Journal of Musculoskeletal Disorders and Treatment
Exploring Cross-Curriculum Content of Undergraduate Musculoskeletal Therapy Courses Regarding Articular Cartilage; Implications of Surveying UK Healthcare Curriculum Providers
Philip Bright* and Karen Hambly
Research Department, European School of Osteopathy, UK
*Corresponding author:
Philip Bright, Research Department, European School of Osteopathy, UK, E-mail: philbright@eso.ac.uk, pb301@kent.ac.uk
J Musculoskelet Disord Treat, JMDT-2-010, (Volume 2, Issue 1), Original Article
Received: January 05, 2016 | Accepted: March 28, 2016 | Published: March 30, 2016
Citation: Bright P, Hambly K (2016) Exploring Cross-Curriculum Content of Undergraduate Musculoskeletal Therapy Courses Regarding Articular Cartilage; Implications of Surveying UK Healthcare Curriculum Providers. J Musculoskelet Disord Treat 2:010.
Copyright: © 2016 Bright P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background:Assessing curriculum across undergraduate healthcare education can be challenging with potential heterogeneity. Focus on a subset of healthcare may indicate variability in curriculum content. Knee articular cartilage and associated injury and repair procedures demand attention; debilitation and development of osteoarthritis severely affect patient quality of life. The level to which musculoskeletal (MSK) therapy education encompasses this area across disciplines is poorly understood.
Objectives:To explore if UK MSK courses differ in articular cartilage content based on the final professional qualification.
Design:Cross-sectional online questionnaire.
Method:Universities and Colleges Admissions Service (UCAS) database was searched to identify providers from: physiotherapy; osteopathy; chiropractic; sports therapy. A questionnaire was developed and invitation to engage sent to course personnel. Details of 16 specific articular cartilage and related course characteristics were captured. Questions were scored based on prevalence reported (0-16). Inter-professional differences between scores were explored using Kruskal-Wallis and Mann-Whitney U test.
Results/findings:Seventy-six participants were identified from 107 providers. Eleven (14%) responses were received; physiotherapy (30%), sports therapy (30%), osteopathy (40%). Mean scores were 11.33, 13.67 and 8.5 respectively. No significant difference was found between scores based on profession/entry requirements; surgical repair elements scored significantly lower (p < 0.05).
Conclusions:Findings provide indication of consistency of detail on articular cartilage in UK MSK undergraduate curriculum: post-surgery rehabilitation was not consistently represented; generic protocols were well-reported. Considerations for subsequent research are how to ensure student practitioners are provided with contemporary knowledge to provide patient-centred, evidence-based care through programme delivery.
Keywords
Musculoskeletal, Curriculum, Articular cartilage repair, Knee
Background
Assessing curriculum content across undergraduate healthcare education providers can be challenging with various factors influencing the dissemination of core knowledge to support the key attributes expected in practitioners [1]. The adoption of evidence-based good clinical practice (GCP) is difficult to gauge as are transition timescales of significant research into guidelines, frameworks and curriculum [2]. The breadth of content within healthcare education over a broad range of disciplines would suggest heterogeneity in providers [3]. A focus on a single clinical research interest and a subset of healthcare may provide indication of the variability of adopting standards into curriculum.
Articular cartilage lesions are a major source of debilitation in the population as a precursor to osteoarthritis (OA) [4]. The sequelae of this can be reduced range of motion, withdrawal from physical activity and lower quality of life [5]. Exercise interventions for knee OA have been identified as a priority area for research [6] and there are a number of articular cartilage repair (ACR) procedures available. Provocative techniques such as microfracture and Pridie drilling seek to stimulate cartilage regeneration while osteochondral autograft transfer system (OATS) and mosaicplasty look to transplant healthy cartilage from low-load areas [7]. Cell-based treatments such as platelet-rich plasma (PRP) injections and defect-filling harvested or bioengineered chondrocytes have shown varying effectiveness [8,9]. Third-generation techniques such as matrix assisted chondrocyte implantation/transplantation (MACI/T) are being shown to have notable efficacy over rival invasive approaches [10].
