Journal of Musculoskeletal Disorders and Treatment
The Effects of Manual Mobilization on the Mobility of the Thoracic Spine in Patients with Ankylosing Spondylitis
Uwe Lange1,2*, Martin Sperling1,2, Katrin Richter1,2, Gabriel Dischereit1,2, Ulf Müller-Ladner1,2 and Ingo H. Tarner1,2
1Department of Internal Medicine and Rheumatology, University of Giessen, Germany
2Department of Rheumatology, Osteology and Physical Medicine, Kerckhoff-Klinik, Germany
*Corresponding author:
Uwe Lange, Department of Rheumatology, Osteology, Physical Medicine, Kerckhoff-Klinik, Germany, Tel: 0049-0-6032-996-2101, E-mail: U.Lange@kerckhoff-klinik.de
J Musculoskelet Disord Treat, JMDT-2-011, (Volume 2, Issue 2), Original Article
Received: February 11, 2016: Accepted: April 23, 2016: Published: April 26, 2016
Citation: Lange U, Sperling M, Richter K, Dischereit G, Müller-Ladner U, et al. (2016) The Effects of Manual Mobilization on the Mobility of the Thoracic Spine in Patients with
Ankylosing Spondylitis. J Musculoskelet Disord Treat 2:011.
Copyright: © 2016 Lange U, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective:To explore the effects of manual mobilization on thoracic spine mobility, respiratory function and disease activity in patients with ankylosing spondylitis (AS).
Methods:Two groups, each consisting of 12 patients, were treated with standard physiotherapy during a regular inpatient stay. After randomization, one group was also treated with manual mobilization of the thoracic spine for an average of 6 sessions, whereas the other group only received conventional physiotherapy. The primary outcome parameter was the mobility of the thoracic spine represented by the Ott's sign. The secondary outcome parameters were pain (VAS), respiratory function (differences of chest expansion and inspiratory vital capacity - IVC), Bath Ankylosing Spondylitis Disease Activity Index (BASDAI), and Bath Ankylosing Spondylitis Functional Index (BASFI).
Results:Mobility of the thoracic spine (Ott's sign) increased significantly within the group of manually mobilized patients compared to baseline (hospital admission) at each of the follow-up visits (p_discharge < 0.002, p_1month < 0.002, p_3months < 0.004). No significant impact on thoracic spine mobility could be found in the control group. Comparing both groups, manually mobilized patients had significantly improved mobility at the time of discharge from the hospital (p < 0.002) as well as 1 month later (p < 0.009). No difference could be shown after 3 months. The group treated with manual mobilization showed also a significant pain reduction compared to baseline (p_discharge < 0.006, p_1month < 0.005, p_3months < 0.013). Parameters of the respiratory function test increased during therapy with manual mobilization. Compared to baseline, chest expansion improved at all follow-up visits (p_discharge < 0.001, p_1month < 0.026, p_3months < 0.005). The therapy also had a positive impact on the IVC at the time of discharge (p < 0.003) and after 3 months (p < 0.008). Regarding the scores (BASDAI, BASFI), a significant decrease was detected, thus reflecting a general improvement of the manually treated patients in terms of disease activity and function. Overall, the observed effects on most outcome parameters lasted until the follow-up visit at 1 month after discharge but could be observed up to 3 months later.
Conclusion:The results show that physiotherapy including manual mobilization of the thoracic spine promotes mobility, improves respiratory function and has a positive influence on disease activity and physical function. Therefore, manual mobilization of the spine (without ankylosis) should be included in the physical therapy concept of patients with AS. Since the effects appear to last for approximately 3 months, manual mobilization should be strongly considered as an additive physiotherapeutic option.
Keywords
Ankylosing spondylitis, Exercise, Manual mobilization, Physiotherapy
Introduction
Ankylosing spondylitis (AS) is a chronic inflammatory rheumatic disease, which is frequently associated with HLA-B27. It predominantly affects young adults with a peak age of onset between 20 and 30 years. Furthermore, AS is mainly affecting the sacroiliac joints (with sacroiliitis being one of the hallmarks) with predilections of the axis skeleton, peripheral joints, and inflammation at sites of bony insertions for tendons and ligaments (enthesitis). An involvement of other organs, such as gastrointestinal tract, anterior uvea, lung, kidney, and heart, has also been described [1,2].
