are hypercholesterolemic, 19.4% are hypertriglyceridemia, and 7.2% are diabetic. Obese women have a high probability of having all CVD risk; among obese women 47% had hypertension (p = 0.002), 33.30% hypercholesterolemia (p = 0.006), 25% diabetes (p = 0.001) and 55.5% hypertriglyceridemia (p = 0.0001).
Conclusion:The risk factors of CVD in our study are very high. The results of our study show that the increase in hypertension, triglycerides, total cholesterol and decrease HDL are strongly associated with obesity (p < 0.05). All these parameters are factors in the development of CVD. According to WHO these factors are considered among the modifiable risk factors (WHO, 2003). The burden of obesity poses a serious public health problem in the region. It is strongly associated with CVD risk. Its prevention requires a multisectoral approach.
Keywords
Overweight, Obesity, Women of childbearing age, Cardiovascular diseases, Oujda, Morocco.
Introduction
Obesity is defined by WHO as abnormal or excessive fat accumulation in the body that presents a risk that can lead to health problems [1]. It is nowadays described as a global epidemic, affecting Developed Countries (PD) such as the Netherlands in Development (PED) [1]. Furthermore, non-communicable diseases (NCDs), mainly cardiovascular diseases (CVD) currently represent a real health scourge in the world. According to WHO, CVD is the leading cause of mortality, almost 30% of total deaths 17.3 million [2], 80% of these deaths occur in middle-income countries. In Morocco, as in most developing countries, CVD were responsible for 30.4% mortality (first cause of mortality) [3].
Numerous epidemiological studies have highlighted that obesity and overweight have serious consequences for health [1]. Obesity, especially when it is massive, has a deleterious effect on multiple metabolic pathways leading the development of many complications, "chronic diseases" such as CVD, type 2 diabetes, high blood pressure (hypertension) stroke, pulmonary embolism, some cancers, osteoarthritis, diseases of the gall bladder and respiratory abnormalities, including sleep apnea [4]. Obesity causes a decrease in life expectancy by 5 to 7 years for women and men regardless of gender and smoking [5]. A low elevation of BMI for example 28 to 29 corresponds to an increased risk of death by 10% [6]. Despite this, few studies have focused on the study of the relationship between obesity and NCDs in Morocco. In this context, we considered in this study, the estimated prevalence of overweight/obesity and abdominal obesity and evaluation of chronic disease risk associated with particular risks of CVD in the population of the prefecture Oujda-Angad.
Materials and Methods
Our study was conducted in the prefecture of Oujda-Angad, the capital of the region of Eastern Morocco, it is located at the northern limit-East of Morocco, is located 12 km from the Algerian border and 60 km from the Mediterranean coast. The area covers 1,714 km2 or 2.06% of the surface area of the East. The province consists of 11 municipalities (urban and three rural 8). The population is about 477,100, which locates in the Urban areas (86%), including 243,334 women. The illiteracy rate in the prefecture level is 30% [7]. The urban area of the prefecture of Oujda is considered a commercial and industrial administrative center.
The data from this study are from a cross-sectional survey, which took place in the prefecture of Oujda-Angad.
The study included 624 women aged 20 to 49 years and healthy non-pregnant, randomly selected. Data on socioeconomic and demographic level were collected using a questionnaire. Several variables were collected to characterize the women surveyed, including age, household size, number of children, occupation, education level, occupation of head of household and dwelling type.
Anthropometric data
Anthropometric measurements were measured according to WHO standards [8]. Weight in kg was determined by weighing a person Seca type and size by a graduated height board 1 mm Seca kind. Measuring the weight and size has allowed calculating BMI (weight in kg compared to height squared). Obesity was defined on the basis of body mass index (BMI) > 30 kg/m2 and overweight for a BMI between 25 and 29.9 kg/m2. Waist and hip circumference were measured using a tape graduated in millimeters, respectively horizontal level of the umbilicus and the horizontal level of the maximum protrusion of the gluteal muscles, and then a waist report hip measurement was calculated. Abdominal obesity was defined a threshold TT > 88 cm or TT/TH > 0.85 (WHO, 2003).