The procedures available for ACR are well-documented [11] but the lack of high-level evidence for outcomes prevents unequivocal recommendation from the National Institute for Health and Care Excellence (NICE) in the UK [12]. Positive outcomes could rely on sufficient support from therapists providing staged rehabilitation protocols that respect the phases of repair, remodelling and maturation [13]. The current UK provision of post-surgical ACR rehabilitation is incumbent on therapists operating within a National Health Service (NHS) setting or private therapists. Protocols are in place based on basic science and empirical studies [14]; the knowledge transfer timescale from published guidelines to standard clinical practice is not currently quantifiable. This theory-practice gap may be attributable to inherent student mind-set and inability to synthesise classroom and clinical experience [15]. Quality improvements in US physical therapists management of the critically-ill indicated that this was attributable to appropriate, entry-level, curriculum content [16]. The core-knowledge and awareness of handling articular cartilage lesions may have a similar foundation at the initial training available to UK musculoskeletal (MSK) therapists.
MSK medicine is established in UK undergraduate healthcare curriculum [17]; it is not widely reported as to how the subtlety of articular cartilage tissue quality, injury, repair and rehabilitation is taught at this level across MSK therapies. This understanding is the foundation for therapists working with ACR; a previous review detailed that the standard of studies for ACR were of a higher quality when a rehabilitation therapist was party to the authorship [18]. The demand on the availability of such therapists will increase as ACR procedures become common place in an NHS setting. Potentially rehabilitators can be sourced from a range of any qualified provider of MSK therapies with the advent of Commissioning Groups under recent UK health reforms [19]. General Practitioners will have to respond to patients’ informed choice given that the reported confidence of handling MSK conditions by GP’s is low as a consequence of shifting priorities in medical school curricula [20].
The potential range of MSK providers may differ in terms of entry-level skill set and their practical application of curricula requirements. Comparative curriculum review across such a range of healthcare providers is challenging; in North America, the use of a Curriculum Inventory Standard to enable education programme comparison is being explored to mitigate the diversity in interpretation of requirements [21]. This suggests that inter-MSK therapy course comparison is rare although assessment is implicit within UK-regulated individual healthcare degree-level course providers. The Quality Assurance Agency (QAA) for Higher Education (HE) establishes codes for educational provision and academic standards that are generic across degree-awarding institutions and partnerships [22]. The course content itself is a reflection of the demands of the practice standards that govern the professional conduct of MSK therapies [23-26]. Stand-alone curriculum assessment can be multi-factorial in approach: conformity to standards; problem-based approaches; peer evaluation; student experience; course-review and baseline knowledge are key elements [15,27-31]. This reflection by research complements the QAA guarantee of HE quality and regulators enforcing curricula that instil gross base standards per institution. Modular content will then distil these standards through individual or sessional dissemination subjected to the interpretation of the course administrators and lecturers. Determining variability in interpretation in various MSK curricula for the management of singular conditions or topic areas has not been explored.
Aims and Objectives
The aim of this study was to complete a census to determine the coverage of articular cartilage-specific content within MSK therapy undergraduate curriculum.
The research question was: do UK musculoskeletal therapy courses differ in specific articular cartilage content based on the final professional membership award?
The primary objective was to explore how MSK therapy course content reflects current articular cartilage considerations using a scored questionnaire with a cross-sectional survey approach. This was with a view to possibly identify limitations in undergraduate curriculum content within specific MSK professions and determine candidature for subsequent specific knowledge transfer initiatives. Secondary objectives were to investigate the characteristics of the courses that report variable content in the consideration of articular cartilage; a priori selection of course duration, HE level for content delivery and course entry requirements were determined.
Alternative hypotheses
There is a significant difference in the scoring of reported curriculum content regarding articular cartilage between undergraduate MSK therapies based on professional membership.
Methods
Design
Cross-sectional survey using an online questionnaire.
Procedure
The study deployed an online questionnaire; the questions were developed in order to support the stated primary and secondary objectives. The instrument was developed in the Bristol Online Survey (BOS, University of Bristol, 2014) software platform; the following summarises the sections and questions comprising the instrument.
Section1 - articular cartilage: This was composed of 4 main questions that dealt with content of the MSK therapies’ undergraduate courses. Questions 1-4 dealt with articular cartilage (AC) physiology, arthrokinematics, surgical techniques and rehabilitation; each was composed of four further sub-questions concerning specific element coverage. Responses were scored with one point awarded for each cartilage element selected as covered. Answers for 'No', 'Not known' or 'Prefer not to say' were scored as zero. The total maximum score possible for any single responder was 16. Each sub-question also enquired as to the positioning of ACR in HE and allowed for any other comments the respondents were willing to provide on the topic.
