Journal of Family Medicine and Disease Prevention
The Effect of Integrated TCM with Chemotherapy on Quality of Life and TCM Syndrome
Tsai-Ju Chien1,2*, Chung-Hua Hsu2,3, Shang-Chih Chang2,3, Yu-Yu Chang4 and Fang-Yu Li5
1Division of Oncology, Taipei City Hospital, Taiwan
2Institute of Traditional Medicine, National Yang-Ming University, Taiwan
3Branch of Linsen and Chinese Medicine, Taipei City Hospital, Taiwan
4Department of Pharmacy Practice, Tri-Service General Hospital, Taiwan
5Institute of Health Policy and Management, National Taiwan University, Taiwan
*Corresponding author: Tsai-Ju Chien, Branch of Zhong-xing, Taipei City Hospital, Institute of Traditional Medicine, School of Medicine, National Yang-Ming University, 4F, No7, Lane 51, Rd. Gin-Lin, Zhongshan Dist., Taipei City 104, Taiwan, Tel: +886-979305521, E-mail: silence021@gmail.com
J Fam Med Dis Prev, JFMDP-3-049, (Volume 3, Issue 1), Original Article; ISSN: 2469-5793
Received: December 23, 2016 | Accepted: January 20, 2017 | Published: January 23, 2017
Citation: Tsai-Ju C, Chung-Hua H, Shang-Chih C, Yu-Yu C, Fang-Yu L (2017) The Effect of Integrated TCM with Chemotherapy on Quality of Life and TCM Syndrome. J Fam Med Dis Prev 3:049. 10.23937/2469-5793/1510049
Copyright: © 2017 Tsai-Ju C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: To evaluate the benefit of Traditional Chinese Medicine (TCM) in improving the quality of life (QOL) and TCM syndrome in cancer patients undergoing chemotherapy.
Methods: Sixty-one cancer patients from the oncology and integrated therapy wards in Taipei City Hospital who met the inclusion criteria were enrolled through consultation with their doctors. Participants were allocated to chemotherapy group (n = 31) or integrated therapy group (n = 30). All participants completed the QOL questionnaires and received TCM syndrome analysis. Data were collected before and after eight weeks of treatment and analyzed by using statistical analysis software SPSS V.19.0.
Results: After eight weeks of treatment, significant reductions were found in all aspects of QOL in the chemotherapy group, including physical (p = 0.007), psychological (p = 0.014), social (p = 0.030) and environmental (p = 0.015). The proportion of chemotherapy group participants with TCM Qi deficiency (qìxū) and Yin deficiency (yīnxū) syndromes increased significantly (p = 0.010; p = 0.023). The physical aspect of QOL in the integrated therapy group improved significantly (p = 0.041), and no increasing proportions of Qi or Yin deficiency syndromes were noted (p > 0.05). Correlational analysis showed that Qi deficiency had the most significant impact on QOL (p = 0.01).
Conclusion: Results of this study show that cancer patients who receive integrated therapy have better QOL and lower incidence of Qi deficiency syndrome than patients receiving chemotherapy alone. Further research is warranted to evaluate the clinical efficacy of integrated treatment with TCM.
Keywords
Cancer, Chemotherapy, Integrated therapy, Traditional chinese medicine, Quality of life (QOL)
Introduction
Epidemiological studies have revealed that cancer incidence increases year by year, making cancer one of the leading causes of death globally. Thus, healthcare institutions and physicians are paying much attention to cancer-related issues. In recent decades, the treatment modalities for cancer have updated, although the primary treatments for cancer are still chemotherapy and radiotherapy. Cancer treatment guidelines developed and published by the National Comprehensive Cancer Network (NCCN) have been widely accepted and adopted for universal application [1].
