Journal of Family Medicine and Disease Prevention
Prolonged Esophageal Button Battery Impaction in a 15 Month-Old: A Case Report
Jennifer Marshalla* and Kelly Williamson
Department of Emergency Medicine, Advocate Christ Medical Center, USA
*Corresponding author: Jennifer Marshalla, Department of Emergency Medicine, Advocate Christ Medical Center, 4440 West 95th Street, 185W, Oak Lawn, Illinois 60453, USA, Tel: 708-684-5375, 217-414-5837, E-mail: jmarshalla@gmail.com
J Fam Med Dis Prev, JFMDP-2-044, (Volume 2, Issue 3), Case Report; ISSN: 2469-5793
Received: July 21, 2016 | Accepted: September 10, 2016 | Published: September 13, 2016
Citation: Marshalla J, Williamson K (2016) Prolonged Esophageal Button Battery Impaction in a 15 Month-Old: A Case Report. J Fam Med Dis Prev 2:044. 10.23937/2469-5793/1510044
Copyright: © 2016 Marshalla J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background:Ingestion of button batteries in the pediatric population is exceedingly dangerous and increasingly more common.
Objective:The ingestion of button batteries in the pediatric population can rapidly lead to esophageal erosion and perforation and must be appropriately diagnosed and treated to prevent mortality.
Case report:A 15 month-old female was transferred to the emergency department from a gastroenterologist's office after a chest x-ray revealed an esophageal foreign body. The patient was undergoing evaluation for regurgitation of food and refusal to eat solid food for three months with their primary care physician. X-ray of the neck upon arrival in the emergency department revealed that the foreign body was consistent with a button battery. The button battery was likely lodged in the esophagus for the three months that the child was having difficulty with feeding.
Discussion:Button battery ingestion in children is increasingly common and can cause significant injury if not identified quickly. If lodged in the esophagus, button batteries can cause injury due to their caustic and electric properties, as well as by direct pressure.
Conclusion:We present this atypical case to increase awareness surrounding this diagnosis amongst primary care physicians. Button battery ingestion in children can be life-threatening and physicians must maintain a high index of suspicion for the diagnosis in children who present with vomiting, coughing or gagging, regurgitation of food, refusal to eat, or chest pain.
Introduction
Button batteries are small, coin-shaped batteries that are used in a variety of electronic items, including children's toys. Ingestion of these button batteries by the pediatric population is a common occurrence with an annual incidence greater than 3,500 cases in the United States [1]. The peak incidence occurs in children ages 6 months to 3 years [2]. Button battery ingestion can lead to esophageal perforation and death within hours if not appropriately diagnosed. This case presents a child who had a button battery in the esophagus for a substantial duration of 3 months with negligible consequences.
Case Report
A 15 month-old female was transferred to the emergency department from a gastroenterologist's office after a chest x-ray revealed an esophageal foreign body. The patient was initially evaluated by her primary care physician three months prior for sudden refusal to eat solid foods. At the time, this was related to the patient not being ready for solid food advancement, though she had been tolerating solid food prior to 12 months of age. The patient was ultimately sent for gastroenterology evaluation when she continued to refuse to eat solid foods three months later; any attempt resulted in regurgitation of the food. Chest radiograph at the office reportedly revealed a foreign body in the mid-esophagus and the patient was transferred to the emergency department for evaluation and removal by otolaryngology.
On general exam, the patient was well appearing and tolerating her secretions. Her vital signs were: temperature 36.6°C, blood pressure 111/73 mmHg, pulse 122 beats/min, respiratory rate 24 breaths/min, and pulse oximetry 100% on room air. On head and neck exam, her trachea was midline and there was no subcutaneous emphysema. Oral mucosa was moist. Lungs were clear to auscultation bilaterally and she demonstrated no difficulty with respirations. The remainder of the physical exam was unremarkable.
