International Journal of Surgery Research and Practice
Time Required between Two Positioning Methods for Shoulder Arthroscopy. A Non-Randomized Controlled Study
Xavier Zwiebel1, Anne-Marie Bédard2, Alexandre Leclerc2 and Mélissa Laflamme2*
1Medical Student, Université Laval, Centre Hospitalier de l'Université Laval (CHUL), Canada
2Clinical professor, Department of Orthopaedic Surgery, CHU de Québec - Centre Hospitalier de l'Université Laval (CHUL), Canada
*Corresponding author: Melissa Laflamme, MD, FRCSC, MSc, Orthopaedic Surgeon, Clinical Professor, Université Laval CHU de Québec, Pavillon CHUL, 2705 Boul, Laurier Bureau D-1211, Québec (QC) G1V 4G2, Canada, Tel : 418-522-4444, Fax : 418-654-2288, E-mail: melissa.laflamme.2@ulaval.ca
Int J Surg Res Pract, IJSRP-2-027, (Volume 2, Issue 2), Research Article; ISSN: 2378-3397
Received: January 15, 2015 | Accepted: August 25, 2015 | Published: August 27, 2015
Citation: Zwiebel X, Bédard AM, Leclerc A, Laflamme M (2015) Time Required between Two Positioning Methods for Shoulder Arthroscopy. A Non-Randomized Controlled Study. Int J Surg Res Pract 2:027. 10.23937/2378-3397/1410027
Copyright: © 2015 Zwiebel X, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: The objective of this non-randomized controlled study of 40 patients was to compare the positioning time required between the beach chair (20 patients) and the lateral decubitus position (20 patients) for a shoulder arthroscopy.
Methods: A single evaluator measured the speed of setup and the time was divided in four periods. All surgeries were performed at a single hospital by two fellowship-trained upper extremity orthopaedic surgeons using the SPIDER Limb positioner (Smith Nephew, Memphis, TN, USA) and under regional and general anaesthesia. The anaesthesia period was performed with the patient's supine before the positioning.
Results: The time required from positioning to the first incision is faster in lateral decubitus than in beach chair position (18:28 min vs 22:44 min, p < 0.0001). The setup time by the beneficiary attendant (10:13 min vs 14:12 min, p < 0.0001) and the time to set up the operative fields (7:42 min vs 8:39 min, p = 0.006) also indicate the same tendency. The duration of the anaesthetic period, excluding the time required for the regional block, is also faster in the lateral decubitus position (13:40 min vs 17:09 min, p = 0.17). Moreover, the correlation between weight and time positioning is inversely proportional in lateral decubitus position and proportional in beach chair position.
Conclusion: Because time difference between both positions is only a few minutes, surgeons should choose the position they are most comfortable with, according to their preferences and experience.
Keywords
Positioning, Shoulder arthroscopy
Introduction
Shoulder arthroscopy can be performed with the patient either in the lateral decubitus or the beach chair position [1,2]. Since the advent of the beach chair position, orthopaedic surgeons have been debating which of those two positions is superior [1]. Each one has its own advantages and disadvantages, whether for the ease of setup, the risks and complications, the intraoperative visualization or the joint accessibility. The current literature does not show one position to be superior over the other [3-8]. Most orthopaedic surgeons use the same position, regardless of the pathology, depending on their preference and expertise. No previous study objectively demonstrates a difference in time required for patient positioning in lateral decubitus and beach chair position. The purpose of this study was to compare the time required to achieve both positioning. Considering the issue of time constraints in the operating room, theater efficiency needs to be optimized whenever possible. In this study, we hypothesized that the lateral decubitus position would require less time to set up. Our secondary hypothesis was that the higher the patient's BMI was, the slower the positioning would be in both positions. Ethics was not required in this study.
