International Journal of Surgery Research and Practice
Ranking and Rating Analyses of Barriers to Surgical Care for Children in Guatemala
Brian C Gulack1, Shirin Heydari2, Ligia Figueroa3, Shannon Tew4, Brad M Taicher4, Sherry S Ross5, David Boyd6 and Henry E Rice1,6*
1Department of Surgery, Duke University Medical Center, Durham, NC, USA
2Mending Kids International, Burbank, California, USA
3Moore Pediatric Surgical Center, Guatemala City, Guatemala
4Department of Anesthesiology, Duke University Medical Center, Durham, NC, USA
5Department of Urology, University of North Carolina-Chapel Hill, Chapel Hill, NC, USA
6Duke Global Health Institute, Duke University, Durham, NC, USA
*Corresponding author: Henry E Rice, MD, Division of Pediatric Surgery, Duke University Medical Center, Durham, Box 3815, NC, 27710, USA, Tel: (919)-681-5077, Fax: (919)-681-8353, E-mail: rice0017@mc.duke.edu
Int J Surg Res Pract, IJSRP-2-032, (Volume 2, Issue 2), Original Article; ISSN: 2378-3397
Received: October 28, 2015 | Accepted: November 18, 2015 | Published: November 20, 2015
Citation: Gulack BC, Heydari S, Figueroa L, Tew S, Taicher BM, et al. (2015) Ranking and Rating Analyses of Barriers to Surgical Care for Children in Guatemala. Int J Surg Res Pract 2:032. 10.23937/2378-3397/1410032
Copyright: © 2015 Gulack BC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Barriers to surgical care for children in low and middle income countries (LMICs) remain poorly defined. In this study, we used two consumer decision analysis tools to measure how families view the importance of different barriers to pediatric surgical care in Guatemala.
Methods: Our subject population was a convenience sample of parents or guardians of children receiving surgical care at a single non-governmental organization in Guatemala City. Respondents performed rating and ranking surveys to determine the relative importance of eight barriers to surgical care using a structured questionnaire.
Results: We included 46 respondents in this study. By rating analysis, the most significant barriers to care were the cost of surgery, perceived quality of care, and transportation issues. By ranking analysis, the most significant barriers to care were the cost of surgery, waiting time for surgery, and perceived quality of care.
Conclusions: Based on rating and ranking analyses, the cost of care is the most significant barrier to pediatric surgical care in Guatemala, although perceived quality of care is also important for families. Using complementary analysis tools provided enhanced insight into how families view the importance of different barriers to care, and should help policy makers develop programs to enhance surgical access for children.
Keywords
Pediatric surgery, Global surgery, Barriers to care
Introduction
Barriers to surgical care in low and middle-income countries (LMICs) remain poorly understood. This is particularly true of surgical care for children, where families are required to make complex decisions amidst multiple obstacles. Unmet surgical care contributes to at least 11% of the global burden of disease [1]. For many disease processes in children, surgery is a cost-effective health intervention, as it results in a high degree of averted disability-adjusted life years (DALYs) with costs comparable to many other health interventions [2].
Guatemala has a fractionated health care system which limits access to surgical care [3]. The Guatemalan health system is made up of three major components: the public health system through the Ministry of Public Health and Social Welfare, social insurance through the Guatemala Social Security Institute, and private care [3]. Health care financing and capacity have not increased in recent decades, resulting in a deficiency of coverage [3-5]. International and national non-governmental organizations (NGOs) are increasingly used to fill these gapsin health care, with several hundred health care NGOs currently in operation in Guatemala [3,5-7].
Previous studies have suggested that barriers to surgical care in LMICs are multiple, and include issues of accessibility, affordability, or acceptability [8-10]. In Guatemala, financial factors are among the most important barriers for families seeking surgical care, although issues such as trust, quality of care, and language are also important [6,7,10]. Most studies examining barriers to surgical care are usually performed using self-reported questionnaires, and generally do not measure the relative importance of different barriers for families or how the effects of different barriers may be interlinked.
Business-analysis tools, including consumer rating and ranking scales, offer quantitative approaches to measure how people view different variables when making complex decisions, such as seeking access to surgical care. Rating systems, which ask an individual to assign an importance value for each barrier, determine the order of importance of a list of variables, although multiple barriers can ranked at the same level [11]. Ranking scales force a respondent to choose between each variable, although they do not determine how significant the difference is between variables [11,12]. Each of these analytic tools offers complementary information to understand how people view different variables that impact decision making. The purpose of this study was to compare the significance of different barriers to surgical care for children in Guatemala using rating and ranking surveys. Understanding which barriers are most important for families may assist in the development of policies to increase access to surgical care for children.