The most common symptom of AS is low back pain. This first and common symptom of AS is resulting in morning stiffness, and limited mobility [1,2]. Subsequently, AS can substantially affect quality of life and daily life in various ways, e.g. household or work-related tasks becoming more difficult as a result of the limited joint and spinal motion. In the multidisciplinary treatment plan, exercise plays an essential part [3-5]. It can include home exercise, individual or group exercise with a physical therapist, or physical therapy treatments. Therefore, each patient should be evaluated and instructed by a physical therapist. The exercise should consist of posture training, deep breathing, back extension, and other stretching movements [3-6].
Based on the ameliorating effects of disease-targeted physiotherapy, the aim of the present study was to explore the effects of manual mobilization on thoracic spine mobility, respiratory function and disease activity in patients with AS without ankylosis of the thoracic spine.
Materials, Methods and Design
Patients and interventions
Two groups of regular inpatients of our rheumatology department, each consisting of 12 patients were treated with conventional physiotherapy (6 sessions including exercise, respiratory training, massage of the back, electrotherapy, and mud packs) over 9 days. After randomization (using computer-generated random numbers) 12 patients were treated with manual mobilization of the thoracic spine (manual therapy [MT] group, without ankylosis of the thoracic spine) for an average of 6 sessions, whereas the other group continued to receive conventional physiotherapy (physiotherapy group - control group). Manual therapy was performed in all patients by the same physiotherapist. Table 1 shows the demographic, clinical, and therapeutic characteristics of both groups.
![]()
Table 1: Demographic, clinical, and therapeutic characteristics.
View Table 1
Inclusion criteria were: Men and women aged 18-65 years with the diagnosis of AS defined by the modified New York criteria [7].
Exclusion criteria were: Current inflammation of the thoracic spine (exclusion by MRI of the thoracic spine), initial or complete ankylosis of the thoracic spine (exclusion by MRI or X-ray), and contraindication for manual mobilization [inflammatory and destructive processes, trauma, osteoporosis, hemodilution therapy - e.g. coumarin].
Manual mobilization technique of the thoracic spine: At first, the structures were prepared. For this, the patient was seated on a chair in straight position (initial position), than followed a progressively maximal sagittal flexion of the cervical and thoracic column with subsequently maximal extension and erection of the spine in end-range position (8-10 times repetition for 2-3 minutes). Then, the patient rested in ventral position on a divan bed, both arms in sidewise position for an optimal ventral mobilization of the vertebrae (manual mobilization according to the concept of Kaltenborn and Evjenth). Therefore, the therapist fixed with his right index and middle finger both processi transversi of each thoracic segment. Afterwards, the ulnar side of the other hand dropped on the position of the two fingers of the right hand and applied force under a translational gliding and stretching from caudal to a ventral position. Each thoracic segment was treated in this way for 3 minutes. After each session, the stabilization of the achieved movement was trained by proprioceptive neuromuscular facilitation (PNF)-scapula pattern for 2-3 minutes. All mobilizations were performed within the available range of movement, without eliciting muscular resistance or pain sensations from the patients.
Outcome parameters
The primary outcome parameter was the mobility of the thoracic spine represented by the Ott's sign (a mark is placed between the vertebra prominence of the 7th cervical vertebral body and another mark is made 30 cm below. The patient then bends maximally forward without bending the knees and the distance is measured again (normal expansion > 2.5 cm).
The secondary outcome parameters were pain (visual analog scale - VAS, measured by a scale from 0 [no pain] to 10 [maximal pain] over the last 24 hours), respiratory function (differences of chest expansion measured at the level of the fourth intercostal space or just below the breasts in females [normal expansion > 2.5 cm], and inspiratory vital capacity = IVC, measured by lung function testing, Master-Screen® Body from Viasys Healthcare, version 5.2), disease activity (Bath Ankylosing Spondylitis Disease Activity Index - BASDAI), and functional index (Bath Ankylosing Spondylitis Functional Index - BASFI). The outcome parameters were measured at baseline (admission to the hospital), at the end of the intervention (discharge), and at one and three months after discharge.
