International Journal of Surgery Research and Practice
Stone Ileus: An Unusual Presentation of Crohn's Disease
Charles Ma, H Tracy Davido*
Department of Critical Care and Acute Care Surgery, University of Minnesota Health, USA
*Corresponding author: H Tracy Davido MD, Assistant Professor of Surgery, Department of Critical Care and Acute Care Surgery, University of Minnesota Health, 11-115A Phillips Wangensteen Building, 420 Delaware St. SE, MMC 195, Minneapolis, MN 55455, USA, Tel: 612-626-6441, E-mail: davi1098@umn.edu
Int J Surg Res Pract, IJSRP-3-046, (Volume 3, Issue 2), Case Report; ISSN: 2378-3397
Received: March 04, 2016 | Accepted: September 27, 2016 | Published: September 30, 2016
Citation: Ma C, Davido HT (2016) Stone Ileus: An Unusual Presentation of Crohn's Disease. Int J Surg Res Pract 3:046. 10.23937/2378-3397/1410046
Copyright: © 2016 Ma C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Stone ileus, also known as enterolith ileus enterolithiaisis, is a rare complication of cholelithiasis and an even rarer symptom of Crohn's disease. Gallstone ileus is secondary to fistula formation between the gallbladder and the gastrointestinal (GI) system. Enterolithiasis of Crohn's disease is thought to arise from the stasis of succus within the small bowel eventually leading to stone formation and growth. Both gallstone ileus and enterolithiasis of Crohn's disease can result in subsequent mechanical bowel obstruction. Gallstone ileus accounts for 1% to 4% of mechanical bowel obstructions, with higher a incidence in women over age 60 [1]. But enterolithiasis of Crohn's disease, give its rarity, is not well represented in the literature. However, stone ileus, regardless of its etiology, is associated with significant morbidity and mortality, and it remains a clinically challenging diagnosis. The cornerstone of treatment is surgical, with an emphasis on prompt enterolithotomy after diagnosis. Reviews of the current literature often describe gallstone ileus in patients with a diseased intracorporeal gallbladder. We instead describe a case of stone ileus in a patient with a surgically absent gallbladder that was the initial presenting symptom of Crohn's disease. To date, we have found no reports in the literature of enterolith ileus as the presenting symptom of Crohn's disease.
Case Report
A 67-year-old morbidly obese woman came to the emergency department at our institution with an upper respiratory infection, decreased appetite, and malaise. Her past medical history was significant for an open cholecystectomy more than 30 years earlier. She had no additional past surgical history or diagnoses. The initial workup revealed acute renal failure, with significant electrolyte abnormalities and dehydration. She underwent intravenous fluid resuscitation and electrolyte replacement in the Medical Intensive Care Unit; however, while hospitalized, she developed new-onset nausea and vomiting. A nasogastric tube was placed, which returned 1800 mL of bilious fluid, and the surgery service was consulted.
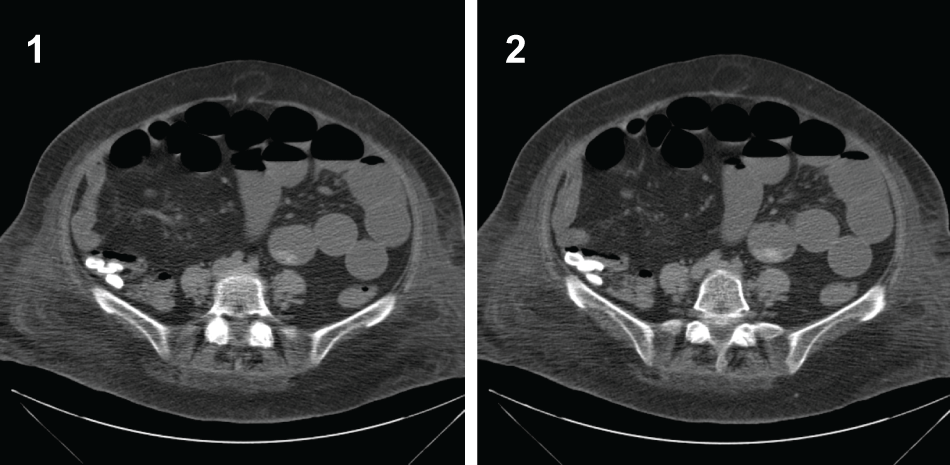
On further questioning, the patient revealed that she had had, for many years, intermittent severe cramping abdominal pain, diarrhea, nausea and vomiting. Her subsequent physical examination revealed a subcostal surgical scar in the right upper quadrant, consistent with an open cholecystectomy and a mildly distended abdomen without peritoneal signs. Laboratory tests results were within normal limits except for an elevated creatinine level. Abdominal computed tomography (CT) demonstrated radiopaque calcifications consistent with stone ileus in the right lower quadrant (Figure 1 and Figure 2).