Materials and Methods
Study recruitment
Study subjects included one parent or guardian (hereafter referred to as parent) of children receiving care during April 2013 at the Moore Pediatric Surgical Center (Centro QuirurgicoPediatrico Moore), which is a NGO based surgical center in Guatemala City. Previous studies have confirmed that families choose to seek care at this clinic when they are not able to access care in the public health sector or other part of the health system [10]. Children of the respondents were undergoing a range of general surgical and urology procedures, performed by a U.S. team working alongside with Guatemalan staff. Using convenience sampling, 51 parents were invited to participate by a clinical social worker or health promoter of a total of 85 families being considered for surgical intervention. Of these 51 families, 46 parents enrolled in the study, and five declined study enrollment. All interviews were conducted in Spanish or the interviewee's primary indigenous language with the use of a trained interpreter during the child's hospital stay.
The Duke University Medical Center Institutional Review Board determined this study exempt from review. Families were enrolled in this study after reviewing the risks and benefits with the interviewer and having an opportunity to ask questions. All parents signed an informed consent document with the help of a trained interpreter. All collected information was de-identified, with no protected health information recorded.
Questionnaire instrument
Following study enrollment, each respondent completed a structured questionnaire (Appendix) designed to collect their opinions about issues which affected their own access to surgical care in Guatemala. We collected demographic data, including child age, gender, distance the patient lived from the clinic, and yearly family income as well as operative data including the type of operation. The questionnaires contained two separate sections, one in which barriers to surgical care were rated for significance, and the other in which they were ranked.
For the rating portion, each parent was asked to rate the importance of eight barriers to care in Guatemala which led to them seeking care at this center. These barriers were chosen based on our previous research as well as other studies of surgical barriers in LMICs, and included the cost of surgery, distance to hospital, waiting time for surgery, language barriers, transportation issues, ability to take time off of work, quality of care at an available institution, and lack of local surgical health center [7,9,13]. We used a Likert scale to assess the significance of each barrier, which were rated from 1 (least significant) to 5 (most significant) [14]. For the ranking portion, we asked each parent to rank the same eight barriers in order of significance, using a scale from 1 (most significant) to 8 (least significant). Questionnaires were available in English and Spanish, and translators worked individually with each parent to ensure each question was fully understood.
Statistical analysis
We summarized parametric continuous datausing means and standard deviation, and non-parametric continuous datausing medians and interquartile ranges (IQR). All categorical data were summarized in count and percentage form. We determined the median rating and ranking along with interquartile range for each barrier to surgical care. Barriers to care were ranked from most to least significant for both types of analyses, and compared. All data analysis was performed using R version 3.1.0 (Vienna, Austria).
Results
This study included 46 parents of children undergoing surgery. The median age of the children was 6.5 years (Interquartile range [IQR]: 2,10, Table 1), and 12 (26.1%) children were female. The most common surgical procedures included orchiopexy (18, 39.1%) and hernia repair (17, 37.0%). Other procedures included lipoma excision, fibroid excision, keloid resection, hydrocele repair, hypospadias repair, and orchiectomy. Median distance travelled to the clinic was 75 km (IQR: 25, 125).The median waiting time (from time surgery was determined to be required to the operation) was 14.5 months (IQR: 6.5, 36).
![]()
Table 1: Demographics of children undergoing surgical procedures.
