International Journal of Surgery Research and Practice
Post-cardiotomy Rescue Extracorporeal Cardiopulmonary Resuscitation in Neonates with Single Ventricle after Intractable Cardiac Arrest: Attrition after Hospital Discharge and Predictors of Outcome
Anastasios C. Polimenakos1,2*, Patrice Wojtyla1, Vincent Rizzo1, Chawki F. ElZein1 and Michel N. Ilbawi1
1Division of Pediatric Cardiovascular Surgery, Advocate Hope Children's Hospital, Oak Lawn IL, Illinois, USA
2Division of Pediatric Cardiovascular Surgery, Children's Hospital of Georgia, Augusta GA, Georgia, USA
*Corresponding author: Anastasios C Polimenakos, MD, Associate Professor of Surgery, Medical College of Georgia, Director, Congenital Cardiovascular Surgery, Children's Hospital of Georgia, 1120 15th street, BAA8300, Augusta, GA 30907, Georgia, USA, E-mail: anapolisis@aol.com
Int J Surg Res Pract, IJSRP-3-039, (Volume 3, Issue 1), Research Article; ISSN: 2378-3397
Received: November 02, 2015 | Accepted: March 25, 2016 | Published: March 28, 2016
Citation: Polimenakos AC, Wojtyla P, Rizzo V, ElZein CF, Ilbawi MN (2016) Postcardiotomy Rescue Extracorporeal Cardiopulmonary Resuscitation in Neonates with Single Ventricle after Intractable Cardiac Arrest: Attrition after Hospital Discharge and Predictors of Outcome. Int J Surg Res Pract 3:039. 10.23937/2378-3397/1410039
Copyright: © 2016 Polimenakos AC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objectives: Extracorporeal cardiopulmonary resuscitation (ECPR) in children with cardiac arrest refractory to conventional cardiopulmonary resuscitation (CPR) has been reported with encouraging results. We reviewed outcomes of neonates with functional single ventricle (FSV) surviving post-cardiotomy ECPR after hospital discharge.
Methods: Fifty-eight patients who required post-cardiotomy extracorporeal membrane oxygenation (ECMO) since the introduction of our ECPR protocol (January 2007-December 2011) were identified. Forty-one were neonates. Survival analysis was conducted.
Results: Of 41 neonates receiving post-cardiotomy ECMO 32 had FSV. Twenty-one had ECPR. Fourteen underwent Norwood operation (NO) for hypoplastic left heart syndrome (HLHS). Seven had non-HLHS FSV. Four (of 7) underwent modified NO/DKS with systemic-to-pulmonary shunt (SPS), 2 SPS only and 1 SPS with anomalous pulmonary venous connection repair. Mean age was 6.8 ± 2.1 days. ECMO median duration was 7 days (interquartile range (IQR25-75: 4-18). Survival to ECMO discontinuation was 72% (15 of 21 patients) and at hospital discharge 62% (13 of 21 patients). The most common cause of late attrition was cardiac. At last follow-up (median: 18 months; IQR25-75:3-36) 47% of patients were alive. Duration of ECMO and failure of lactate clearance within 24 hours from ECMO deployment determined late survival after hospital discharge (p < 0.05).
Conclusions: Rescue post-cardiotomy ECMO support in neonates with FSV carries significant late attrition. ECMO duration and failure in lactate clearance after deployment are associated with unfavorable outcome.
Introduction
Since the first [1] reported use of extracorporeal membrane oxygenation (ECMO) its applications have expanded to include resuscitation after complex congenital heart disease (CHD). ELSO registry [2] and others [3] indicate that ECMO after repair of functional single ventricle (FSV) has poorer prognosis than other cardiac lesions.
Increased duration of CPR in neonates and infants with hospital cardiac arrest carries substantial morbidity and high mortality [2-7]. Extracorporeal cardiopulmonary resuscitation (ECPR) is the rapid deployment of ECMO to provide immediate cardiovascular support for patients who have cardiac arrest refractory-to-conventional-CPR strategies [3,8]. The demonstrable survival benefit of ECPR over conventional CPR strategies has resulted in steadily increasing ECPR application. Appropriate patient selection and institutional effectiveness to deploy ECMO in a timely fashion may influence outcome [8-12].
