Journal of Family Medicine and Disease Prevention
On the Tip of the Tongue: Tongue Necrosis as the Initial Presentation of Systemic Vasculitis in Adult and Pediatric Patients - Case Reports and a Literature Review
Reshmi Raveendran1, Sharon Banks2*, Michael Beck3, Shirley Albano-Aluquin2, Shyam Sabat4 and Barbara Ostrov2,5
1Department of Medicine, Penn State Milton S. Hershey Medical Center, USA
2Department of Medicine, Division of Rheumatology, Penn State Milton S. Hershey Medical Center, USA
3Department of Pediatrics, Division of Hospitalist Medicine, Penn State Milton S. Hershey Medical Center, USA
4Department of Radiology, Penn State Milton S. Hershey Medical Center, USA
5Department of Pediatrics, Division of Pediatric Rheumatology, Penn State Milton S. Hershey Medical Center, USA
*Corresponding author:
Sharon Banks DO, Department of Medicine, Division of Rheumatology, Penn State Milton S. Hershey Medical Center, 500 University Drive mail code H038, Hershey, PA. 17033, USA, Tel: 717-531-5384, Fax: 717-531-8274, E-mail: sbanks@ psu.edu
J Fam Med Dis Prev, JFMDP-2-047, (Volume 2, Issue 4), Case Report; ISSN: 2469-5793
Received: August 17, 2016 | Accepted: November 24, 2016 | Published: November 28, 2016
Citation: Raveendran R, Banks S, Beck M, Albano-Aluquin S, Sabat S, et al. (2016) On the Tip of the Tongue: Tongue Necrosis as the Initial Presentation of Systemic Vasculitis in Adult and Pediatric Patients - Case Reports and a Literature Review. J Fam Med Dis Prev 2:047. 10.23937/2469-5793/1510047
Copyright:© 2016 Raveendran R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Tongue necrosis is a rare manifestation of large to medium vessel vasculitis. It has rarely been reported in adults and children. We present two cases of tongue necrosis in adult and pediatric patients with pathologically different etiologies related to different subsets of vasculitis and review their clinical course. To our knowledge, this is the first comprehensive review of the literature on the vasculitides which cause tongue necrosis in adults and children which include giant cell arteritis, polyarteritis nodosa and granulomatosis with polyangiitis. For giant cell arteritis, the most commonly reported etiology of vasculitis induced tongue necrosis; an overview of the presentations, labs, treatment and symptoms of the reported cases is shown. Vasoconstrictors in the treatment of tongue swelling are discouraged due to its negative effect on an underlying vasculitis. Physicians should consider vasculitis in the differential diagnosis of tongue necrosis in both adult and pediatric patients and confirm histologically. Early detection and management with immunosuppressive medications can improve outcomes for these patients.
Keywords
Tongue necrosis, Vasculitis, Polyarteritis nodosa, Giant cell arteritis, Granulomatosis with polyangiitis
Introduction
Vasculitis is a broad-term that refers to systemic diseases resulting from inflammation of blood vessels [1]. For classification purposes, vasculitides are differentiated by the size of the vessel affected, the typical symptoms and diagnostic approach. Temporal arteritis, also known as giant cell arteritis (GCA) is a vasculitis that typically affects medium to large-sized vessels in older adults [1]. The vessels that are affected are usually related to the head and neck; however other anatomic sites can be involved including the thorax and abdomen [2]. Common presenting symptoms include headache, jaw claudication, blurred or loss of vision and scalp tenderness. Less common presentations include abdominal and brain ischemia [2]. Polyarteritis nodosa (PAN) on the other hand, is a vasculitis that typically affects medium-sized vessels [1]. Common presentations associated with PAN include renal failure, hypertension, abdominal pain, neuropathy and skin ulcerations [3]. The disease primarily affects adults with rare presentations in children [3]. Less common presentations of the various vasculitic syndromes affecting almost every organ system are reported throughout the medical literature [2-34], including tongue necrosis due to involvement of the lingual arteries. In the following, we present two cases of bilateral tongue necrosis seen in an adult and child at our institution and perform the first published comprehensive review of the literature regarding this presentation of systemic vasculitis.
