International Journal of Surgery Research and Practice
Utilizing Patient Perspectives to Help Reduce Postoperative Readmission Rates
Vanessa Nomellini*, Sarah E Tevis, Mary O'Leary, Maria Brenny-Fitzpatrick, Tamara LeCaire, Gregory D Kennedy, Emily R Winslow and Sharon M Weber
Department of Surgery, University of Wisconsin Hospitals and Clinics, Madison, WI, USA
*Corresponding author: Vanessa Nomellini, MD, PhD. Department of Surgery, University of Wisconsin, 600 Highland Avenue, Madison, WI 53792-7375, USA, Tel: (608) 265-0500, Fax: (608) 252-0913, E-mail: vnomellini@uwhealth.org
Int J Surg Res Pract, IJSRP-2-030, (Volume 2, Issue 2), Case Report; ISSN: 2378-3397
Received: September 04, 2015 | Accepted: October 26, 2015 | Published: October 29, 2015
Citation: Nomellini V, Tevis SE, O'Leary M, Brenny-Fitzpatrick M, LeCaire T, et al. (2015) Utilizing Patient Perspectives to Help Reduce Postoperative Readmission Rates. Int J Surg Res Pract 2:030. 10.23937/2378-3397/1410030
Copyright: © 2015 Nomellini V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: CMS recently began penalizing hospitals for readmissions if they exceeded benchmark rates. While many strategies have been proposed to help minimize readmissions, none have evaluated surgical patients' perspectives.
Study design: All patients with unplanned readmissions within 30 days of discharge from a general surgery service over a three month period were interviewed. Patients admitted to a general surgery service from 2011 - 2012 as identified by the NSQIP database were used as a comparison.
Results: A total of 50 patients were enrolled in the study. There were no differences between the study patients and NSQIP patients in terms of age or gender, but there was a significant difference in ASA class (p < 0.01). The majority of patients had a scheduled follow up appointment, however 66% were readmitted before they were able to attend and 6% were readmitted from their postoperative clinic visit. When asked about suggestions to improve discharge planning, 50% were satisfied with the process. Among the other half, 32% suggested improving discharge instructions, 28% advocated for better communication within the care team, 12% felt the discharge process was too long, 12% thought they were discharged too soon, and 8% suggested better communication with family.
Conclusions: Understanding the perspectives of surgical patients allows providers to identify targets for quality improvement aimed at reducing readmissions. Using this concept, systems can be developed which target high-risk patients in need of early follow-up, with the ultimate goal of lowering postoperative readmission rates.
Keywords
Patient perspectives, Patient suggestions, Readmission, Surgery, Discharge planning, Adult, Healthcare
Introduction
In recent studies, the centers for medicare and medicaid services (CMS) have acknowledged that hospital readmissions are "prevalent and costly" [1,2]. These studies show that about 20% of all Medicare patients are readmitted within 30 days of discharge from the hospital. From this analysis, it was concluded that excessive re-hospitalization is a marker of poor quality and high cost, as reiterated by other studies [1-6]. As a result, hospitals with all-cause readmission rates greater than the national benchmark are now being assessed more carefully and have the potential for payment penalties. It was recently shown that, in specific postoperative patient populations, the risk of hospital readmission is primarily related to patient factors. Only 4% of the variation in readmission rates could be attributed to hospital factors and less than 1% to surgeon volume [7,8]. While it is crucial that institutions focus their efforts to reduce readmission rates, it is important to recognize that a different strategy may be necessary for surgical patients compared with medical patients [8].
A number of tools have been created as an attempt to decrease hospital readmission rates [9-11]. However, these tools may not be applicable at all institutions, since they do not address differences in the specific patient population and the individual community resources, which is fundamental to improving transitions of care [9,10]. In addition, it has become clear that most risk-prediction tools are inadequate [5]. Due to these limitations, and with the increasing focus on patient and family-centered care, we sought to determine whether patient perspectives can elucidate novel approaches to improve the discharge process, with the ultimate goal of preventing unnecessary readmissions. Therefore, a pilot study to obtain feedback from patients who were readmitted to a general surgery service within 30 days of discharge was performed.
Methods
This study included all patients initially admitted to a general surgical service who were readmitted within 30 days of discharge at University of Wisconsin Hospital. A total of 59 patients were readmitted over a three month period. Patients were excluded if they were readmitted for a planned elective surgery.