Since 2007, we have encountered post-cardiotomy neonates with FSV of any type for which our established ECPR protocol was utilized. Neonates with FSV receiving post-cardiotomy ECPR were identified and late outcomes assessed.
Patients and Methods
Fifty-eight patients who required post-cardiotomy ECMO since the introduction of our ECPR protocol (January 2007-December 2011) were identified. From 41 neonates receiving post-cardiotomy ECMO 32 had FSV. Twenty-three had ECPR. Two had a second ECMO run.
Patients were included in the ECPR group if venoarterial ECMO was used as part of the initial active resuscitation from a cardiac arrest. Patients hemodynamically unstable but without active cardiac arrest were excluded. A retrospective review was conducted and survival analysis undertaken.
Vasoactive-Inotrope score (VIS) was calculated as previously described [13]. VIS was classified as: (1) Class-I: ≤ 10, (2) Class-II: 11-14, (3) Class-III: 15-19, (4) Class-IV: 20-24, (5) Class-V: ≥ 25.
Systolic function was qualitatively evaluated by apical and parasternal short-axis images as (SVNL) normal myocardial function, (RVNL-1) mild-to-moderate myocardial dysfunction, and (SVNL-2) severe myocardial wall dysfunction. Echocardiograms were obtained within 24 hrs from ECMO deployment, during ECMO, prior to decannulation, at hospital discharge, and periodically thereafter. All echocardiograms were reviewed by an independent echocardiographer.
Significant adverse events were categorized as follows: (1) brain/neurological injury(BNI) (clinical or electroencephalographic seizures, significant central nervous system hemorrhage or ischemia, intraventricular hemorrhage (> grade-I) by ultrasound or computed tomographic scan); (2) renal injury (serum creatinine ≥ 1.7 mg/dL or need for dialysis); (3) sepsis; (4) respiratory complications (ventilator-associated pneumonia, acute respiratory distress syndrome, or pulmonary hemorrhage); (5) cardiac complications (SVNL-2, heart transplantation [HTxP] or other major cardiac event); (6) gastrointestinal complications; (7) bleeding (requiring intervention); (8) unplanned reoperation/reintervention; (9) multiple organ failure (MOF) (requiring medical intervention to maintain function).
ECMO decannulation was considered successful when "native'' circulation was maintained for 48 hours after decannulation without ECMO recannulation. Primary outcomes were survival to discharge from the hospital, late death (defined as death any time after hospital discharge), and "late attrition". "Late attrition" was the primary outcome and defined as the combined end-point involving late death, need for HTxP or failure to reach suitability for Fontan completion (CF).
Any patient who reached end-stage myocardial function or unsuitability for CF and no contraindication were present HTxP was offered as part of our Institution care protocol for patients with SV physiology.
The study was approved by the Institutional Review Board. Need for parental consent was waived.
Management principles
ECMO rapid deployment strategy, ECPR protocols and intensive care unit management were described in detail previously [14]. Indications and mode of deployment remained constant throughout the study. Once ECPR was required, the predefined protocol was initiated. Timing of weaning was dependent on hemodynamic stability during ECMO support, correction of the underlying cause, and the presence of residual cardiac lesions. Separation from ECMO assist was accomplished as previously described [14].
Statistical analysis
Data were expressed as mean ± standard deviation (SD) or median with interquartile range (25-75IQR) for continuous variables and as frequencies and percentages for categorical variables. Continuous variables were compared by using the Mann-Whitney and student-t tests, as appropriate. Fisher's exact test and chi-square analyses were used for dichotomous and categorical variables. The probability of freedom from events was estimated according to Kaplan-Meier method. For all end-points, time was measured from initiation of ECMO. All non-mortality secondary end-points were considered to have been censored in the event of late death, HTxP or determination of Fontan unsuitability. Univariate analysis was carried out using p-value of less than 0.05. SPSS 15.0.1 for Windows (SPSS Inc, Chicago, IL) was used.
