Journal of Musculoskeletal Disorders and Treatment
Treatment of Sports-Related Injured Knee with Incidental Extra-articular Giant Cell Tumor of the Pes Anserinus Tendon Sheath
Sungwook Choi1, Younghee Maeng2, Kyungryeol Lee3 and Donghee Kim1*
1Department of Orthopedic Surgery, Jeju national university, South Korea
2Department of Pathology, Jeju national university, South Korea
3Department of Radiology, Jeju national university, South Korea
*Corresponding author: Donghee Kim, Department of Orthopaedic Surgery, Jeju National University Hospital 1753-3, Ara-1 dong, Jeju-si, Jeju Self-Governing Province, South Korea (690-716), Tel: +82-064-717-1690, Fax: +82-064-717-1131, Mobile phone: +82-010-6660-3041, E-mail: kikiehdgml@hanmail.net
J Musculoskelet Disord Treat, JMDT-3-031, (Volume 3, Issue 1), Case Report
Received: August 24, 2016 | Accepted: February 10, 2017 | Published: February 13, 2017
Citation: Choi S, Maeng Y, Lee K, Kim D (2017) Treatment of Sports-Related Injured Knee with Incidental Extra-articular Giant Cell Tumor of the Pes Anserinus Tendon Sheath. J Musculoskelet Disord Treat 3:031.
Copyright: © 2017 Choi S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report a case of a 21-year-old male with knee injury with a giant cell tumor of the tendon sheath resulting in a pes anserinus. As seen in this case, in a sports-related knee injury with an associated giant cell tumor, an initial treatment of the mass was performed first. After the confirmation of non-recurrence after 1 year follow up, the treatment of the sports related injury was followed. In any type of knee injury associated with giant cell tumor, initial treatment of the mass followed by treatment of the injury in a step by step manner showed us excellent outcome.
Keywords
Knee, Giant cell tumor of tendon sheath, Extra-Articular giant cell tumor
Introduction
The first description of "Pigmented villonodular synovitis (PVNS)" was presented by Jaffe, et al. [1]. PVNS which is composed of benign growths of polygonal histocyte-like cells associated with multinucleated giant cells is usually subgrouped according to its site (intra- versus extra-articular) and growth pattern (nodular or diffuse) [2]. The subgroups of pigmented villonodular synovitis differ according to their clinical characteristics and biological behaviors. Clinically, PVNS is a proliferative condition that affects synovial joints, in either a focal or a diffuse manner. In contrast, a giant cell tumor of the tendon sheath (GCTTS) affects the tendon sheath [3]. The incidence rate of GCTTS is estimated at 9.2 cases per 1 million people [4]. Only 12 reports of extra-articular giant cell tumor of the pes anserinus have been published sofar [5]. The extra-articular form of the disease commonly presents as a solitary mass with or without symptoms. Most lesions related to GCTTS develop in the small joints, particularly in the fingers, and GCTTS is known to be the second most common soft tissue tumor of the hand, after ganglion tumors [2,6]. It may be overlooked in a rare case which there exists mass within a sports-related injured knee. We report a rare case of sports-related injured knee with an incidental extra-articular giant cell tumor arising from the pes anserinus tendon sheath.
Case Presentation
A 21-year-old male presented with moderate pain in his left knee joint. He injured his left knee in a basketball match two weeks prior to presentation. He complained of instability when stepping down stairs. Physical examination revealed positive results for the anterior drawer test, Lachman's test and McMurray's test. Preoperative magnetic resonance imaging (MRI) showed a complete anterior cruciate ligament (ACL) tear, medial meniscus (MM) tear, and a mass-like lesion suggesting a hematoma or GCTTS on the anteromedial side of the left proximal tibia. The mass was enhanced heterogeneously in T2-weighted images (Figure 1). He had not suffered any symptoms related to the mass. In order to harvest from the pes anserinus for an autologous graft, exploration was performed. The mass was fixed to the insertion site of the pes anserinus-conjoined tendon. The mass was harvested from the tendon sheath of the semitendinosus and gracilis tendons for a frozen biopsy (Figure 2). The frozen section revealed the presence of a brown-yellowish multinodular mass. Microscopically, the tumor was moderately cellular and composed of sheets of round or polygonal cells admixed with collagen bundles. Scattered multinucleated giant cells and regional collections of xanthoma cells were observed. Upon the pathologic confirmation of GCT, a marginal excision of the mass was performed, and the semitendinosus and gracilis tendons were sacrificed due to the direct involvement of the lesion (Figure 2). Though the knee joint was not involved, ACL reconstruction was not performed because of the risk of recurrence of tumor. However, the MM tear was repaired because an unrepaired MM tear with weight bearing leads to aggravation of the tear and delay rehabilitation. There was no evidence of recurrence on MRI findings, and the patient received an operation for ACL reconstruction 12 months postoperatively (Figure 1).The patient is currently in remission without functional deficit after 2 years of follow up. The Lysholm knee scoring scale improved from 68 to 95, 2 years postoperatively.
