International Journal of Women's Health and Wellness
Osteitis Pubis in a 30-Year Old Postpartum Recreational Runner: A Case Report
Kurt Schiess*, Dani Moffit and Tim Braun
Department of Sport Science and Physical Education, Idaho State University, Pocatello, USA
*Corresponding author:
Kurt Schiess, Department of Sport Science and Physical Education, Idaho State University, 912 S 8th Ave, Stop 8105, Pocatello, ID 83209-8105, USA, Tel: 208-705-2230, E-mail: schikurt@isu.edu
Int J Womens Health Wellness, IJWHW-1-009, (Volume 1, Issue 1), Case Report; ISSN: 2474-1353
Received: November 18, 2015 | Accepted: December 28, 2015 | Published: December 31, 2015
Citation: Schiess K, Moffit D, Braun T (2015) Osteitis Pubis in a 30-Year Old Postpartum Recreational Runner: A Case Report. Int J Womens Health Wellness 1:009. 10.23937/2474-1353/1510009
Copyright: © 2015 Moffit D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: The pelvic girdle instability of postpartum women can lead to further complications such as SI joint stability and osteitis pubis. Pain post-birth is common; however, pain for an extended period of time (i.e. six months) may indicate further complication. Here we present a case of osteitis pubis in a multiparous woman.
Case Report: A 30-year old female recreational runner presented groin, hip adductors, rectus abdominis, and inguinal ligament pain. Previous history revealed the pain started three years prior, recently increasing with activities of daily living. After birth of her third child, pain increased so she could not perform daily tasks such as grocery shopping, and was unable to hold her children. Examination revealed normal gait, level iliac crests, and normal lumbar curve. Palpation revealed tenderness over her right adductors and in medial thigh near the pudendal region. Differential diagnoses included hip adductor strain, hernia, and pudendal nerve irritation. A CT scan showed potential spigelian hernia. The patient's family physician performed an injection for suspected pudendal nerve irritation. Neurontin was prescribed, increasing her pain. An ultrasound did not show a hernia, so an MRI was ordered for further diagnosis. The MRI showed pubic symphysis arthritis with edema in the parasymphyseal region; diagnosis was osteitis pubis. Multiple ultrasound guided injections of Celestone and Kenalog was performed over two months. A home exercise program including aquatic rehabilitation and massage over six months was performed by the patient.
Discussion: Pain in postpartum women should be temporary. A diagnostic challenge arises when the pain is prolonged and no mechanism of injury is indicated. Every patient who has given birth should be educated on the importance of recovery time and lumbopelvic strengthening before returning to full activity. Delaying treatment after prolonged pain may lead to other concerns such as instabilities and inflammatory conditions.
Keywords
Pudendal nerve, Spigelian hernia, Neurontin, Celestone, Pubic symphysis
Introduction
Pelvic girdle pain presents a diagnostic challenge in any population but especially in pregnant and postpartum women [1,2]. During pregnancy this condition is common, affecting approximately 45% of this population [1]. After delivery, pelvic girdle pain prevalence ranges from 5 to 37% of the postpartum population [2]. This pain typically resolves within six months of birth but a small percentage of postpartum women experience symptoms lasting for several months to years [2]. With this pain commonly viewed as temporary, the diagnostic process is often delayed allowing for the development of osteitis pubis [1]. We present a case of osteitis pubis in a multiparous women diagnosed via MRI with contrast. Treatment consisted of injections and a home rehabilitation program.
Case Report
A 30-year old female postpartum recreational runner presented with pain in the right groin, hip adductors, rectus abdominis, and the inguinal ligament. This pain began to present itself four years prior, five months after the birth of her second child during a 10K race; this seemed to be what triggered the cascade of pain, initiating in her groin. However, the patient waited to seek medical attention until the pain was intolerable, approximately one year after the birth of her third child. During the four years prior, running, biking, and walking for long periods of time caused mild pain in the groin, similar to a strain. Over the course of several months, the pain increased with activities of daily living until she could no longer perform tasks such as grocery shopping and holding her children. It was at this time the patient sought an evaluation from her family physician.