Methods
A comprehensive review of the medical literature was performed using MEDLINE and PUBMED. All cases of tongue necrosis due to necrotizing vasculitis of different types affecting pediatric and adults were reviewed and collated. Permission was given by both patients presented in the case reports to report their histories and clinical course in this review.
Case 1
A previously healthy 68-year-old female presented from an outside hospital with a one month course of gradual tongue swelling in association with neck swelling and oral and submandibular pain. At the onset, she presented to her primary care physician and was prescribed oral amoxicillin for presumed sinusitis. Due to her persistent symptoms she was admitted for possible angioedema. She was treated with 40 mg of IV dexamethasone over a 24-hour period, H1 and H2 blockers, antibiotics, and a dose of icatibant without reduction in her symptoms. CT scan of her head and neck was consistent with acalculous sialadenitis. Lab tests including C1q, C1 esterase inhibitor, C3, C4, ANA and ANCA were normal with the exception of elevations of sedimentation rate (ESR) and C - reactive protein (CRP) to 55 mm/Hr and 6.58 mg/L (normal < 0.8 mg/L), respectively. Initial tongue biopsy of the swollen anterior tongue was significant for fungal overgrowth with chronic-appearing underlying inflammation without evidence of amyloidosis. She was started on an antifungal and after 2-weeks; she was transferred to our hospital due to failure to improve.
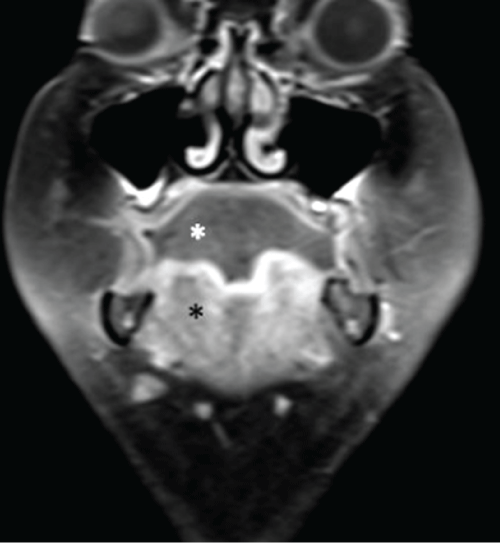
Upon admission to our hospital she was afebrile, tachycardic and in moderate pain. Physical exam was concerning for poor movement of her tongue anteriorly as well as laterally and she had difficulty with articulation. Her tongue was also noted to be smooth with a whitish-appearing plaque on the anterior region. MRI of the mouth and tongue was performed showing necrotic tissue (Figure 1). The patient had pain on palpation of her tongue around the plaque and sensation was decreased on the plaque itself. She was started on 60 mg of prednisone daily.
.
Figure 1: Coronal fat saturated postcontrast T1 weighted MR image through anterior tongue shows non-enhancing necrotic tissue (white asterisk) in the superior portion and normal enhancing tissue inferiorly (black asterisk) of adult patient.
View Figure 1
With persistent symptoms, a repeat biopsy of the tongue was attempted. Upon gentle traction of her tongue for the biopsy, her anterior tongue sloughed off. Adjacent to the area of detachment she was noted to have healthy-appearing granulation tissue at the border. Pathology of the detached tongue was significant for full thickness coagulative necrosis with prominent bacterial and fungal overgrowth. While findings of the remaining tongue showed acute and chronic inflammation associated with vascular proliferation consistent with granulation tissue. CT angiography of the neck was performed to determine an etiology for the diminished blood supply to the tongue and was significant for a beaded appearance and luminal irregularity of the right mid-cervical internal carotid artery. Upon further history, she admitted to having intermittent jaw claudication as well as blurred vision and mild scalp tenderness for one-month prior. Due to the bilateral involvement of the tongue, bilateral temporal artery (TA) biopsies were obtained in order to increase the diagnostic yield in this case specifically. Biopsies revealed lymphocytes, histiocytes, and multinucleated giant cells with focal destruction of the internal elastic lamina and marked intimal thickening significantly decreasing the lumen of the arteries consistent with bilateral active giant cell arteritis (Figure 2). She received 1 mg/kg of methylprednisolone and underwent gastrostomy tube placement for severe dysphagia and need for nutrition and medications. She was transitioned to liquid prednisone 20 mg twice daily. On rheumatology follow-up, her prednisone dose has been reduced over 6 months with no recurrence of tongue swelling or necrosis and resolution of facial pain and neck swelling. She was started on methotrexate subcutaneous injection for steroid sparing purposes and has been doing well.