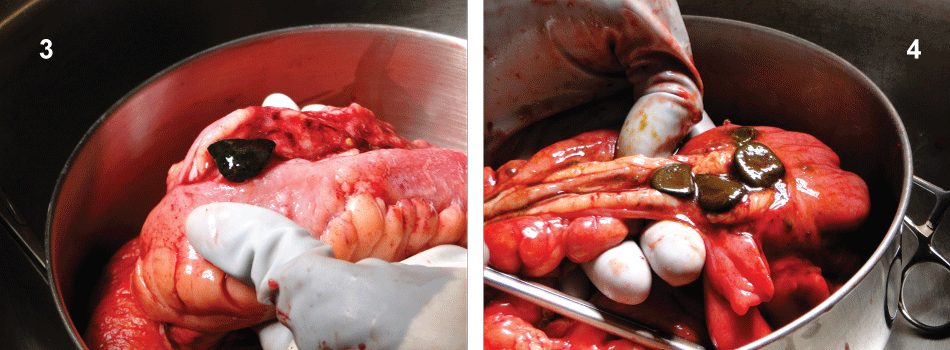
The patient then underwent an urgent exploratory laparotomy. We found dilated but viable small bowel with decompressed colon. Near the transition point, along the terminal ileum and cecum, we encountered severe inflammation with fat wrapping, adhesions, and edema. Given these circumstances, it was impossible to discern the exact number of stones present and their location, precluding an enterolithotomy. We therefore decided to perform an ileal cecectomy with a primary anastomosis to normal bowel tissue proximal to the terminal ileum and distal to the cecum. During our enterotomy of the removed specimen, we found 4 gallstones in the terminal ileum and 3 gallstones in the cecum. Their maximum dimension approached 2 cm (Figure 3 and Figure 4).
.
Figure 3 and 4: Intraoperative photos of ileocecectomy demonstrating significant scarring & induration, multiple obstructing enteroliths and creeping mesenteric fat.
View Figure 3 and 4
Pathologic examination of the specimen revealed small bowel mucosa with active chronic ileitis. Microscopic examination revealed transmural inflammation. But the colonic mucosa and lymph nodes were normal. Concomitant Crohn's disease could not be ruled out.
The patient's postoperative course was complicated by prolonged ileus, (requiring total parenteral nutrition) and by hypotension (requiring pressor support). Both conditions resolved by postoperative day 11. She resumed a soft mechanical diet. On postoperative day 16, she was discharged home. At her 1-month follow-up, she was in good health with normal bowel function. But at 6 weeks, she required a brief readmission to the hospital for dehydration secondary to choleretic diarrhea, which improved with intravenous fluids, Imodium, and Colestid. However, the final pathologic analysis of the specimen was concerning for inflammatory bowel disease, so she was subsequently referred to the gastroenterology service for ongoing treatment. The patient has since been treated as having Crohn's disease with continued amelioration of her GI symptoms.
Discussion
Small bowel obstruction due to enteroliths is exceedingly rare, and only a few such case reports exist in the literature [2,3]. The pathophysiology of Crohn's disease has been known to create enteroliths via stasis of small bowel contents, these small bowel stones tend to gather near the ileocecal junction, as do gallstones when passed into the GI tract. We believe that our patient is the first ever reported with bowel obstruction enterolithiasis as the presenting symptom of Crohn's disease. She also had a distant history of cholelithiasis and of an open cholecystectomy. Delayed gallstone ileus is even more rare, but also warrants review.
Gallstone ileus accounting for mechanical bowel obstruction is uncommon in the general population, but its incidence has been reported to be as high as 25% in older patients. Because of comorbidities, the associated mortality rate is also high, approaching 18% in select case series [4]. Diagnosis is often difficult and delayed; before gallstone ileus is even considered, other causes of small bowel obstruction are often thought of first, such as: adhesions, intussusception, tumors, hernias, volvulus, and foreign bodies. In patients with gallstone ileus, Rigler's triad, (the classic radiologic presentation consisting of small bowel obstruction, 1 or more ectopic gallstones, and pneumobilia), is seen on only 15% of plain radiographs [5]. Therefore, CT remains the imaging modality of choice [6].