During cancer treatment, most patients experience certain cancer-related symptoms, including dizziness, fatigue, nausea, vomiting, dry mouth with mucositis, shortness of breath, night sweats, and bone marrow suppression, which may be related to the use of anti-cancer agents or to the disease itself [2,3]. Therefore, many patients seek for complementary or integrative therapy beyond the standard or mainstream medical treatment [4,5]. Some complementary therapies, such as Traditional Chinese Medicine (TCM), may help to relieve certain symptoms associated with cancer or side effects related to cancer treatment, improving patient's sense of well-being [6,7]. In recent years, TCM-based herbal medicines have gained increasing acceptance worldwide. Some pharmaceutical companies also view TCM as rich resources for drug discovery [8]. In TCM theory, yin and yang are used extensively to explain the histological structure, physiological function and pathological changes of the human body, and to serve as a guide for diagnosis or treatment. People can only stay healthy within a condition of yin/yang dynamic balance or harmony. Meanwhile, the Qi (energy) and blood represent the dynamic energy and nutrition status of the body. Disturbances or imbalances of yin/yang or Qi/Blood will lead to disease and related symptoms. Thus, in TCM theory, the differential diagnosis of cancer-related symptoms is based on TCM syndrome, which is a group of components related to the deficiency or stasis of yin/yang and Qi/Blood. The criteria of these deficiency syndromes were noted in table 1. In previous cancer research [5], we divided the cancer-related TCM deficiency syndrome into four categories: Qi deficiency (qìxū); Blood deficiency (xuèxū); Yin deficiency (yīnxū); and Yang deficiency (yángxú). The symptom of Qi deficiency has been proven to have a high correlation with cancer-related fatigue and reduced quality of life [QOL] [9]. The principle of applying TCM treatment to cancer patients is to supply the Qi that corresponds to human energy levels.
![]()
Table 1: Classification criteria for the diagnosis of TCM deficiency syndrome groups.
View Table 1
Meanwhile, no clinical data are available from studies evaluating whether the integration of chemotherapy with TCM will improve QOL and TCM syndrome in cancer patients. Accordingly, this study aimed to assess QOL and TCM syndrome in cancer patients receiving chemotherapy alone or integrated therapy (chemotherapy combined with TCM).
Participants and Methods
Research design and participants
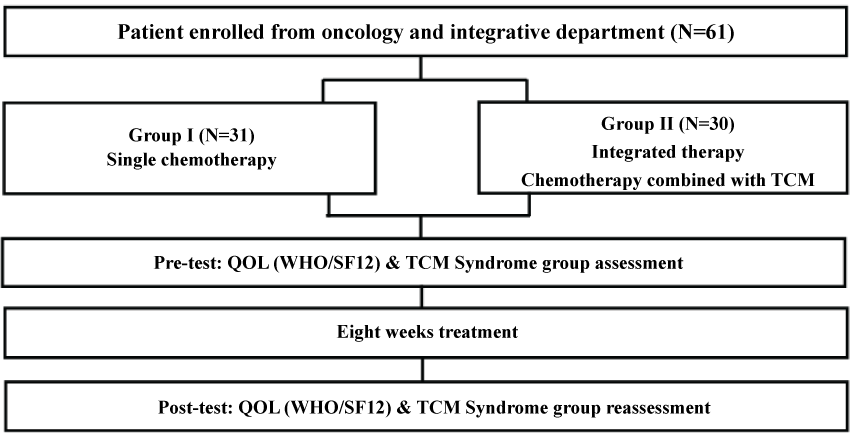
The study protocol and design were reviewed and approved by the Taipei City Hospital Institutional Review Board (reference number: TCHIRB-10). Verbal and written informed consent were obtained from all participants after informing them the study design, intervention, data collection, and the rights of participants. Patients choose to receive integrative therapy or only chemotherapy based on heir wills for ethnic consideration; hence this is an observational, cross-section, non-randomized study. Group one was cancer patients undergoing chemotherapy alone, and the other group was cancer patients undergoing integrated therapy, including chemotherapy combined with TCM treatment. Accordingly, we enrolled patients from the oncology ward at Taipei City Hospital. After consulting with their physicians, patients chose either chemotherapy or integrated therapy (chemotherapy combined with TCM treatment) as their intention. Figure 1 shows the flowchart of the research design and participant enrollment in this study.
.
Figure 1: The flowchart of the research design and participant enrollment in this study.
View Figure 1
Inclusion and exclusion criteria: Patients were required to meet inclusion criteria as follows:
1) Patients diagnosed with metastatic cancer (Cancer stage IV) and under active treatment.
