International Journal of Surgery Research and Practice
Predictors of Survival after Adult to Adult Living Donor Liver Transplantation (A-ALDLT)
Emad Hamdy Gad1* , Ayman Alsebaey2 and Maha Lotfy3
1Hepatobiliary Surgery Department, National Liver Institute, Menoufiya University, Shibin El- Kom, Menoufiya, Egypt
2Hepatology Department, National Liver Institute, Menoufiya University, Shibin El-Kom, Menoufiya, Egypt
3Anesthesia department, National Liver Institute, Menoufiya University, Shibin El-Kom, Menoufiya, Egypt
*Corresponding author: Emad Hamdy Gad, Hepatobiliary and liver transplantation, National Liver Institute, Menoufiya University, Shebein Elkoum, Egypt, Tel: 02-0100-3031128, E-mail: Emadgadsalemaa@yahoo.com
Int J Surg Res Pract, IJSRP-1-006, (Volume 1, Issue 1), Research Article; ISSN: 2378-3397
Received: August 24, 2014 | Accepted: September 24, 2014 | Published: September 26, 2014
Citation: Gad EH, Alsebaey A, Lotfy M (2014) Predictors of Survival after Adult to Adult Living Donor Liver Transplantation (A-ALDLT). Int J Surg Res Pract 1:006. 10.23937/2378-3397/1410006
Copyright: ©2014 Gad EH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
List of Abbreviations
DDLT Deceased donor liver transplantation
IRB Institutional review board
BMI Body Mass Index
CUSA Cavitron ultrasonic surgical aspirator
CNIs CalciNeurin Inhibitors
CsA CycloSporine
FK or FK-506 Tacrolimus
GRWR Graft Recipient Weight Ratio
HBV Hepatitis B virus
HTK Hydroxy tryptophan ketoglutarate
HCC HepatoCellular Carcinoma
HCV Hepatitis C Virus
SFSS Small for size syndrome
HPB HepatoPancreatoBiliary
A-ALDLT Adult to adult living donor liver transplantation
LT Liver Transplantation
MELD Model for End stage Liver Disease
MMF Mycophenolate MoFetil
NLI National Liver Institute
SRL SiRoLomus
Abstract
Objectives: Adult-to-adult living donor liver transplantation (A-A LDLT) is an effective therapeutic modality to treat patients with end-stage liver disease. The aim of this study was to define the pre-, intra- and post- operative factors that may influence patient outcome.
Methods: The data from 161 (A-A LDLT) patients who had operations between 2003 and 2013 were collected and analyzed retrospectively after exclusion of mortality due to intra-operative bleeding. Data were analyzed using uni- and multi-variate analysis according to factors that are known to be associated with outcome in these patients.
Results: Overall, the accurate survival rate of recipients at, 6 months, 1, 3, 5 and 7 years was 67.7%, 63.4 %, 59.0%, 58.4% and 57.1% respectively. On univariate analysis, the following factors were significant predictors of survival, male recipients, Actual GRWR > 0.8, right lobe graft, blood transfusion< 10 units and absence of vascular complications. On multivariate analysis, male recipients, blood transfusion >10 units and absence of vascular complications were independent predictors.
Conclusions: The reduction of intraoperative RBC, prevention and treatment of vascular complications, selection (GRWR > 0.8, right lobe graft and male recipients) are required to achieve better survivals among patients undergoing A-A LDLT.
Keywords
Living Donor Liver Transplantation, Outcome post LDLT. Vascular complications.
Introduction
Liver transplantation (LT) is a widely accepted treatment method for patients with end-stage liver diseases [1]. Studies have shown that advances in surgical technology, anesthesia management, and the detection and treatment of complications made over the last decade or so have significantly improved the 1-, 5- and 10-year survival rates by 85%, 70%, and 60%, respectively [2]. In response to the organ donor shortage, A-A LDLT has emerged as an effective alternative to deceased donor liver transplantation (DDLT), Compared to DDLT, LDLT offers a reduced waiting time and more optimal timing of surgery, but it is also associated with a high surgical risk and complications for the recipient because of differences in graft quality, size and preservation time [3]. In Egypt, the availability of deceased donors remains extremely limited, because traditional religious and emotional issues continue to present obstacles in regard to performing DDLT. For this reason, LDLT is the primary type of liver transplantation in Egypt. Different studies have reported some risk factors that affect recipient survival and graft loss after DDLT [4,5]. On the other hand, in LDLT, graft and recipient survival are decided by the combination of donor, intraoperative and recipient factors and the risk factors of survival after LDLT were mentioned in different studies. [6-10]. The aim of this study was to define the pre-, intra- and post- operative factors that may influence patient outcome after A-ALDLT.
