International Journal of Surgery Research and Practice
Renal Transitional Cell Carcinoma: Case report from the Regional Hospital Buea, Cameroon and Review of Literature
Enow Orock GE1*, Eyongeta DE2 and Weledji PE3
1Pathology Unit, Regional Hospital Buea, Cameroon
2Urology Unit, Regional Hospital Limbe, Cameroon
3Surgical Unit, Regional Hospital Buea, Cameroon
*Corresponding author: Enow Orock George, Pathology Unit, Regional Hospital Buea, South West Region, Cameroon, Tel: (237) 77716045, E-mail: enowrock24@yahoo.com
Int J Surg Res Pract, IJSRP-1-007, (Volume 1, Issue 1), Case report; ISSN: 2378-3397
Received: September 01, 2014 | Accepted: September 26, 2014 | Published: September 29, 2014
Citation: Enow Orock G, Eyongeta DE, Weledji PE. (2014) Renal Transitional Cell Carcinoma: Case report from the Regional Hospital Buea, Cameroon and Review of Literature. Int J Surg Res Pract 1:007. 10.23937/2378-3397/1410007
Copyright: © 2014 Enow Orock G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Although transitional cell carcinoma is the most common tumour of the renal pelvis, we report the first histologically-confirmed case in our service in a period of about twenty years. The patient is a mid-aged female African, with no apparent risks for the disease. She presented with the classical sign of the disease (hematuria) and was treated by nephrouretectomy for a pT3N0MX grade II renal pelvic tumour. She is reporting well one year after surgery. The case highlights not only the peculiar diagnosis but also illustrates the diagnostic and management challenges posed by this and similar diseases in a low- resource setting like ours. It also underscores the importance of routine histological analysis of specimens, an investigation that is not so common in our practice.
Keywords
Renal, Transitional cell, Carcinoma
Introduction
There are various types of renal cancers, each derived from a different cell type within the kidney with peculiar morphology and clinical behavior. The major morphological classifications (WHO/AFIP, modified Mainz classification, and the Heidelberg classification) distinguish eight subtypes of renal cell tumors [1]. Classification is primarily based on cytologic appearance and the cell type of origin in combination with growth pattern and genetic alterations [2,3].
There is evidence that the frequency of upper urinary tract malignancies is increasing [4]. Renal transitional cell or renal urothelial carcinoma is a malignant tumor arising from the transitional (urothelial) epithelial cells lining the urinary tract from the renal calyces to the ureteral orifice. Transitional cell carcinoma in this location occurs in about 5% of all urothelial cancers and 7% of all primary renal carcinomas [5]. It is most commonly found in the bladder and ureters.
According to the American Cancer Society, an estimated 70,980 bladder cancers and 57,760 kidney cancers were diagnosed in the United States in 2009. Primary renal pelvis and ureteric malignancies, on the other hand, are much less common with an estimated 2,270 cases diagnosed and 790 deaths in 2009 [6]. Worldwide statistics vary with the highest incidence found in the Balkans where urothelial cancers account for 40% of all renal cancers and are bilateral in 10% of cases [7]. We report a first histologically-confirmed case of renal pelvic transitional cell carcinoma in 20 years of practice in a mid-aged African woman.
Case Report
AMC is a 50-year-old female primary school teacher, with a past history of one cesarean section for her only child 28 years earlier. Her husband had died 4 years ago from an unknown splenic tumor. She presented with intermittent, massive, gross hematuria of 2 years duration. The patient was a non smoker and denied pain, fever, neither vomiting nor any lower urinary tract symptoms. She had however been treated as recurrent urinary tract infection until a few months ago, when she was referred to our urology department after presenting with progressive fatigue associated to the above symptoms. Except for pallor and prostration, physical examination was unremarkable. CT urogram showed right hydronephrosis up to the upper third of the right ureter on a non functioning kidney (figure 1). Neither a stone nor any obstructive lesion could be identified on the CT scan (Figure 1).
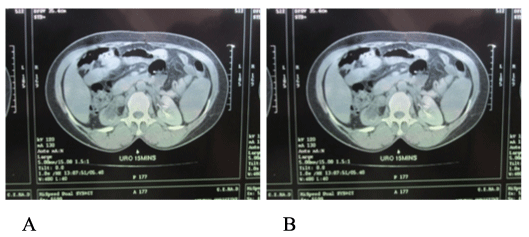
Figure 1A and 1B: CT scan revealed a right hydronephrosis.