View Table 1
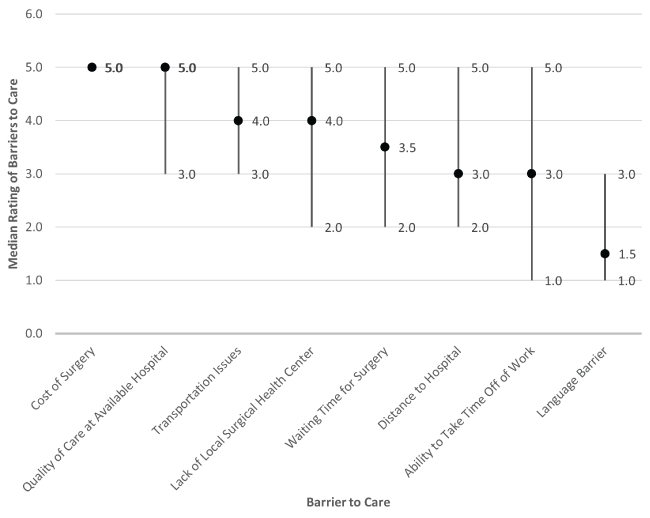
Rating assessment demonstrated that the cost of surgery (median rating: 5, IQR: 5, 5) and the perceived quality of care (median rating: 5, IQR: 3, 5) were the most significant barriers to surgical care, with language differences the least significant barrier (median rating: 1.5, IQR: 1, 3, Figure 1). Ranking analysis of these same barriers demonstrated that the cost of surgery was the most significant barrier to care (median ranking: 1, IQR: 1, 7.8), however waiting time for surgery was also of significance to families (median ranking: 3, IQR: 2.2, 4, Figure 2). A lack of local surgical health centerwas the least significant barrier (median ranking: 5, IQR: 4, 7).
.
Figure 1: Median rating for each barrier to surgical care along with interquartile range. Variables are ordered from highest median rating (5) to lowest (1).
View Figure 1
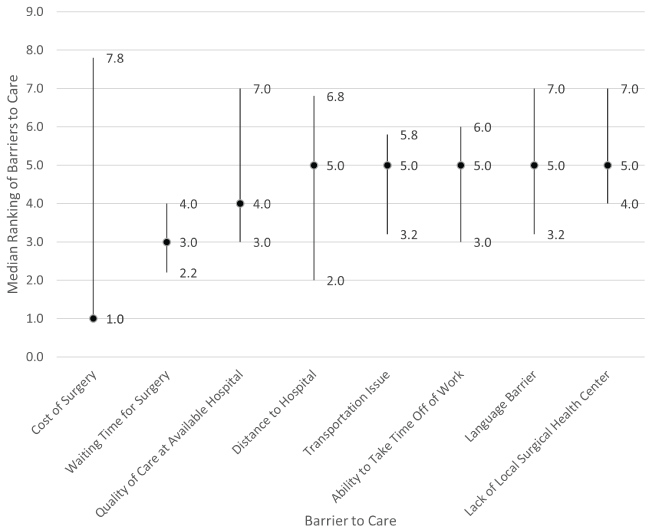
.
Figure 2: Median ranking for each barrier to surgical care along with interquartile range. Variables are ordered from most significant median ranking (1) to least (8).
View Figure 2
Comparison of rating and ranking results demonstrated several differences between the two methods (Figure 3). The cost of surgery was the most significant barrier to surgical care in both the rating and ranking analyses. However, the perceived quality of care was the second most significant barrier based on the rating scale, but was the third highest using the ranking scale. Furthermore, the waiting time for surgery was the fifth most significant barrier in the rating results, although it was the second most significant barriers in the ranking results.
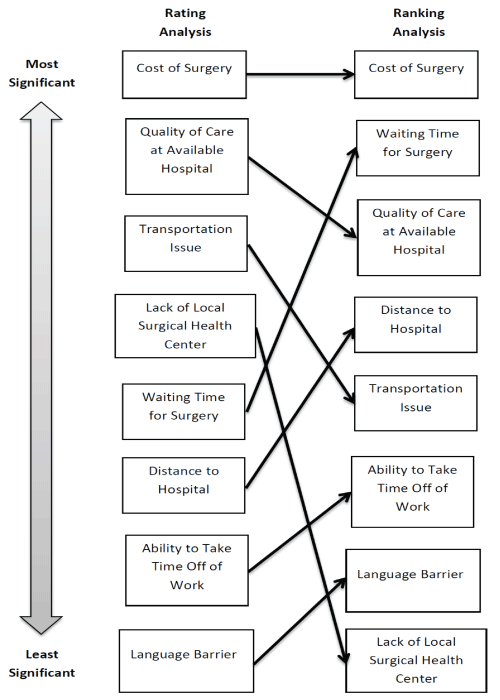
.
Figure 3: Comparison between rating and ranking analyses of barriers to care. Barriers were listed in order from most to least significant by median/interquartile range for rating and ranking analyses. Arrows were drawn to demonstrate the differences in the findings of the two types of analyses.