Section 2 course details: This required nominal details for the course offering in question, captured the following:
• Title of the full-time musculoskeletal undergraduate course.
• Qualification gained.
• Awarding institution details.
• Entry requirements.
• Duration of the course.
• Regulatory standards and professional competencies supporting course validation.
Participants
The Universities and Colleges Admissions Service (UCAS) online database was selectively searched to identify UK only HE course providers of musculoskeletal therapies. Excel (2010 v14, Microsoft) was used to store course website details and email addresses for delivery of the questionnaires. The curriculum course leaders and key personnel were identified through manual verification on individual university websites via course-specific content.
Inclusion/exclusion criteria: Any tertiary educational establishments offering an undergraduate degree level programme in a regulated musculoskeletal therapy available on UCAS was included. This was drawn from the following disciplines: physiotherapy, osteopathy, chiropractic and sports therapy. The courses had to be affiliated to professional, regulated bodies and map curriculum to practice standards. Any non-UK, non-degree, post-graduate, discontinued course was excluded despite relevance in the field.
Distribution
Participants were invited via email (Microsoft Outlook Web App, v14.3) to complete the questionnaire using an embedded hyperlink to the instrument. Invitations were personalised based on the details on course personnel held on the university websites. Subsequent email reminders to participate were sent at 3, 6 and 10 week intervals. The questionnaire was piloted amongst the teaching staff of the University of Kent and European School of Osteopathy unaffiliated with course provision; no revisions arose from the pilot. It was hoped to achieve a 95% response rate to comply with the census approach; 89 of 107 UCAS listed, potential participating institutions [32]. Recruitment took place between December 2014 and April 2015.
Ethics: Ethical consideration and approval was provided by the Research Ethics Committee of the University of Kent.
Analysis
Summary descriptive and inferential statistics were calculated; to determine potential differences between the various professions, characteristics of the HE providers/courses and mean rank answer scores, the Kruskal-Wallis test was run with pair wise Mann-Whitney U post-hoc testing. All data were recorded and analysed using a combination of Excel to generate pivot tables and SPSS (v21, IBM) for non-parametric tests.
Results
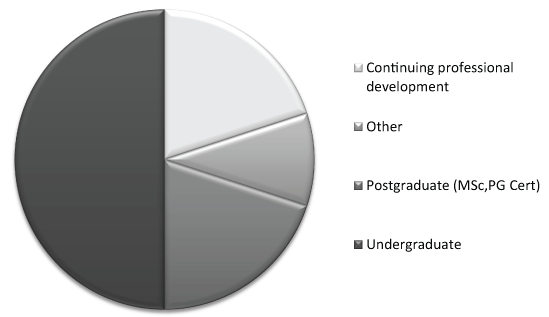
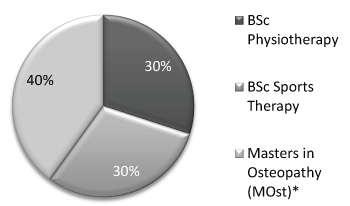
Refinement (duplicate and foundation degree filtering) of the 107 UCAS listed courses led to 76 participants identified as course leaders or primary course contacts and invited to take the questionnaire (physiotherapy: 34, sports therapy: 33, osteopathy: 6, chiropractor: 3). Eleven responses were received (14% response rate) but only 10 were explicitly referring to undergraduate courses and suitable for analysis. The proportion of final qualification of the reported courses is represented in Figure 1 and the regulatory bodies underpinning the individual curriculum can be viewed in Figure 2.
.
Figure 1: Qualifications issued by respondent's institution.
*Integrated Masters is an undergraduate programme
View Figure 1
.
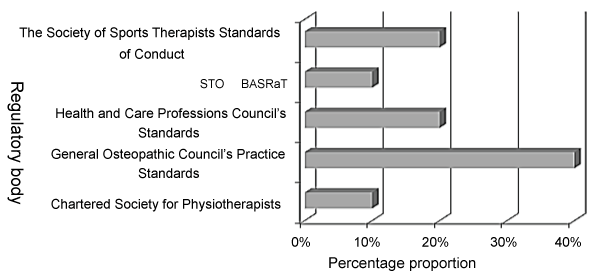
Figure 2: Respondents regulatory practice standards supporting curricula.