View Figure 1
Kidney function tests showed hypercreatinemia (creatinine 13.46g/l �normal range is 6-12g/l, BUN 0.37g/l), and a complete blood count revealed a hypochromic microcytic anemia with a hemoglobin of 9.5g/dl. Urine culture was sterile. On cystoscopy, there was no bladder tumour except for active bleeding observed from the right ureteral orifice. Diagnostic ureterorenoscopy could not be performed. Urine cytology revealed fresh red blood cells with masses of atypical urothelial cells suggestive of urothelial carcinoma but the localization was inconclusive, neither could the tumour be graded. A right radical nephroureterectomy was performed via a two incisions (Figure 2). The specimen "en bloc" (Figure 3) was sent for pathological analysis. The patient is reporting well one year post-operation.
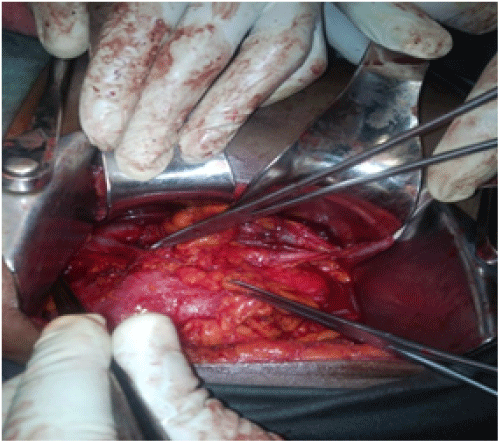
Figure 2: In situ dissection showing the inferior vena cava, right renal vein
(on right angle clamp), and ureter (on vessel loop) during nephrouretectomy
View Figure 2
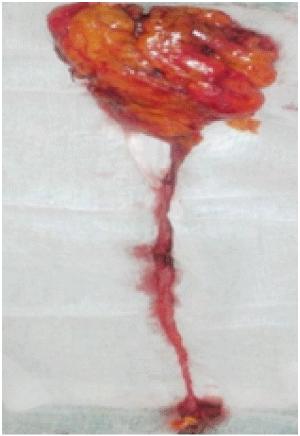
Figure 3: "En bloc" dissection showing Kidney (above), ureter and bladder
cuff (below).
View Figure 3
At macroscopy an 11x6x5cm right nephrouretectomy specimen was found attached to an 18cm long ureter with a 3cm diameter bladder cuff at the lower end (Figure 3). On section, multi cystic renal parenchyma was seen. There was a 6 cm unifocal grayish tumour occupying the inferior renal pelvis with extension into the proximal ureter to about 4cm. It was well encapsulated and firm with hemorrhagic and necrotic foci. No satellite nodes or perinephric fatty invasion was seen (Figure 4).
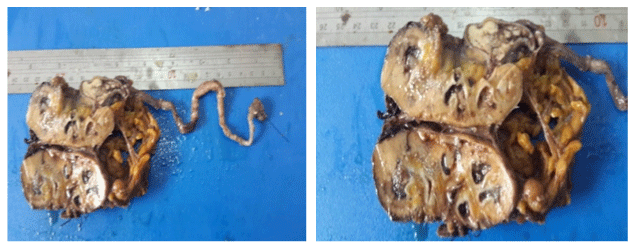
Figure 4A & 4B: Macroscopic section of kidney showing low and high
power view of tumour with ureteral extension in upper right corner of picture
View Figure 4
Histology of sections revealed non keratinized, well-differentiated, papillary proliferations made of fibrovascular core and lined by many layers of atypical transitional cells (Figure 5). Mitosis were few (about 4/HPF) and necrotic foci were observed. The surgical limits were free of tumour. A pathological diagnosis of a well-differentiated papillary transitional cell carcinoma of the renal pelvis with complete surgical excision was made. The tumour was graded II and staged as pT3NoMX.
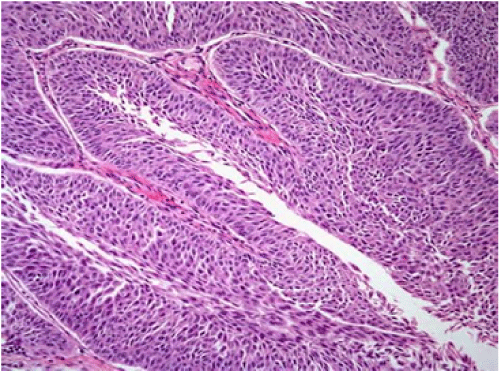
Figure 5: Photomicrograph showing a well-differentiated papillary
transitional cell carcinoma.