.
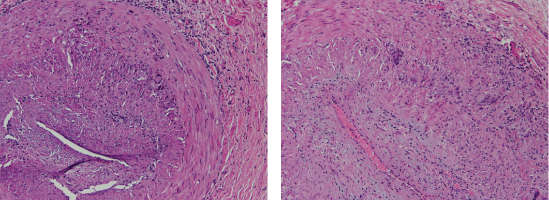
Figure 2: Right and left TA sections of adult patient. Examination reveals small caliber artery with mixed inflammatory infiltrate composed of lymphocytes, histocytes, and multinucleated giant cells with focal destruction of internal elastic lamina and marked intimal thickening significantly decreasing the lumen of the arteries.
View Figure 2
Case 2
A 6-year-old girl with no significant past medical history was admitted due to two weeks of fever and skin rash. Her symptoms began with bilateral ear pain and low-grade fevers to 38 °C for which her pediatrician had started her on amoxicillin for acute otitis media. Despite antibiotics and acetaminophen, she continued to have persistent fevers. She was reevaluated by her pediatrician and was found to have three painful lesions along her lower lip which were conservatively managed. Eight days after initial evaluation she continued to have low-grade temperatures, fatigue and new arthralgias of her right arm, involving the elbow and wrist. By the fourteenth day of symptoms, due to progressive pharyngeal pain, poor oral intake, and the appearance of several new painful subcutaneous nodules, she was reevaluated and sent to the emergency department at the Children's Hospital.
Upon admission, she was febrile to 38.4 °C, tachycardic and had an elevated blood pressure to 139/64. She was mildly ill-appearing, but non-toxic. On examination, she did not have any conjunctival changes, but her tongue was painful and coated with exudate. There was not a strawberry tongue and there were no tongue ulcerations. There was no lymphadenopathy or organomegaly, but renal artery bruits were auscultated on abdominal examination. Her joint exam was normal. She had scattered 0.5 to 2 cm painful nodules on her lip, forehead, forearm and shin.
Studies revealed a leukocytosis of 16.9 × 109/L with neutrophilia. Hemoglobin was 11.6 g/dL and an ESR was 45 mm/Hr. Liver and renal function tests were normal. Urinalysis revealed microscopic hematuria. Her ASO and Anti-DNase B titer were both elevated at 528 and 1360 units/mL respectively. Complement levels were normal, ANCA was not detected and ANA was negative. Echocardiogram was normal with no evidence of coronary dilation or aneurysms.
She remained febrile and persistently hypertensive requiring pharmacologic management. Her tongue pain continued to worsen during her hospital stay and she was noted to have a new deep, linear necrotic ulceration on the superior aspect of her tongue.
A nodule biopsy of one of the skin nodules showed small to medium arteries with intravascular thrombus in the wall of the vessel, neutrophils and fibrin consistent with polyarteritis nodosa (Figure 3). Renal ultrasound and visceral arterial duplex were normal; subsequent MRA revealed stenosis of the left renal artery (Figure 4). She was diagnosed with post-streptococcal systemic PAN with tongue necrosis. She was given corticosteroids with six cycles of intravenous cyclophosphamide. With long-term follow-up over 13 years she has had complete resolution of the illness with complete healing of the tongue necrosis, however still requires management of renovascular hypertension with an ACE inhibitor.
.
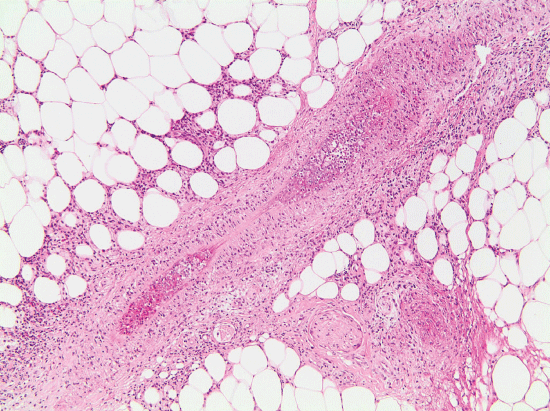
Figure 3: Skin biopsy. Coursing through the subcutaneous fat is a small artery with intravascular fibrin and neutrophils. Acute inflammatory cells also traverse the wall of the vessel. The immediately surrounding fat shows mixed inflammation that is rich in eosinophils.
