Journal of Musculoskeletal Disorders and Treatment
Necrotizing Fasciitis without Inflammatory Signs in Patients Receiving Anti-Interleukin-6 Receptor Antibody (Tocilizumab): Two Cases Report
Masaki Fujioka1,2*, Kiyoko Fukui2 and Satoko Ishiyama2
1Department of Plastic and Reconstructive Surgery, Nagasaki University, Japan
2Department of Plastic and Reconstructive Surgery, National Hospital Organization Nagasaki Medical Center, Japan
*Corresponding author:
Fujioka Masaki, M.D., Ph.D., Department of Plastic and Reconstructive Surgery, National Hospital Organization Nagasaki Medical Center, 1001-1 Kubara 2, Ohmura City, Nagasaki, Japan, Postal code: 856-8562, Tel: +81-0957-52-3121, Fax +81-0957-54-0292, E-mail: mfujioka@nagasaki-mc.com
J Musculoskelet Disord Treat, JMDT-2-027, (Volume 2, Issue 4), Case Report
Received: October 17, 2016; Accepted: October 29, 2016; Published: November 01, 2016
Citation: Fujioka M, Fukui K, Ishiyama S (2016) Necrotizing Fasciitis without Inflammatory Signs in Patients Receiving Anti-Interleukin-6 Receptor Antibody (Tocilizumab): Two Cases Report. J Musculoskelet Disord Treat 2:027.
Copyright: © 2016 Fujioka M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Tocilizumab is a monoclonal antibody directed against the interleukin-6 receptor and used for the treatment of rheumatoid arthritis (RA). However, patients treated with tocilizumab have risk of infection, such as necrotizing fasciitis (NF). We report two cases of NF involving patients who had been treated with tocilizumab, and highlight the risk of serious soft tissue infection.
Case 1:A 79-year-old woman, who had been treated with tocilizumab for RA, developed NF in her left leg. However, both the white blood cell (WBC) count and C-reactive protein (CRP) were within their normal ranges. Debridement of infectious soft tissue was performed immediately, and the wound was resurfaced with a free skin graft 3 weeks after the primary surgery.
Case 2:A 63-year-old woman who had been treated with tocilizumab for RA developed NF in her right thigh. She showed a normal WBC count and CRP level at the first examination. Debridement was performed immediately, and the wound was resurfaced with a free skin graft 4 weeks later.
It was difficult to make an initial diagnosis of NF, because inflammatory signs, such as WBC and CRP elevation, were absent. This paradoxical phenomenon is explained by the influence of IL-6 blocking therapy. Appropriate diagnostic methods, including computed tomography imaging and exploratory incision, should be performed for an early diagnosis, which can improve the prognosis of patients with NF following tocilizumab treatment.
Keywords
Necrotizing fasciitis, Anti-interleukin-6 receptor antibody, Rheumatoid arthritis, Tocilizumab, Life-threatening infection
Introduction
Biological agents targeting inflammatory cytokines have proven more effective than conventional antirheumatic drugs for suppressing disease activity in rheumatoid arthritis (RA) [1]. Tocilizumab is a monoclonal antibody directed against the interleukin-6 (IL-6) receptor, and it is recognized as an excellent biologic treatment in inflammatory rheumatic conditions [2]. However, patients treated with these immuno-suppressive agents have risk of infection [3]. Furthermore, tocilizumab completely suppresses induced C-reactive protein (CRP), which may mask early inflammatory signs [2].
Necrotizing fasciitis (NF) is a life-threatening infection with pain and fever caused by the progressive inflammatory necrosis of soft tissue. Because the prognosis is worse when the host is immunocompromised, immediate surgical debridement is indispensable [4].
We report two cases of NF involving patients who had been treated with tocilizumab, and highlight the risk of soft tissue infection and the lack of early inflammatory signs in laboratory data.