Statistical analysis
Statistical analysis was made with the Software Statistical Package for Social Sciences (SPSS program, V11.5, SPSS, Inc., Chicago, IL, USA) for Windows. At first the data were listed descriptive (mean ± SD), group differences were analyzed by the Mann-Whitney U -test and differences between the measuring time of the outcome parameters were detected by the Wilcoxon-test. Statistical significance was defined as a p value < 0.05 (Table 2).
![]()
Table 2: Results.
View Table 2
Ethics approval
The study protocol was approved by the local ethics committee of the University of Giessen. The study was conducted in accordance with the Helsinki Declaration of 1975, as revised in 1983. Moreover, all patients submitted written consent forms, and all patients screened for participation in the study agreed to take part and fully completed the study.
Results
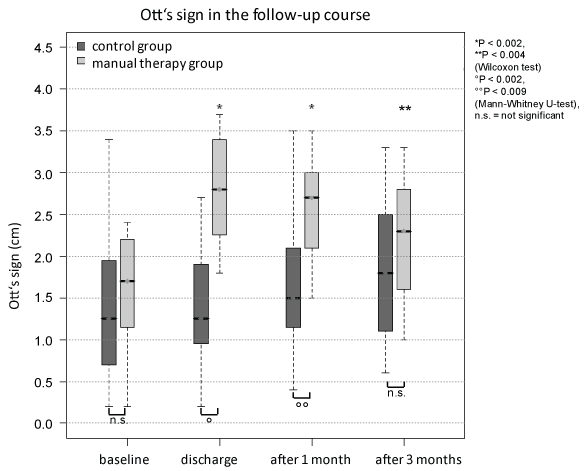
The MT-group showed a significantly increased mobility of the thoracic spine (Ott's sign) compared to baseline (hospital admission) at each of the follow-up visits (p_discharge < 0.002, p_1month < 0.002, p_3months < 0.004), whereas no significant impact on thoracic spine mobility could be noted in the control group (Figure 1 and Table 1). Comparing both groups, manually mobilized patients had significantly improved mobility at the time of discharge from the hospital (p < 0.002) as well as 1 month later (p < 0.009). No difference could be shown after 3 months.
.
Figure 1: The Ott's sign was not significantly different at baseline and after 3 months between both groups. At discharge and after 1 month (°p < 0.002, °°p < 0.009, Mann-Whitney U-test) was a significant group difference. Only the group of manually mobilized patients showed a significantly increased mobility of the thoracic spine (Ott's sign) compared to baseline (hospital admission) at each of the follow-up visit (*p < 0.002, **p < 0.004, Wilcoxon test).
View Figure 1
.
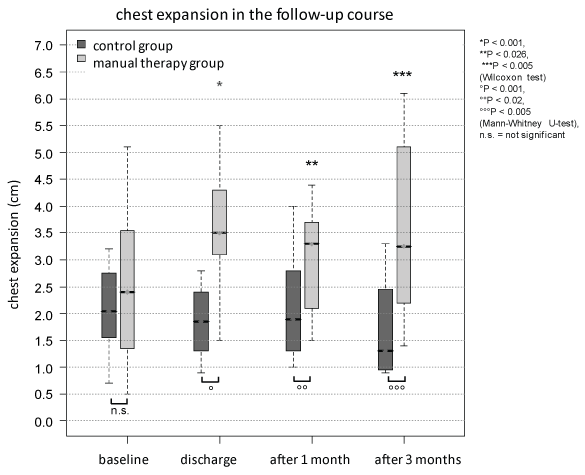
Figure 2: The chest expansion showed no significant difference at baseline between both groups, but was significant different at discharge, after 1 month and 3 months (°p < 0.001, °°p < 0.02, °°°p < 0.005, Mann-Whitney U-test). Only the group of manually mobilized patients improved with the chest expansion compared to baseline (hospital admission) at each follow-up visit (*p < 0.001, **p < 0.026, ***p < 0.005, Wilcoxon test).