View Figure 3
.
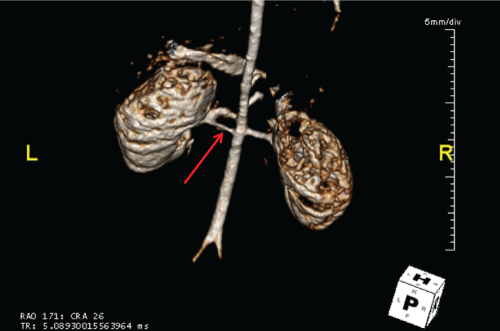
Figure 4: Abdominal MRA of the pediatric patient referenced in Case 2. Note the mild to moderate stenosis of the proximal portion of the lower left renal artery (red arrow). No definite stenosis of the right renal artery is demonstrated.
View Figure 4
Discussion
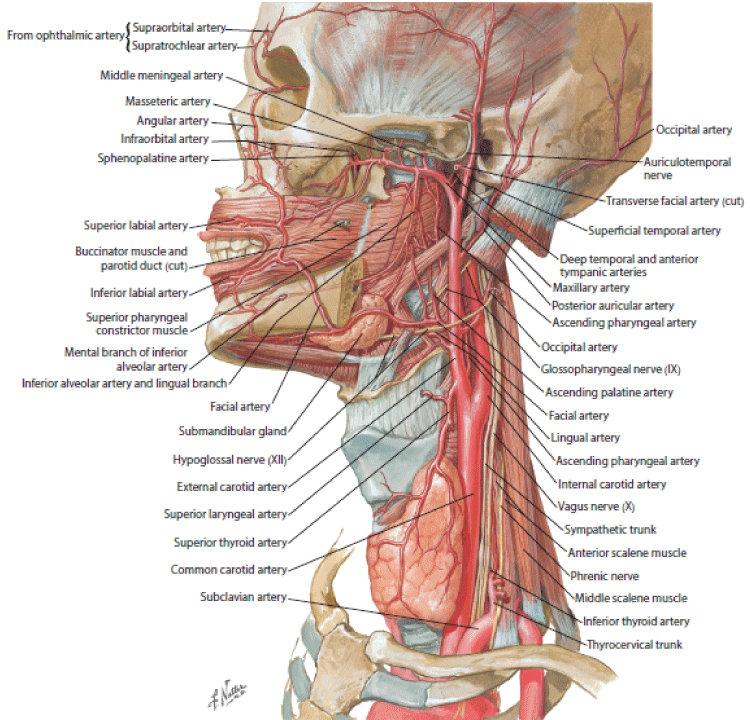
Tongue necrosis is a rare occurrence given the tongue's extensive collateral blood supply from the lingual artery, tonsillar branch of the facial artery and the ascending pharyngeal artery (Figure 5). Their common origin is the external carotid artery which goes on to become the superficial temporal artery, the site of temporal arteritis. While unusual, tongue necrosis may occur in the setting of trauma, radiation therapy, malignancy, or hypoperfusion from cardiac causes or sepsis, or due to inflammatory causes such as vasculitis [4-6].
.
Figure 5: Arteries of oral and pharyngeal regions. Note the arteries that supply the tongue including the lingual artery, facial artery and ascending pharyngeal artery and their origin, the external carotid which goes on to become the superficial temporal artery.