2) Eastern Cooperative Oncology Group (ECOG) performance scores [10] < = 2 and aged 20 to 75 years.
3) Currently undergoing chemotherapy for at least eight weeks.
4) Able to understand the purpose and process of this study and provide signed informed consent.
Patients were excluded if any of the following criteria were present:
1) Terminal disease or life expectancy < 3 months.
2) The presence of psychiatric problems.
3) Completion of the chemotherapy treatment course.
4) Development of a significant event (e.g., surgery, acute myocardial infarction, severe infection such as pneumonia, or under ventilator use) is causing withdrawal from the study.
5) Any other condition the physician-in-charge deemed would make the patient unsuitable for the study.
TCM syndrome assessment
All participants in both groups were evaluated by qualified TCM doctors and an oncologist to complete the TCM syndrome assessment before and after eight weeks treatment.
TCM practitioners determine diagnoses regarding Yin (yīn), Yang (Yáng), Qi (qì), and Blood (xuè), as well as organ imbalances identified by signs and symptoms observed by the doctors and reported by the patients. If patiens have been noted with more than one deficiency syndromes, they will be categorized into the group of which they suffered more according to TCM doctors' evaluation. Table 1 shows the TCM syndrome groups categorized according to the ancient TCM theory. Four related groups are Qi deficiency; blood deficiency; Yin deficiency; and Yang deficiency, as previously described [11]. Validation testing showed that the validity and reliability of the diagnostic criteria were well defined with an alpha coefficient of 0.89 and Cronbach's alpha coefficient of 0.88 [12] (Table 1).
QOL measurement
We assessed patients' QOL using the World Health Organization QOL (WHOQOL-BREF) and Short-Form Health Survey (SF-12) questionnaires before and after eight weeks of treatment to compare the changes in QOL after treatment and differences in QOL between the two study groups. The WHOQOL-BREF instrument is a validated and well-accepted scale for general health-related QOL research [12,13]. The scale comprises 26 items, measuring the following broad domains: physical health, psychological health, social relationships and the environment. The SF-12 is a multipurpose short-form survey with 12 questions, all selected from the more comprehensive SF-36 Health Survey [14,15]. The questions are combined, scored, and weighted to create two scales that provide glimpses into the mental and physical functioning and overall health-related QOL. The official SF-12 is weighted and summed to provide easily interpretable scales for evaluating physical and mental health [14]. The Physical and Mental Health Composite Scores (PCS & MCS) are then computed using the scores of twelve questions ranging from 0 to 100, where a zero score indicates the lowest level of health and 100 indicates the highest level of health [16].
Results
Characteristics of the participants
Table 2 presents the baseline characteristics of the two groups. The average age of chemotherapy group participants (64.1 y/o) was higher than that of the integrated therapy group (49.2 y/o). Gender distribution was also significantly different between groups. A higher percentage of females chose integrated therapy than those that chose chemotherapy along, which may correspond to having more breast cancer patients in the integrated therapy group. Despite age and gender distribution, patients' performance and treatment strategies (most are receiving curative treatment) were similar between the two groups (Table 2).
![]()
Table 2: Demographic characteristics of study participants.
View Table 2
QOL comparison between chemotherapy and integrated therapy groups
Table 3 shows QOL measured in the two groups before and after eight weeks of treatment. Among patients who received chemotherapy alone (chemotherapy group), significant reductions were noted after eight weeks of treatment in all domains of the WHOQOL-BREF, including physical (p = 0.007), psychological (p = 0.014), social (p = 0.030) and environmental areas (p = 0.015). In contrast, patients receiving integrated therapy had significant increases in physical health scores of the WHOQOL-BREF (p = 0.041), while no specific changes were noted in the other domains.Overall, results of the WHOQOL-BREF showed that the integrated therapy group demonstrated QOL improvements (55.7:61.2, p = 0.041) while the chemotherapy group demonstrated a decline in QOL (63.5: 57.7, p = 0.007) as shown in table 3.
![]()
Table 3: Comparison the WHO-BREF & SF-12 quality of life scores between chemotherapy and integrated therapy.