X-ray of the neck in the emergency department revealed that the foreign body in the proximal thoracic esophagus had a double density border, consistent with a button battery. The radiographs from the case demonstrating the double density boarder of a button battery on anterior-posterior films are attached figure 1. The patient was evaluated by an ear, nose, and throat (ENT) surgeon in the emergency department and emergently taken to the operating room for esophagoscopy with foreign body removal, bronchoscopy, and nasogastric tube placement. A circumferential eschar was noted in the esophagus once the foreign body was removed, though the patient did not suffer a transmural burn. The foreign body was labeled with the inscription “CR2016 3 VOLTS ENERGIZER,” consistent with a lithium button battery sized 20 mm with a height of 1.6 mm. Post-procedure, the patient was admitted to the pediatric intensive care unit for close monitoring; IV antibiotics (Unasyn 380 mg q 6 hours) and ranitidine were initiated.
.
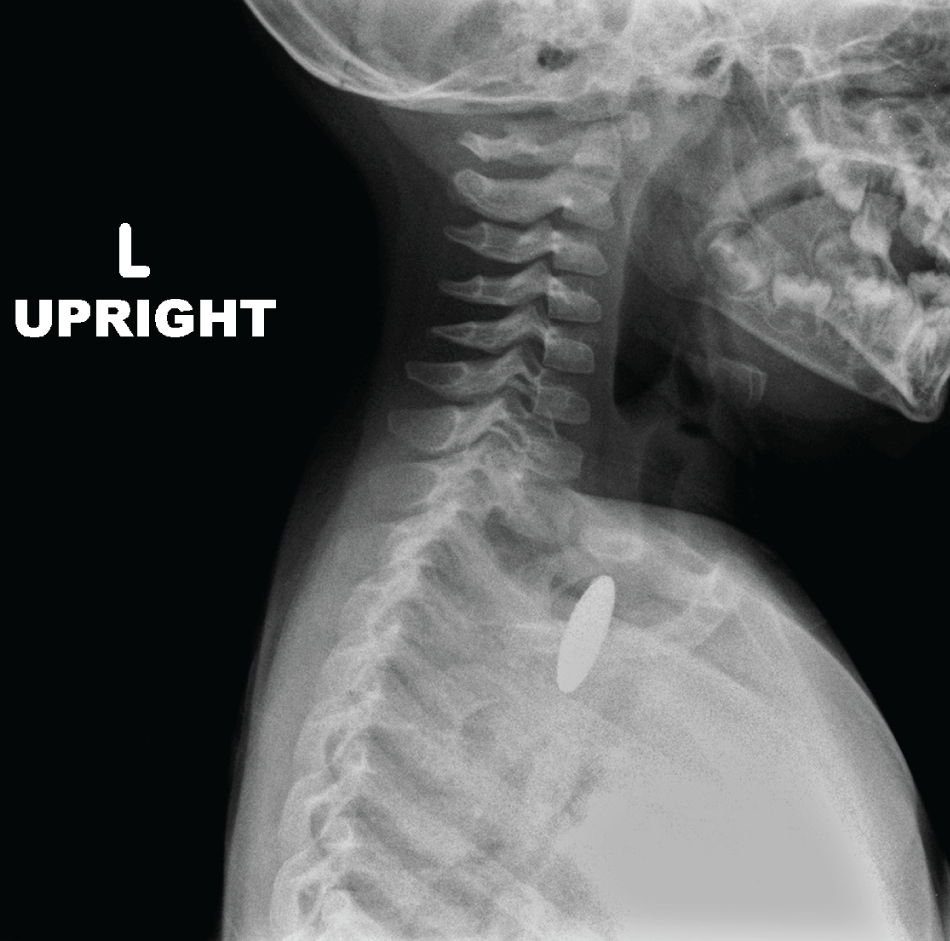
Figure 1: Lateral neck x-ray.
The lateral neck x-ray shows the button battery lodged in the proximal thoracic esophagus with the trachea anterior to the button battery.
View Figure 1
The patient had an esophagram the following day, which revealed no further injury and she was discharged home on post-operative day 2. In follow-up one month later, the patient was completely normal, with no interim history of dysphagia. She was eating foods of all consistencies without aspiration or difficulty. She had postoperative speech therapy evaluation, which was normal as well, and so the decision was made to not complete additional swallow study or esophagram.