Results
Patients characteristics
From 41 neonates receiving post-cardiotomy ECMO 32 had FSV. Twenty-one had an index course of ECPR. Fourteen underwent Norwood operation (NO) for hypoplastic left heart syndrome (HLHS). Pulmonary blood flow reconstitution was established with right ventricle-to-pulmonary-shunt (RVPAS) (n = 8) and modified Blalock-Taussig - shunt (mBTS) (n = 6). Seven neonates had non-HLHS FSV. Four underwent Damus-Kay-Stansel (DKS) or modified-NO (2RVPAS and 2mBTS). Three neonates underwent systemic-to-pulmonary shunt (SPS). One had obstructed anomalous pulmonary venous connection.
Mean age and weight were 7.5 ± 2.7 days and 3.57 ± 1.7 Kg, respectively. Three patients had gestational age less than 35 weeks at birth and 4 weighted less than 2.5 kg (LBW) at the time of surgical repair. Major indication for ECPR was acute cardiac arrest (17; 81%) and respiratory failure followed by cardiac arrest (4; 19%). The median interval between the beginning of CPR and the initiation of ECMO (CPR duration) was 36 minutes (IQR25-75: 25-52). Demographic and clinical data are depicted in table 1.
![]()
Table 1: Demographic and clinical variables: Survivors§ and non-survivors.
View Table 1
Early results and hospital survival
ECMO median duration was 7 days (IQR25-75 4-21). ECMO was successfully discontinued in 15 (72%) patients. All 15 maintained "native'' circulation for 48 hours. Thirteen (62%) patients survived to hospital discharge (Figure 1). Non-survivors had overall significantly more complications than survivors. One or combinations of them were present in over 70% of non-survivors compared to 30% of survivors (p 0.05).
.
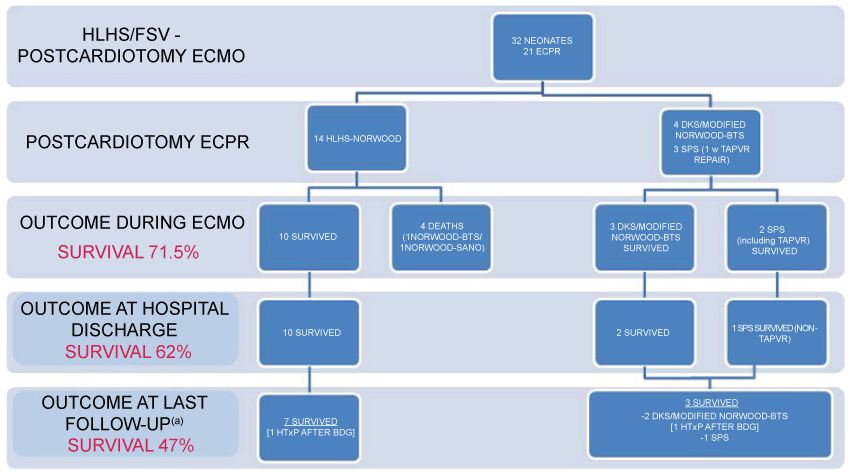
Figure 1: Longitudinal follow-up and outcome. Mean interval 17.4 ± 5.1 months.
BTS: Blalock-Taussig shunt; DKS: Damus-Kay-Stansel operation; FSV: Functional Single Ventricle; HLHS: Hypoplastic Left Heart Syndrome; SPS: systemic-to-pulmonary shunt; TAPVC: Total Anomalous Pulmonary Venous Connection; HTxP: Heart Transplantation
View Figure 1
The causes for hospital mortality included multi-organ failure (MOFS) (n = 6, 28%), sepsis or necrotizing enterocolitis (NEC) (n = 5, 24%), and intraventricular or cerebral hemorrhage (n = 4, 19%), failure of cardiac recovery (n = 2, 9%). There was one reoperation during ECMO for severe tricuspid valve insufficiency (NO-RVPAS). The patient suffered major intraventricular hemorrhage and ECMO support was withdrawn. Six more reoperations (2 in the same patient) were performed off ECMO and prior to hospital discharge. Only one survived hospital discharge. Both patients with GS/CA did not survive hospital discharge.
Seven patients during ECMO and 3 after decannulation required filtration or peritoneal dialysis. Four did not survive hospital discharge. Serum creatinine level and achieving negative fluid balance (within 72 hours following ECMO and 24 hours following decannulation from ECMO) were not statistically different between survivors and non-survivors (p 0.7).