View Table 3
Regarding QOL measurement using the SF-12 questionnaire, patients receiving chemotherapy alone experienced a greater decline in mental health scores (p = 0.008) than in physical health scores (p = 0.083), while no obvious changes were noted in these scores in the integrated therapy group (Table 3).
Comparison of TCM syndrome between the chemotherapy and integrated therapy groups
Table 4 presents the results of TCM syndrome evaluation between the two groups. Before the study, the only difference in TCM syndrome was the proportion of Yin deficiency, which was higher in the integrated therapy group than in the chemotherapy group (33.3%:3.1%, p = 0.003). However, after eight weeks of treatment, the proportion of Yin deficiency increased significantly in patients receiving chemotherapy alone (p = 0.023), and a significant difference was also noted in the percentage of Qi deficiency (p = 0.010). However,no noticeable changes were observed in TCM deficiency syndrome in the integrated therapy group. Patients who underwent chemotherapy alone experienced greater levels of Qi and Yin deficiency-related TCM syndrome than those receiving integrated treatment (Table 4).
![]()
Table 4: The comparison of TCM deficiency syndrome between chemotherapy and integrated therapy.
View Table 4
Correlations between different TCM syndrome components and QOL
Table 5 presents the results of correlation analysis between the four different TCM deficiency syndromes and QOL. Only Qi deficiency syndrome was noted to correlate significantly with poor QOL. Significant differences were identified in the scores of each domain of the WHOQOL-BREF scale, including the physical (p < 0.001), psychological (p < 0.001), social (p = 0.011) and environmental (p = 0.004) domains. In the SF-12 scale, both the mental and physical health scores of QOL were significantly lower in patients with Qi deficiency than in other patients (p < 0.001). No significant correlations were found between the other three TCM deficiency syndromes and QOL (Table 5).
![]()
Table 5: The correlation of different TCM deficiency syndrome with quality of life.
View Table 5
Discussion
The effects of integrated therapy on QOL
Results of the present study show that patients benefit from receiving integrated therapy as demonstrated by improvements in QOL. The average ages in the integrated therapy group were younger (49.2 y/o) than those in the chemotherapy group (64.1 y/o). What's more, we noted that patients in the integrated therapy group had much lower physical health scores (55.7) even their average is younger than the other group. However, they experienced much greater improvement in physical health after the eight weeks of treatment compared to the chemotherapy group (55.7 > 61.2, p = 0.041 vs. 63.5 > 57.7, p = 0.007). Whether the younger patients have better adaptability or better response to TCM combined treatment could be an issue worth further discussion; at least, the contradictory significant difference shows that the physical health benefits of integrated therapy may overcome the age effect. The difference may also be explained by a greater response from integrated therapy and higher expectations of physical health among younger patients, so that they may be more active in seeking alternative (TCM) or integrative therapy. Also, a higher percentage of females chose integrated treatment, which may correspond to having more breast cancer patients in the integrated therapy group. This phenomenon indicates that younger patients having greater awareness, understanding and acceptance of integrative therapy, and also that female having a greater inclination to accept TCM. We assumed that these younger participants in the integrated group expect more considerable improvement in their health-related QOL as a result of treatment. In the present study, the patients who received integrated therapy were indeed satisfied with improvements in their physical health. A critical study addressed that Herbal medicine and western medicine may be considered as entirely separate distinctive entities and disciplines, but, in fact, both can be combined for better results [17]. To date, more and more Chinese herbs have been proven to have an anti-tumor effect through the mechanisms of anti-inflammatory action, immune modulation, and suppression of tumor growth [18-21]. Some recently published studies even show that TCM decoction may benefit colon cancer patients from autonomic dysfunction [22,23]. For example, the usual Qi supplied by the Chinese herb "Astragalus membranaceous" has been shown to affect proliferation, invasion, and apoptosis of cancer cells [24]. Also, the extract of Astragalus membranaceous has been used in treating cancer-related fatigue with a positive effect [25].