Upon initial examination, she exhibited normal gait, level iliac crests, and normal lumbar curve. Palpation revealed no swelling, demonstrated tenderness over her right adductors near the inguinal crease and groin, with no contra lateral pain. Normal hip active and passive hip range of motion was noted by the physician. There was no indication of sacroiliac joint instability beyond expected variations due to childbirth. There was nothing of note during any of her three pregnancies that may have contributed to her pain. Differential diagnoses considered included femoral acetabular impingement, hernia, sacroiliac dysfunction, and hip adductor sprain. The physician prescribed 300 mg Gabapentin (Neurontin) twice daily. The patient was told to begin an exercise program to strengthen her abdominal muscles. Three months after the initial evaluation, the patient returned because the pain had not abated. The physician ordered CT scan which indicated a potential spigelian hernia. Though the physician believed it to not be noteworthy, it was suggested she see a pelvic specialist for further evaluation. In the meantime, the physician began treatment for pudendal nerve irritation. He performed a pudendal nerve block with 20 mg/mL of lidocaine and methylprednisolone acetate (Depo-Medrol); a noted increase in pain occurred the following day in response to the procedure.
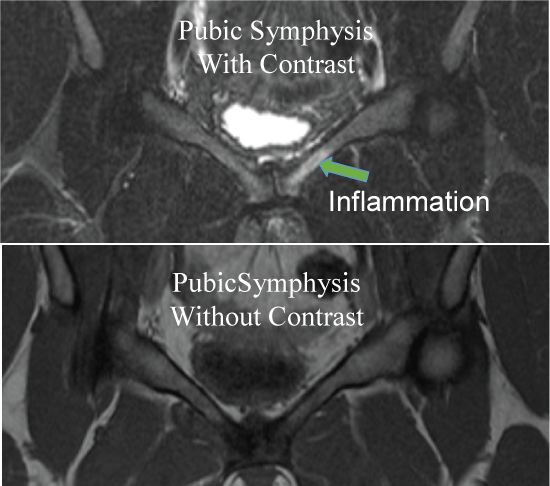
The patient chose to seek a second opinion from a sports medicine physician with expertise in hernia diagnosis. A diagnostic ultrasound examination did not reveal a hernia. The sports medicine physician ordered an MRI with contrast for further diagnostic imaging (Figure 1).The clinical findings of the MRI revealed arthritis in the pubic symphysis with edema in the parasymphyseal region. These findings denote osteitis pubis, typically resulting from pelvic instability. The physician attributed the condition to her pregnancies. The condition was potentially escalated to this level because of a lack of postpartum exercise and inadequate recovery time after childbirth.
The sports medicine physician performed a guided ultrasound injection with 1% lidocaine to numb the area, followed by 2ccs of betamethasone sodium phosphate (Celestone) into the pubic symphysis. After the first injection, her pain increased. At her two week follow-up appointment, it was thought the injection was unsuccessful, and a second injection was performed using the ultrasound, 1% lidocaine, and 1.5ccs of triamcinolone (Kenalog 40). The second injection allowed her to be pain-free for approximately six weeks, but periodic pain returned. Two months after the second injection, the patient had another follow-up exam and injection. The third injection was performed using ultrasound, 1% lidocaine, and 1cc of triamcinolone (Kenalog 40) with an additional 0.5cc of triamcinolone (Kenalog 40) in the anterior end of the capsule. By her next exam, her pain was intermittent, and did not warrant another injection. Following her third injection, the sports medicine specialist recommended a home exercise program including aquatic rehab and massage. The protocol continued for approximately six months. Over the course of this time, her activities of daily living were no longer painful and she was able to have a gradual return to running without further exacerbation of symptoms. No follow-up care or imaging was necessary after the six months of rehabilitation.
Discussion
Pubic pain during and shortly after pregnancy is common. In some cases this pain does not resolve, leading to the necessity to consider other causes. A thorough patient history can determine the increased likelihood for osteitis pubis [3]. Differential diagnoses include femoral acetabular impingement, hernia, sacroiliac joint dysfunction, pudendal nerve irritation, and hip adductor strain. In the process of differentiating the cause of pain, the use of orthopaedic special tests will aid proper diagnosis as well as medical imaging. Multiparous women have a higher incidence of pelvic diastasis (1/300 to 1/30,000 pregnancies) which can lead to pain and arthritis in the pubic symphysis [4]. Approximately 50% experience lumbopelvic pain while pregnant with most symptoms resolving within one to three months, but there are a substantial amount of women who do not fully recover [5]. Osteitis pubis related to childbirth occurs due to hormones relaxing the ligament, causing a diastasis of the pubic symphysis [4,6]. This leads to inflammation, pain and instability in the joint [6-8]. Medical imaging proven to be effective in diagnosing osteitis pubis include X-rays [3,9,10], bone scans [3,10], CT scans [3,9,10], ultrasound [3], and diagnostic laparoscopy [3]; MRI with contrast being the most successful [3,9,11].