View Figure 2
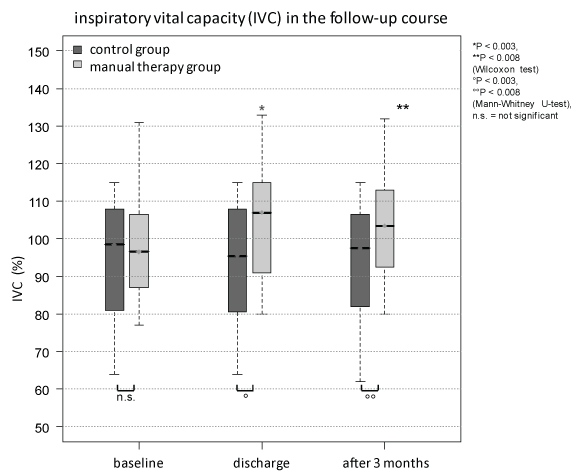
Parameters of the respiratory function test increased during therapy with manual mobilization (Figure 2, Figure 3 and Table 1). Compared to baseline, chest expansion improved at all follow-up visits (p_discharge < 0.001, p_1month < 0.026, p_3months < 0.005). The therapy had also a positive impact on the IVC at the time of discharge (p < 0.001) and after 3 months (p < 0.007) in the MT-group.
.
Figure 3: The inspiratory vital capacity (IVC %) showed no significant difference at baseline, but at discharge and after 3 months there was a significant difference between both groups (°p < 0.003, °°p < 0.008, Mann-Whitney U-test). During the follow-up course only in the group of manually mobilization showed a significant increase compared to baseline at discharge and after 3 months (*p < 0.003, **p < 0.008, Wilcoxon test).
View Figure 3
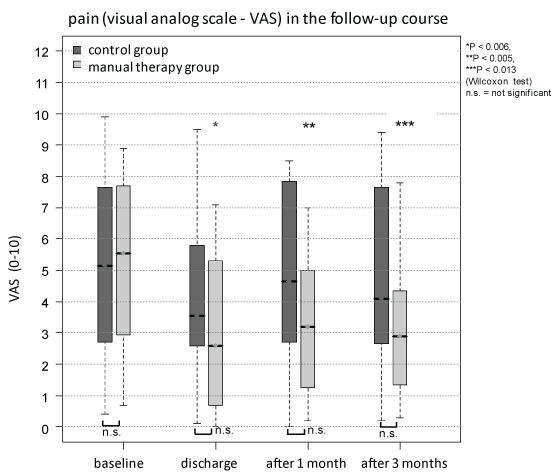
An effect on reducing pain (VAS) was not achieved, but the group treated with MT showed a significant pain reduction compared to baseline during the follow-up (p_discharge < 0.006, p_1month < 0.005, p_3months < 0.013 Figure 4 and Table 1). Of interest, seven of 12 MT-patients were able to finish the NSAID medication at discharge (lasting up to 3 months), but none of the control-group.
.
Figure 4: Pain, measured by the visual analog scale, showed no significant difference between both groups during the follow-up. Merely the group treated with manual mobilization presented a significantly pain reduction compared to baseline (*p < 0.006, **p < 0.005, ***p < 0.013, Wilcoxon test).
View Figure 4
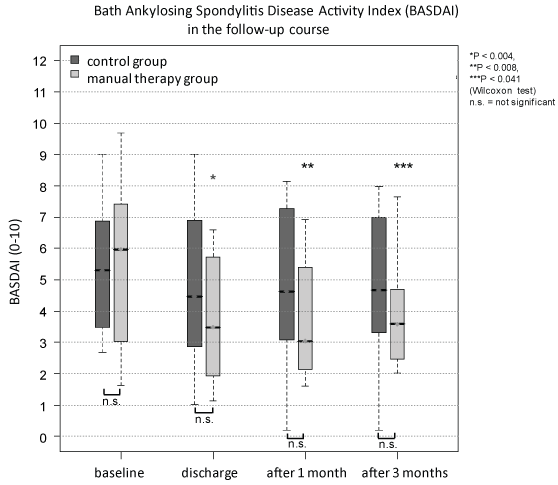
Regarding the scores (BASDAI, BASFI), a significant decrease could also be confirmed reflecting a general improvement of the manually treated patients in terms of disease activity and function (Figure 5, Figure 6 and Table 1).