Biological Data
The blood pressure (BP) was measured using a digital sphygmomanometer in women sitting position, after a rest 20 minutes. Average two spaced steps 20 minutes retained. Hypertension is defined using the World Health Organization thresholds/International Society of Hypertension (WHO/ISH): systolic BP ≥ 140 mmHg and/or diastolic BP ≥ 90 mmHg.
Diabetes and fasting hyperglycemia were determined from glycaemia Fasting using the Organization's thresholds World Health (WHO) (WHO, 2003): ≥ 1.26 g/L for diabetes, and > 1.1 to 1.25 g/L for hyperglycemia fasting (glucose dosage per method oxidase).
Total cholesterol was defined as any value of cholesterol Total (TB), determined by the method the enzyme cholesterol oxidase, exceeding 2 g/L (5.16 mmol/L). There HDL-C fraction was determined by precipitation with phosphotungstic acid and MgCl2. The concentration of LDL-C was calculated using the formula Friedewald.
Hypertriglyceridemia was defined any value as triglycerides (assay by an enzymatic method) > 1.5 g/L. Dyslipidemia refers to a total cholesterol > 2.0 g/L and/or triglyceride levels > 1.5 g/L. The hypoHDLemie is retained as defined IDF: HDL-C < 0.50 g/L for women.
The metabolic syndrome is determined following the definition of the IDF (rate high triglycerides, low HDL-C, hypertension, fasting hyperglycemia, abdominal obesity).
The study data were entered and analyzed using SPSS Version20 for Windows. The results are expressed as mean standard deviation or percentage. The correlations between BMI, and various sociodemographic variables were assessed by the Spearmantest. The chi-square test is used to compare the two percentages. The significance level was set at 0.05.
Ethics
The study was approved and conducted under the responsibility of the ethics committee of the University of Ibn Tofail (Kenitra) and had permission from the regional legal representing of the Moroccan health ministry (Oujda). Finally, an information text, prepared in Arabic and French, was distributed to eligible women and free and informed consent has been obtained on a form also prepared in Arabic and French.
The study data were entered and analyzed on SPSS software version 20 for Windows. The results are expressed as mean ± standard deviation, or as a percentage. Correlations are determined by the Spearman test. The Chi-square test is used to compare two percentages, while the comparison averages was made by the test Student t. The level of significance was set at 0.05.
Results
Anthropometric data
The average age of women was 31.74 ± 7.15 years (Table 1). According to table 2 the age of 20 years to 29 years the most represented (38.7%), more than 30% of women are illiterate, most are housewives (96.8%) and majority of women are married (96%). For married women about 51.6% are mothers of children under 2.71% of women living in households with more than 5 persons (Table 2).
![]()
Table 1: Parameters anthropometric indicators of nutritional status of women and the biological characteristics of women aged 20 to 49 in the prefecture of Oujda-Angad.
View Table 1
![]()
Table 2: Socio-demographic characteristics of women
View Table 2
The body mass index (BMI) was 27.75 kg/m2 ± 5.90 kg/m2, with a minimum of 16.71 kg/m2 and a maximum of 45.82 kg/m2. The average size is 1.61 ± 0.06 m with an average weight of 72.87 ± 15.32 kg (Table 1). The BMI values indicate that the prevalence of obesity and overweight among women surveyed are respectively 30.61 and 38%. The results also show that the BMI increases with the number of pregnancy (p < 0.001) and the number of children (p < 0.001). The level of education is not involved in obesity but we note that the prevalence of obesity decreases with the level of education, 37% of women are illiterate obese. We also note that 88% of working women is obese.