Discussion
Button batteries are small, coin-shaped objects that are found in many children's toys. Button batteries range in size, but typically the larger diameter batteries, around 20 mm, cause the most severe problems. These objects can lodge within the esophagus of a child and lead to esophageal perforation, tracheo-esophageal fistulas, and hemorrhage from arterial fistulization. Button battery ingestion can cause injury in three primary ways: leakage of caustic alkaline electrolyte; ischemic necrosis caused by direct pressure; and production of external electrolytic current that hydrolyzes tissue fluids creating hydroxide at the negative pole [3]. The esophagus is susceptible to foreign body retention because of its anatomic areas of narrowing and weak peristalsis [1]. Significant esophageal damage has been reported as early as two hours post ingestion [4]. While both coins and button batteries present as round radiolucent objects on chest radiograph, button batteries are easily distinguished by their characteristic double-rimmed appearance, as seen in the radiographs attached from this case [5] (Figure 2).
.
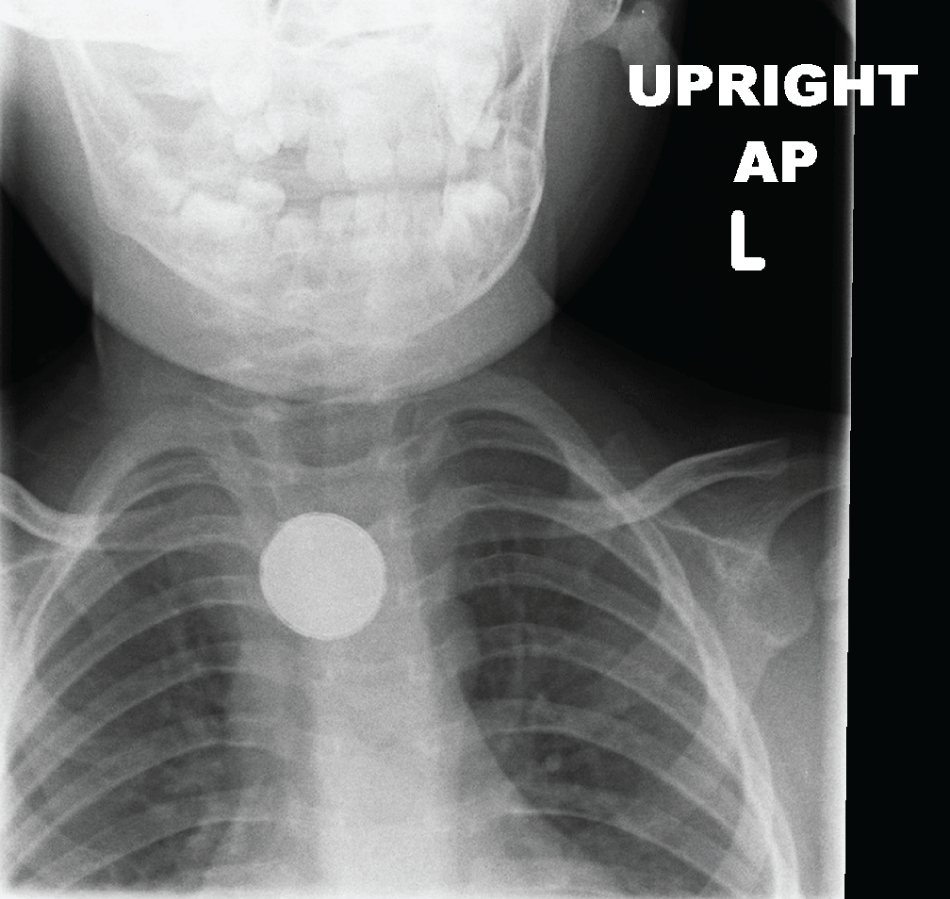
Figure 2: Anteroposterior neck x-ray.
The anteroposterior neck x-ray performed in the emergency department shows the double-rimmed appearance of the button battery lodged in the proximal thoracic esophagus.