Methods
Study design
All 40 patients had a shoulder arthroscopy at CHU de Québec, Pavillon CHUL in Quebec City by one of two fellowship-trained upper extremity orthopaedic surgeons. They were men and women over 18 years old with any type of shoulder pathology requiring a shoulder arthroscopy. No examination under anaesthetic was performed. The main exclusion criterion was the use of a position other than lateral decubitus position or beach chair position. The evaluator randomly selected 40 shoulder arthroscopy cases over a period of seven months (20 in the beach chair position and 20 in the lateral decubitus position). Surgeon #1 performed all the beach chair position cases, and surgeon #2 performed all of the lateral decubitus position cases according to their preferences and training. Both used the SPIDER® Limb positioner (Smith Nephew, Memphis, TN, USA), a pneumatically powered arm traction device during surgery. This system allows an easier intraoperative positioning and support of the patient's limb. Controlled by a foot pedal, the pneumatically powered arm maintains traction through out the procedure. Surgeries were all performed under general and regional anaesthesia (interscalene block anaesthesia) performed by one of the 14 experienced anaesthesiologists working in this hospital. The use of an arterial cannula and cerebral oxymetry was not standardized for all cases. Cerebral monitoring (INVOS) is known as a standard of care during cardiac surgery in our center. At the beginning of the study, cerebral oxymetry was not used for shoulder arthroscopy cases. It has been introduced during the study period for shoulder arthroscopy in the beach chair position only. Arterial cannula was use at the discretion of the anaesthesiologists in charge depending onpatient's comorbidities (age, history of stroke, BMI, coronary heart disease, etc.).
Both surgeons were aware of the study but the nurses, beneficiary attendants and anaesthesiologists were not. Two nurse's teams of three were part of the operating room staff in both positioning. Both teams were well experienced in shoulder arthroscopy.
The role of a beneficiary attendant in our health system is to take care of the patient once the general anesthesia is completed. His job is to securely and optimaly position the patient on the operating table with or without the intervention of the resident and/or the surgeon. He is not involved during the draping and the surgery itself. Three different beneficiary attendants took part in the setup of all cases, all being experienced in both positioning methods. Approximately 200 shoulder arthroscopy cases are performed each year in our center by the two upper extremity surgeons involved in this study.
Positioning
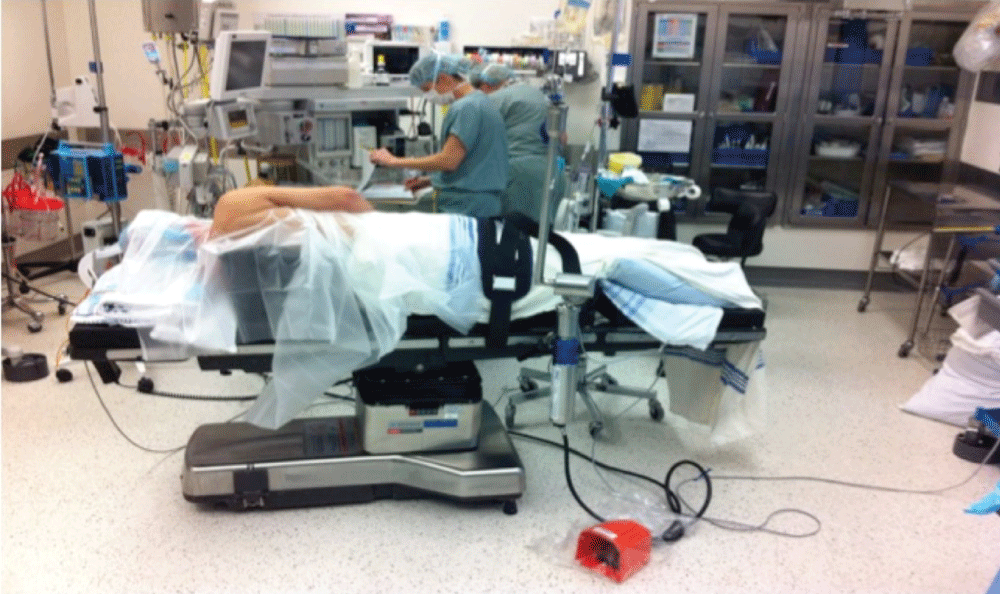
Lateral decubitus position: The patient is placed laterally on a standard operating table, with the operative shoulder exposed vertically (Figure 1). A bean bag and a strap are used to support the patient. The head is maintained in neutral position with pillows or a foam pad and the eyes and upside ear are protected by plastic drapes. Pressure points are padded on both legs and an axillary roll is used to protect the axillary neurovascular structures [1,2]. The non-operative arm is placed on an arm board, with 90° of forward flexion. The operative limb is placed into a foam traction sleeve connected to the SPIDER® Limb positioner (Smith Nephew, Memphis, TN, USA). The device allows application of a traction force on the limb to distend the gleno-humeral space and allows modifications to the amount of abduction (40-45°) and forward flexion (10-20°) [2,4,5].