Biological data
Mean values for systolic BP and diastolic are 120.67 ± 17.1 mmHg and 74.2 ± 10.56 mmHg, respectively (Table1). Prevalence Total of hypertension is 35%. Hypertension was not associated at studies (Table 3), because the majority of women surveyed are illiterate or with an educational level primary. Furthermore, we observed that the prevalence of hypertension increases with age (Figure 1), and 47% obese women with hypertension (p = 0.01) (Table 3). The risk of arterial hypertension in obese is multiplied by 2 (OR = 2.7 [0.95-7.61]). Hypertension is associated to the abdominal obesity (p = 0.02) (Figure 1). On the other hand there is the strong association between hypertension and cholesterol total triglycerides, HDL-C and LDL-C.
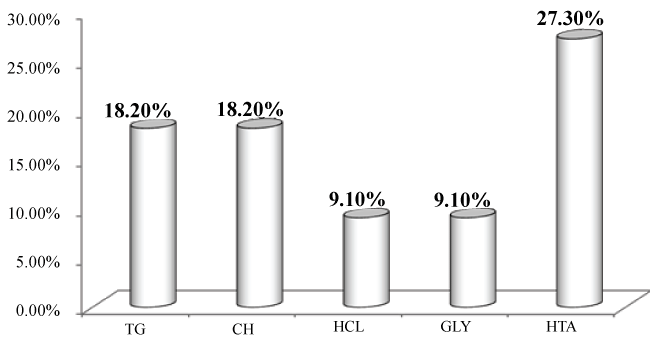
.
Figure 1: Distribution of risk factors in abdominal obesity of women surveyed. (TG: Triglyceride; CH: Cholesterol; GLY: Young blood glucose; HTA: Arterial hypertension)
View Figure 1
![]()
Table 3: Correlation between sociodemographic factors. BMI and risk factors of CVD.
View Table 3
The values of fasting glucose range from 0.96 ± 0.29 g/L, with a prevalence of hyperglycemia 7.2%. Hyperglycemia is associated with age (p = 0.03). Hyperglycemia increases with BMI (OR = 1.5 [1.05-1.57]; p = 0.001) it affects 25% of the obese. However, no association was found between hyperglycemia and sociodemographic factors (p > 0.05) (Table 3).
Hypercholesterolemia increases significantly with age (p = 0.01), it affects 37% of women aged 40-49, 18.8% of 30-39 and 8.33% of 20-29 ans. Distribution by BMI shows that high cholesterol increases significantly with obesity, 32% of obese women with hypercholesterolemia (OR = 3.1 [1.092-9.18] (p = 0.02)). Correlations with sociodemographic factors shows that high cholesterol is associated with the marital status of women (p = 0.04) (Table 3).
The increase in triglycerides is associated with age (p = 0.005) (Table 3), the age group of 40-49 years is the most affected by hypertriglyceridemia (38%), against 19% of 30-39 years (p = 0.003), hypertriglyceridemia is associated with BMI (OR = 2; p = 0.001). No association was found between hypertriglyceridemia and sociodemographic factors (Table 3).
The average values of HDL and LDL were respectively 0.48 g/L ± 0.11 g/L and 0.98 g/L ± 0.26 g/L, the rate of LDL in the sample is normal in all women. However, low HDL levels are associated with obesity, as 15% have lowered levels of HDL (p < 0.05). The relationship between anthropometric indices in women and risk factors is presented in table 3.
The metabolic syndrome (MS) affects 35% of women surveyed as defined in the IDF. The SM increases with age, it affects 25% of women between 20 and 29, and 37.5% of women aged between 40 and 49. The high prevalence of MS is due to the incidence of obesity abdominal and hypertriglyceridemia. Obesity/metabolic syndrome risk is multiplied by 3.6 (OR= 3.6 [1.34-9.6]).