Materials and Methods
After approval of institutional review board (IRB) and obtaining written informed consents from both donors and recipients, we retrospectively analyzed the pre-, intra- and post- operative factors that may influence patient outcome in the department of hepatopancreatobiliary (HPB) surgery, national liver institute (NLI), university of Menoufiya, Menoufiya, Egypt, in the period from April 2003 to November 2013 or patient death with median follow up period of 25.6 � 25.6 m (range, 0-120). The study included 161 (A-A LDLT) patients who had operations between April 2003 and February 2013 after exclusion of mortality due to intra-operative bleeding. All donors were< 19 years old and the donor work-up included liver function tests, liver biopsy, ultrasound examination, psychological assessment and CT angiography, along with hepatic volumetric study and vascular reconstructions The following data were studied:
A- Preoperative Variables:
Donor's age, gender, body mass index (BMI), donor to recipient relation, Femal to male donor to recipient matching, blood group matching, liver biopsy of donors, recipients' age, gender, the primary disease, Child Pugh and MELD scores, co morbidity (DM, HTN) and portal hypertension.
B- Intraoperative Variables: Type of graft (Right or Left), duration of the operation per hours, actual graft weight, actual graft recipient weight ratio (GRWR> or < 0.8), cold and worm ischemia times per minute, blood transfusion < or > 10 units.
The donor operation was performed through a right subcostal incision extended to the upper midline under general anesthesia. Intraoperative cholangiography was used to define the biliary anatomy of donors, the right or left lobes of the liver were mobilized and the vena cava was dissected. The CUSA device was used to divide the liver parenchyma without inflow occlusion. The falciform ligament was reconstructed, the stumps of the divided hepatic and portal veins were closed by continuous non-absorbable sutures, after graft harvesting, it was perfused in the back table with Hydroxy tryptophan ketoglutarate (HTK) solution and weighted to determine the actual GRWR [8] (Figure 1).
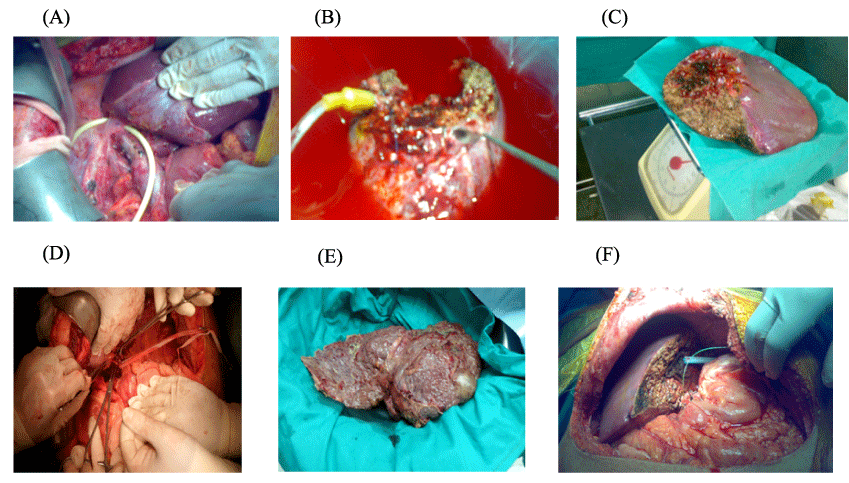
Figure 1: Donor and recipient operations
View Figure 1
In the recipient surgery, the native liver was explanted while carefully preserving the inferior vena cava. After reconstructing the hepatic and portal veins, the hepatic artery was anastomosed by the use of a surgical loupe or microscopy. The biliary tract was reconstructed by a duct-to-duct hepatico- choledochostomy or a Roux-en-Y hepatico-jejunostomy [7] (Figure1).