.
Figure 5: The Bath Ankylosing Spondylitis Disease Activity Index (BASDAI) was not significant different between both groups at baseline and the followed visits. During the follow-up course only the manual treated group showed a significant decrease compared to baseline (*p < 0.004, **p < 0.008, ***p < 0.041).
View Figure 5
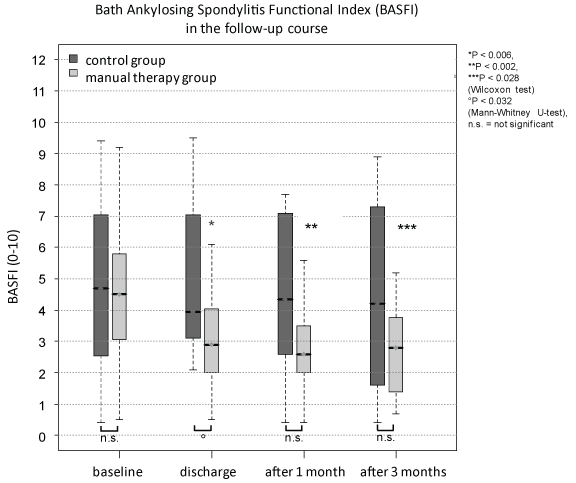
.
Figure 6: The Bath Ankylosing Spondylitis Functional Index (BASFI) was not significant different between both groups at baseline, after 1 month, and 3 months. At discharge there was a significant difference between both groups (°p < 0.032, Mann-Whitney U-test). In the follow-up course only the manual treated group presented a significant decrease compared to baseline (*p < 0.006, **p < 0.002, ***p < 0.028).
View Figure 6
Most notably, the observed effects on most outcome parameters could be observed at the follow-up visit at 1 month after discharge and lasted up to 3 months later.
Discussion
Most AS patients with mild disease usually restricted to a small area of involvement, e.g. single vertebrae, are able to maintain almost full functional and employment capacity [1,2]. However, a minority of patients develop severe skeletal functional restrictions or even life-threatening extra-musculoskeletal complications. Disease activity is variable in the individual patient, with symptoms usually persisting over decades, and approximately 1% of patients develop a stage of complete disease inactivity and/or long-term remission [8].
International recommendations and guidelines for AS therapy include medication and also physical therapy options. The prognosis of AS has further improved with the use of TNF blockers, especially in those treated very early in disease [9]. In this regard, a meta-analysis indicated that the anti-TNF alpha agents were similar in efficacy in AS [10]. The responses are typically rapid, but 20-30% of patients do not respond to or do not tolerate anti-TNF agent [6]. However, only to these positive effects of anti-TNF agents in the treatment of AS, the questions arises, if physical therapy and rehabilitation are still necessary in the age of anti-cytokine therapy. In contrast, the following aspects underlined physiotherapeutic and rehabilitative therapy in the management of AS: For preventive strategies and modulation of anatomical structure and reduced joint and spine function physical medicine is an essential tool [3-6]. Furthermore, detailed examination is indicated in initial stages of the disease to improve or to conserve function whereas an indication for disease modifying antirhreumatic drugs is not essential. Moreover, regular exercise acts as a positive formative stimulus of remodeling for joints and function, for endurance training (modulation of reduced cardio-pulmonary function) and for psycho-physical conditioning. Optimal treatment of reduced functional health needs physical and rehabilitative medicine for short- and long-time effects [3-6]. Components like body function, structures, activities, and participation with respect to the international classification of functioning; disabilities and health (ICF) are only partially ameliorated, where as context factors are not modified. Besides, psychological aspects are not sufficiently improved under a pharmacological therapy. Moreover, distinct aspects of rehabilitation and physical medicine are the inclusion of different co-morbidities and severity as well as an adequate patient education. Recently, our group performed a proof-of-concept study, in which the dose of the TNF-blocker etanercept was applied with 50% of the standard dose and combined with standard intensive physiotherapy (3 sessions of 30 minutes per week) over a time period of 4 months with a follow up to 6 months. The results provided a strong evidence that intensive physiotherapy could substitute for a reduction of TNF-dosage and become a therapeutic alternative, especially in the context of cost-effectiveness [11].