.
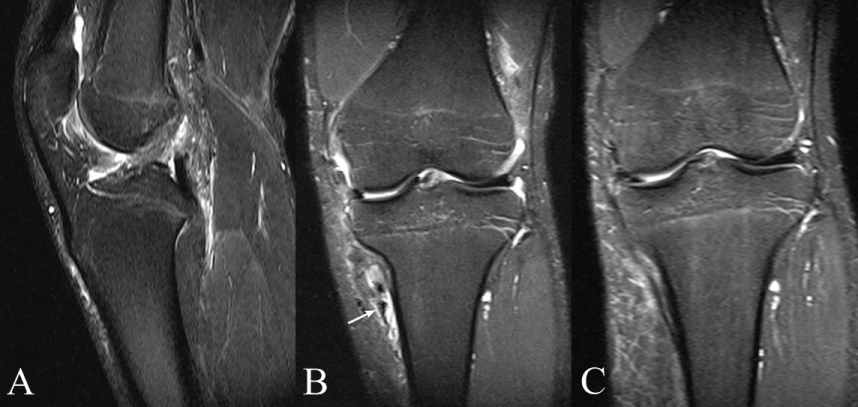
Figure 1: A) ACL tear. A T2- weighted image revealing increased signal intensity in the ACL, indicating an ACL tear; B) MM tear. A T2-weighted coronal image showing a bucket-handle tear of the MM. The torn segment is displaced into medial aspect. A lesion (arrow) in the medial region of the proximal tibia; C) Images of a follow-up MRI of the left knee, 12 months after surgery. There was no evidence of recurrence.
View Figure 1
.
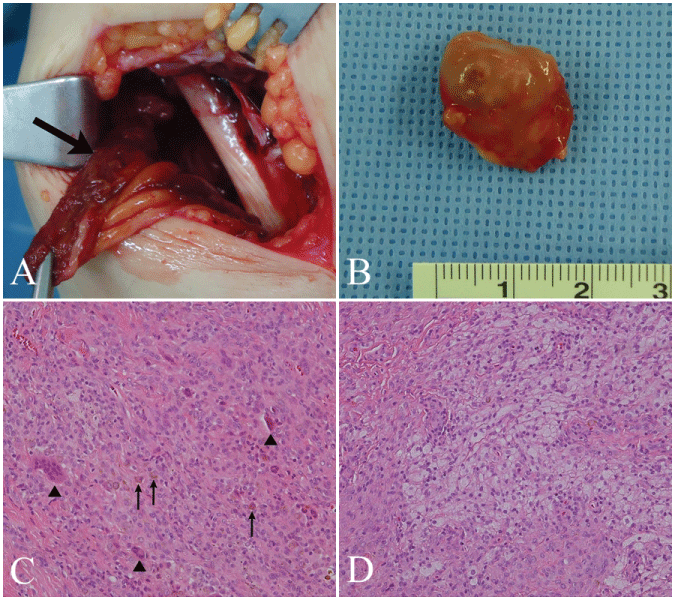
Figure 2: A) Intraoperative picture of a mass (arrow) in the anteromedial side of the proximal tibia; B) A macroscopic picture of the mass (1.8 × 2.0 × 2.2 cm) after excision of the tumor. The gross specimen showing a brownish-yellowish pigmented and multinodular mass; C) Microphotograph showing sheets of round or polygonal cells and scattered multinucleated giant cells (arrow heads) admixed with hemosiderin pigment (arrows) (hematoxylin and eosin stain, X200); D) Geographic collections of xanthoma cells (hematoxylin and eosin stain, X200).