Case Report
Case 1
A 79-year-old woman was referred from an emergency unit for left leg pain with slight fever (37.5 °C) of 2 days' duration. She had been treated for 2 years with tocilizumab (4 mg/kg every 2 weeks) for RA, and transfused 5 days before referral. At the first examination, she had swelling in the left leg spreading from the step to the knee with erythema (Figure1a). Skin incision showed the infected subcutaneous fat and pus (Figure 1b). E. coli was isolated from the pus. Hematological studies revealed a white blood cell (WBC) count of 4.4 × 109/L and normal CRP (< 3.0 mg/L), indicating no inflammation. The LRINEC (Laboratory Risk Indicator for Necrotizing Fasciitis) score was 2 [5]. The debridement of infectious soft tissue was performed immediately, followed by wound cleansing with saline and treatment with intravenous antibiotics (clindamycin: 600 mg every 8 h, cephazolin: 2 g every 6 h). Confirming the improvement of both the patient's wound and general condition, free skin grafting was performed to resurface the whole wound three weeks after the primary surgery. All the wounds were healed within 3 weeks after the secondary surgery. The patient was discharged 6 weeks after admission, and was able to live at her home without relapse.
.
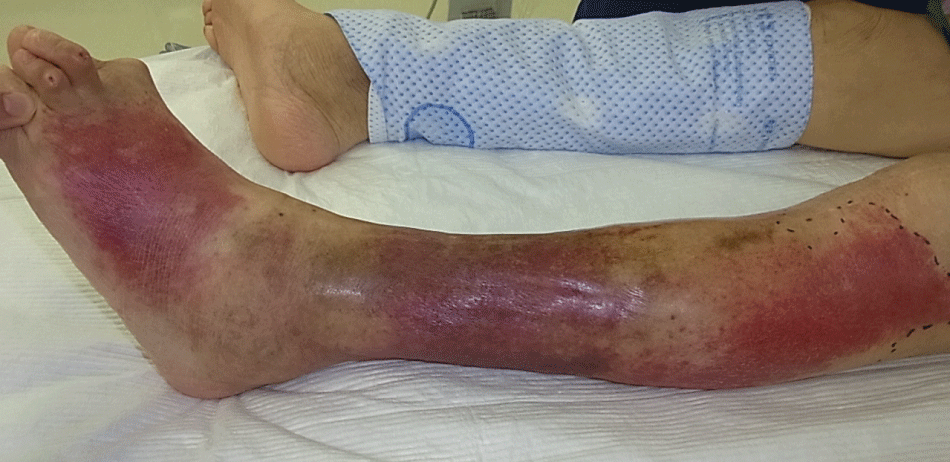
Figure 1A: The first examination of Case 1. The patient had swelling and pain of the left leg spreading from the step to the knee with erythema.
View Figure 1A
.
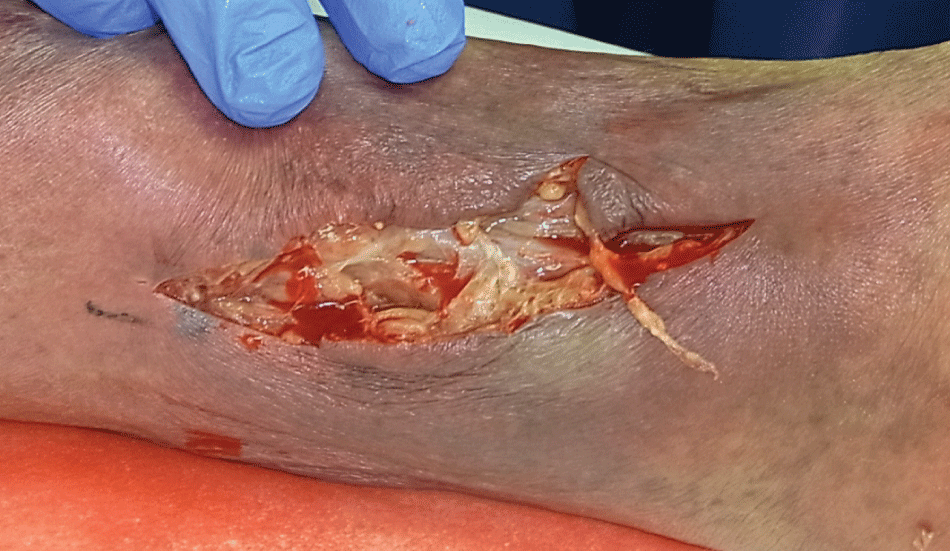
Figure 1B: Skin incision showed the infected subcutaneous fat and pus, indicating necrotizing fasciitis.