Our study is not the first study to show that TCM can be utilized as an adjuvant therapy to reduce chemotherapy toxicity and improve patients' QOL. Other studies have indicated that TCM may prolong survival, enhance immediate tumor response, and improve physical performance and energy in some cancer patients [26,27]. A recent systematic review found that some advanced cancer patients receiving chemotherapy can benefit from such adjuvant TCM ingredients as Codonopsis pilosula, Atractylodes macrocephaly, Poria Cocos, or Astragalus membranaceous; patients receiving these treatments had improved tumor response rates, survival, and QOL, as well as having fewer adverse events [28]. Accordingly, results of the present study have demonstrated that integrated therapy with TCM support leads to improvement in physical health and increases patients' energy levels.
Integrating TCM into cancer care
The different philosophies underlying Oriental and Western cultures have contributed to differences in the development of TCM and Western medicine practices. The TCM theory treats each human being as a unique universe. The concept of yin and yang is fundamental to the practice of TCM and is the foundation of understanding, diagnosing and treating health issues. At both primary and in-depth levels, TCM treatment seeks to balance yin and yang in each person. Accordingly, in TCM theory, "Qi" is the vital energy that maintains blood circulation, warms the body and fights disease [9]. Within the body, a dynamic flow automatically and continuously balances and rebalances the elements of yin and yang, Qi and blood. As such, the distinct principle of TCM helps human beings maintain health by using herbs or medications to modulate Yin/Yang and Qi/Blood imbalances. The theory base is owing to the properties of each herb are related to yin, yang, Qi, and blood. Since the syndrome differentiation of TCM plays a crucial role in the treatment of cancer patients, a complementary TCM medicine can be chosen based on the patients' TCM syndrome group, which can be Yin, Yang, Qi, and blood deficiency or excess [29]. For example, results of the present study indicate that cancer patients receiving chemotherapy alone have a high correlation with Qi and Yin deficiency. In integrated therapy using TCM with chemotherapy, this result suggests that a Qi supplement should be chosen for patients with Qi deficiency and a yin supplement for patients with yin deficiency. The mechanisms of Qi and yin deficiency syndromes may be related to changes in cytokine expression and bone marrow suppression [30], which are linked, in turn, to treatment with chemotherapy or radiotherapy. A recent published TCM decoction "Kuan-Sin-Yin" was noted with effect of improving autonomic nerve dysfunction through supply Qi and Yin based on TCM theory as well as regulating cytokine secretion in advanced colon cancer [22,23,19]. In this situation, no conflict is found between TCM theory and Western medicine. In fact, some scholars have proposed that the Yin-Yang theory may be applied to regulate cellular function through modulating cAMP and c/GMP concentration and NK cell activity [29,31,32]. Additionally, the regulation of Yin/Yang may also be of benefit to autonomic dysfunction, which refers to the control of granulocyte and lymphocyte activity by the sympathetic and parasympathetic nervous systems [33-35].
Another important concept of TCM is that "Qi" supply is a primary principle in the use of integrated therapy for cancer care. Studies have shown a high correlation between Qi deficiency and cancer-related fatigue [36,37]. Similarly, in the present study, a considerable proportion of Qi deficiency was found in the chemotherapy group. Accordingly, Qi supplements would be the necessary TCM medication for treating cancer patients and is worth further study. Related studies have evaluated whether Qi supplementary herbs with immunomodulatory and tumor suppressive effects can improve QOL in cancer patients [19,38,39]. Some herbs such as astragali radix and Poria cocos has been procvd with effect of Qi-supply and iummune enhancement in cancer patients [40,41]. To sum up, the TCM theory and Western medicine complement each other via the TCM focus on promoting energy (Qi) and harmony while Western medicine concentrates on suppressing tumor cells. However, as our results have shown, tumor cell suppression through chemotherapy often associates with the reduced energy and imbalances of the Yin/Yang and Qi/Blood found in cancer patients, which emphasizes the need for complementary TCM and integrated therapy [8].