Obese women have a high probability of having all the risk of cardiovascular diseases among obese women with hypertension 47% (p = 0.002), 33.5% had hypercholesterolemia (p = 0.02), 25% hyperglycemia (p = 0.001), 55% hypertriglyceridemia (p = 0.001) (Figure 2). Women with abdominal obesity (TT > 88 cm) were more likely to have low HDL (p = 0.03) and a high prevalence of hypertriglyceridemia and hypercholesterolemia (Figure 1).
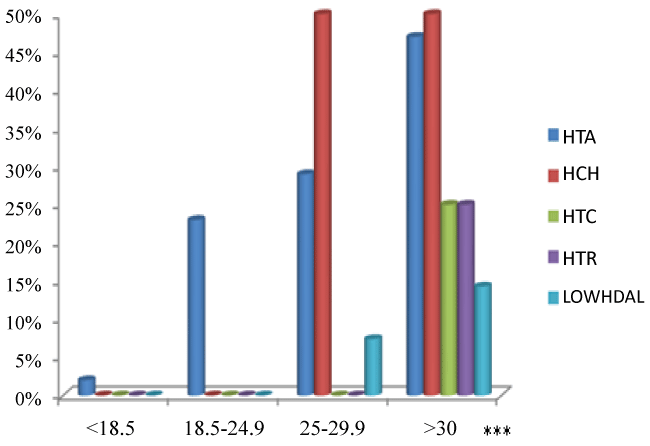
.
Figure 2: Prevalence of CVD risk factors by BMI
(HTA: arterial hypertension; HCH: hypercholesterolemia; HTG: hyperglycemia; HTR: hypertriglyceridemic)
View Figure 2
Discussion
The objective of this study was to evaluate the risk of chronic diseases associated with obesity including risks of CVD, in a context where the nutritional transition that is underway in Morocco. The results of our survey, which took place in the Eastern region, revealed a high prevalence of obesity and overweight and abdominal obesity in women in our sample, the values obtained are respectively: 30.61%; 38.78% and 79.10%.
Our results are similar to those of other regions of Morocco such as Rabat Sale [9], where the prevalence of obesity was 32.4%. These figures are higher than national data published by the HCP in 2013 (26%) [10], which confirms that obesity is on the rise in Morocco. Moreover, one can notice great differences in some areas of the country, with lower figures as in the High Atlas in Marrakech (13.3%) [11]; or with larger numbers reflecting a wide abundance of obesity as it is found in the north east of Casablanca [12] with a prevalence of 43.8%. These alarming rates of obesity show that this epidemic has become a scourge of health in our study area like all regions of Morocco.
The results of our survey showed a high prevalence of hypertension, which is 35%, this value is slightly above the last digit national 33.6% [13], which shows that hypertension is currently a real health problem Morocco. We found that the prevalence of hypertension was not associated with age and is more pronounced among women aged 40 to 49 years. The results of the WHO MONICA project and the NHANES III study showed that the prevalence of hypertension increases progressively with age, however, the study found that the risk of developing hypertension is multiplied by 5.6 among overweight people ages 20 to 44 years and two for person aged 44 to 74 years [14]. Our results show that hypertension is associated with increased BMI (p = 0.001) and among obese women, 47% were hypertensive.
The positive association between obesity and hypertension is consistent with other studies [15], Hajjar and his teams have shown that increasing BMI is responsible for 30% of the prevalence of hypertension [16]. The study of NHANES II confirmed that hypertension is three times higher in overweight people than those of normal weight [17].
The increase of hypertension in obese women is similar in all age groups in our sample, with a slightly higher prevalence among obese women aged 30 to 39 without statistical significance. The risk that obese develop hypertension was similar in women and men in all age groups regardless of their ethnic origin [1]. Therefore, the increase in body weight during early adult life can be more dangerous to health.