View Figure 2
As ingested button batteries can rapidly lead to airway compromise, initial management includes thorough airway assessment. Once airway stability is confirmed, further management includes broad-spectrum antibiotics to cover oral flora and consultation with gastroenterology or ENT for immediate removal of foreign body to prevent further damage to the esophagus. Following removal, patients will require an esophogram to evaluate for esophageal stenosis and fistula formation. If there are any associated voice changes or stridor, patients will require flexible laryngoscopy to evaluate for vocal cord paresis [6]. Guidelines are in place by the National Capital Poison Center for assessment and treatment of button battery ingestions [1].
In the case described above, the patient presented for 3 months of inability to tolerate solid foods and regurgitation of food and was ultimately diagnosed with an ingested button battery lodged in her esophagus. Upon removal, the surgeon noted surprisingly limited injury despite long-term ingestion of a button battery sized 20 mm in diameter. It is possible the battery had already been spent prior to ingestion, causing such limited damage, but the parents were unable to report where the battery came from. Button battery ingestion is typically diagnosed within the first several hours to days following the event given the propensity for rapidly evolving critical illness. In another case of pediatric button battery ingestion, the child had symptoms for one day prior to evaluation and suffered a partial-thickness burn, which later developed into an esophageal stricture of the upper esophagus [7]. As children may not yet be able to report a history of ingestion, it is imperative for physicians to consider esophageal foreign body in patients who present with vomiting or refusal to eat to prevent such a prolonged course of missed diagnosis.
The pediatric literature reports one case of a 2-year-old male who presented with similar symptoms of food regurgitation and frequent vomiting for 7 months who was ultimately diagnosed with a button battery ingestion; he suffered a complicated course after diagnosis and ultimately required thoracotomy for foreign body removal [8]. Another case of a 17-month-old girl who likely had an esophageal button battery ingestion for at least 18 days resulted in death from esophageal rupture and aspiration of blood into the bronchus [9]. To the best of the authors' knowledge, there is no similarly reported case of esophageal button battery ingestion of a significant duration with such limited consequence.
Conclusion
Button battery ingestions that remain in the esophagus can result in severe complications and death within hours to days. This case presents a child who had a button battery in the esophagus for 3 months. It is important for physicians to keep ingestion of button batteries in their differential for children presenting with vomiting, coughing or gagging, refusal to eat, and complaints of retrosternal pain. It is also important to obtain an immediate anterior-posterior and lateral plain film to help determine the cause of symptoms. Treatment includes prompt gastrointestinal or ENT consult for immediate removal by endoscopy to prevent further complications.
References
-
National Capital Poison Center.
-
Thabet MH, Basha WM, Askar S (2013) Button battery foreign bodies in children: hazards, management, and recommendations. Biomed Res Int 2013: 846091.
-
Centers for Disease Control and Prevention (2012) Injuries from Batteries among Children Aged Less Than 13 Years- United States, 1995-2010. MMWR 61: 661-666.
-
Litovitz T, Whitaker N, Clark L, White NC, Marsolek M (2010) Emerging battery-ingestion hazard: clinical implications. Pediatrics 125: 1168-1177.
-
Tanigawa T, Shibata R, Katahira N, Ueda H (2012) Battery ingestion: the importance of careful radiographic assessment. Intern Med 51: 2663-2664.
-
Jatana, KR, Litovitz T, Reilly JS, Koltai PJ, Rider G, et al. (2013) Pediatric button battery injuries: 2013 task force update. International Journal of Pediatric Otorhinolaryngology 77: 1392–1399.
-
Kim SH, Keum B, Chun HJ (2015) Drooling, Irritability, and Refusal to Eat in a 22-Month-Old Child. Button Battery Ingestion. Gastroenterology 149: 544-545.
-
Alam E, Mourad M, Akel S, Hadi U (2015) A case of battery ingestion in a pediatric patient: what is its importance? Case Rep Pediatr 2015: 345050.
-
Guinet T, Gaulier JM, Moesch C, Bagur J, Malicier D, et al. (2016) Sudden death following accidental ingestion of a button battery by a 17-month-old child: a case study. Int J Legal Med 130: 1291-1297.