View Figure 5
Discussion
In an-8-year population study in Cameroon, Enow orock et al. [8] found kidney cancer to account for about 1% of the total cancer burden in the Yaounde population. In the same study, renal malignancies were found to be more predominant in the pediatric age group 0-14 years accounting for about 55% of cases. The histological predominant cancer types reported in this study were nephroblastoma and papillary carcinoma. No case of transitional cell carcinoma was found. In another report, the crude rate for renal cancer in the same population was found to be 0.69 and 0.35 for males and females respectively [9]. In these, renal malignancies were found to be more predominant in the male sex at 52.7% [9]. The patient we present is a 50 years old African female.
The exact cause of upper urinary tract transitional cell carcinoma is not known. However, several risk factors for the disease have been identified. These include amongst others; exposure to various chemicals, infections, drugs, genetics, diet and cigarette smoking [10,11]. This later appears to be the most significant acquired risk factor for upper urinary tract urothelial cancer where it accounts for 70% and 40% of the disease in men and women respectively. Dietary exposure to aristolochic acid has been identified as a significant risk factor for Balkan nephropathy and subsequent transitional cell carcinoma [7]. Analgesic abuse is a risk factor which has become rare [10,12].
Chronic bacterial infection with urinary calculus and obstruction may predispose to the development of urothelial cancer. In these cases, a squamous cell carcinoma is the most common entity. Schistosomiasis also may predispose to this. Some chemotherapy drugs are implicated in the development of urothelial cancers in the upper and lower urinary tract, particularly after drug-induced hemorrhagic cystitis. Analgesic abuse and chronic infections are more likely risk factors in our community, though this has never been studied. In the case of our patient, no risk factor was identified with her disease. She had however been presumptively treated for chronic urinary tract infection without any confirmatory investigations.
Tumours of the renal pelvis reportedly rarely occur before age 40 years, with peak incidence in the 60-70 years age group. Men are affected approximately 2 times as frequently as women [13]. The incidence is slightly higher in African Americans than in other races. Unlike these findings, our patient was female, and was within the reported predominant age group for the disease (50 years). The tumour may occur as a unique diagnosis, though association with other histological types has been reported [14]. The tumour in the case we presented was unassociated to another histological type.
This cancer is rarely reported as an incidental finding as symptoms are significant enough to suggest the diagnosis in a relatively short time after disease development. Only a small percentage (1-2%) of patients is asymptomatic. Gross hematuria is the most common presenting symptom, occurring in 75-95% of patients, while microscopic hematuria occurs in 3-11% of patients [15]. Gross hematuria was the main presenting symptom in our patient. Approximately 14-37% of patients report a dull pain attributed to the gradual obstruction of the collecting system. Renal colic also may occur with the passage of blood clots. Physical examination of patients is usually not informative or specific, especially in patients with early-stage disease. A palpable flank mass may be noted in fewer than 20% of patients. The classic clinical triad of hematuria, pain, and mass is also rare (15%) and is usually an indicator of advanced disease [15]. It was surprising that our case did not complain of pain in spite of the gross obstructive uropathy revealed on CT scan (Figure 1) and at macroscopy in figure 4.
Apart from transitional cell carcinoma which accounts for more than 90% of renal pelvic tumors; other cancer types seen include squamous cell carcinoma and adenocarcinoma. The predominant histologic pattern of urothelial carcinoma is a papillary tumor with stratified, nonkeratinizing epithelium supported on a thin fibrovascular core. This is similar to our finding as seen in figure 5 above. This tumour is histologically identical to urinary bladder cancer. The 2 malignancies share the same risk factors and can occur as a part of "field cancerization," which results from exposure of urothelium to carcinogens excreted by or activated in the urine. Hence, upper urinary tract urothelial tumors may be multifocal, and in 2-10% of cases, they are bilateral as well. In our case, no known risk factor was identified and the tumour was unifocal and unilateral [15,16]. There was extension into the ureter to about 4cm (Figure 4).
Tumour size relates to prognosis and range between extremes of 3-12cm diameter, and most is between [16]. Grossly these tumours are reported to be soft, grayish red masses with glistening surfaces that resemble the transitional cell tumours of the bladder microscopically and may extend down the ureter [17]. This was similar to our finding.