There was echocardiographic evidence of ventricular recovery (SVNL or SVNL-1) within 48 hours following ECMO in 90% of survivors (vs 55% of non-survivors, p 0.08). More than 50% of those with SVNL-2 after 48 hours following ECMO did not survive hospital discharge. Early outcomes between ECPR survivors and non-survivors are summarized in table 2.
![]()
Table 2: Early ♦§outcomes: Survivors vs non-survivors
View Table 2
Late attrition and time-related events
At last follow-up [median: 18 months; IQR25-75: 3-36)] 47% of patients were alive and neurologically intact. Three patients died after hospital discharge at a mean interval of 5.7 ± 3.3 months. One died from NEC. Another died from acute shunt occlusion followed by cardiac arrest prior to arrival in the emergency room. The third had a ventricular fibrillation arrest in outside facility from which she succumbed.
After hospital discharge 2 survivors required HTxP after stage-II palliation at 7.9 and 16.3 months, respectively, due to severe heart failure. Both are alive at last follow-up.
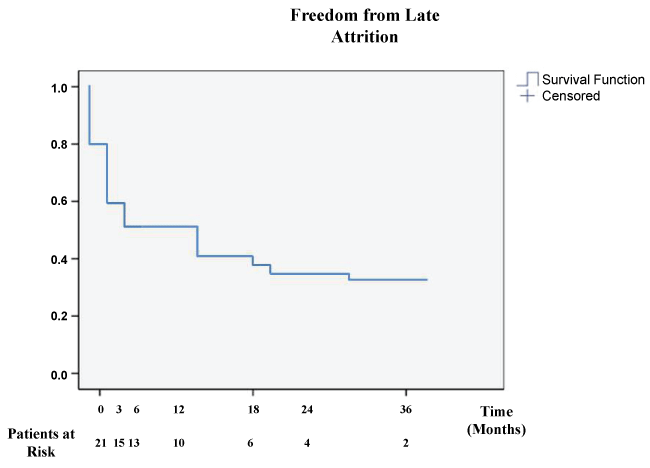
Freedom from late attrition at 3, 6, and 18, and 36 months was 59.2 ± 12.9%, 51.5 ± 14.7%, 41.6 ± 15.1%, and 34.3 ± 15.7%, respectively (Figure 2). For the extent of the follow-up period the combined end-point of attrition and survival attenuation progressed with an average rate of 0.71-0.75% and 0.42-0.45% per month, respectively.
The most common cause of late attrition was cardiac related. Late outcomes between survivors and non-survivors are summarized in table 3.
![]()
Table 3: Late §outcomes: Survivors vs non-survivors.
View Table 3
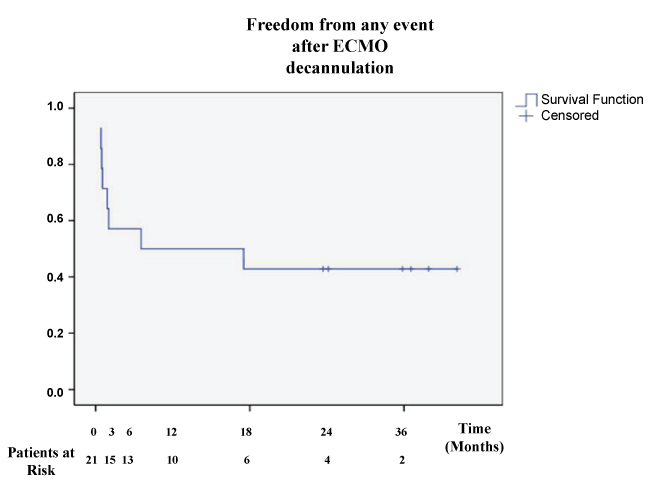
Freedom from any significant event (different than the primary end-points) after ECMO decannulation requiring readmission with the intent to treat (unplanned intervention/reoperation, end-organ adverse event) at 36 months was 42.1 ± 17.4% (Figure 3).
.
Figure 3: Freedom from any significant* event after ECMO decannulation.
*requiring readmission with the intent to treat (unplanned intervention/reoperation, end-organ adverse event)/events related to primary end-points are excluded.