NB. STO - Sports Therapy Organisation; BASRaT - British Association of Sport Rehabilitators and Trainers
View Figure 2
The participants' course requirements ranged from AAB to BCC A-Level grades with generally lower entry requirements for the Masters in Osteopathy (MOst) (Table 1); course duration ranged from 3 to 4 years with shorter longevity reported for the BSc programmes. Mean scores were: physiotherapy 11.33 (± 4.16), sports therapy 13.67 (± 3.21), osteopathy 8.5 (± 2.89). No significant difference was found between content scores based on award or entry requirements although scores were reportedly higher for the sports therapy programmes.
![]()
Table 1: Curriculum characteristics, questionnaire summary scores and levels of significance between groups.
View Table 1
![]()
Table 2: AC elements percentage content reporting and corresponding HE level.
View Table 2
The summary of coverage of articular cartilage content (Table 2) demonstrates that the respondents reported the main elements of physiology, injury and repair were represented on their respective programmes. The surgical repair procedural elements were not widely included in curriculum content (the exception being sports therapy with 67% claiming coverage) and calculated scores for this question were significantly lower than other responses (p < 0.05). There was, however, no statistically significant difference between scores for the individual surgery elements (p > 0.05). Surgical rehabilitation content was commonly reported; post-surgery protocols were covered in all BSc responders and 50% of MOst responders. HE levels for content were spread across the range available for tertiary education (4-7); level 7 is representative of Master's level study and was reported for osteopathy (MOst) and sports therapy (BSc) programmes. Individual course titles where the ACR elements were taught were typically reported as anatomy and physiology with some nuances based around the core provision (Table 3). The responses to questioning on the ideal positioning of ACR within HE programmes suggested equivocal attitudes on the topic (Figure 3); fifty percent of responders were supportive of material at undergraduate level with the remainder advocating CPD and postgraduate courses.
![]()
Table 3: Course titles representing ACR content.
View Table 3
Discussion
The aim of this study was to complete a census to determine the coverage of articular cartilage-specific content within MSK therapy undergraduate curriculum. In terms of exploring if UK musculoskeletal therapy courses differ in articular cartilage content based on final professional membership, no statistically significant difference was found between responders' professions and the reporting of specific articular cartilage content. This is potentially suggestive of alignment in content within the responding groups. The trend in calculated scores indicated greater content coverage within the sports therapy courses but this was not statistically significant. Other grouping characteristics such as entry requirements and course duration were also seen to have no effect on scoring outcome.
Healthcare curriculum content has to meet QAA requirements but effectively researching cross-curriculum is challenging and may make comparison difficult. Mapping to common terminology is possible [33]; this facilitates minutiae overview but does not directly describe the context in which the topic is delivered and requires MESH terms to be embedded as key curriculum metadata. Novel adoption of MESH and automatic term mapping at curriculum design phase may expedite research in this area. This 'big data' can lend itself to further visual exploration through emerging technologies and Web 3.0 development [34]. Lack of a clear, topic-based, curriculum mapping structure may have limited the responses in this current study; documented learning outcomes and course content are possibly too generic to facilitate detailed examination.
Models of curriculum design may be a factor influencing reporting as institutional nuances potentiate heterogeneity. The responses may be indicative of content for providers that use a constructive alignment for curriculum development based around learning outcomes [35]. The low response rate could indicate that institutions using organic approaches to curriculum design were unable to fulfil engagement as prescribed outcome is offset by students' inquiry-based learning [36]; no absolutes are possible at the detailed level required by this study. Consequently further consideration should be given to how students perceive content is covered and how they see curriculum development preparing them for practice in MSK disciplines [37,38].
The recent NICE draft proposal [39] on limiting use of third-generation ACR to research-only proposals may indicate that this is not wholly suitable as an area to gauge curriculum conformity. It also potentially informs why recognition of surgical procedural elements was limited; possible evidence of the difficulty sourcing research material and enhancing practice knowledge reported in other areas of healthcare [40]. Micro fracture technique is routine practice within the NHS [41] but this procedure was not indicated over other ACR approaches in this study. The issues of knowledge transfer and lack of expedient adoption of research findings into practice are implicated to some extent [42]; over 25 years of research data detail the ACR procedures in question [43] yet these surgical options had lowest reported representation across all professions.