Patients with squamous cell carcinoma usually present with advanced disease and renal calculi are present in 14-50% of patients. Primary adenocarcinoma of the renal pelvis accounts for less than 1% of upper urinary tract urothelial tumors and is associated with chronic urolithiasis, hydronephrosis, and pyelonephritis. Patients are also at risk for the development of bladder tumours, which has an estimated incidence of 20-48%, occurring within a 5 year period. On the other hand, patients with primary bladder cancer develop upper urinary tract urothelial cancer in 2-4% of cases [18]. The frequency of upper urinary tract urothelial cancer may reach 21% in patients with bladder carcinoma in situ (CIS) and in those with certain occupational exposures [19].
Tumour stage is the most important prognostic factor for upper urinary tract urothelial cancer. Survival correlates closely with tumour stage. In our case it was staged as a pT3N0MX tumour. Tumour grade is another predictor of prognosis. Tumour grade usually follows tumour stage, and patients with high-grade carcinomas have more advanced disease stage. Stage and grade correlate in as many as 83% of cases, though stage remains a more accurate predictor of prognosis [20]. The tumour in our patient was histioloically well differentiated and graded as II (Figure 5). Stage T3 renal tumors have a better prognosis than ureteral tumours do. A retrospective study by Park et al [21] found that in patients with stage pT3 disease, 5-year cancer-specific survival rates were 77.5% for renal pelvic tumours invading the renal parenchyma versus 49.7% for tumours invading peripelvic or periureteral fat. The 5-year recurrence-free survival rates for the 2 tumour types were 75.6% and 32.0%, respectively [21]. The authors suggested that the thickness of the renal parenchyma may protect against local tumour spread [21].
Transitional cell carcinoma may develop in the contralateral kidney after radical nephroureterectomy. In a European multicenter dataset of patients who underwent nephroureterectomy for non metastatic transitional cell carcinoma, a history of bladder transitional cell carcinoma preceding the upper urinary tract tumour was the only predictor of recurrence in the contralateral upper tract [22]. Our patient had no history of previous tumour nor are there any signs of contralateral recurrence so far.
Urinalysis and urine culture are necessary preliminary investigations indicated for management of the disaese. The presence of microscopic hematuria suggests urinary tract tumors, which must be ruled out even if the hematuria resolves. The presence of more than 2-5 Red Blood Cells (RBCs) per High-Power Field (HPF) is considered sufficient to warrant further investigation to rule out upper urinary tract renal transitional cell carcinoma. It is also important to evaluate for urinary tract infections and cytologic studies may be helpful. Voided-urine cytology is a convenient and noninvasive method of diagnosis, but it is subjective and lacks the necessary sensitivity for diagnosing upper urinary tract urothelial tumours, especially low-grade neoplasms. Our cytology reported presence of malignant cells consistent with a transitional cell carcinoma. Unfortunately, the slides were discarded before micrographs of this cytology could be documented.
Fluoroscopically guided brush biopsy increases the diagnostic accuracy to 80-90%. A 2012 study concluded that urine cytology and Fluorescence In Situ Hybridization (FISH) are the single tests with best overall performance for the detection of urothelial carcinoma. Combining cytology and FISH improved the sensitivity; failure of cytology to detect grade 3 carcinoma in situ tumors decreased by 62.5% when FISH was performed in cytology-negative patients [23]. We were unable to perform these further investigations in our setting.
In the past, Intravenous Urography (IVU) was the most commonly used diagnostic method for the evaluation of patients with hematuria. In current practice, however, it is increasingly being replaced by Computed Tomography (CT) urography [24ram]. CT scanning is useful in the diagnosis and staging of renal urothelial tumours as it can distinguish between radiolucent renal stones and upper urinary tract urothelial tumours [24,25].
CT scanning also can be used for determining the local extent of the u and presence of distant metastases, but is of limited value in predicting the pathologic stage of upper urinary tract urothelial tumours with an accuracy of 43-77%. In our case the CT scan was unable to detect the tumour and was reported as normal (Figure 1). Cystoscopy may help to localize bleeding site (left or right) and rule out or confirm concomitant bladder lesions. This test was useful in our investigations as stated in case report above.