The dilemma and prospects of integrating TCM in cancer care
TCM support is just part of the integrative therapy in cancer care. Studies have shown that Western medicine is the primary choice in the treatment phase, although study participants noted more side effects associated with chemotherapy and radiation. TCM was then applied in the recovery phase [42]. For participants in the present study, we considered the use of concurrent TCM with chemotherapy for relieving the related symptom such as pain, nausea/vomiting, and adverse effects of chemotherapy to improve patients' QOL and prolong their survival, as shown in previous studies [43,44]. Other studies support the use of TCM as a complementary therapy for cancer patients since TCM may enhance the potency of chemo/radiotherapy and reduce inflammation within the surrounding cancerous tissues [8]. However, the importance of communication between doctors and cancer patients should also be encouraged. In the present study, good cooperation between oncologists and the TCM doctors helped to avoid drug interactions and adjust the dosage of related medicines. Meanwhile, one of the difficulties in promoting integrated therapy lies in when it is not performed in a well-developed integrated medical center is that poor communication between doctors and patients may affect treatment adherence and may impair doctor-patient relationships.
The prospects of defining a role for TCM in integrative therapy for cancer care can be developed in two ways. The first way is to apply TCM philosophy and theory within integrated cancer therapy, especially since TCM accentuates taking the human being as a unique system and, accordingly, takes care of patients with holistic modulation and improvement of the whole body rather than removing the tumor mass or killing cancerous cells [8]. The second way to develop the role of TCM in cancer care is to evaluate the anti-cancer effects and underlying mechanisms of TCM-derived compounds or herbal extracts in larger and well-designed trials.
Limitation
As patients have free will to choose adopt TCM as an complementary therapy incurrent medical context; this was not a randomized trial, which could be a limitation of the study. Furthermore, the sample size of the study is too small to draw convincing results. However, this is just a preminary, observation study, providing us with a hint and direction to conduct further study relevant to TCM deficiency syndrome.
Conclusion
Results of the present study have shown that integrating chemotherapy with TCM improves QOL and TCM syndrome in cancer patients. Qi deficiency and Yin deficiency are the most common TCM syndrome components noted in cancer patients receiving chemotherapy. Further integration of TCM with Qi and Yin supplementary medicine would be a direction worth investigating in the future. For TCM to flourismore, h in integrative cancer care, new providers, new provider models, a realignment of incentives and a commitment to health promotion and disease management will be required.
References
-
NCCN - Evidence-Based Cancer Guidelines, Oncology Drug Compendium, Oncology Continuing Medical Education.
-
Wang XJ, Lopez SE, Chan A (2015) Economic burden of chemotherapy-induced febrile neutropenia in patients with lymphoma: a systematic review. Crit Rev Oncol Hematol 94: 201-212.
-
de Souza CM, Visacri MB, Ferrari GB, Tuan BT, Costa AP, et al. (2015) Nausea, vomiting and quality of life of patients with cancer undergoing antineoplastic treatment: an evaluation by pharmacists. Int J Pharm Pract 23: 357-360.
-
Huang SM, Chien LY, Tai CJ, Chen PH, Lien PJ, et al. (2015) Effects of symptoms and complementary and alternative medicine use on the yang deficiency pattern among breast cancer patients receiving chemotherapy. Complement Ther Med 23: 233-241.
-
Rossi E, Vita A, Baccetti S, Di Stefano M, Voller F, et al. (2015) Complementary and alternative medicine for cancer patients: results of the EPAAC survey on integrative oncology centres in Europe. Supportive care in cancer: official journal of the Multinational Association of Supportive Care in Cancer 23: 1795-1806.
-
Liu TG, Xiong SQ, Yan Y, Zhu H, Yi C (2012) Use of chinese herb medicine in cancer patients: a survey in southwestern china. Evid Based Complement Alternat Med 769042.
-
Li X, Yang G, Li X, Zhang Y, Yang J, et al. (2013) Traditional Chinese medicine in cancer care: a review of controlled clinical studies published in chinese. PLoS One 8: e60338.
-
Hsiao WL, Liu L (2010) The role of traditional Chinese herbal medicines in cancer therapy-from TCM theory to mechanistic insights. Planta Med 76: 1118-1131.
-
Chung-Hua Hsu C-JL, Tsai-Ju Chien, Che-Pin Lin, Chien-Hung Chen, Mei-Jen Yuen, et al. (2011) The Relationship between Qi Deficiency, Cancer related Fatigue and Quality of Life in Cancer Patients. J Tradit Complement Med 2: 129-135.