View Figure 5
Tongue necrosis has been reported worldwide in the setting of GCA, albeit rarely, with the first reported case in 1959 [4]. In the published tongue necrosis cases due to GCA (Table 1), all patients were over the age of 50 with the predominant age ranging from 70-80 years with a mean age of 75. The average age of GCA reported in the literature is 72 years, which mirrors the age of the reported tongue cases published [33]. In the literature, the ratio of women to men with GCA is about 2.5 to 1 [34] while the female predominance is more pronounced at 4:1 in the patients with tongue involvement. In our tongue necrosis review (Table 1), a ratio of 4:1 female to male (84% female) was found in our 34 patients. As is known with other disorders, such as myocardial infarction, atypical presentations in women may cause a delay in diagnosis, and may explain this gender difference in our cases. This delay may lead to progression of symptoms to full necrosis rather than solely tongue pain or paresthesias that are more commonly reported symptoms in GCA.
![]()
Table 1: Literature review of temporal arteritis and tongue necrosis in adults.
View Table 1
The presenting symptoms in our study group were typical for GCA in 75% of cases and included diffuse headache, jaw pain, visual loss or decreased vision and scalp pain. However, only 10% of our group reviewed had polymyalgia rheumatica (PMR) symptoms, which is lower than the typical GCA patient population (about 50% with PMR) [33], again possibly contributing to the delay in diagnosis. More unusual symptoms related to tongue involvement included swelling, difficulty moving the tongue and pain. The whole tongue manifested as a gray, cyanotic swollen tongue was involved in some patients and 30% only one side of the tongue. Ulceration can also be initially seen. Sloughing or loss of the tongue as the process progresses is not unusual and reported in our patient.
Laboratory testing for GCA commonly involves measuring inflammatory markers, most often the ESR and/or CRP. The ESR was over 50 in most cases reviewed and ranged from 25 to > 100 mm/h. These are consistent with the reported results in more typical case presentations of GCA, as well [33]. Diagnostic evaluation has also included cerebral angiography demonstrating narrowing of the external carotid artery suspicious for vasculitis as well as TA ultrasound demonstrating the halo sign; a periluminal dark halo seen on ultrasound of the temporal artery and TA biopsy which is the gold standard for diagnosis [35]. When the whole tongue is involved as in our case, bilateral arterial ischemia is the suspected underlying pathology. In 80% of the cases we have summarized (Table 1) the pathology demonstrated TA ischemia on biopsy. This is a greater proportion of positive biopsies than commonly found in GCA patients, for whom about 50% are usually confirmed histologically [33]. This too may reflect the lag time to diagnosis in the tongue necrosis population, enabling a longer interval for more pathologic vascular changes to develop.
All of the cases in our review were managed with moderate to high or pulse dose corticosteroids (1 mg/kg/day vs. pulse methylprednisolone of 1000 mg/day for 3 days). Additional immunosuppression with cyclophosphamide was administered in one case and azathioprine in several cases. All patients had outpatient continuation of oral prednisone and rheumatology follow-up for ongoing management [33,34].
Of the 33 tongue necrosis cases reviewed in addition to our patient (Table 1), 5 or 15% had a precipitating agent, such as ergots or other vasoconstrictors that may have aggravated the underlying arterial narrowing due to the unrecognized arteritis. Our first case presented with the unusual finding of bilateral tongue necrosis, which may have progressed after the use of the vasoconstrictor icatibant was administered for suspicion of hereditary angioedema. Unfortunately icatibant is a vasoconstrictor as it inhibits bradykinin, a known vasodilator. It is possible the vasoconstriction effect of icatibant exacerbated the underlying ischemia from her bilateral temporal arteritis and further reduced blood supply to the tongue causing the results we observed. The arteriolar destruction was confirmed by pathology from TA biopsies [27] Per review of the current literature, this is the first reported case of tongue necrosis from pathologically proven bilateral temporal arteritis in the setting of icatibant, although other vasoconstrictors have been implicated.
There have been two prior reported cases of tongue necrosis in the setting of medium to small vessel necrotizing vasculitis. Polyarteritis nodosa (PAN) (Table 2) has been reported in two children previously with both of the pediatric cases following streptococcal infection, as in our patient [3,30]. The mechanism for post-streptococcal PAN is poorly understood, however it is likely secondary to damage to the intima and media layers of vessels due to immune deposits causing destruction of the vessels and compromising blood flow [1]. The literature cases had a presentation similar to our case, including fever, tongue pain, swelling or oral blisters, leukocytosis, high ESR and high titers of anti-DNase-B and ASO antibodies. The tongue pain and swelling with oral lesions ultimately led to the diagnosis following this atypical presentation. Tissue biopsy typically demonstrates fibrinoid necrosis. Treatments have been high dose prednisone oral or IV and in one case cyclophosphamide.