Moreover, in the study of Framingham, obese women are more likely to develop hypertension: 2 for BMI values between 24.0 and 29 kg/m2 and 6 times higher BMI 31.0 kg/m2. The risk estimates from the Framingham suggest that about 78% of cases of hypertension in men and 65% among women can be directly attributed to obesity. Thus, a weight gain of 5 kg was associated with a 30% increase in the incidence of hypertension, while the loss of weight reduces the risk of high blood pressure [18]. Weight loss of 5 kg reduced systolic blood pressure and diastolic pressure 4.4 mmHg of 3.6 mmHg [19]. In the same sense, the INTERSALT study was conducted in more than 10,000 people in 52 centers and 32 countries around the world has found a significant relationship clearly established between increased blood pressure and increased BMI. The increase in BMI of one unit was associated with an increase of 0.91 mmHg for men and 0.72 mmHg for women.
In our sample the prevalence of hypertriglyceridemia is 18.6%. Our results are higher compared to other studies in Morocco 11.1% in Smara [20] and 3.3% in Rabat [21]. Hypertriglyceridemia increases with age (p = 0.01) it affects 50% of women 40 to 49 years. The prevalence of hypertriglyceridemia by age and BMI shows that overweight women have a higher risk of hypertriglyceridemic in all age groups.
In our study the BMI is associated with an elevation of plasma triglycerides (p = 0.004). Thus, various studies have shown that hypertriglyceridemia is significantly high in obese [22]. The NHANES II study in America showed that triglyceride levels increase with increasing BMI among women and men of all ethnicities [23].
On the other hand we found that 22.9% of women have high cholesterol, this result is similar to that of the study in Rabat-Sale (23.2%) [21]. Also, which shows that excess weight is associated with increased total cholesterol levels, 32% of obese women with hypercholesterolemia. In addition, several studies have shown that the increase in BMI was associated with higher total cholesterol [24].
He showed a strong correlation between body weight and the rate of total cholesterol. The Framingham study [25] demonstrated that an increase of 10% by weight is associated with an increase of 0.3 mmol/l of blood cholesterol. The relative risk of high cholesterol in obese adults is 1.5 times compared to the adult NHANES II [17].
Obesity also appears to be associated with a decrease in HDL cholesterol. Indeed, it turned out that an increase in BMI of a unit is accompanied by a decrease in HDL cholesterol of about 3 mg/dL [26]. The NHANES II study found that HDL cholesterol levels are inversely associated with BMI in all age groups. In this sense, the results of our study have confirmed this negative correlation between BMI and HDL cholesterol levels.
The increase in weight is also accompanied by an increase in LDL. Our results show that LDL increases with BMI without statistical significance. In a previous study, a one-unit increase in BMI has caused an increase in LDL of 5.5 mg/dL [25]. In our study the rate of LDL increases with body weight (p = 0.001).
The results show that hyperglycemia affects 7.5% while 6.2% have type 2 diabetes Our results show that hyperglycemia is associated positively with increasing BMI (p = 0.03), 25% of obese women have hyperglycemia. Similarly, the NHANES data show a direct association between BMI and the prevalence of type II diabetes. Ziegler and his colleagues in 1998, the incidence of type 2 diabetes is three times higher in obese subjects [27].
Obese women are more likely to develop type 2 diabetes during follow-up of 14.5 times for BMI values between 24.0 to 29 kg/m2, between 31.0 to 40 times 34 kg/m2 and 93 times for BMI greater than 35.0 kg/m2, compared to the group with a BMI less than 22.0 kg/m2 [28]. A study in 50 women with diabetes are not known obese adults revealed a type 2 diabetes in 12% of cases and glucose intolerance in 26% [29]. Slein and colleagues in 2004 stressed that the risk of type 2 diabetes is multiplied by 2.9 in obese aged 20 to 75 years [30].