-
Falkson G, Gelman R, Falkson CI, Glick J, Harris J (1991) Factors predicting for response, time to treatment failure, and survival in women with metastatic breast cancer treated with DAVTH: a prospective Eastern Cooperative Oncology Group study. J Clin Oncol 9: 2153-2161.
-
Chien TJ, Lin CP, Song YL, Hsu CH (2013) The impact of chemotherapy in cancer patients: reflection on traditional chinese symptom complex, cancer-related fatigue, and quality of life. Holist Nurs Pract 27: 273-281.
-
Chien TJ, Song YL, Lin CP, Hsu CH (2012) The correlation of traditional chinese medicine deficiency syndromes, cancer related fatigue, and quality of life in breast cancer patients. J Tradit Complement Med 2: 204-210.
-
Yao G, Chung CW, Yu CF, Wang JD (2002) Development and verification of validity and reliability of the WHOQOL-BREF Taiwan version. J Formos Med Assoc 101: 342-351.
-
Ware J Jr, Kosinski M, Keller SD (1996) A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care 34: 220-233.
-
Ware JE, Kosinski M, Keller SD (1998) SF-12: how to score the SF-12 physical and mental health summary scales. In: Lincoln, Quality Metric incorporate, New England Medical Center Hospital. (3rd edn), Health Assessment Lab.
-
Reimer T, Gerber B (2010) Quality-of-life considerations in the treatment of early-stage breast cancer in the elderly. Drugs Aging 27: 791-800.
-
Lu WI, Lu DP (2014) Impact of chinese herbal medicine on american society and health care system: perspective and concern. Evid Based Complement Alternat Med 2014: 251891.
-
Chang HH, Yeh CH, Sheu F (2009) A novel immunomodulatory protein from Poria cocos induces Toll-like receptor 4-dependent activation within mouse peritoneal macrophages. J Agric Food Chem 57: 6129-6139.
-
Li TF, Lin CC, Tsai HP, Hsu CH, Fu SL (2014) Effects of Kuan-Sin-Yin decoction on immunomodulation and tumorigenesis in mouse tumor models. BMC Complement Altern Med 14: 488.
-
Xu W, Yang G, Xu Y, Zhang Q, Fu Q, et al. (2014) The possibility of traditional chinese medicine as maintenance therapy for advanced nonsmall cell lung cancer. Evidence-based complementary and alternative medicine. eCAM.
-
Oh HM, Kang YJ, Kim SH, Lee YS, Park MK, et al. (2005) Agastache rugosa leaf extract inhibits the iNOS expression in ROS 17/2.8 cells activated with TNF-alpha and IL-1beta. Arch Pharm Res 28: 305-310.
-
Chien TJ, Liu CY, Ko PH, Hsu CH (2016) A Chinese Decoction, Kuan-Sin-Yin, Improves Autonomic Function and Cancer-Related Symptoms of Metastatic Colon Cancer. Integr Cancer Ther 15: 113-123.
-
Chien TJ, Liu CY, Lu RH, Kuo CW, Lin YC, et al. (2016) Therapeutic efficacy of Traditional Chinese medicine, "Kuan-Sin-Yin", in patients undergoing chemotherapy for advanced colon cancer - A controlled trial. Complement Ther Med 29: 204-212.
-
Wang T, Xuan X, Li M, Gao P, Zheng Y, et al. (2013) Astragalus saponins affect proliferation, invasion and apoptosis of gastric cancer BGC-823 cells. Diagn Pathol 8: 179.
-
Chen HW, Lin IH, Chen YJ, Chang KH, Wu MH, et al. (2012) A novel infusible botanically-derived drug, PG2, for cancer-related fatigue: a phase II double-blind, randomized placebo-controlled study. Clin Invest Med 35: E1-E11.
-
Li SG, Chen HY, Ou-Yang CS, Wang XX, Yang ZJ, et al. (2013) The efficacy of Chinese herbal medicine as an adjunctive therapy for advanced non-small cell lung cancer: a systematic review and meta-analysis. PLoS One 8: e57604.