View Figure 2
Discussion
In GCTTS, extra-articular lesions without articular communication are extremely rare. Tumors around joints often get mistaken to sports related injury and hence misdiagnosis often takes place. Statistics about sports-related injury around the knee with young athletes suggest annual rate of 0.3 per 100 individuals; however, tumors occurring on knee often appear at the same age group thus they may be misinterpreted as sports related injury or common pain [7]. There is no known cause of GCTTS, while prognostic factors and optimal treatments are also lacking. The lesion presents as a firm, slow-growing, non-tender mass, without recent trauma or neurologic symptoms. MRI is currently the modality of choice for the diagnosis of GCTTS. The MR imaging features of GCTTS reflect the histological characteristics which typically include a low to intermediate signal intensity on T1- and T2-weighted images due to the presence of hemosiderin. The lesion is also demarcated by a low-signal intensity capsule as a result of fibrosis or hemosiderin deposition [7].Complete excision of the tumor including the affected tissue is the treatment of choice to prevent recurrence [4]. The incidence of local recurrence is high, ranging from 4 to 45% [8]. Recurrence of GCT is assumed to be due to incomplete excision of the tumor or satellite lesion [9]. Once, radiotherapy had been recommended to prevent recurrence after excision [10]. But recent studies regarding radiation therapy delineates questionable efficiency due to possibility of serious toxicity such as skin necrosis or a drainage sinus. At the same time, the necessity of radiation therapy keeps decreasing while new targeted medical therapies are being introduced [11].
Diagnosis of sports-related injured knee with incidental GCTTS requires specific attention to several important features. First, it should be noted that an awareness on GCTTS that may occasionally occur in the knee allows for earlier diagnosis in patients with sports-related knee injuries. This case was difficult to make a precise diagnosis due to the accompanying traumatic injuries, including ACL rupture and meniscus tear. Second, MRI results and plain radiographs must be evaluated thoroughly to accurately assess the mass. If abnormal findings are present, such as bony involvement, soft tissue swelling, synovial sarcoma, lipoma, or ganglion, GCTTS should be differently diagnosed.
In a sports-related knee injury associated with GCTTS, an initial marginal excision of the mass was performed first. After the confirmation of non-recurrence within a year since the initial surgery was applied, the treatment of the sports related injury was followed. In any type of knee injury associated with GCTTS, initial treatment of the mass followed by treatment of the injury in a step by step manner showed us excellent outcome.
Acknowledgements
This research was supported by the 2015 scientific promotion program funded by Jeju National University Grant.
References
-
Jaffe HL LL, Sutro CJ (1941) Pigmented villonodular synovitis,bursitis and tenosynovitis. A discussion of the synovial and bursal equivalents of the tenosynovial lesion commonly denoted as xanthoma, xanthogranuloma, giant cell tumor or myeloplaxoma of the tendon sheath, with some consideration of this tendon sheath lesion itself. Arch Pathol 31: 73.
-
Ushijima M, Hashimoto H, Tsuneyoshi M, Enjoji M (1986) Giant cell tumor of the tendon sheath (nodular tenosynovitis). A study of 207 cases to compare the large joint group with the common digit group. Cancer 57: 875-884.
-
Addicott BT, Jose J, Kaplan LD, Clifford PD (2009) Imaging series. Pigmented villonodular synovitis. Am j Orthop 38: 635-636.
-
Murphey MD, Rhee JH, Lewis RB, Fanburg-Smith JC, Flemming DJ, et al. (2008) Pigmented villonodular synovitis: radiologic-pathologic correlation. Radiographics 28: 1493-1518.
-
Zhao H, Maheshwari AV, Kumar D, Malawer MM (2011) Giant cell tumor of the pes anserine bursa (extra-articular pigmented villonodular bursitis): a case report and review of the literature. Case reports in medicine 2011.
-
Granowitz SP, Mankin HJ (1967) Localized pigmented villonodular synovitis of the knee. Report of five cases. J Bone Joint Surg Am 49: 122-128.
-
Al-Nakshabandi NA, Ryan AG, Choudur H, Torreggiani W, Nicoloau S, et al. (2004) Pigmented villonodular synovitis. Clin radiol 59: 414-420.
-
Ho CY, Maleki Z (2012) Giant cell tumor of tendon sheath: cytomorphologic and radiologic findings in 41 patients. Diagn cytopathol 40: 94-98.
-
Williams J, Hodari A, Janevski P, Siddiqui A (2010) Recurrence of giant cell tumors in the hand: a prospective study. J Hand Surg Am 35: 451-456.
-
Friedman M, Schwartz EE (1957) Irradiation therapy of pigmented villonodular synovitis. Bulletin of the Hospital for Joint Diseases 18: 19-32.
-
Stephan SR, Shallop B, Lackman R, Kim TW, Mulcahey MK (2016) Pigmented Villonodular Synovitis: A Comprehensive Review and Proposed Treatment Algorithm. JBJS Rev 4.