Within the first day of admission, patients were asked five questions about their discharge process and disposition. To be sure the patients' answers were not influenced by the presence of the physicians on their care team, the questions were asked by the Nurse Case Managers during their usual intake survey, which includes objective questions, such as the type of insurance they carry. Four of these questions were objective and one was open-ended. The questions in order of presentation were: "Did you have a follow up visit scheduled with your doctor?", "Who is the primary caregiver that assists with patient care?", "Did you have a clear understanding of your health care instructions when you left the hospital?", "Who is the primary caregiver that assists with patient care?", and "What suggestions do you have to improve planning for your discharge from the hospital?". The open ended questions were analyzed by content analysis and themes were identified by three separate individuals. The themes generated by all three individuals were then compared and found to be identical, providing validation for the results [12].
To assure the demographics of our patient population was representative of our overall population, a comparison group of patients from our institutional NSQIP data was analyzed, inclusive of 2011 and 2012. The total number of patients included in this comparison arm was 948. Since our study group only included readmitted patients, we also compared the readmitted patients captured by NSQIP between 2011 and 2012 for a separate analysis. Of note, NSQIP captures readmissions up to 30 days after surgery, as opposed to 30 days after discharge, and includes all readmissions.
Chi square tests were used to evaluate for associations between patients in the study group and the NSQIP comparison group. Statistics were performed using SPSS statistical program (IBM, Armonk, New York). A p value of < 0.05 was considered statistically significant.
Results
Patient demographics
Of the 59 patients readmitted to a general surgery service during the three month study period, nine were excluded because they were readmitted for a planned procedure. As a result, a total of 50 patients were included in the study. Based on admissions data, the total number of patients admitted to a general surgery service during the same period of time was 1,250, putting our overall readmission rate at 4%, which is lower than our overall institutional readmission rate of around 10% [13].
Table 1 shows the characteristics of the population studied. In order to determine whether patients were representative of the overall group of readmitted patients, comparison was made to those captured in NSQIP from 2011 to 2012. As shown in table 1, there was no significant difference in age or gender between the readmitted patients from the current study and those who were readmitted between 2011 and 2012 as identified by NSQIP. When comparing ASA class, on the other hand, there were no patients in the current study who were ASA class 5. As a result, there was a significant difference between the study group and the patients identified by NSQIP. To be sure this was adequate sampling, the study group was also compared to the overall population of patients admitted to a general surgery service between 2011 and 2012 identified by NSQIP and no differences were found between age or gender, but ASA class was statistically different (Table 1).
![]()
Table 1: Patient demographics compared with the 2011-2012 NSQIP database.
View Table 1
Reasons for readmission
When analyzing the reasons for readmission in our study group, a severe intra-abdominal process requiring intervention was the most frequent diagnosis (30%) as shown in table 2. These processes included intra-abdominal abscess, bleeding, perforation, or evisceration requiring an operation or invasive procedure. Other common reasons were nausea, vomiting, and dehydration with no identifiable cause (22%), bowel obstruction (20%), and a superficial wound problem (16%). Less frequently patients were readmitted with a hernia (4%), GI bleeding (4%), uncontrolled pain with no identifiable source (4%), and development of a pancreatic pseudocyst after a laparoscopic cholecystectomy (2%).
When comparing these readmission diagnoses with NSQIP, an additional eleven diagnoses were identified. These are indicated in table 2 as "other", as they were found to be present in less than 2% of patients in both groups. These diagnoses included pancreatitis, thyrotoxicosis, marginal ulcer, UTI, adrenal insufficiency, cholecystitis, Clostridium difficile associated diarrhea, symptomatic anemia, and pneumonia. There was no statistical difference between these two groups (p = 0.84).
![]()
Table 2: Readmission diagnosis.
View Table 2
Patient and family involvement
During the intake survey, the patients answered the questions directly 72% of the time (Table 3); 22% of the time, questions were answered by a family member. In 6% of the cases, both the patient and a family member answered the questions. When asked who the primary caregiver was, 46% cared for themselves, 28% were cared for by their spouse, 20% were cared for by another family member, 4% were cared for by a facility, and 2% had no answer (Table 3).
![]()
Table 3: Patient and family involvement.
View Table 3
Follow up appointment
Only 82% of patients stated they had a follow up visit with their doctor. Of those who had a scheduled appointment, only 28% of the patients were able to attend. 66% were readmitted before their scheduled appointment and 6% were readmitted at their first clinic visit. Charts were subsequently reviewed to verify this, and there was 100% correlation with patient answers.