View Figure 3
Discussion
Inadequate access to surgical care in LMICs remains a significant global health concern, particularly for children [8]. In this study, we used two decision-analysis tools, rating and ranking scales, to measure how parents view different barriers to surgical care for children in Guatemala. We found those financial barriers and the perceived quality of care are the most significant obstacles to surgical care in Guatemala using rating and ranking analyses. Language barriers and ability to take time away from work were the least significant barriers. There was some variation between the two analyses with regards to other barriers. For example, the significance of the lack of a local surgical health center was the fourth most significant barrier in the rating analysis, but the eighth in the ranking analysis.
Our findings confirm most studies using other research methods that have shown that financial barriers as well as the quality of care are the dominant barriers to accessing surgical care in many LMICs [7,13,15]. Our results also align with case studies of NGOs providing care in Guatemala, which have shown the importance of quality of care and trust in this health system during decisions to seek care [5,6]. As Guatemala has a public health care system which offers free or reduced cost surgical care for children, the significance of cost as the most important barrier suggests that financial issues other than the direct cost of care, such as lost wages, drug costs or other financial strains, impact how families access surgical care. As the perceived quality of care was of great important to most families, this suggests that trust in existing health systems affect how families access surgical care for their children, and outweighs the importance of other barriers such as language or transportation.
The ability to receive surgical care depends on many factors, which are commonly framed as issues of accessibility, affordability, and availability [9,10]. These concepts and have been described as a Three Delays framework, including delays in seeking care, delays in reaching care, and delays in receiving care [8]. Our current study support the role of all of these delays in Guatemala, particularly delays in seeking care due to financial and geographic restrictions as well as low confidence in public health services.
In contrast to previous studies in Guatemala which have shown the importance of distance on access to primary care services, we have demonstrated that distance to a hospital and the lack of a local hospital are among the least significant barriers to surgical care [16-18]. Although this finding may be related to our specific patient population, it is unlikely as many of our subjects waited a significant time for surgery, and therefore was likely dealing with other issues unrelated to the actual distance to a surgical center.
The use of two complementary analysis tools demonstrates some discrepancies in results, and is of importance to interpretation of our findings. Rating systems, which assign a value for each barrier, can be used to determine the order of importance of a list of variables to an individual [11]. However they do not force a respondent to choose between two barriers, which can lead to multiple barriers being ranked at the same level [11]. Ranking scales force a respondent to choose between each variable, however they do not determine how significant the difference is between two variables [11,12]. Although rating systems are relatively simple and can easily indicate which of two variables is of greater importance, it can be difficult to determine the actual difference between variables when many variables are of similar significance [11]. Ranking methods forces a respondent to determine the order of the significance of a list of variables, but it does not allow them to suggest that two variables are more similar in importance than two others [11]. Ranking is also more conceptually taxing than simple rating, which can limit its accuracy and may be of concern in a setting with language barriers or where participants may have limited education [11]. Researchers who use these analytic tools should be aware of the inherent limitations of each approach.
There are several limitations in our study. Most importantly, we examined the views of families who chose to access surgicalcare at a single site NGO-based site, and their experiences may not be generalizable to those who use the public sector or those who cannot access care. However, all of our respondents had previous experiences with the public sector, which impacted their decision to seek care outside of that system. Second, our study population was primarily ladino and Spanish-speaking, and under-representative of the indigenous Mayan population in Guatemala [7]. This sampling bias may explain why language barriers and the ability to take time off of work were the least significant barriers to care in our study, which contrasts with other studies which demonstrate the importance of language barriers on healthcare access in Guatemala [5,19]. Third, the rating portion of the survey was asked before the ranking portion, and therefore mental exhaustion may have reduced accuracy of the ranking portion. Future studies should vary the order of testing to control for these confounders.
In conclusion, using rating and ranking analyses, we have demonstrated that the cost of care and the perceived quality of care at an available hospital are the most significant barriers for children receiving NGO-based surgical care in Guatemala. Language barriers and the ability to take time off of work are among the least significant. Efforts to decrease barriers to pediatric surgical care should focus on decreasing the cost of surgery as well as to increase the quality of care at available institutions. However, the interplay between barriers as families access surgical care systems is still not completely understood, and further study of these processes is critical to assist policy makers in developing programs to enhance access to surgical care for children.
Acknowledgements
We would like to acknowledge the support of Allison Bender, Ken Moore, Maria Jose de Gallardo and the staff at the Moore Pediatric Surgical Center for their invaluable assistance.