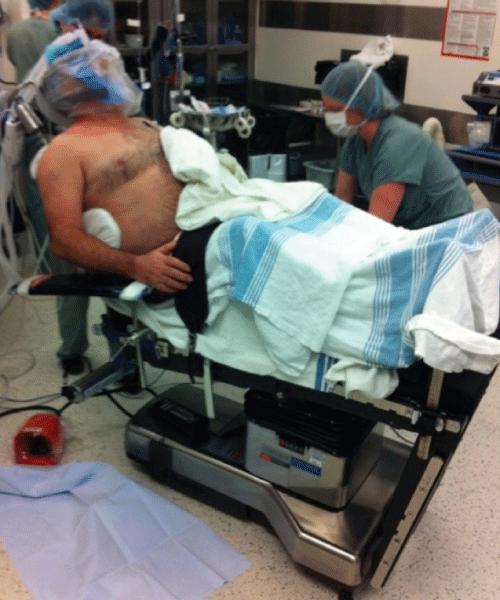
Beach chair position: The patient is placed in the supine position on the operative tablewith the T-Max Shoulder Positioner attached. The upper body leans on a pneumatic device attached to the operative table (Figure 2). The head, neck and torso are supported in neutral position by special straps and attachments. The patient is placed into 10-15° of Tredelenberg, with the hips flexed to 45-60° and knees flexed to 30° with a knee bolster [1,2]. Under the feet, an extra padded device (not part of T-Max system) is attached to the table to prevent the patient from sliding down during the intervention. Pressure points are padded and the eyes and the head's operative arm side are protected by plastic drapes. The non-operative arm is placed on an arm board. The operative arm is placed into the same foam traction sleeve than the other position and supported by the SPIDER® Limb positioner (Smith Nephew, Memphis, TN, USA).
Draping
This was similar to both positioning. Once the operative limb was scrubbed, the surgeon and the resident draped the limb using standard sterile techniques to allow for adequate arthroscopic portals placement.
Intervention
For every surgery, the same evaluator was in the operating room during the shoulder arthroscopy to measure the time required for the entire setup according to four different periods: the anaesthetic period (P0), the installation period (P1), the modification period (P2) and the draping period (P3). As soon as the patient entered the operating room, the evaluator triggered the timer. The anaesthetic period starts at this very moment until the beneficiary attendant gets close to the patient in order to start the positioning. At this time, the installation period starts and stops when the beneficiary attendant finishes the setup. The modification period is next. It begins by the time the orthopaedic surgeon modifies the position until he stops the modifications. Finally, the draping period occurs when the nurse gives the first drapes to the surgeon and stops when the first incision is made. An important thing to note is that the interscalene block was performed in or outside the OR depending on the cases order of the day. As a rule in this hospital, if the shoulder arthroscopy is the first case of the day, the interscalene block is performed in the OR right before the general anesthesia. If it is later (the second or third case of the day), the interscalene block is performed in the induction room (outside the OR) to save time between cases.
Demographic data about the patient's age, weight, height, body mass index (BMI) and sex were obtained form patient's medical records. The presence or absence of the surgeon and resident and the number of beneficiary attendants during the installation period were recorded. The operated side was also noted. Data regarding the use of an arterial cannula and/or a cerebral oxymetry as well as where the interscalene block was performed (induction room or operative room) were also extracted from patient's medical records after the surgery.
Statistical analysis
Statistical analysis was performed using Excel 2013 Software (Microsoft). Student-T's tests were performed on the time results separated in periods. Significance level was set to p < 0.05. Regression correlation analysis was then calculated to look for a relation between the time required for positioning and patient's weight and height. No power calculation was performed.
Results
Demographic characteristics of both groups are presented in table 1. Overall, the total time (time ± SD) to achieve the lateral decubitus position for a shoulder arthroscopy (installation period, modification period and draping period; (P1 + P2 + P3)) was 4:15 minutes faster than the beach chair position (18:28 ± 2:20min vs 22:43 ± 2:39min, p < 0.0001). In addition, when only the installation period by the beneficiary attendant was considered with the modification period by the surgeon (P1 + P2), the time was 3:37 minutes faster in this position (10:46 ± 2:01min vs 14:23 ± 2:46min, p < 0.0001). Furthermore, the draping (P3) was 0:47 minute faster with the patient in lateral decubitus position (7:42 ± 0:49min vs 8:39 ± 0:52min, p = 0.006). These results were all statistically significant. Table 2 summarizes the comparison of the different periods between groups.