Timing of readmission
With the discovery that the majority of patients were being readmitted prior to their follow up appointment, further investigation regarding the time between discharge and readmission was performed. 56% of patients were readmitted within seven days of being discharged and 80% were readmitted within fourteen days (Figure 1a). This is similar to the NSQIP population, wherein 53% were readmitted within seven days of discharge and 78% within 14 days (Figure 1a). On further evaluation of the patients' charts, the average number of days between the day of discharge and the day of the scheduled appointment was eleven. The distribution of the scheduled follow up appointments is delineated in figure 1b.
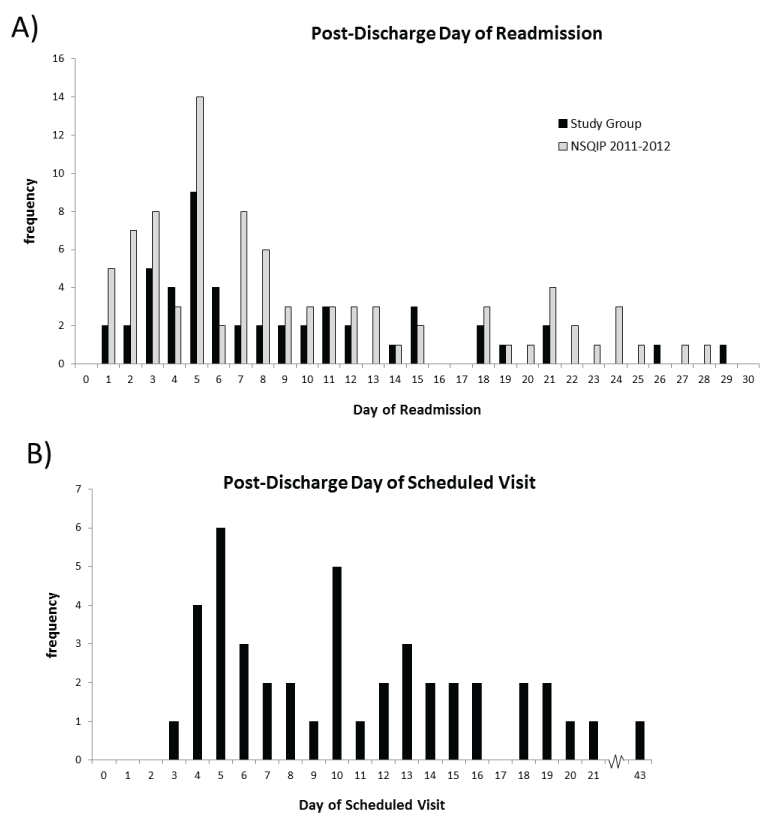
.
Figure 1: a) Frequency data indicating day of readmission relative to patient discharge dates. Black bars indicate the current study group and grey bars indicate patients identified by NSQIP between the years of 2011 and 2012. Of note, 56% of patients were readmitted within seven days of being discharged and 80% were readmitted within fourteen days in our study. This is similar to the NSQIP population, wherein 53% were readmitted within seven days and 78% within 14 days.
b) Frequency data indicating the timing between the discharge date and the timing to the initial postoperative visit in the current study.
View Figure 1
Patient suggestions for improving the discharge process
In response to the question regarding whether they had a clear understanding of their healthcare instructions when they left the hospital, 88% said they did, 10% said they didn't, and 2% did not answer. Of those who said no: one patient said they chose not to engage in the discharge instructions, one did not find the discharge instructions helpful, one did not understand the discharge instructions, one said no one explained the discharge instructions to them, one did not feel well enough to listen, and one was discharged to a long term acute care facility with no discharge instructions given to them directly.
Forty-nine percent of patients said they had no suggestions to improve discharge planning. Of the 51% who did have suggestions, six different themes were identified (Figure 2). About one-third of those who had suggestions stated that there was either wrong or not enough information on their discharge instructions. Another third indicated that there could be better communication within the team, including residents, nurses, faculty, and other staff involved in their care. As for the remaining third, 12% felt that the discharge process could be expedited, 12% thought they were discharged too soon, 8% indicated that the care team should ensure communication of the discharge instructions with family members, and 8% had responses that were unrelated to the discharge process. Specifically, one patient did not want to be required to have tube feeds anymore and one did not want to have difficulty sleeping anymore.