View Figure 1B
Case 2
A 63-year-old woman was transferred to our emergency unit for a right thigh ulcer. She had visited another hospital complaining of a temperature of 38.5 °C of 9 days' duration; however, hematological studies on the first day had revealed a WBC count of 7.2 × 109/L and normal CRP level (< 3.0 mg/L), indicating no inflammation. She had undergone treatment with intravenous antibiotics at the initial hospital, but the fever had continued and skin necrosis had developed on the 7th day. She was transferred to our medical center on the 9th day. She had been treated for 3 years with tocilizumab (8 mg/kg every 4 weeks) for RA, and was transfused 14 days before referral.
At the first examination, she had infectious skin necrosis of the right thigh with pain, indicating necrotizing fasciitis (Figure 2a). Proteus mirabilis was isolated from the pus. Hematological studies revealed a WBC count of 13.1 × 109/L and high level of CRP (56.0 mg/L), indicating severe inflammation. However the LRINEC score was 2. The debridement of infectious soft tissue was performed immediately (Figure 2b), and intravenous antibiotics (clindamycin: 600 mg every 8 h, meropenem: 0.5 g every 8 h) and immunoglobulin were administered.
.
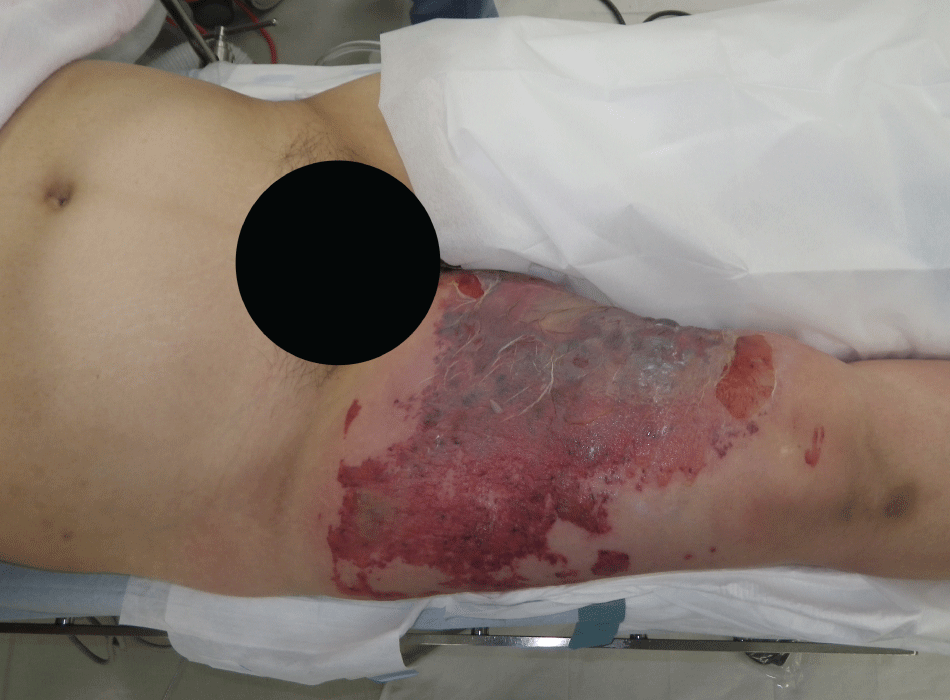
Figure 2A: The first examination of Case 2. The patient had infectious skin necrosis of the right thigh with pain.
View Figure 2A
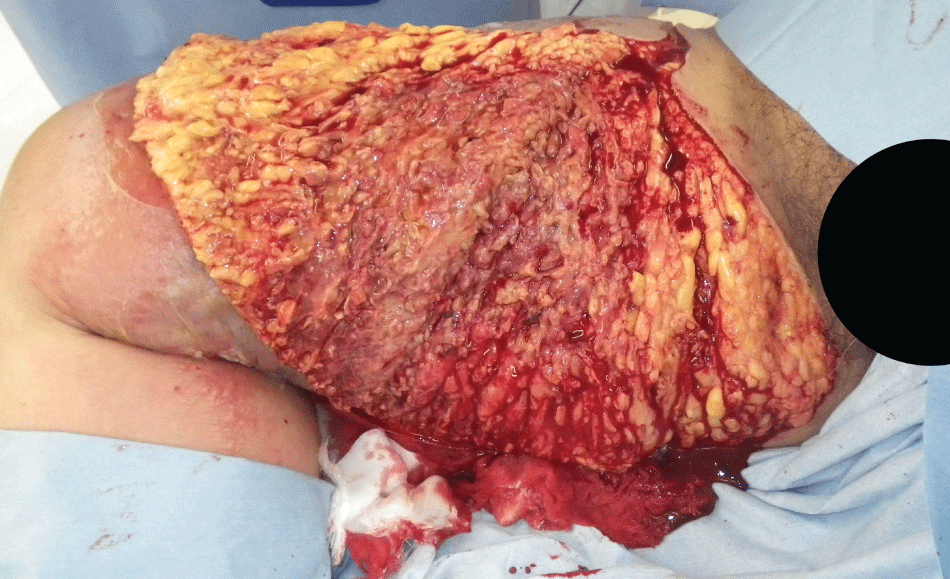
.