![]()
Table 1: Baseline characteristics of the 40 patients
View Table 1
![]()
Table 2: Time required for each period between groups
View Table 2
The modification period (P2) alone was shorter (0:22 ± 0:02min vs 1:51 ± 0:42min) and less frequent (15% vs 30% of the time) in the beach chair position. For all 20 cases in the beach chair group, surgeon #1 was present during the installation period. In the lateral decubitus cohort, surgeon #2 was absent 8 out of 20 times. We explain this difference mainly by the complexity of the head positioning in the beach chair position, as the beneficiary attendant needed more supervision compared to the lateral decubitus position. Surgeon's personality may also have a role. However, surgeon's intervention during the installation period of the lateral decubitus did not accelerate the whole set up time. In fact, the time was slower by 0:58 minute (18:51 ± 2:53min vs 17:53 ± 1:01min, p = 0.38). In some cases, a second beneficiary attendant helped with the positioning. His presence did not accelerate the procedure in the beach chair cohort (15:13 ± 3:12min vs 13:38 ± 2:03min) (Table 3). On the contrary, in the lateral decubitus group, the installation period was faster with the intervention of a second beneficiary attendant (6:44 ± 1:23min vs 9:00 ± 2:16min). Table 4 reveals that the patient's BMI were higher (30.9 vs 25.9 p = 0.002) and patients were heavier (94.1kg vs 78.1kg p = 0.002) in both cohorts when two beneficiary attendants proceeded to the set up.
![]()
Table 3: Time required for P1 when 1 versus 2 beneficiary attendants were present
View Table 3
![]()
Table 4: Morphologic data of patient's when1 versus 2 beneficiary attendants were present
View Table 4
As shown in table 5, the duration of the anaesthetic period (P0) was significantly shorter when the interscalene block was performed in the induction room instead of the operating room when we combined both groups (25:48 ± 5:19min vs 15:28 ± 6:45 min, p < 0.0001). When using only patients who had their interscalene block performed in the induction room, therefore excluding the time required for the regional anaesthesia, the anaesthetic period was shorter in the lateral decubitus position by 3:29 minutes (13:40 ± 5:41min vs 17:09 ± 7:24min). In the beach chair position, the anaesthetic period was longer when either an arterial cannula or a cerebral oxymetry was apply (Table 6). No patients in the lateral decubitus position had one of those device applied.
![]()
Table 5: Time for anaesthetic period (P0) depending on the location of the regional block
View Table 5
![]()
Table 6: Time required to apply monitoring devices in the beach chair cohort (N=19)
View Table 6
The patient's morphology influenced the time required for positioning. In the beach chair cohort, the time positioning variation according to the weight (r = 0.58) and BMI (r = 0.56) was proportional. On the other hand, it was inversely proportional as a function of patient's weight (r = -0.55) and BMI (r = -0.41) in the other cohort.
Discussion
This non-randomized controlled study demonstrates a significantly faster set up in the lateral decubitus position. We explain this difference mainly by the ease and the simplicity of the setup to move from the supine to the lateral position. In the beach chair position, moving from the supine to the sitting position demands more rigour and time to place the head, the neck and the torso correctly to minimize complications such as cerebral hypoperfusion [1,8-10] . However, these results are not clinically significant and the use of the lateral decubitus position does not improve the overall efficiency of an operative day.
Surgeon #1 using the beach chair position supervised the installation for all 20 cases. This can be explained by the complexity of the head and neck positioning. In the lateral decubitus position, surgeon #2 was absent during the installation period in almost half of the cases. The absence of supervision during installation increased the frequency of surgeon's modification interventions and the duration of those interventions. However, even if the surgeon was always there to supervise and oversee, as seen with the beach chair position proponent, the setup was not faster. Indeed, the presence of the surgeon during the set up did not accelerate the whole setup and even seemed to slow it down, although our results were not significant.
Moreover, the use of two beneficiary attendants instead of one did not seem to accelerate the set up (P1) except for the lateral decubitus group. A second beneficiary attendant helped with the procedure mostly when the patients were heavier and their BMI was significantly higher. Therefore, those morphologic parameters act as major confounding factors on time positioning and specifically on the importance of a second beneficiary attendant contribution.
As shown in the regression correlation analysis, patient's morphology influences the setup speed. In the lateral decubitus position, the setup speed varied inversely with patient's BMI and weight. In the other group, the setup speed varied directly with all the same morphologic parameters. Thus, a heavy patient was more difficult to manage in beach chair position. To prevent exaggerated dorsolombar flexion or the patient from sliding, it is necessary to place patient's hips at the exact flexion location on the operative table. This technical aspect made it more laborious to sit heavier and taller patients properly. Moreover, it was more difficult to stabilize the head and the neck on the support device. Height impaired the lower limb positioning and pressure points padding. In the lateral decubitus position, the bigger the patient was, the faster was the set up. Our explanation for this is that it was harder to position a thin patient on his side because of the absence of a belly. A larger belly offers some stability once the patient is on his side until the beanbag is deflated.