![]()
Table 2: Literature review of polyarteritis nodosa and tongue necrosis in pediatrics.
View Table 2
Tongue necrosis has also been rarely reported in granulomatosis with polyangiitis (GPA) (Table 3). These two cases involved middle aged females both with pulmonary and renal manifestations. Involvement of the oral mucosa is common in GPA with lesions reported in 6-50% mainly consisting of oral ulcers on the tongue, strawberry gingivitis, and osteonecrosis of the palate; however tongue necrosis is rarely described. The oral lesions generally do respond well to oral steroids and cyclophosphamide.
![]()
Table 3: Literature review of tongue necrosis in granulomatosis with polyangiitis.
View Table 3
Due to the rich blood supply of the lingual tissue, tongue necrosis rarely develops in patients with systemic vasculitis. Despite the aggressive nature of these diseases it is important to note that all but one of the vasculitis cases reviewed improved with the proper treatment including corticosteroids and, in some cases, more aggressive immunosuppression. Treatment generally led to healing of the tongue and improvement in the systemic illness.
As we have reviewed, once other potential etiologies are ruled out, practitioners must promptly consider the range of necrotizing vasculitides in both children and adult patients who present with the unusual finding of tongue necrosis. Avoiding the use of vaso constricting medications is crucial. Obtaining tissue for histopathologic diagnosis is important in making a correct diagnosis. This paper is the first comprehensive review on this rare entity providing a summary of both adult and pediatric published cases. With prompt diagnosis and treatment, the prognosis appears to be favorable despite the aggressive nature of the underlying necrotizing vasculitic disease.
Acknowledgements
The authors would like to acknowledge Dr. Carolina Candotti who provided writing assistance and care of the patient presented in Case 1.
Disclosures
Raveendran-None; Banks-None; Beck-None; Albano-Aluquin -None; Sabat-None; Ostrov-None.
References
-
Monarch PA, Merkel P (2014) Vasculitis American College of Rheumatology. ACR Web, 03.
-
Zadik Y, Findler M, Maly A, Rushinek H, Czerninski R (2011) A 78-year-old woman with bilateral tongue necrosis. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 111: 15-19.
-
Buonuomo SP, El Hachem M, Callea F, Bracaglia C, Diociaiuti A, et al. (2013) Necrosis of the Tongue as First Symptom of Polyarteritis Nodosa (PAN): Unusual Presentation of a Rare Disease in Children. Rheumatol Int 33: 1071-1073.
-
Sainuddin S, Saeed NR (2008) Acute bilateral tongue necrosis--a case report. Br J Oral Maxillofac Surg 46: 671-672.
-
Llorente Pendás S, De Vicente Rodríguez JC, Gonzalez Garcia M, Junquera Gutierrez LM, Lopez Arranz JS (1994) Tongue necrosis as a complication of temporal arteritis. Oral Surg Oral Med Oral Pathol 78: 448-451.
-
Allen P (1980) Giant cell arteritis presenting with necrosis of the tongue--a case report. Br J Oral Surg 18: 162-165.
-
Arnung K, Nielsen IL (1979) Temporal arteritis and gangrene of the tongue. Acta Med Scand 206: 239-240.
-
Biebl MO, Hugl B, Posch L, Tzankov A, Weber F, et al. (2004) Subtotal tongue necrosis in delayed diagnosed giant-cell arteritis: a case report. Am J Otolaryngol 25: 438-441.
-
Bondeson J, Ericsson UB, Falke P, Mattiasson I, Nyman U, et al. (1992) Tongue necrosis in temporal arteritis provoked by ergotamine. J Intern Med 232: 541-544.
-
Brearley BF, Macdonald JG (1961) Temporal Arteritis Resulting in Infected Gangrene of Tongue. Br Med J 1: 1151-1152.
-
Brodmann M, Dorr A, Hafner F, Gary T, Pilger E (2009) Tongue necrosis as first symptom of giant cell arteritis (GCA). Clin Rheumatol 28 Suppl 1: S47-49.