Figure 2B: Intra-operative view of immediate debridement. The necrotic subcutaneous fat due to infection was recognized.
View Figure 2B
The entire wound was resurfaced with a free skin graft 4 weeks after admission, and the patient made a full recovery within 2 months. The patient was discharged 6 weeks after admission, and was able to live at home without relapse.
Discussion
The infection risk associated with RA treatment had been evaluated. Corticosteroids are well-known to increase infection risk by inducing immunosuppression, and combination therapy of corticosteroids and conventional disease-modifying antirheumatic drugs (methotrexate, azathioprine, leflunomide, cyclophosphamide, cyclosporine) were shown to increase the risk of serious infections in RA patients [6].
Regarding biological targeted therapies, all agents tend to suppress immunity and are associated with increased risk of infection. Tumor necrosis factor alpha (TNF-α) is a cytokine secreted by macrophages in response to inflammatory stimuli and is involved in immune regulation and inflammation. TNF inhibitors were the first class of biological agents on the market for the treatment of RA, many incidents of infection were reported [7]. Rituximab targets CD20-positive B cells. B cells can contribute to the initiation and maintenance of the inflammatory cascade in RA. By binding to CD20, rituximab depletes subpopulations of peripheral B cells. The T cell costimulation modulator abatacept is a human soluble fusion protein that resembles the natural CTLA4 molecule. Upon antigen recognition T cells require a costimulatory signal for full activation. Abatacept interferes with the CD80/CD86 binding to T cell CD28 with higher avidity than CD28 [8].
Tocilizumab is a monoclonal antibody which inhibits the interleukin-6 receptor, which can be found both on cell surfaces and in the circulation, and it works quickly and effectively in RA. It blocks the downstream effects of IL-6, a cytokine with pleiotropic effects that contributes to the inflammation cascade, by affecting the function of neutrophils, T cells, B cells, and monocytes. Additionally, IL-6 is a potent inducer of the hepatic acute phase response. Thus, the most common adverse events of tocilizumab are infections, including fatal meningitis, septic arthritis, pleurisy, and soft tissue infection [3,9]. Several cases of severe infection in patients during biological targeted therapies have been described. Fujiwara, et al. reported that two patients with RA who developed pneumonia with minimal clinical symptoms during treatment with tocilizumab [10]. Bari, et al. reported a case of patients with severe bacterial arthritis and sepsis who underwent treatment with tocilizumab [11].
According to soft tissue infection, Jones and Ding [12] evaluated the safety of tocilizumab monotherapy, and reported that skin and subcutaneous infections occurred with a higher frequency. Among these soft tissue infections, NF is known to be an aggressive and life-threatening infection with reported mortality rates of between 10 and 20% [13]. Thus, immediate surgical debridement of affected tissue and antibiotic administration are required in the treatment of NF [4,14]. Furthermore, patients treated with tocilizumab can be in a long-lasting immunosuppressive state, because the half-life of tocilizumab is 8-14 days [15]. Yoshida, et al. presented a first case of NF with less inflammatory symptoms in a patient with rheumatoid arthritis treated with tocilizumab in 2012, and van de Sande, et al. also reported a resemble case of NF [15,16].
Masked early symptoms of inflammation can cause a risk of progressive infection. Two groups (Hamilton, et al. and Weng, et al.) investigated the influence of anti-inflammatory drugs for Group A streptococcus soft tissue infection using mice and both groups warned that nonsteroidal anti-inflammatory drugs (NSAIDs) can mask the signs and symptoms of developing infection, and can enhance infection of injured tissues, accelerate disease progression, and increase mortality rate. They concluded that NSAIDs may inhibit neutrophil aggregation or degranulation, so interfere with the function of lymphocytes and inhibit monocyte superoxide production. Moreover, NSAIDs can augment production of cytokines, such as TNF-α, IL-1, and IL-6, on infection. These are interesting reports, because biological targeted therapies can suppress production of cytokines more strongly [17,18].