The association between obesity and CVD has been the subject of several studies. Since 1983 the analysis of Framingham, after 26 years of follow up, concluded that obesity was a significant independent predictor of cardiovascular disease after adjustment for risk factors. In 2002, Wilson and colleagues have shown that the risk of CVD was higher among overweight men from 1.07 to 1.44 and from 1.12 to 1.69 for overweight women, after adjusting for the age, smoking, hypertension, and diabetes type II [29]. The study Manson and his colleagues showed that the risk of death from CVD was higher among overweight women (IMC ≥ 27) compared to women of normal height (BMI < 19), among obese women (BMI ≥ 32) the risk of death from CVD was 4.1 [6]. This result is confirmed by the study of the American Cancer Society I, involving 324,135 people, who found that being overweight increases the risk of death from CVD for healthy people. CVD mortality risk is strongly associated with BMI in all age groups even at a young age [31] attributed to CVD mortality was dependent on the age obese. Women aged 30 to 54 with a high BMI had an increased risk of death from CVD.
The Nurses Health study involving women aged 30-55 years, ischemic stroke was 75% higher among women with a BMI > 27 and 137% higher in those with a BMI > 32, compared to women who had a BMI < 21 [32].
Although obesity is associated with a set of DTM, some authors have shown that abdominal obesity that is easily measured (waist circumference) is the most important factor in the development of atherosclerosis disease, diabetes type 2 [33], and CVD. The study by Suk and his team showed that the risk of ischemic cerebrovascular accidents is three times higher among those with a waist report/tower top hip 88 cm [34]. It is well known that the risk of cardiovascular disease incidence and mortality increases with the degree of abdominal obesity. It is shown that people with abdominal obesity often have more metabolic disorders and are therefore more likely to develop diabetes than those who do not have central obesity [23]. Measurement of abdominal fat in CT studies have shown that subjects with abdominal obesity, have a more atherogenic metabolic profile and diabetogenic compared with those who have exclusive excess subcutaneous fat [35]. A recent study has mounted that abdominal obesity is associated with the metabolic syndrome, has increased triglycerides, hyperglycemia and serum uric acid [28].
Insulin resistance, the release of free fatty acids into the circulation and adipokines such as leptin, interleukin 6, angiotensin II, adiponectin, resistin, TNF-α, markers of inflammation are explanations that link obesity to type 2 diabetes, hypertension and coronary heart disease.
The results of our study the Moroccan population is highly exposed to risk factors of CVD, which are positively associated with obesity. In view of these changes in health status, the Moroccan population appears well into a new era, that of the epidemiological transition.
Among the main factors responsible for obesity in the world, the nutrition transition is facilitated by globalization, industrialization and urbanization. The nutrition transition is underway in Morocco is characterized by changes in eating habits and the transition from a traditional diet high in fiber and low in fat and sugar, a diet rich in animal products, fats, salt and sugar, and low in fiber [36]. The profound lifestyle changes and habits of the Moroccan population are characterized firstly by densification energy from the diet, and the other by a sedentary lifestyle and decreased physical activity. This energy imbalance between calories consumed and expended, is a key element for the development of obesity and its attendant associated diseases.
The role of dietary factors in the genesis of obesity is important and it is granted by the literature [2]. According to the HCP, the eating habits of Moroccan evolving towards a Western way. The average dietary energy supply increased from 2202 kcal/person/day in 1970 to 3,052 in 2007 [36].
Conclusion
The results reported in this work show a worrying prevalence of obesity and overweight, and his close relationship with cardiovascular disease in the Moroccan population. The burden of obesity is a major public health problem in the region. Prevention requires a multifactorial approach to help women maintain their ideal and healthy weight.
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
Bour abdellatif is the project leader and participated in all stages of this work. Sellam elbakkay conducted the field work, the statistical analysis, writing the manuscript, and has reviewed all the statistical analysis of the study. All authors participated in the discussion of the results and reviewing the manuscript, and approved the final manuscript.