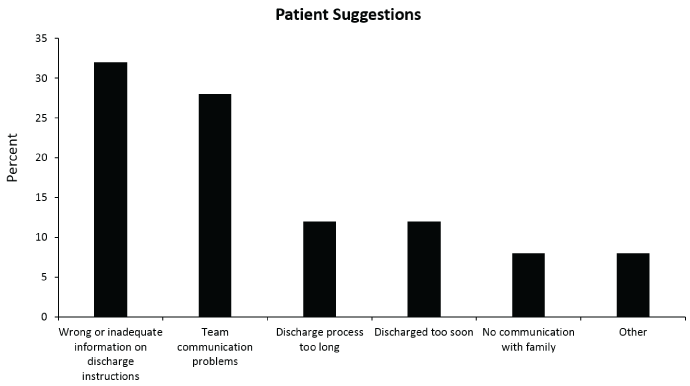
.
Figure 2: Categories of patient responses to the question, "What suggestions do you have to improve planning for your discharge from the hospital?" by percentage.
View Figure 2
Discussion
Overall, this study demonstrated that patients' opinions on the discharge process can be identified and can relay pertinent information that otherwise may not have been recognized. In particular, this study showed that the majority of our surgical patients are readmitted prior to their follow up appointment. In addition, patients' perspectives on the discharge process revealed a number of systems-level problems that may contribute to their readmission.
Various strategies to help reduce readmission rates have been developed in a number of states. One example is the STARR initiative (State Action on Avoidable Re-hospitalization), in which the entire state, rather than an individual institution, is responsible for the discharge disposition of the patient across all levels of need [9]. Project RED (or Re-Engineered Discharge), provides a step-by-step plan for practitioners to follow at discharge to ensure proper education of both the patient and all caregivers involved after discharge [10]. Project BOOST (or Better Outcomes by Optimizing Safe Transitions) has been implemented in at least six hospitals across Illinois in order to improve the transition from hospital to home [14]. Finally, the Madison VA has developed C-TraC (or Coordinated Transitional Care Program) which is a telephone-based initiative within the VA system which aims to improve post-discharge outcomes [15]. These tools have been shown to be very effective in reducing hospital readmissions, but clearly demonstrate that the effectiveness of a program involves in-depth understanding of the institution's patient population and causes for readmission [9,10,16,17]. Additionally, there are likely subsets of patients, such as the elderly, that require a more complex assessment of their needs at discharge to ensure proper transition from the acute inpatient setting to the next level of care [17,18].
With the initiation of the hospital consumer assessment of healthcare providers and systems (HCAHPS) survey, patient input into their own healthcare is becoming increasingly more influential [19-21]. A number of studies have shown that improving the discharge process overall can lead to significant decreases in health care costs and improve flows in hospital utilization [3,10,11,22]. In addition, other studies demonstrate that improving the discharge process significantly improves patient satisfaction and lowers risk-adjusted 30-day readmission rates [23,24].
From some of the objective questions used in the current study, simple solutions to avoid unnecessary readmissions were identified. For one, 18% did not have a follow up appointment scheduled. With the use of an electronic medical record, ensuring that patients have a follow up appointment scheduled should be an automatic part of the discharge order set. Of those who did have a postoperative visit scheduled, the mean was 11 days after discharge. This is quite striking, as 56% of patients were readmitted within 7 days of discharge and 80% within 14 days. We recently published a study showing that the two largest risk factors contributing to postoperative readmission are multiple complications and short length of stay [25]. Taken together, these studies suggest that earlier follow up or a delay in discharge may be indicated for high risk patients.
For both the current study population, as well as the patients identified by NSQIP, the patients at the highest risk for readmission were those who underwent a colorectal or hepatobiliary procedure (data not shown). However, these are also one of the more frequently performed operations within the general surgery department. In a concurrent study at our institution, we have identified factors which predict readmission 30 days from discharge in general surgery patients based on NSQIP data (accepted for publication). These include pre-operative steroid use, bleeding disorders, increased operative time, prolonged length of stay, and in-hospital complications. From this, a validated nomogram was created which can identify patients at high risk for readmission. Others have also shown that overall complication rates and pre-operative comorbidities are strong predictors of surgical readmissions [4-6,25-29]. With the ability to predict those who are at high risk for readmission, the timing of follow up appointments can be individually tailored in a more effective manner.
Perhaps the most powerful information comes from the subjective question. Of those who had a suggestion, about one third of the study population admitted that their discharge instructions were wrong or did not have enough information. To remedy this, more detailed discharge order sets that are specific to each subspecialty have been constructed. In addition, discharge instructions are being audio recorded so that patients or family members can listen after discharge.