Delayed diagnosis and late treatment of NF results in poorer outcomes, including death [19]. However, the clinical differentiation of NF from cellulitis appears is difficult, because their early phases can be very similar. In these cases, physicians may become confused and perform delayed surgical treatment [13,17]. Borschitz, et al. [20] compared the initial clinical and laboratory presentations of NF and cellulitis, and concluded that a significantly elevated CRP level would have led to the identification of 83% of the NF patients as opposed to those with cellulitis.
The LRINEC score was developed to distinguish NF from other soft-tissue infections [5], and it is composed of the following six different variables: CRP, total white cell count, hemoglobin, serum sodium, serum creatinine, and serum glucose. Among them, a special emphasis is placed on the CRP level, with 4 points being added in the LRINEC score if the level exceeds 150 mg/L. Patients with more than 6 points in the LRINEC score may have higher mortality and amputation rates. Thus, it is believed that a rise in the CRP level is the most important factor in the diagnosis of NF [21].
Although our patients showed a typical clinical appearance, symptoms, and course of NF, CRP showed a normal level (less than 3,0 mg/L), resulting in only 2 points in the LRINEC score, which indicated little sign of a serious infection. This paradoxical phenomenon might be explained by the influence of IL-6 blocking therapy. Il-6 is a strong inducer of the acute-phase response, which can elevate acute-phase proteins, such as CRP. Thus, IL-6 blocking therapy can suppress acute-phase reactions and symptoms of a severe infection, and normalize serum levels of CRP, which might mask acute inflammatory signs. Several case reports of NF in RA patients undergoing IL-6 blocking therapy have been published [16,22]. Van de Sande, et al. [15] also reported that initial investigations showed a normal CRP level and WBC count of 9.1 × 109/L, although the patient developed NF clinically. The discrepancy between clinical futures and laboratory data may lead to misdiagnosis and prevent early treatment. Although our patients were promptly diagnosed with NF and underwent surgical debridement immediately, suppression of an acute-phase reaction and related symptoms may lead to a delay in treatment, resulting in more severe sepsis.
Conclusion
Two patients who developed NF with a normal level of CRP and WBC count due to the use of tocilizumab were reported. In these cases, it was difficult to make an initial diagnosis of NF because the patients lacked typical laboratory findings, such as elevated CRP.
However, both cases showed severe pain and clear skin redness or necrosis. Appropriate diagnostic methods, including computed tomography imaging and exploratory incision, should be performed for an early diagnosis, which can improve the prognosis of patients with NF following tocilizumab treatment.
Financial Disclosure and Products
There were no external sources of funding in the form of grants supporting the work presented in this manuscript.
Conflict of Interest
There are no conflicts of interest, including financial, consultant, institutional, and other relationships, that might lead to a perceived bias.
Ethical Considerations
The procedures followed were in accordance with the ethical standards of our institutional committee on human experimentation and with the Helsinki Declaration of 1975, as revised in 1983.
Patients in our manuscript were also informed about the patient's ethical rights by the author, and agreed that the patient's illustrative material, including face, could be used for the aim of the medical study, and also agreed to the photos being published in a medical journal.
References
-
Ling-dong Quant, Geoffrey M Thiele, Jun Tina, Dong Wang (2008) The Development of Novel Therapies for Rheumatoid Arthritis. Expert Opin Ther Pat 18: 723-738.
-
Nishimoto N, Hashimoto J, Miyasaka N, Yamamoto K, Kawai S, et al. (2007) Study of active controlled monotherapy used for rheumatoid arthritis, an IL-6 inhibitor (SAMURAI): evidence of clinical and radiographic benefit from an X-ray reader-blinded randomised controlled trial of tocilizumab. Ann Rheum Dis 66: 1162-1167.
-
Campbell L, Chen C, Bhagat SS, Parker RA, Ostor AJ (2011) Risk of adverse events including serious infections in rheumatoid arthritis patients treated with tocilizumab: a systematic literature review and meta-analysis of randomized controlled trials. Rheumatology 50: 552-562.