View Figure 3
Risk factors for late survival
Mean CPR duration between ECPR-survivors and non-survivors was 37.2 ± 5.8 and 40.6 ± 6.9 minutes, respectively (p 0.09).
Median duration of ECMO between survivors and non-survivors was 4 days (IQR25-75: 3-7) and 9 days (IQR25-75: 6-13), respectively (p 0.01).
From 24 variables included, failure of serum lactate clearancewithin 24 hours following rescue ECMO (p 0.02) and ECMO duration (p 0.01) were associated with attenuated survival after hospital discharge (Table 1).
Discussion
Despite increasing experience with ECMO support in children with cardiac failure, survival over more than decade has remained unchanged [2-6,8,15,16].
Rescue-ECMO is a potentially lifesaving intervention to reverse refractory cardiopulmonary arrest after surgical intervention for CHD. When ECMO is deployed during CPR efforts outcomes vary and are, usually, poorer compared to non-rescue ECMO [4,8,17]. Neonates with FSV are more vulnerable to myocardial damage and less tolerant to any disturbance added to the demands of balancing two circulations [18]. Thus, the most important factor for achieving favorable outcome with ECPR is the prompt establishment of adequate organ perfusion. Once the decision is made, the target deployment time should not exceed 45 minutes.
The intended focus of this study was to assess the attrition toll observed after hospital discharge in neonates with complex FSV (including HLHS). As "late attrition" was considered, not only the physical demise (death) of the patient, but also, the failure in accomplishing long-term transition to total cavopulmonary connection (CF) or non-HTxP status.
The in-hospital survival (over 60%) is different from what has been reported by others with observed survival at hospital discharge between 34% to 52% [8,15,16,18,19] and favorably compared to those with postcardiotomy non-rescue ECMO [12,15,20,21].
Late mortality among hospital survivors after ECM Oranges between 4% to 12% [22]. The reported causes of death relate mainly to the underlying heart condition and/or associated illnesses rather than ECMO support itself. Our study indicated that late attrition after hospital discharge exceeded 25% for the combined end-point (death, HTxP or unsuitability for CF) with an average rate of 0.71-0.75% per month. This longitudinal analysis revealed that nearly two-thirds of studied patients were either dead, required HTxP or deemed not suitable candidates for CF.
As previously reported [10,14,17], CPR duration prior to ECMO deployment is not associated with decreased hospital or late survival. CPR adequacy and potential link of ineffective CPR to poor outcome were not assessed. Consistent with other studies [9,12,17,20,21,23] longer duration of extracorporeal supportcarries constant complement of risksand hasfuture deleterious effects on end-organ systems which may contribute to late attrition [24].
One consistent finding in other studies [11,12,20,21] is that serum lactate abnormal values indicate either the overall hypoperfusion before or oxygen delivery/extraction mismatch following ECMO deployment. We previously demonstrated [14] that peak serum lactate level (threshold value 8.9 mmol/L) within 24 hours following ECPR predicts unfavorable outcome. Furthermore, failure of serum lactate clearance within 24 hours after ECMO deployment is associated with late mortality in this series. We strongly advocate delivering higher initial ECMO flows after intractable cardiac arrest in FSV when end-organs including the myocardium have likely had a degree of hypoxic injury. However, persistent need for higher flows may represent ongoing myocardial dysfunction, residual defect or technically imperfect operative outcome. Persistent higher flows are likely to promote decreased lung compliance and plasma exchange; strong indicators of early mortality [23].
It is recommended that all hemodynamically significant residual lesions to be corrected prior to ECMO withdrawal, as this may impact not only successful transition to stable "native" circulation, but also, determine late cardiac performance. Planned echocardiographic evaluation helps to assess ventricular recovery, identify hemodynamically significant residual lesions, guide effective management and ECMO flows or determine the need for early HTxP. Attenuated myocardial recovery, despite prolonged ECMO support, calls for early consideration of alternative supportive (ventricular assist device) or replacement (HTxP) therapy.