-
Qi F, Li A, Inagaki Y, Gao J, Li J, et al. (2010) Chinese herbal medicines as adjuvant treatment during chemo- or radio-therapy for cancer. Biosci Trends 4: 297-307.
-
Chen M, May BH, Zhou IW, Xue CC, Zhang AL (2014) FOLFOX 4 combined with herbal medicine for advanced colorectal cancer: a systematic review. Phytother Res 28: 976-991.
-
Seki K, Chisaka M, Eriguchi M, Yanagie H, Hisa T, et al. (2005) An attempt to integrate Western and Chinese medicine: rationale for applying Chinese medicine as chronotherapy against cancer. Biomed Pharmacother 59: S132-S140.
-
Tian H, Qin W, Wu W, Guo P, Lu Y, et al. (2015) Effects of Traditional Chinese Medicine on Chemotherapy-Induced Myelosuppression and Febrile Neutropenia in Breast Cancer Patients. Evidence-based complementary and alternative medicine. eCAM.
-
George WJ, Polson JB, O'Toole AG, Goldberg ND (1970) Elevation of guanosine 3',5'-cyclic phosphate in rat heart after perfusion with acetylcholine. Proc Natl Acad Sci U S A 66: 398-403.
-
Wood M, Hall L, Hockenberry M, Borinstein S (2015) Improving Adherence to Evidence-Based Guidelines for Chemotherapy-Induced Nausea and Vomiting. J Pediatr Oncol Nurs 32: 195-200.
-
Kawamura T, Toyabe S, Moroda T, Iiai T, Takahashi-Iwanaga H, et al. (1997) Neonatal granulocytosis is a postpartum event which is seen in the liver as well as in the blood. Hepatology 26: 1567-1572.
-
Suzuki S, Toyabe S, Moroda T, Tada T, Tsukahara A, et al. (1997) Circadian rhythm of leucocytes and lymphocytes subsets and its possible correlation with the function of the autonomic nervous system. Clin Exp Immunol 110: 500-508.
-
Stone CA, Kenny RA, Nolan B, Lawlor PG (2012) Autonomic dysfunction in patients with advanced cancer; prevalence, clinical correlates and challenges in assessment. BMC Palliat Care 11: 3.
-
Longhurst JC (2010) Defining meridians: a modern basis of understanding. J Acupunct Meridian Stud 3: 67-74.
-
Chien LW, Chen FC, Hu HY, Liu CF (2014) Correlation of electrical conductance in meridian and autonomic nervous activity after auricular acupressure in middle-aged women. Journal of alternative and complementary medicine 20: 635-641.
-
Sun YX (2009) Immunological adjuvant effect of a water-soluble polysaccharide, CPP, from the roots of Codonopsis pilosula on the immune responses to ovalbumin in mice. Chem Biodivers 6: 890-896.
-
Yu-Yun Chang L-YW, Chia-Yu Liu, Chung-Hua Hsu (2014) Effect of KUAN SIN YIN and buddhism-based program on quality of life in cancer outpatienst: a pilot study. Register of Chinese Herbal Medicine Journal Spring 111: 5-13.
-
Lee JJ, Lee JJ (2010) A phase II study of an herbal decoction that includes Astragali radix for cancer-associated anorexia in patients with advanced cancer. Integr Cancer Ther 9: 24-31.
-
Cheng S, Eliaz I, Lin J, Thyagarajan-Sahu A, Sliva D (2013) Triterpenes from Poria cocos suppress growth and invasiveness of pancreatic cancer cells through the downregulation of MMP-7. Int J Oncol 42: 1869-1874.
-
Wang JW, Yang ZQ, Liu C, Chen SJ, Shen Q, et al. (2015) Cancer survivors' perspectives and experience on western medicine and traditional Chinese medicine treatment and rehabilitation: a qualitative study. Patient Prefer Adherence 9: 9-16.
-
Liu X, Hua BJ (2008) Effect of traditional Chinese medicine on quality of life and survival period in patients with progressive gastric cancer.
-
Taixiang W, Munro AJ, Guanjian L (2005) Chinese medical herbs for chemotherapy side effects in colorectal cancer patients. Cochrane Database Syst Rev 25: CD004540.