Not unexpectedly, another third of patients noted team communication problems. One way we have attempted to combat this problem is by utilizing a multidisciplinary rounding technique. In this model, all teams involved in patient care - including nursing, nutrition, pharmacy, physical and occupational therapy, and social work - participate in daily rounds. This creates a system of checks and balances to ensure that all aspects of the patient's needs are accounted for and aims to ensure that a long term plan is in place prior to discharge.
One other major suggestion made by patients is directly related to the discharge process itself. Many thought the process was too long and others felt that there was not enough communication with the family members. As a result, a discharge collaborative project at our institution has been created in which providers are required to communicate an anticipated discharge date with the patient each day, as well as a confirmed date and time, once known. While the data are still being collected on this project, it has become evident that the discharge process has become much more organized and efficient within various hospital units, which is in accordance with studies published elsewhere [4,10,21,22]. In addition, we are attempting to reorganize our surgical clinics to be able to accommodate patients who have issues postoperatively that can be managed in the clinic setting. This will hopefully result in decreasing the burden to the emergency department and eliminating any unnecessary hospital readmissions.
The main limitation to this study is the small sample size. As this was a pilot study, the aim was mainly to gather specific information from the patients so that more robust data could be collected in future studies. Currently, these data are being utilized to configure larger-scale projects in which more detailed patient interviews are being performed. Another limitation is that the data collected was from a single institution. However, as iterated above, many of the universal tools to reduce readmissions do not take into account the needs of the individual characteristics of its patient population. As such, limiting the study to our institution-or, at most, hospitals in the surrounding community-is more valuable for analysis and creates an opportunity for more individualized care. Another limitation is that we assessed patients who were readmitted within thirty days of discharge, rather than thirty days of surgery, which is the parameter used for NSQIP. Despite this, there was no difference in patient age or gender between the NSQIP readmitted patients and those in our study, which was likely due to the fact that the majority of patients were readmitted before 14 days and these patients were captured in NSQIP. However, in the study group, more patients had a lower ASA class compared with both the readmitted and the combined NSQIP patient population, indicating that the study population was less moribund. Finally, approximately 22% of the time, questions were answered by a family member. As other studies have shown, patient satisfaction responses are very different if the patient versus family member answers the questions [30].
In summary, the use of patient perspectives to help identify improvements in the discharge process may help characterize the individual needs of patients as they transition out of the acute inpatient setting. With this information, institutional changes can be made to improve the transitions of care, with the ultimate goal of reducing readmission rates. Future studies will require cost analysis to determine whether changes made at our institution correlate with a reduction in health care spending and hospital utilization.
Acknowledgements
We would like to acknowledge Glen Leverson, PhD for providing statistical advice for this study. Dr. Sharon Weber had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
References
-
United States. Congress. House. Committee on Ways and Means. Subcommittee on Health (2008) Medicare Payment Advisory Commission's annual March report: hearing before the Subcommittee on Health of the Committee on Ways and Means, U.S. House of Representatives, One Hundred Tenth Congress, first session, March 1, 2007. Washington: U.S. G.P.O: For sale by the Supt. of Docs., U.S. G.P.O.
-
Jencks SF, Williams MV, Coleman EA (2009) Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med 360: 1418-1428.
-
Benbassat J, Taragin M (2000) Hospital readmissions as a measure of quality of health care: advantages and limitations. Arch Intern Med 160: 1074-1081.
-
Feigenbaum P, Neuwirth E, Trowbridge L, Teplitsky S, Barnes CA, et al. (2012) Factors contributing to all-cause 30-day readmissions: a structured case series across 18 hospitals. Med Care 50: 599-605.
-
Kansagara D, Englander H, Salanitro A, Kagen D, Theobald C, et al. (2011) Risk prediction models for hospital readmission: a systematic review. JAMA 306: 1688-1698.
-
Lucas DJ, Haider A, Haut E, Dodson R, Wolfgang CL, et al. (2013) Assessing readmission after general, vascular, and thoracic surgery using ACS-NSQIP. Ann Surg 258: 430-439.
-
Hyder O, Dodson RM, Nathan H, Schneider EB, Weiss MJ, et al. (2013) Influence of patient, physician, and hospital factors on 30-day readmission following pancreatoduodenectomy in the United States. JAMA Surg 148: 1095-1102.
-
Weber SM, Greenberg CC (2014) Medicare Hospital Readmission Reduction Program: what is the effect on surgery? Surgery 156: 1066-1068.
-
Boutwell AE, Johnson MB, Rutherford P, Watson SR, Vecchioni N, et al. (2011) An early look at a four-state initiative to reduce avoidable hospital readmissions. Health Aff (Millwood) 30: 1272-1280.