As concerns treatment, surgical intervention is the main form of radical treatment for localized disease which is uniformly fatal if untreated. Traditional radical surgery in this case consists of total nephroureterectomy with excision of a bladder cuff around the ureteral orifice [26,27]. This is the procedure that was offered to our patient. Otherwise, 30-75% of patients develop tumor recurrence in the ureteral stump or around the ipsilateral ureteral orifice. In a multicenter study of 1363 patients with upper urinary tract urothelial carcinoma who were treated with radical nephroureterectomy, the 5-year cancer-specific survival probability was approximately 73% [28]. Our patient is alive and well one year following surgery.
Patients with low-stage, low-grade tumours respond well to either radical or conservative surgical treatment. In a retrospective review of patients treated with renal-sparing ureteroscopic management, Pak et al. [29] reported that renal preservation approached 81%, with cancer-specific survival of 94.7%. There was significant cost savings over the cost of nephroureterectomy; these authors recommend conservative endoscopic management as the gold standard for low-grade and superficial-stage disease. However, preoperative cytology and ureterorenoscopically-performed biopsies have limited accuracy in predicting the correct tumor grade. Additional diagnostic procedures should be done prior to definitive surgical intervention [30]. We were unable in our setting to carry out more invasive pre operative investigations. Most transitional cell carcinomas are single or multiple and usually papillary and a nephroureterectomy is effective for localized disease [31,32] as our case illustrates.
Conclusion
Renal cancer is relatively rare and understudied in our community. A transitional cell carcinoma of the kidney is even rarer. We present this first case diagnosed in our service in about two decades. The case highlights the challenges faced by health providers in general and cancer care givers in particular in this low resource setting. It also underscores the necessity for routine histological analysis of surgical specimens (an uncommon practice in our setting) in order to document tumour morphology and possibly discover rare types that hitherto were thought not to occur in our environment. Further studies on the disease are recommended.
Author Contributions
Enow Orock GE: Examined the specimen, made the diagnosis and wrote part of article
Eyongeta DE: performed the surgery and wrote the case report
Weledji PE: Reviewed the article
References
-
Kovacs G, Akhtar M, Beckwith BJ, Bugert P, Cooper CS, et al. (1997) The Heidelberg classification of renal cell tumours. J Pathol 183: 131-133.
-
van den Berg E, Dijkhuizen T, Oosterhuis JW, Geurts van Kessel A, de Jong B, et al. (1997) Cytogenetic classification of renal cell cancer. Cancer Genet Cytogenet 95: 103-107.
-
Akaza H, Koiso K, Niijima T (1987) Clinical evaluation of urothelial tumors of the renal pelvis and ureter based on a new classification system. Cancer 59: 1369-1375.
-
Jemal A, Siegel R, Ward E, Hao Y, Xu J, et al. (2009) Cancer statistics, 2009. CA Cancer J Clin 59: 225-249.
-
Guinan P, Vogelzang NJ, Randazzo R, Sener S, Chmiel J, et al. (1992) Renal pelvic cancer: a review of 611 patients treated in Illinois 1975-1985. Cancer Incidence and End Results Committee. Urology 40: 393-399.
-
American Cancer Society (2009) Cancer Facts & Figures 2009.
-
Grollman AP, Shibutani S, Moriya M, Miller F, Wu L, et al. (2007) Aristolochic acid and the etiology of endemic (Balkan) nephropathy. Proc Natl Acad Sci U S A 104: 12129-12134.
-
Enow Orock GE, Eyongeta DE, Weledji EP (2013) Malignant tumours of the kidney in Yaounde, Cameroon. An 8 years population study and literature review. AJIH 1: 6-10.
-
Enow Orock GE (2012) Incidence per 100 000 by age group. In: Doh AS, Ndom P (edn) Cancer Incidence and Trends in Yaounde, Cameroon. Amsterdam: Lambert Academic Publishing: 62-67.
-
Colin P, Koenig P, Ouzzane A, Berthon N, Villers A, et al. (2009) Environmental factors involved in carcinogenesis of urothelial cell carcinomas of the upper urinary tract. BJU Int 104: 1436-1440.
-
McDougal WS, Cramer SF, Miller R (1981) Invasive carcinoma of the renal pelvis following cyclophosphamide therapy for nonmalignant disease. Cancer 48: 691-695.
-
Palvio DHB, Andersen JC, Falk E (1987) Transitional cell tumours of the renal pelvis and ureter associated with capillarosclerosis indicating analgesic abuse. Cancer 59: 972-976.