We considered the anaesthetic period independently from the positioning period because this period was dependent of several variables, such as the working speed of the anaesthesiologist, his blood pressure monitoring technique with or without arterial cannula and the use of cerebral monitoring. It is likely that the P0 period could be influenced by those variables that could not be controlled. The order of the operative cases also played a role. As a general rule in our center, if the shoulder arthroscopy was the first case of the day, the interscalene regional block was done right before the general anaesthesia in the operative room (OR). If it was later, the regional anaesthesia was performed in the induction room before entering the operative room, thus saving some OR time. Our results show that this can save as much as 10 minutes. The fact that the anaesthetic period, excluding the regional anaesthesia, was slower in the beach chair position can be explained by the insertion of an arterial cannula and / or the use of a cerebral oxymetry to better monitor patients for cerebral hypoperfusion. Those devices were not required in the lateral decubitus position where patients are not at risk for this unique complication [1,8,9].
The primary strength of this study is the fact that nurses, beneficiary attendants and anaesthesiologists were not aware of the study; therefore they did not change their usual procedures. Only one evaluator collected all the data to minimize the information bias. Moreover, the study has a good external validity as all the positions were achieved as described in the literature, by standard beneficiary attendants and upper extremity orthopaedic surgeons. We also acknowledge some limitations. Only one surgeon was assigned to each position. Therefore, surgeon's personality could have influenced the results. Furthermore, weight, height and BMI acted as confounding factors on the contribution of a second beneficiary attendant. Finally, the high number of different anaesthesiologists was certainly a factor affecting the P0 period.
Conclusion
The positioning for shoulder arthroscopy can be challenging. Even if the lateral decubitus position is statistically faster to set up, the time difference is not enough to be clinically significant. It does not allow the surgeon to perform an additional operative case in an operative day. There is still no objective evidence to support one position over the other. The orthopaedic surgeons should choose the position based on their experience, comfort and preferences. Further studies should focus on the impact patient's morphology on time required for positioning.
References
-
Peruto CM, Ciccotti MG, Cohen SB (2009) Shoulder arthroscopy positioning: lateral decubitus versus beach chair. Arthroscopy 25: 891-896.
-
Paxton ES, Backus J, Keener J, Brophy RH (2013) Shoulder arthroscopy: basic principles of positioning, anesthesia, and portal anatomy. J Am Acad Orthop Surg 21: 332-342.
-
Gross RM, Fitzgibbons TC (1985) Shoulder arthroscopy: a modified approach. Arthroscopy 1: 156-159.
-
Phillips BB (2008) Arthroscopy of the upper extremity. In: Canale ST, Beaty JH Campbell's operative orthopaedics. Philadelphia: CV Mosby Elsevier 2923-2926.
-
Skyhar MJ, Altchek DW, Warren RF, Wickiewicz TL, O'Brien SJ (1988) Shoulder arthroscopy with the patient in the beach-chair position. Arthroscopy 4: 256-259.
-
Terry MA, Altchek DW (2003) Diagnostic shoulder arthroscopy technique: Beach chair position. In: Tibone JE, Savoie FH 3rd, Shaffer BS Shoulder arthroscopy. New York: Springer-Verlag 9-15.
-
Tibone JE (2003) Diagnostic shoulder arthroscopy in the lateral decubitus position. In: Tibone JE, Savoie FH 3rd, Shaffer BS Shoulder arthroscopy. New York: Springer-Verlag 3-8.
-
Warren RF, Morgan C (2008) Shoulder positioning: Beach chair vs. lateral decubitus: Point/counterpoint. Arthroscopy Association of North America Newsletter.
-
Murphy GS, Szokol JW, Marymont JH, Greenberg SB, Avram MJ, et al. (2010) Cerebral oxygen desaturation events assessed by near-infrared spectroscopy during shoulder arthroscopy in the beach chair and lateral decubitus positions. Anesth Analg 111: 496-505.
-
Dippmann C, Winge S, Nielsen HB (2010) Severe cerebral desaturation during shoulder arthroscopy in the beach-chair position. Arthroscopy 26: S148-150.