Treatment types range from conservative management to steroid injections, with a last resort of surgical treatment [9]. Conservative options include activity modification and physical therapy with a gradual increase in activity [9]. Hip strengthening and flexibility exercises will assist in pelvic stabilization allowing for a potential decrease in symptoms [3]. Water-based and land-based exercise, concurrent with manual therapy should be part of the protocol [12]. Recommendations for postpartum exercises consist of restoring motor control and stability of the hip and lumbopelvic areas [3]. Rehabilitation should be done for 18-20 weeks, three times per week, with each session lasting 30-60 minutes [5]. Intra-articular corticosteroid injections into the joint may resolve symptoms during painful rehabilitation [7,10]. Some patients require multiple injections to aid their recovery [10].
Conservative measures failing to provide resolution may lead to surgery [10]. Patients who undergo surgery could return to full activity in approximately seven weeks with a 92% success rate polypropylene mesh surgery [10]. Curettage surgery has a 72% success rate with a recovery time of nearly 5 months [10].
This case presents a unique diagnostic challenge of pelvic pain development in a postpartum recreational female runner. As this is a case, no causal inferences can be made. When returning to her desired activity level of running 5K/10K races, she did not gauge her readiness accurately. Having been through two previous pregnancies and subsequent births, she self-treated her pain as a muscle strain. She was unaware that postpartum exercise should include strengthening of pelvic muscles. Medical professionals, knowing the benefits of postpartum exercise [4,5], should educate their patients for pelvic health. In addition, women should be educated on the importance of sufficient recovery time for the ligaments to return to normal and encouraged to participate in a lumbopelvic strengthening protocol postpartum before returning to full activity [5]. Knowing the post-delivery pain should be temporary can decrease incidence of further complications in postpartum women.
Acknowledgements
I would like to acknowledge Dr. Karen Apple by for her feedback during the initial writing of this case.
References
-
Vermani E, Mittal R, Weeks A (2010) Pelvic girdle pain and low back pain in pregnancy: a review. Pain Pract 10: 60-71.
-
Ferreira CW, Alburquerque-Sendi NF (2013) Effectiveness of physical therapy for pregnancy-related low back and/or pelvic pain after delivery: a systematic review. Physiother Theory Pract 29: 419-431.
-
Jansen JA, Mens JM, Backx FJ, Stam HJ (2008) Diagnostics in athletes with long-standing groin pain. Scand J Med Sci Sports 18: 679-690.
-
Yoo JJ, Ha YC, Lee YK, Hong JS, Kang BJ, et al. (2014) Incidence and risk factors of symptomatic peripartum diastasis of pubic symphysis. J Korean Med Sci 29: 281-286.
-
Stuge B, Laerum E, Kikesola G, Vollestad N (2004) The efficacy of a treatment program focusing on specific stabilizing exercises for pelvic girdle pain after pregnancy: a randomized controlled trial. Spine 29: 351-359.
-
Becker I, Woodley SJ, Stringer MD (2010) The adult human pubic symphysis: a systematic review. J Anat 217: 475-487.
-
Atkins JM, Taylor JC, Kane SF (2010) Acute and overuse injuries of the abdomen and groin in athletes. Curr Sports Med Rep 9: 115-120.
-
Fitzgerald CM, Plastaras C, Mallinson T (2011) A retrospective study on the efficacy of pubic symphysis corticosteroid injections in the treatment of pubic symphysis pain. Pain Med 12: 1831-1835.
-
Hiti CJ, Stevens KJ, Jamati MK, Garza D, Matheson GO (2011) Athletic osteitis pubis. Sports Med 41: 361-376.
-
Choi H, McCartney M, Best TM (2011) Treatment of osteitis pubis and osteomyelitis of the pubic symphysis in athletes: a systematic review. Br J Sports Med 45: 57-64.
-
Hechtman KS, Zvijac JE, Popkin CA, Zych GA, Botto-van Bemden A (2010) A minimally disruptive surgical technique for the treatment of osteitis pubis in athletes. Sports Health 2: 211-215.
-
Vijayakumar P, Nagarajan M, Ramli A (2012) Multimodal physiotherapeutic management for stage-IV osteitis pubis in a 15-year old soccer athlete: a case report. J Back Musculoskelet Rehabil 25: 225-230.