-
Jack BW, Chetty VK, Anthony D, Greenwald JL, Sanchez GM, et al. (2009) A reengineered hospital discharge program to decrease rehospitalization: a randomized trial. Ann Intern Med 150: 178-187.
-
Landman JH (2013) A statewide partnership for reducing readmissions. Healthc Financ Manage 67: 79-86.
-
Savin-Baden M, Major CH (2012) Qualitative research: the essential guide to theory and practice. Milton Park, Abingdon, Oxon; New York: Routledge.
-
Tevis SE, Kohlnhofer BM, Weber SM, Kennedy GD (2014) Postdischarge complications are an important predictor of postoperative readmissions. Am J Surg 208: 505-510.
-
Williams MV, Li J, Hansen LO, Forth V, Budnitz T, et al. (2014) Project BOOST implementation: lessons learned. South Med J 107: 455-465.
-
Gilmore-Bykovskyi A, Jensen L, Kind AJ (2014) Development and Implementation of the Coordinated-Transitional Care (C-TraC) Program. Fed Pract 31: 30-34.
-
Meyers AG, Salanitro A, Wallston KA, Cawthon C, Vasilevskis EE, et al. (2014) Determinants of health after hospital discharge: rationale and design of the Vanderbilt Inpatient Cohort Study (VICS). BMC Health Serv Res 14: 10.
-
Kind AJ, Jensen L, Barczi S, Bridges A, Kordahl R, et al. (2012) Low-cost transitional care with nurse managers making mostly phone contact with patients cut rehospitalization at a VA hospital. Health Aff (Millwood) 31: 2659-2668.
-
Altfeld SJ, Shier GE, Rooney M, Johnson TJ, Golden RL, et al. (2013) Effects of an enhanced discharge planning intervention for hospitalized older adults: a randomized trial. Gerontologist 53: 430-440.
-
Giordano LA, Elliott MN, Goldstein E, Lehrman WG, Spencer PA (2010) Development, implementation, and public reporting of the HCAHPS survey. Med Care Res Rev 67: 27-37.
-
Sheetz KH, Waits SA, Girotti ME, Campbell DA Jr, Englesbe MJ (2014) Patients' perspectives of care and surgical outcomes in Michigan: an analysis using the CAHPS hospital survey. Ann Surg 260: 5-9.
-
Mohammed K, Nolan MB, Rajjo T, Shah ND, Prokop LJ, et al. (2014) Creating a Patient-Centered Health Care Delivery System: A Systematic Review of Health Care Quality From the Patient Perspective. Am J Med Qual.
-
Naylor MD, Brooten D, Campbell R, Jacobsen BS, Mezey MD, et al. (1999) Comprehensive discharge planning and home follow-up of hospitalized elders: a randomized clinical trial. JAMA 281: 613-620.
-
Strong S, Bettin A (2015) An initiative to improve patient discharge satisfaction. Rehabil Nurs 40: 52-59.
-
Boulding W, Glickman SW, Manary MP, Schulman KA, Staelin R (2011) Relationship between patient satisfaction with inpatient care and hospital readmission within 30 days. Am J Manag Care 17: 41-48.
-
Kohlnhofer BM, Tevis SE, Weber SM, Kennedy GD (2014) Multiple complications and short length of stay are associated with postoperative readmissions. Am J Surg 207: 449-456.
-
Gibson A, Tevis S, Kennedy G (2014) Readmission after delayed diagnosis of surgical site infection: a focus on prevention using the American College of Surgeons National Surgical Quality Improvement Program. Am J Surg 207: 832-839.
-
Kelly KN, Iannuzzi JC, Rickles AS, Monson JR, Fleming FJ (2014) Risk factors associated with 30-day postoperative readmissions in major gastrointestinal resections. J Gastrointest Surg 18: 35-43.
-
Muthuvel G, Tevis SE, Liepert AE, Agarwal SK, Kennedy GD (2014) A composite index for predicting readmission following emergency general surgery. J Trauma Acute Care Surg 76: 1467-1472.
-
Tevis SE, Kennedy GD (2013) Postoperative complications and implications on patient-centered outcomes. J Surg Res 181: 106-113.
-
Elliott MN, Zaslavsky AM, Goldstein E, Lehrman W, Hambarsoomians K, et al. (2009) Effects of survey mode, patient mix, and nonresponse on CAHPS hospital survey scores. Health Serv Res 44: 501-518.