The non-pharmacological treatments include patient education and exercise. Home exercise is effective, but supervised exercise programs or formal physical therapy can be of greater benefit [12]. Optimally, an initial evaluation and training by a physical therapist should be part of the therapeutic regimen. Exercises include postural training, range of motion stretching, recreational activities, and hydrotherapy. In addition, pain relief measures such as local heat or cold can be added. At least, patients with AS should participate in an unsupervised home exercise program [13]. Here, inpatient rehabilitation is rarely needed [14].
Patients who are doing clinically well with pharmacologic treatment will nevertheless benefit from education and exercise [15-18]. A randomized trial involving 62 patients clinically stable on anti-TNF therapy showed statistically significant benefit in the BASDAI and in spinal range of motion after two and six months when combining an intensive rehabilitative exercise treatment program with an educational-behavioral program, compared with the educational-behavioral treatment alone or a control group [18].
At present, there is strong evidence for physiotherapy, especially for exercise, in AS patients [12,19-21], whereas valid data for manual therapy in AS are still insufficient. Therefore, the present study explored the effects of manual mobilization on the thoracic spine mobility, respiratory function and disease activity in patients with ankylosing spondylitis (AS).
The mobility of the thoracic spine (reflected by Ott's sign) increased significantly within the group of manually mobilized patients compared to baseline (hospital admission) at each of the follow-up visits, whereas no significant improvement on thoracic spine mobility could be observed in the control group. Comparing both groups, manually mobilized patients had significantly improved mobility at the time of discharge from the hospital as well as 1 month later, without longstanding effect after 3 months.
Only the group treated with manual mobilization showed a significant pain reduction compared to baseline during the follow up. Parameters of the respiratory function test increased during therapy with manual mobilization. When compared to baseline, chest expansion improved also at all follow-up visits. Furthermore, the therapy also showed a consecutive positive impact on the IVC at the time of discharge and after 3 months. Regarding the scores (BASDAI, BASFI), a significant decrease was detected, thus reflecting a general improvement of the manually treated patients in terms of disease activity and function.
Taken together, this is one of the first studies exploring the feasibility and effects of manual mobilization on the mobility of the thoracic spine in patients with AS. The presented results are in accordance to another study of manual mobilization of thoracic kyphosis in elderly postmenopausal patients with osteoporosis [22]. Three months of rehabilitation with manual mobilization ameliorated significantly thoracic kyphosis, back pain and quality of life.
Of note, the observed effects in the present study on most outcome parameters lasted until the follow-up visit at 1 month after discharge but were observed to 3 months later, supporting the idea that a distinct exercise program and manual therapy are essential for a long-term therapy strategy in AS patients. A potential limitation of this pilot study is the small number of patients. However, the promising results need to be emphasized by large-scale studies. Furthermore, long-term effects are of great interest.
Conflict of Interest
None of the authors have any conflicts of interests.
References
-
Braun J, Sieper J (2014) Axiale Spondylarthritis. (3rd edn), UNI-MED, Bremen, London, Boston.
-
Khan MA (2003) Clinical features of ankylosing spondylitis. In:. Hochberg MC, Silman AJ, Smolen JS, Weinblatt ME, Weisman MH, Rheumatology. (3rd edn), Mosby, London, New York, Oxford, Philadelphia, 1161-1181.
-
Engel JM, Uhlemann C, Berg W, Lange U (2003) Physical Medicine in Rheumatology – Differential Indicative Prescription in rheumatoid arthritis, ankylosing spondylitis and progressive systemic sclerosis. Akt Rheumatol 28: 218-224.