-
Fujioka M, Nishimura G, Miyazato O, Yamamoto T, Okamoto F, et al. (2003) Necritizing fasciitis and myotitis that originated from gastrointestinal bacterial infection:Two fatel cases. Scand J Plast Reconstr Surg Hand Surg 37: 239-242.
-
Su YC, Chen HW, Hong YC, Chen CT, Hsiao CT, et al. (2008) Laboratory risk indicator for necrotizing fasciitis score and the outcomes. ANZ J Surg 78: 968-972.
-
Doran MF, Crowson CS, Pond GR, O'Fallon WM, Gabriel SE (2002) Predictors of infection in rheumatoid arthritis. Arthritis Rheum 46: 2294-2300.
-
Greenberg JD, Reed G, Kremer JM, Tindall E, Kavanaugh A, et al. (2010) Association of methotrexate and tumour necrosis factor antagonists with risk of infectious outcomes including opportunistic infections in the CORRONA registry. Ann Rheum Dis 69: 380-386.
-
Keyser FD (2011) Choice of Biologic Therapy for Patients with Rheumatoid Arthritis: The Infection Perspective. Curr Rheumatol Rev 7: 77-87.
-
Nguyen MT, Pødenphant J, Ravn P (2013) Three cases of severely disseminated Staphylococcus aureus infection in patients treated with tocilizumab. BMJ Case Rep.
-
Fujiwara H, Nishimoto N, Hamano Y, Asanuma N, Miki S, et al. (2009) Masked early symptoms of pneumonia in patients with rheumatoid arthritis during tocilizumab treatment: a report of two cases. Mod Rheumatol 19: 64-68.
-
Bari SF, Khan A, Lawson T (2013) C reactive protein may not be reliable as a marker of severe bacterial infection in patients receiving tocilizumab. BMJ Case Rep.
-
Jones G, Ding C (2010) Tocilizumab: a review of its safety and efficacy in rheumatoid arthritis. Clin Med Insights Arthritis Musculoskelet Disord 3: 81-89.
-
De Roos WK, van Lanschot JJB, Bruining HA (1991) Fournier's gangrene: the need for early recognition and radical surgical debridement. Neth J Surg 43: 184-188.
-
Marks C, Marks R (2012) Dermatological conditions requiring intensive care. Hautarzt 63: 727-738.
-
van de Sande MG, van Slobbe-Bijlsma ER (2012) Necrotizing fasciitis in a rheumatoid arthritis patient treated with tocilizumab. Rheumatology (Oxford) 51: 577-578.
-
Yoshida A, Ota T, Sasaoka S, Matsuura H, Fujimoto W, et al. (2012) Necrotizing fasciitis in a patient with rheumatoid arthritis treated with tocilizumab. Mod Rheumatol 22: 317-318.
-
Stephanie M Hamilton, Clifford R Bayer, Dennis L Stevens, Amy E Bryant (2014) Effects of Selective and Nonselective Nonsteroidal Anti-inflammatory Drugs on Antibiotic Efficacy of Experimental Group A Streptococcal Myonecrosis. J Infect Dis 209: 1429-1435.
-
Weng TC, Chen CC, Toh HS, Tang HJ (2011) Ibuprofen worsens Streptococcus pyogenes soft tissue infections in mice. J Microbiol Immunol Infect 44: 418-423.
-
Pakula AM, Kapadia R, Freeman B, Skinner RA (2012) A 3-year experience with necrotizing fasciitis: favorable outcomes despite operative delays in a busy acute care hospital. Am Surg 78: 1059-1062.
-
Borschitz T, Schlicht S, Siegel E, Hanke E, von Stebut E (2015) Improvement of a Clinical Score for Necrotizing Fasciitis: 'Pain Out of Proportion' and High CRP Levels Aid the Diagnosis. PLoS One 10: e0132775.
-
Colak E, Ozlem N, Kucuk GO, Aktimur R, Kesmer S (2016) Laboratory Risk Indicators for Necrotizing Fasciitis and Associations with Mortality. Turk J Emerg Med 14: 15-19.
-
Hashimoto N, Yamaoka T, Koguchi-Yoshioka H, Tanaka A, Tanemura A, et al. (2015) Development of necrotising fasciitis in a patient treated for rheumatoid arthritis with tocilizumab. Acta Derm Venereol 95: 370-371.