Acknowledgement
The authors wish to thank to Mr. Regional Director of Health, the Delegate of the delegation of the Health of Oujda-Angad Province and all the staff of the health centers that have contributed directly or indirectly to this study is for their assistance in collecting data for this study. We also thank all the members of Team Food and Nutrition Transition (ETAN), laboratory tests Organics, Department of Biology, Faculty of Science, Ibn Tofail University Morocco.
References
-
OMS (2003) Obesite: prevention et prise en charge de l'epidemie mondiale. Serie de Rapports techniques, n° 894, Geneve.
-
OMS (2013) Maladies non transmissibles. Aide-memoire N°355 Mars 2013.
-
Ministere de la Sante (2011) Direction de la Planification et des Ressources Financieres. Enquete Nationale sur la Population et la Sante Familiale.
-
Poirier P, Lemieux I, Mauriege P, Dewailly E, Blanchet C, et al. (2005) Impact of waist circumference on the relationship between blood pressure and insulin: the Quebec Health Survey. Hypertension 45: 363-367.
-
Peeters A, Barendregt JJ, Willekens F, Mackenbach JP, Al Mamun A, et al. (2003) Obesity in adulthood and its consequences for life expectancy: a life-table analysis. Ann Intern Med 138: 24-32.
-
Manson JE, Willett WC, Stampfer MJ, Colditz GA, Hunter DJ, et al. (1995) Body weight and mortality among women. N Engl J Med 333: 677-685.
-
Direction de la statistique (2005). Recensement General de l'Habitat et de la Population 2004. Haut Commissariat au Plan.
-
OMS (1995) Rapport d'un comite d'experts, Utilisation et interpretation de l'anthropometrie, Organisation Mondiale de la sante, Geneve.
-
El Hsaini H, Agnes G, Jacques B, Aguenaou H, Edwige L, et al. (2013) Coexistence de surpoids/obesite et d'anemie chez les femmes de Rabat-Sale. Biomatec Journal, 8: 57-67.
-
Haut Commissariat au Plan (2011) Direction de la statistique. Enquete Nationale Anthropometrique. Principaux resultats. Haut Commissariat au Plan.
-
Lahmam A, Baali A, Hilali MK, Cherkaoui M, Chapuis-Lucciani N, et al. (2008) Obesity, overweight and body-weight perception in a High Atlas Moroccan population. Obes Rev 9: 93-99.
-
Jafri A, Taki H, Belhouari A, Benajiba N, Bour A, et al. (2009) Investigation on the anthropometric status of the north-east Casablanca (Morocco) population. Ann Nutr Metab 55: 294-294.
-
Tazi MA, Abir-Khalil S, Chaouki N, Cherqaoui S, Lahmouz F, et al. (2003) Prevalence of the main cardiovascular risk factors in Morocco: results of a National Survey, 2000. J Hypertens 21: 897-903.
-
Yusuf S, Hawken S, Ounpuu S, Dans T, Avezum A, et al. (2004) Effect of potentially modifiable risk factors associated with myocardial infarction in 52 countries (the INTERHEART study): case-control study. Lancet 364: 937-952.
-
Khan SB, Noor L, Hafiz-ur-Rehman, Hameedullah, Hafeezullah M, et al. (2010) Prevalence of hypertension among obese and non-obese patients with coronary artery disease. J Ayub Med Coll Abbottabad 22.
-
Hajjar I, Kotchen TA (2003) Trends in prevalence, awareness, treatment and control of hypertension in the United States, 1988-2000. JAMA 290: 199-206.
-
Van Itallie TB (1985) Health implications of overweight and obesity in the United States. Ann Intern Med 103: 983-988.
-
Vasan RS, Larson MG, Leip EP, Kannel WB, Levy D (2001) Assessment of frequency of progression to hypertension in non-hypertensive participants in the Framingham Heart Study: a cohort study. Lancet 358: 1682-1686.
-
Cook NR, Obarzanek E, Cutler JA, Buring JE, Rexrode KM, et al. (2009) Joint effects of sodium and potassium intake on subsequent cardiovascular disease: the Trials of Hypertension Prevention follow-up study. Arch Intern Med 169: 32-40.