The lack of adoption of a definitive approach to ACR has potentially influenced the reported knowledge of surgical approaches in this study. There is recognition that generic rehabilitation principles may be limited [44] and recommendations suggest that specific and targeted rehabilitation has not been sufficiently explored [43]. ACR has potential requirement for specialist physical therapy dependent on the individual patient and approach used [45]. Although generic protocols are reportedly presented at undergraduate level, the need to specialise around ACR is arguably a post-graduate area and requires further exploration before adoption into wider musculoskeletal therapy curriculum. The findings reported here may be subject to a Pygmalion effect in that a desire to meet the expectations and aspirations of research-led education influenced responders [46]. Individuals may have answered with a more positive bias to conform to the professional expectations demanded by regulation.
Generic rehabilitation protocols may fail to engender the nuances required for individuals [14,47]; the ability to recognise the necessary adaptations or specialisation may also be indicative of the complex processing developed at HE Level 7 and above [48]. Undergraduates are becoming increasingly expected to deal with uncertainty and complexity by potentially working with pedagogues as peers from early stages of HE [49]. The conflicting levels reported in this study with BSc programmes stating Level 7 content may be indicative of this shift in education. The lack of unequivocal reporting of positioning of material certainly suggests uncertainty in dealing with ACR elements and further uncertainty regarding the depth of knowledge and understanding to achieve professional competency at undergraduate level.
A focus on patient engagement, self-care and compliancy is a potential path that complements the professional competency required to recognise individual patient needs. This requires further innovative use of ubiquitous technology but has been limited due to inconsistency in study design and failure to conceptualise appropriate intervention strategies [50]. Potential to maximise therapist and patient interaction has not been fully explored using the new Web 2.0 and 3.0 developments or mobile device applications. In light of the uncertainty suggested by this study, development of a multi-media clinical technology interface delivering best practice advice for patients and MSK therapists is warranted. This may go some way to offset potential variability in practitioner competence by providing consistency of approach underpinned by the latest evidence.
Limitations of this study include the use of a non-validated instrument, sample size and suitable access to the necessary key personnel. The potential to increase response rate possibly resides with a multi-media approach [51]; although optimal strategies were followed, the burden of workload in academia may have been prohibitive. Perceived competitive advantage between professions may also be a possible reason why the response rate was low, restricting generalisation of the findings. Chiropractic is not represented in the responders although investigation into curriculum mapping within the profession has surfaced outside of the UK [52,53]. The focus has previously been on looking at evidence-based content regarding commonly treated conditions and preparedness to practise. It is possible that the field of articular cartilage repair and rehabilitation is considered to be outside this evidence-based remit. This may be of concern given that 80% of knee cartilage defects will continue to degrade and 1 in 2 patients that present for treatment will suffer with the sequelae of this condition [54].
Future work requires using shared meta-data within curriculum design to allow potential mapping across providers. Repeated efforts are required to ensure curriculum content analysis becomes both an educational and healthcare research activity in MSK medicine. Further institutional strategies and innovative approaches to designing and reporting curriculum will be vital in determining how suitable research is integrated into the student experience.
Conclusion
The findings of this study provides some indication of the level of detail on articular cartilage physiology, arthrokinematics and rehabilitation considerations as represented in undergraduate curricula within UK MSK therapy courses. The current approaches to rehabilitating ACR patients post-surgery were not consistently represented but generic protocols were well-reported at an undergraduate level. Considerations for subsequent research are: how to measure research translation into curriculum content and which curriculum model best supports this; how to ensure student practitioners are provided with suitable contemporary knowledge to provide patient-centred, evidence-based care through programme delivery.
References
-
Keiffer MR (2015) Utilization of clinical practice guidelines: barriers and facilitators. Nurs Clin North Am 50: 327-345.
-
Pryce R Davis, Rosemary S Russ (2015) Dynamic framing in the communication of scientific research: Texts and interactions. Journal of Research in Science Teaching 52: 221-252.
-
Beach MC, Price EG, Gary TL, Robinson KA, Gozu A, et al. (2005) Cultural competency: A systematic review of health care provider educational interventions. Medical care 43: 356.
-
Ivkovic A, Vukasovic A, Porter RM, Hudetz D, Pecina M, et al. (2014) Gene Therapy in Articular Cartilage Repair. Developing Insights in Cartilage Repair.
-
Cross M, Smith E, Hoy D, Nolte S, Ackerman I, et al. (2014) The global burden of hip and knee osteoarthritis: estimates from the global burden of disease 2010 study. Ann Rheum Dis 73: 1323-1330.