-
Lange U, Rehart S (2013) Significance and importance of physical medicine in the context of conservative therapy for rheumatic patients. Orthopäde 42: 813-821.
-
Lange U, Müller-Ladner U (2015) Physiotherapy for rheumatic diseases: What is evidence-based? Akt Rheumatol 40: 475-478.
-
Lange U, Kürten B, Müller-Ladner U, Uhlemann C (2007) Physiotherapeutic and rehabilitation therapy for ankylosing spondylitis. Status quo and are they still necessary in the age of anti-cytokine therapy? Z Rheumatol 66: 727-733.
-
Van der Linden S, Valkenburg HA, Cats A (1984) Evaluation of diagnostic criteria for ankylosing spondylitis. A proposal for modification of the New York criteria. Arthritis Rheum 27: 361-368.
-
Kennedy LG, Edmunds L, Calin A (1993) The natural history of ankylosing spondylitis. Does it burn out? J Rheumatol 20: 688-692.
-
Haibel H, Sieper J (2010) Editorial review: how early should ankylosing spondylitis be treated with a tumor necrosis factor-blocker? Curr Opin Rheumatol 22: 388-392.
-
McLeod C, Bagust A, Boland A, Dagenais P, Dickson R, et al. (2007) Adalimumab, etanercept and infliximab for the treatment of ankylosing Spondylitis: a systematic review and economic evaluation. Health Technol Assess 11: 1-158, iii-iv.
-
Meier F, Müller-Ladner U, Lange U (2014) Efficacy of Intensive Physiotherapy in Combination with Low-dose Etanercept in Active Spondyloarthritis: A Monocentric Pilot Study. J Rheumatol 41: 1897-1898.
-
Dagfinrud H, Kvien TK, Hagen KB (2008) Physiotherapy interventions for ankylosing spondylitis. Cochrane Database Syst Rev 1: CD002822.
-
Elyan M, Khan MA (2008) Does physical therapy still have a place in the treatment of ankylosing spondylitis? Curr Opin Rheumatol 20: 282-286.
-
Lubrano E, D'Angelo S, Parsons WJ, Corbi G, Ferrara N, et al. (2007) Effectiveness of rehabilitation in active ankylosing spondylitis assessed by the ASAS response criteria. Rheumatology 46: 1672-1675.
-
Dubey SG, Leeder J, Gaffney K (2008) Physical therapy in anti-TNF treated patients with ankylosing spondylitis. Rheumatology 47: 1100-1101.
-
Spadaro A, De Luca T, Massimiani MP, Ceccarelli F, Riccieri V, et al. (2008) Occupational therapy in ankylosing spondylitis: Short-term prospective study in patients treated with anti-TNF-alpha drugs. Joint Bone Spine 75: 29-33.
-
Lubrano E, D'Angelo S, Spadaro A, Palazzi C, Olivieri I (2011) Rehabilitation for ankylosing spondylitis in the era of biologics: any room left for this treatment? J Rheumatol 38: 1228-1230.
-
Masiero S, Bonaldo L, Pigatto M, Lo Nigro A, Ramonda R, et al. (2001) Rehabilitation treatment in patients with ankylosing spondylitis stabilized with tumor necrosis factor inhibitor therapy: a randomized controlled trial. J Rheumatol 38: 1335-1342.
-
Viitanen JV, Lehtinen K, Suni J, Kautiainen H (1995) Fifteen months' follow-up of intensive inpatient physiotherapy and exercise in ankylosing spondylitis. Clin Rheumatol 14: 413-419.
-
Analay Y, Ozcan E, Diracoglu D, Aydin R (2003) The effectiveness of intensive group exercise on patients with ankylosing spondylitis. Clin Rehabil 17: 631-636.
-
Ince G, Sarpelt T, Durgan B, Erdogan S (2006) Effects of a multimodal exercise program for people with ankylosing spondylitis. Phys Ther 86: 924-935.
-
Bautmans I, van Arken J, van Mackelenberg M, Mets T (2010) Rehabilitation using manual mobilization for thoracic kyphosis in elderly postmenopausal patients with osteoporosis. J Rehabil Med 42: 129-135.