-
Goicochea M, Correale J, Bonamico L, Dominguez R, Bagg E, et al. (2007) Tongue necrosis in temporal arteritis. Headache 47: 1213-1215.
-
Grahame R, Bluestone R, Holt PJ (1968) Recurrent blanching of the tongue due to giant cell arteritis. Ann Intern Med 69: 781-782.
-
Hellmann DB (2002) Temporal arteritis: a cough, toothache, and tongue infarction. JAMA 287: 2996-3000.
-
Hicks K, Lee FI (1980) Necrosis of the tongue secondary to cranial arteritis. Br J Oral Surg 18: 166-169.
-
Kusanale A, Boardman H, Khoshnaw H (2008) Tongue necrosis: a rare presentation of temporal arteritis. Age Ageing 37: 119.
-
Marcos O, Cebrecos AI, Prieto A, Sancho de Salas M (1998) Tongue necrosis in a patient with temporal arteritis. J Oral Maxillofac Surg 56: 1203-1206.
-
Patterson A, Scully C, Barnard N, Griffiths MJ, Eveson JW, et al. (1992) Necrosis of the tongue in a patient with intestinal infarction. Oral Surg Oral Med Oral Pathol 74: 582-586.
-
Pedersen AT, Jepsen FL (1983) Lingual infarction in giant cell arteritis. A case report. J Laryngol Otol 97: 479-483.
-
Roseman BB, Granite E (1984) Massive tongue necrosis secondary to temporal arteritis. J Oral Maxillofac Surg 42: 682-684.
-
Sofferman RA (1980) Lingual infarction in cranial arteritis. JAMA 243: 2422-2423.
-
Wolpaw JR, Brottem JL, Martin HL (1973) Tongue necrosis attributed to ergotamine in temporal arteritis. JAMA 225: 514-515.
-
Lethert KH, Jacobson DF (2007) Tongue necrosis from temporal arteritis. J Hosp Med 2: 335.
-
Vazquez-Doval J, Martinez-Vila E, Legarda I, Ruiz de Erenchun F (1994) Tongue necrosis secondary to ergotamine tartrate in a patient with temporal arteritis. Arch Dermatol 130: 261-262.
-
Reed C, Inlis MJ (1965) Acute massive gangrene of tongue. Br Med J 2: 575-576.
-
Obermoser G, Posch L, Zelger B (2004) Spitting out the tongue. Br J Dermatol 151: 721-722.
-
Jennings S, Singh S (2011) Necrotic tongue: a rare manifestation of giant cell arteritis. J Rheumatol 38: 2688.
-
Lobato-Berezo A, Alcalde-Villar M, Imbernón-Moya A, Martinez-Perez M, Aguilar-Martínez A, et al. (2014) Tongue necrosis: an unusual clinical presentation of giant cell arteritis. Arthritis Rheumatol 66: 2803.
-
Kumar R, Gupta H, Jadhav A, Khadilkar S (2013) Bitemporal scalp, lip and tongue necrosis in giant cell arteritis: a rare presentation. Indian J Dermatol 58: 328.
-
Ekman-Joelsson BM, Kjellman B, Hattevig G (1995) Tongue necrosis due to vasculitis. Acta Paediatr 84: 1333-1336.
-
Carter LM, Brizman E (2008) Lingual infarction in Wegener's Granulomatosis: a case report and review of the literature. Head Face Med 4: 19.
-
Bachmeyer C, Petitjean B, Testart F, Richecoeur J, Ammouri W, et al. (2006) Lingual necrosis as the presenting sign of Wegener's granulomatosis. Clin Exp Dermatol 31: 321-322.
-
Hunder GG (2015) Giant cell (temporal) arteritis.
-
Gonzalez-Gay MA, Pina T (2015) Giant cell arteritis and polymyalgia rheumatica: an update. Curr Rheumatol Rep 17: 6.
-
Nesher G, Shemesh D, Mates M, Sonnenblick M, Abramowitz HB (2002) The predictive value of the halo sign in color Doppler ultrasonography of the temporal arteries for diagnosing giant cell arteritis. J Rheumatol 29: 1224-1226.