-
Rankin G, Rushton A, Olver P, Moore A (2012) Chartered Society of Physiotherapy's identification of national research priorities for physiotherapy using a modified Delphi technique. Physiotherapy 98: 260-272.
-
Donaldson J, Tudor F, Mcdermott ID (2015) (iv) Treatment options for articular cartilage damage in the knee. Orthopaedics and Trauma 29: 24-30.
-
Bekkers JE, Inklaar M, Saris DB (2009) Treatment selection in articular cartilage lesions of the knee: a systematic review. Am J Sports Med 37 Suppl 1: 148S-55S.
-
Campbell KA, Saltzman BM, Mascarenhas R, Khair MM, Verma NN, et al. (2015) Does Intra-articular Platelet-Rich Plasma Injection Provide Clinically Superior Outcomes Compared With Other Therapies in the Treatment of Knee Osteoarthritis? A Systematic Review of Overlapping Meta-analyses. Arthroscopy 31: 2213-2221.
-
Saris D, Price A, Widuchowski W, Bertrand-Marchand M, Caron J, et al. (2014) Matrix-Applied Characterized Autologous Cultured Chondrocytes Versus Microfracture Two-Year Follow-up of a Prospective Randomized Trial. The American journal of sports medicine 42: 1384-1394.
-
Marcacci M, Filardo G, Kon E (2013) Treatment of cartilage lesions: what works and why? Injury 44 Suppl 1: S11-15.
-
NICE (2005) National Institute for Health and Care Excellence
-
Edwards PK, Ackland T, Ebert JR (2014) Clinical Rehabilitation Guidelines for Matrix-Induced Autologous Chondrocyte Implantation on the Tibiofemoral Joint. J Orthop Sports Phys Ther 44: 102-119.
-
Hambly K, Bobic V, Wondrasch B, Van Assche D, Marlovits S (2006) Autologous Chondrocyte Implantation Postoperative Care and Rehabilitation Science and Practice. The American Journal of Sports Medicine 34: 1020-1038.
-
Thomson D, Boyle D, Legg C, Owen M, Newman M, et al. (2014) Clinical Placements: The Perspectives of UK Physiotherapy Students on How Prepared They Were By Their University For Their First Clinical Placements: An Example of One HEI. International Journal of Practice-based Learning in Health and Social Care 2: 69-79.
-
Ohtake PJ, Strasser DC, Needham DM (2013) Translating research into clinical practice: the role of quality improvement in providing rehabilitation for people with critical illness. Phys Ther 93: 128-133.
-
Oluwajana F, Rufford C, Morrissey D (2011) Exercise, sports and musculoskeletal medicine in UK medical school curricula: a survey. British Journal of Sports Medicine 45.
-
Bright P, Hambly K (2013) Has the Standard of the Reporting of Rehabilitation Improved in Articular Cartilage Repair Studies Involving Third-Generation Autologous Chondrocyte Implantation in the Knee? A Systematic Review. J Sport Rehabil.
-
Jones H (2013) Any qualified provider: facilitating patient choice. Nurs Times 109: 22-23.
-
Wise EM, Walker DJ, Coady DA (2014) Musculoskeletal education in general practice: a questionnaire survey. Clin Rheumatol 33: 989-994.
-
Ellaway RH, Albright S, Smothers V, Cameron T, Willett T (2014) Curriculum inventory: Modeling, sharing and comparing medical education programs. Med Teach 36: 208-215.
-
QAA (2014) UK Quality Code for Higher Education.
-
CSP (2010) Learning & Development Principles
-
GCC (2010) Code of Practice and Standard of Proficiency.
-
GOSC (2012) Standards of Practice.
-
SST (2008) Standards of Proficiency.
-
Lisk K, Flannery JF, Loh EY, Richardson D, Agur AM, et al. (2014) Determination of Clinically Relevant Content for a Musculoskeletal Anatomy Curriculum for Physical Medicine and Rehabilitation Residents. Anatomical Sciences Education 7: 135-143.
-
Dombrowski HT, Vincent OD, Wiley CL (2013) Prevention curricula assessment of osteopathic medical schools in the United States. International Journal of Osteopathic Medicine 16: 207-211.
-
Wass V (2013) Evidence-based practice: missed learning opportunities in undergraduate primary care? Educ Prim Care 24: 312-313.
-
Hartup JK, Murphy RA, Plowman LM, Myers R (2010) Progression through osteopathic training in Australia: The student experience. International Journal of Osteopathic Medicine 13: 160-165.