Conflicts of Interest
None of the authors have any conflicts of interest to disclose.
Authors' Contributions
BCG and HER: Conceived the study. BCG, BT, SR, and DB: Developed the methodology. BCG: Developed the questionnaire. SH, LF, and ST: Contributed to data collection. BCG: Performed the statistical analysis. BCG and HER: Drafted the manuscript. SH, LF, ST, BT, SR, and DB: Critically revised the manuscript. All authors read and approved the final manuscript. BCG and HER are guarantors of the paper.
References
-
Debas HT, Gosselin R, McCord C. Surgery (2006) In: Jamison D, Breman J, Measham A, (eds). Disease control priorities in developing countries. 2nd (edn). New York: Oxford University Press, 1245-1260.
-
Ozgediz D, Poenaru D (2012) The burden of pediatric surgical conditions in low and middle income countries: a call to action. J Pediatr Surg 47: 2305-2311.
-
Bowser DM, Mahal A (2011) Guatemala: the economic burden of illness and health system implications. Policy 100: 159-166.
-
Owen KK, Obregon EJ, Jacobsen KH (2010) A geographic analysis of access to health services in rural Guatemala. Int Health 2: 143-149.
-
Rohloff P, Diaz AK, Dasgupta S (2011) "Beyond Development": A critical appraisal of the emergence of small health care non-governmental organizations in rural Guatemala. Human Organization 70: 427-37.
-
Berry NS (2014) Did we do good? NGOs, conflicts of interest and the evaluation of short-term medical missions in Solola, Guatemala. Soc Sci Med 120: 344-351.
-
Nguyen K, Bhattacharya SD, Maloney MJ, Figueroa L, Taicher BM, et al. (2013) Self-reported barriers to pediatric surgical care in Guatemala. Am Surg 79: 885-888.
-
Meara JG, Leather AJM, Hagander L, Alkire BC, Alonso N, et al. (2015) Global Surgery 2030: Evidence and solutions for achieving health, welfare, and economic development. The Lancet 386: 569-624.
-
Grimes CE, Bowman KG, Dodgion CM, Lavy CB (2011) Systematic review of barriers to surgical care in low-income and middle-income countries. World J Surg 35: 941-950.
-
Stewart BT, Gyedu A, Abantanga F, Abdulai AR, Boakye G, et al. (2015) Barriers to Essential Surgical Care in Low- and Middle-Income Countries: A Pilot Study of a Comprehensive Assessment Tool in Ghana. World J Surg 39: 2613-2621.
-
Alwin DF, Krosnick JA (1985) The measurement of values in surveys: A comparison of ratings and rankings. Public Opinion Quarterly 49: 535-552.
-
Ryan M, Scott DA, Reeves C, Bate A, van Teijlingen ER, et al. (2001) Eliciting public preferences for healthcare: a systematic review of techniques. Technol Assess 5: 1-186.
-
Garrett S, Roche S, Rylands L, Sandoval M, Hall-Clifford R (2011) An investigation of the surgical referral process utilized by non-governmental organizations in Guatemala. Antigua, Guatemala: NAPA-OT Field School.
-
Likert R (1932) A technique for the measurement of attitudes. Archives of Psychology 140: 1-55.
-
Brockington M, Fathima S, Nandi M, Silverberg B (2013) NGO Networks for Health: Patient experiences of surgical missions in Guatemala. Antigua, Guatemala: NAPA-OT Field School.
-
Danel I, LaForgia GM (2005) Contracting for basic healthcare in rural Guatemala-Comparison of the performance of three delivery models. In: LaForgia GM, (ed). Health System Innovations in Central America: Lesson and Impact of New Approaches. Washington DC: The World Bank.
-
Bruce N, Pope D, Arana B, Shiels C, Romero C, et al. (2014) Determinants of care seeking for children with pneumonia and diarrhea in Guatemala: implications for intervention strategies. Am J Public Health 104: 647-657.
-
Kowalsky RH, Newburger JW, Rand WM, Castaneda AR (2006) Factors determining access to surgery for children with congenital cardiac disease in Guatemala, Central America. Cardiol Young 16: 385-391.
-
Hinojosa SZ (2004) Authorizing tradition: vectors of contention in Highland Maya midwifery. Soc Sci Med 59: 637-651.