-
Rguibi M, Belahsen R (2004) Metabolic syndrome among Moroccan Sahraoui adult Women. Am J Hum Biol 16: 598-601.
-
Ayyat O, Gartner A, Ati JE, Mokhtar N, Aguenaou H, et al. (2013) Activite physique habituelle des femmes de Rabat-Sale et relation avec leurs caracteristiques sociodemographiques. Biomatec J 8: 4556.
-
Pi-Sunyer FX (2002) The obesity epidemic: pathophysiology and consequences of obesity. Obes Res 10 Suppl 2: 97S-104S.
-
Folsom AR, Burke GL, Ballew C, Jacobs DR Jr, Haskell WL, et al. (1989) Relation of body fatness and its distribution to cardiovascular risk factors in young blacks and whites. The role of insulin. Am J Epidemiol 130: 911-924.
-
Owen CG, Whincup PH, Odoki K, Gilg JA, Cook DG (2003) Birth weight and blood cholesterol level: a study in adolescents and systematic review. Pediatrics 111: 1081-1089.
-
Messerli FH, Nunez BD, Ventura HO, Snyder DW (1987) Overweight and sudden death. Increased ventricular ectopy in cardiopathy of obesity. Arch Intern Med 147: 1725-1728.
-
Anderson KM, Wilson PW, Garrison RJ, Castelli WP (1987) Longitudinal and secular trends in lipoprotein cholesterol measurements in a general population sample. The Framingham Offspring Study. Atherosclerosis 68: 59-66.
-
Ziegler O, Debry G (1998) Epidemiologie des obesites de l'adulte. EMC. Endocrinologie-Nutrition 10-506-B-20: 7.
-
Maksimovic M, Vlajinac H, Radak D, Marinkovic J, Maksimovic J, et al. (2013) Relationship between Abdominal Obesity and Other Cardiovascular Risk Factors: Cross Sectional Study of Patients with Symptomatic Carotid Disease Srp Arh Celok Lek. 141: 460-465.
-
Wilson PW, D'Agostino RB, Sullivan L, Parise H, Kannel WB (2002) Overweight and obesity as determinants of cardiovascular risk: the Framingham experience. Arch Intern Med 162: 1867-1872.
-
Colditz GA, Willett WC, Stampfer MJ, Manson JE, Hennekens CH, et al. (1990) Weight as a risk factor for clinical diabetes in women. Am J Epidemiol 132: 501-513.
-
Stevens J, Cai J, Pamuk ER, Williamson DF, Thun MJ, et al. (1998) The effect of age on the association between body-mass index and mortality. N Engl J Med 338: 1-7.
-
Rexrode KM, Carey VJ, Hennekens CH, Walters EE, Colditz GA, et al. (1998) Abdominal adiposity and coronary heart disease in women. JAMA 280: 1843-1848.
-
Canoy D, Boekholdt SM, Wareham N, Luben R, Welch A, et al. (2007). Body fat distribution and risk of coronary heart disease in men and women in the European Prospective Investigation Into Cancer and Nutrition in Norfolk cohort: a population-based prospective study. Circulation 116: 2933-2943.
-
Suk SH, Sacco RL, Boden-Albala B, Cheun JF, Pittman JG, et al. (2003) Abdominal obesity and risk of ischemic stroke: the Northern Manhattan Stroke Study. Stroke 34: 1586-1592.
-
Despres JP, Lemieux I, Bergeron J, Pibarot P, Mathieu P, et al. (2008) Abdominal obesity and the metabolic syndrome: contribution to global cardiometabolic risk. Arterioscler Thromb Vasc Biol 28: 1039-1049.
-
Haut Commissariat au Plan (2008) Direction de la statistique. Enquete nationale sur le niveau de vie des menages 2006-2007.