-
Panzarella KJ, Manyon AT (2007) A model for integrated assessment of clinical competence. J Allied Health 36: 157-164.
-
UCAS (2014) UCAS Search [Online].
-
Komenda M, Schwarz D, Å vancara J, Vaitsis C, Zary N, et al. (2015) Practical use of medical terminology in curriculum mapping. Comput Biol Med 63: 74-82.
-
Vaitsis C, Nilsson G, Zary N (2014) Visual analytics in healthcare education: exploring novel ways to analyze and represent big data in undergraduate medical education. PeerJ 2: e683.
-
Biggs JB (2011) Teaching for quality learning at university What the student does. McGraw-Hill Education UK.
-
Healey M (2005) Linking research and teaching exploring disciplinary spaces and the role of inquiry-based learning. Reshaping the university: new relationships between research, scholarship and teaching 67-78.
-
Healey M (2014) Students as partners in learning and teaching in higher education. In: Workshop Presented at University College Cork.
-
Mandrusiak AM, Isles R, Chang AT, Choy NL, Toppenberg R, et al. (2014) Senior physiotherapy students as standardised patients for junior students enhances self-efficacy and satisfaction in both junior and senior students. BMC medical education 14: 105.
-
NICE (2015) National Institute for Health and Care Excellence.
-
Cho N, Gilchrist C, Costain G, Rosenblum N (2011) Incorporating evidence-based medicine in the undergraduate medical curriculum: early exposure to a journal club may be a viable solution. University of Toronto Medical Journal 88: 154-155.
-
Clar C, Cummins E, Mcintyre L, Thomas S, Lamb J, et al. (2005) Clinical and cost-effectiveness of autologous chondrocyte implantation for cartilage defects in knee joints: systematic review and economic evaluation. Health Technology Assessment 9.
-
Damschroder LJ, Aron DC, Keith RE, Kirsh SR, Alexander JA, et al. (2009) Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implement Sci, 4: 50.
-
Biant LC, McNicholas MJ, Sprowson AP, Spalding T (2015) The surgical management of symptomatic articular cartilage defects of the knee: Consensus statements from United Kingdom knee surgeons. Knee 22: 446-449.
-
Clark NC (2015) (vii) The role of physiotherapy in rehabilitation of soft tissue injuries of the knee. Orthopaedics and Trauma 29: 48-56.
-
Schmitt LC, Quatman CE, Paterno MV, Best TM, Flanigan DC (2014) Functional outcomes after surgical management of articular cartilage lesions in the knee: a systematic literature review to guide postoperative rehabilitation. Journal of Orthopaedic & Sports Physical Therapy 44: 565-A10.
-
Dauvrin M, Lorant V (2015) Leadership and cultural competence of healthcare professionals: a social network analysis. Nurs Res 64: 200-210.
-
Mithoefer K, Hambly K, Logerstedt D, Ricci M, Silvers H, et al. (2012) Current concepts for rehabilitation and return to sport after knee articular cartilage repair in the athlete. Journal of Orthopaedic & Sports Physical Therapy 42: 254-273.
-
QAA (2008) The Framework for Higher Education Qualifications in England, Wales and Northern Ireland.
-
Healey M, Jenkins A, Lea J (2014) Developing research-based curricula in college-based higher education. York.
-
Button K, Roos PE, Spasic I, Adamson P, van Deursen RW (2015) The clinical effectiveness of self-care interventions with an exercise component to manage knee conditions: A systematic review. Knee 22: 360-371.
-
McPeake J, Bateson M, O'Neill A (2014) Electronic surveys: how to maximise success. Nurse Res 21: 24-26.
-
Gorrell L, Beirman RL, Vemulpad SR (2015) Curriculum mapping within an Australian master of chiropractic program: Congruence between published evidence for chiropractic and student assessment tasks. The Journal of chiropractic education 29: 29.
-
Saranchuk R, Watkins T (2000) Analysis of the relationship between program design and professional practice in CMCC's undergraduate chiropractic program. The Journal of the Canadian Chiropractic Association 44: 230.
-
Gomoll A, Filardo G, De Girolamo L, Esprequeira-Mendes J, Marcacci M, et al. (2012) Surgical treatment for early osteoarthritis. Part I: cartilage repair procedures. Knee surgery, sports traumatology, arthroscopy 20: 450-466.