Major complications are, rather, inherent phenomenon associated with ECMO [14,22,23]. Hemorrhagic events and increased transfusion requirements are reportedly associated with significant mortality and morbidity early after ECMO [20,24]. Meticulous hemostasis, cell salvage, judiciously escalating anticoagulation following ECMO, use of polymethylpentene-hollow-fiber oxygenator, and miniaturization of ECMO circuit with heparin-bonded biocompatible surface helped eliminating major bleeding complications and, thus, reducing exposure to blood products as demonstrated here.
Renal dysfunction following ECMO represents a surrogate marker of organ perfusion and it has been shown to influence morbidity [11,14,20,21]. Renal morbidity might extend beyond the immediate post-ECMO period.
Children undergoing ECMO are vulnerable to neuro developmental disability (NDD). Acute BNI after ECPR in neonates and infants were reportedly present in more than one third of survivors [6,7,25]. In ECMO survivors late after hospital discharge there have been varied disability rates dependent on the study's reported definition [23,25,26]. The incidence of BNI did not statistically differ between late survivors and non-survivors in our study. Due to the small sample and relatively short follow-up period no meaningful analysis of predictors was possible.
This series is subject to limitations of a single-site retrospectively ascertained patient cohort. Collection of variables was not under the control of investigator and therefore variables that could have had an important influence on outcome may not be available for analysis. Echocardiographic SV qualitative assessment carries inherent limitations especially in dominant right ventricle. Statistical significant differences might be hampered by the small sample and duration of follow-up. Finally, the relatively limited power of the study precluded logistic regression analysis.
In conclusion, despite the heavy toll in resources required, postcardiotomy ECMO for neonates with complex FSV and intractable cardiac arrestcarries a favorable outcome formorethan 60% of thepatients at hospital discharge. ECMO duration and serum lactate clearance within 24 hours following ECPR might influence late survival. Late attrition following hospital discharge exceeds a monthly rate of 0.7%. Cardiac-related events are the dominant cause for late attrition. An interdisciplinary structure and proficiency in ECMO deployment justifies an aggressive strategy towards timely application of ECPR when no other morbid conditions that severely limit survival are present. Early identification of patients requiring heart transplantation might improve late survival.
References
-
Baffes TG, Fridman JL, Bicoff JP, Whitehill JL (1970) Extracorporeal circulation for support of palliative cardiac surgery in infants. Ann Thorac Surg 10: 354-363.
-
ECMO (2002) Registry of extracorporeal life support organization (ELSO). Ann Arbor, MI.
-
Chow G, Koirala B, Armstrong D, McCrindle B, Bohn D, et al. (2004) Predictors of mortality and neurological morbidity in children undergoing extracorporeal life support for cardiac disease. Eur J Cardiothorac Surg 26: 38-43.
-
de Mos N, van Litsenburg RR, McCrindle B, Bohn DJ, Parshuram CS (2006) Pediatric in-intensive-care-unit cardiac arrest: incidence, survival, and predictive factors. Crit Care Med 34: 1209-1215.
-
Morris MC, Wernovsky G, Nadkarni VM (2004) Survival outcomes after extracorporeal cardiopulmonary resuscitation instituted during active chest compressions following refractory in-hospital pediatric cardiac arrest. Pediatr Crit Care Med 5: 440-6.
-
Thiagarajan RR, Laussen PC, Rycus PT, Bartlett RH, Bratton SL (2007) Extracorporeal membrane oxygenation to aid cardiopulmonary resuscitation in infants and children. Circulation 116: 1693-1700.
-
Rhodes JF, Blaufox AD, Seiden HS, Asnes JD, Gross RP, et al. (1999) Cardiac arrest in infants after congenital heart surgery. Circulation 100: II194-199.
-
Jacobs JP, Ojito JW, McConaghey TW, Boden BD, Chang AC, et al. (2000) Rapid cardiopulmonary support for children with complex congenital heart disease. Ann Thorac Surg 70: 742-749.
-
Aharon AS, Drinkwater DC Jr, Churchwell KB, Quisling SV, Reddy VS, et al. (2001) Extracorporeal membrane oxygenation in children after repair of congenital cardiac lesions. Ann Thorac Surg 72: 2095-2101.
-
Chen YS, Chao A, Yu HY, Ko WJ, Wu IH, et al. (2003) Analysis and results of prolonged resuscitation in cardiac arrest patients rescued by extracorporeal membrane oxygenation. J Am Coll Cardiol 41: 197-203.