Delayed gallstone ileus diagnosed more than 30 years after a cholecystectomy is rare. To our knowledge, only 1 similar case has been reported in the literature [7]. Fistula formation allows such stones to pass from the gallbladder into the small bowel. According to one systematic review, cholecystoduodenal fistulas are the most frequent, followed by cholecystocolonic fistulas [8]. Less common are cholecystogastric, cholecystocholedochal, choledochoduodenal, and cholecystojejunal fistulas. Impaction in the enteric system occurs with larger stones (> 2 cm and leads to obstruction, most commonly at the terminal ileum [9]. Symptoms often occur with intermittent obstruction as gallstones migrate down the GI tract, a process commonly referred to in the literature as a “tumbling obstruction.” For our patient, the working hypothesis is that the 2 cm stone was not large enough to completely obstruct the ileocecal valve and had intermittently acted as a ball valve for the past 30-plus years.
The mainstay of therapy for enterolith ileus is surgical with the objective to relieve the obstruction. Usually stone removal is achieved via an enterotomy proximal to the site of obstruction. Concomitant cholecystectomy and fistula closure at the time of enterotomy and bowel decompression is controversial; historically it has been reserved for good operative candidates. If perforation and technical limitations preclude an enterotomy, bowel resection is indicated. In their series, Reisner and Cohen reported a higher mortality rate in a 1-stage procedure (16.9%), as compared with enterolithotomy alone (11.7%). Halabi, et al. found that fistula closure and bowel resection during the initial procedure, as compared with an enterotomy alone, were independent risk factors for a higher mortality rate and a longer hospital stay [10]. In patients at risk for recurrence of enterolith ileus, we prefer interval cholecystectomy and fistula closure in an elective setting over a 1-stage procedure.
Conclusion
Our case report highlights the importance of considering enterolith ileus in the differential diagnosis of older patients with small bowel obstruction, even years after a cholecystectomy. And consideration of this rare presentation of Crohn's disease as the possible etiology of the patient's enterolithiasis and subsequent bowel obstruction.
References
-
Chou JW, Hsu CH, Liao KF, Lai HC, Cheng KS, et al. (2007) Gallstone ileus: report of two cases and review of the literature. World J Gastroenterol 13: 1295-1298.
-
Jones MW, Koper B, Weatherhead WF (2005) Crohn's disease with enterolith treated laparoscopically. JSLS 9: 339-341.
-
Perathoner A, Kogler P, Denecke C, Pratschke J, Kafka-Ritsch R, et al. (2012) Enterolithiasis-associated ileus in Crohn's disease. World J Gastroenterol 18: 6160-6163.
-
Reisner RM, Cohen JR (1994) Gallstone ileus: a review of 1001 reported cases. Am Surg 60: 441-446.
-
Lassandro F, Gagliardi N, Scuderi M, Pinto A, Gatta G, et al. (2004) Gallstone ileus analysis of radiological findings in 27 patients. Eur J Radiol 50: 23-29.
-
Lassandro F, Romano S, Ragozzino A, Rossi G, Valente T, et al. (2005) Role of helical CT in diagnosis of gallstone ileus and related conditions. AJR Am J Roentgenol 185: 1159-1165.
-
Zens T, Liebl RS (2010) Gallstone ileus 30 years status postcholecystectomy. WMJ 109: 332-334.
-
Petrowsky H, Clavien P (2006) Biliary fistula, gallstone ileus, and Mirizzi's syndrome. In: Clavien P, Baillie J, Diseases of the gallbladder and bile ducts: diagnosis and treatment. (2nd edn), Malden (MA): Blackwell Publishing, USA 239-251.
-
Day EA, Marks C (1975) Gallstone ileus. Review of the literature and presentation of thirty-four new cases. Am J Surg 129: 552-558.
-
Halabi WJ, Kang CY, Ketana N, Lafaro KJ, Nguyen VQ, et al. (2014) Surgery for gallstone ileus: a nationwide comparison of trends and outcomes. Ann Surg 259: 329-335.