-
Balslev E, Fischer S (1983) Transitional cell carcinoma of the renal collecting tubules ("renal urothelioma"). Acta Pathol Microbiol Immunol Scand A 91: 419-424.
-
Yokoyama I, Berman E, Rickert RR, Bastidas J (1981) Simultaneous occurrence of renal cell adenocarcinoma and urothelial carcinoma of the renal pelvis in the same kidney diagnosed by preoperative angiography. Cancer 48: 2762-2766.
-
Johansson S, Angervall L, Bengtsson U, Wahlqvist L (1976) A clinicopathologic and prognostic study of epithelial tumors of the renal pelvis. Cancer 37: 1376-1383.
-
Guillou L, Duvoisin B, Chobaz C, Chapuis G, Costa J (1993) Combined small-cell and transition,al cell carcinoma of the renal pelvis. A light microscopic, immunohistochemical, and ultrastructural study of a case with literature review. Arch Pathol Lab Med 117: 239-243.
-
Wegner HE, Bornh�ft G, Dieckmann KP (1993) Renal cell cancer and concomitant transitional cell cancer of the renal pelvis and ureter in the same kidney--report of 4 cases and review of the literature. Urol Int 51: 158-163.
-
Kroft SH, Oyasu R (1994) Urinary bladder cancer: mechanisms of development and progression. Lab Invest 71: 158-174.
-
Vineis P, Magnani C (1985) Occupation and bladder cancer in males: a case-control study. Int J Cancer 35: 599-606.
-
Raabe NK, Foss� SD, Bjerkehagen B (1992) Carcinoma of the renal pelvis. Experience of 80 cases. Scand J Urol Nephrol 26: 357-361.
-
Park J, Ha SH, Min GE, Song C, Hong B, et al. (2009) The protective role of renal parenchyma as a barrier to local tumor spread of upper tract transitional cell carcinoma and its impact on patient survival. J Urol 182: 894-899.
-
Novara G, De Marco V, Dalpiaz O, Galfano A, Bouygues V, et al. (2009) Independent predictors of contralateral metachronous upper urinary tract transitional cell carcinoma after nephroureterectomy: multi-institutional dataset from three European centers. Int J Urol 16: 187-191.
-
Todenh�fer T, Hennenlotter J, Esser M, Mohrhardt S, Tews V, et al. (2013) Combined application of cytology and molecular urine markers to improve the detection of urothelial carcinoma. Cancer Cytopathol 121: 252-260.
-
Vikram R, Sandler CM, Ng CS (2009) Imaging and staging of transitional cell carcinoma: part 2, upper urinary tract. AJR Am J Roentgenol 192: 1488-1493.
-
Jeong YB, Kim HJ (2012) Is it transitional cell carcinoma or renal cell carcinoma on computed tomography image? Urology 79: e42-43.
-
Auld CD, Grigor KM, Fowler JW (1984) Histopathological review of transitional cell carcinoma of the upper urinary tract. Br J Urol 56: 485-489.
-
McCarron JP Jr, Chasko SB, Gray GF Jr (1982) Systematic mapping of nephroureterectomy specimens removed for urothelial cancer: pathological findings and clinical correlations. J Urol 128: 243-246.
-
Margulis V, Shariat SF, Matin SF, Kamat AM, Zigeuner R, et al. (2009) Outcomes of radical nephroureterectomy: a series from the Upper Tract Urothelial Carcinoma Collaboration. Cancer 115: 1224-1233.
-
Pak RW, Moskowitz EJ, Bagley DH (2009) What is the cost of maintaining a kidney in upper-tract transitional-cell carcinoma? An objective analysis of cost and survival. J Endourol 23: 341-346.
-
Straub J, Strittmatter F, Karl A, Stief CG, Tritschler S (2012) Ureterorenoscopic biopsy and urinary cytology according to the 2004 WHO classification underestimate tumor grading in upper urinary tract urothelial carcinoma. Urol Oncol 32: 1685-1687.
-
Hsueh TY, Huang YH, Chiu AW, Shen KH, Lee YH (2004) A comparison of the clinical outcome between open and hand-assisted laparoscopic nephroureterectomy for upper urinary tract transitional cell carcinoma. BJU Int 94: 798-801.
-
Kawauchi A, Fujito A, Ukimura O, Yoneda K, Mizutani Y, et al. (2003) Hand assisted retroperitoneoscopic nephroureterectomy: comparison with the open procedure. J Urol 169: 890-894.