-
del Nido PJ, Dalton HJ, Thompson AE, Siewers RD (1992) Extracorporeal membrane oxygenator rescue in children during cardiac arrest after cardiac surgery. Circulation 86: II300-304.
-
Hoskote A, Bohn D, Gruenwald C, Edgell D, Cai S, et al. (2006) Extracorporeal life support after staged palliation of a functional single ventricle: subsequent morbidity and survival. J Thorac Cardiovasc Surg 131: 1114-1121.
-
Gaies MG, Gurney JG, Yen AH, Napoli ML, Gajarski RJ, et al. (2010) Vasoactive-inotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass. Pediatr Crit Care Med 11: 234-238.
-
Polimenakos AC, Wojtyla P, Smith PJ, Rizzo V, Nater M, et al. (2011) Postcardiotomy extracorporeal cardiopulmonary resuscitation in neonates with complex single-ventricle: analysis of outcomes. Eur J Cardiothorac Surg 40: 1396-1405.
-
Alsoufi B, Al-Radi OO, Gruenwald C, Lean L, Williams WG, et al. (2009) Extra-corporeal life support following cardiac surgery in children: analysis of risk factors and survival in a single institution. Eur J Cardiothorac Surg 35: 1004-1011.
-
Hannan RL, Ojito JW, Ybarra MA, O'Brien MC, Rossi AF, et al. (2006) Rapid cardiopulmonary support in children with heart disease: a nine-year experience. Ann Thorac Surg 82: 1637-1641.
-
Alsoufi B, Al-Radi OO, Nazer RI, Gruenwald C, Foreman C, et al. (2007) Survival outcomes after rescue extracorporeal cardiopulmonary resuscitation in pediatric patients with refractory cardiac arrest. J Thorac cardiovasc Surg 134: 952-959.
-
Pizarro C, Davis DA, Healy RM, Kerins PJ, Norwood WI (2001) Is there a role for extracorporeal life support after stage I Norwood? Eur J Cardiothorac Surg 19: 294-301.
-
Raymond TT, Cunnyngham CB, Thompson MT, Thomas JA, Dalton HJ, et al. (2010) Outcomes among neonates, infants and children after extracorporeal cardiopulmonary resuscitation for refractory in-hospital pediatric cardiac arrest. Pediatr Crit Care Med 11: 362-371.
-
Kumar TK, Zurakowski D, Dalton H, Talwar S, Allard-Picou A, et al. (2010) Extracorporeal membrane oxygenation in postcardiotomy patients: Factors influencing outcome. J Thorac Cardiovasc Surg 140: 330-6.
-
Kolovos NS, Bratton SL, Moler FW, Bove EL, Ohye RG, et al. (2003) Outcome of pediatric patients treated with extracorporeal life support after cardiac surgery. Ann Thorac Surg 76: 1435-1441.
-
Brown KL, Ichord R, Marino BS, Thiagarajan RR (2013) Outcomes following extracorporeal membrane oxygenation in children with cardiac disease. Pediatr Crit Care Med 14: S73-83.
-
Chrysostomou C, Morell VO, Kuch BA, O'Malley E, Munoz R, et al. (2013) Short- and intermediate-term survival after extracorporeal membrane oxygenation in children with cardiac disease. J Thorac Cardiovasc Surg 146: 317-325.
-
Hadley JS, Wang JE, Michaels LC, Dempsey CM, Foster SJ, et al. (2007) Alterations in inflammatory capacity and TLR expression on monocytes and neutrophils after cardiopulmonary bypass. Shock 27: 466-473.
-
Barrett CS, Bratton SL, Salvin JW, Laussen PC, Rycus PT, et al. (2009) Neurological injury after extracorporeal membrane oxygenation use to aid pediatric cardiopulmonary resuscitation. Pediatr Crit Care med 10: 445-451.
-
McMullan DM, Thiagarajan RR, Smith KM, Rycus PT, Brogan TV (2014) Extracorporeal cardiopulmonary resuscitation outcomes in term and premature neonates*. Pediatr Crit Care Med 15: e9-9e16.