C- Postoperative Variables
A. Hospital stay ( per days)
B. Based on our institutional policy
Immunosuppression and postoperative anti-hepatitis B virus (HBV) protocols: the standard is combination of 3 drugs calcineurin inhibitors (CNIs), steroids and mycophenolate mofetil (MMF). The initial methylprednisolone dose is 500 mg intraoperatively with a brief taper of prednisone from 240 to 40 mg/d over 6 days followed by 5�20 mg/d maintenance treatment, with complete withdrawal at the end of 3rd month post LDLT. Cyclosporine (CsA) was used when neurotoxicty or nephrotoxicity developed with Tacrolimus. When CNIs are contraindicated or their side effects halt their use, sirolimus (SRL) was given at an initial dose of 3 mg/m2 and adjusted over time to achieve blood trough levels of approximately 5-8 ng/mL. Biopsy-proven acute rejection episodes were treated with steroid pulses (IV methylprednisolone 200 to 500 mg/d for 3 days), which were tapered over several days to the baseline dose. The postoperative anti-HBV protocols consisted of lamivudine combined with therapy with a low-dose of intramuscular hepatitis B immune globulin. Hepatitis B immune globulin was administered to all recipients with HBV infection during and after the transplantation [8].
c- Complications (Biliary, vascular and small for size syndrome).
Statistical Analysis
All data were tabulated and processed with SPSS software (Statistical Product and Service Solutions, version 21, SSPS Inc, Chicago, IL, USA) and Windows XP (Microsoft Corporation, Redmond, Washington, USA). Qualitative data were expressed in frequency and percentage and analyzed with the chi-square test. Quantitative data were expressed as the mean and standard deviation and were compared with the t test. The previous (preoperative, intraoperative and postoperative) variables were descriptively studied. Univariate analysis and then multivariate analysis for significant predictors in univariate analysis were done to detect the relationship between the previous data and overall survival of patients in the follow up period after A-ALDLT. The Kaplan-Meier method was applied for survival analysis and compared using log-rank tests. In all tests, a P value of < 0.05 was considered significant.
Results
Characters of patients and their donors
They were classified as 141 (87.6%) males, and 20(12.4%) females. Their mean age was 46.27�8.3. Their donors were classified as 109 (67.7%) males and 52(32.3%) females, their mean age was 27.07�6.6 and donor to recipient female to male match was 97(60.2%). The liver biopsy was abnormal (steatosis, minimal or mild PPF) in 32 (19.9%) of donor. The patients were classified according to Child-Pugh score into 9 (5.6%) class A, 47 (29.2%) class B, and 105 (65.2%) class C, and MELD score < 18 was found in 56 (34.8%). 61(37.9%) of them had co morbidity, in the form of Hypertension, DM, cardiac diseases and morbid obesity, Portal HTN affected 154 (95.7%) of them. The donor to recipient Bl. Group matching was classified into identical in 117 (72.7%) and Compatible in 44 (27.3%) of them. The right lobe graft was given to 153 (95%) and the left lobe was given to 8 (5%) of them. The mean actual graft weight was 820.16 � 172.9 and actual GRWR > 0.8 was found in 145 (90.1%) of patients. The mean cold and warm ischemia times were 73.8+51.4 and 51.8+16.09 respectively. More than 10 units of intra-operative blood transfusion were given to 34 (21.1%). The incidence of post operative biliary, vascular and small for size syndrome (SFSS) complications were 72 (44.7%), 34 (21.1%) and 19 (11.8%) respectively (Table 1).
![]()
Table 1: Characters of patients and their donors.
View Table 1
Indications of LT:The most frequent indications were HCV followed by HCC (Table 2).
![]()
Table 2: Indications of LT
View Table 2
Outcome of patients
The overall mortality was 69 (42.9%). While overall 6-months, 1-, 3- and 5- year survival of our patients were 109(67.7%), 102 (63.4%), 95 (59%), 94 (58.4%) and 92(57.1%) respectively, (Table 3).
![]()
Table 3: Outcome of patients
View Table 3
Recipients and donors risk factors as predictors of outcome
A- On univariate analysis, the following variables were found to be statistically significant predictors of outcome: Male recipients, Actual GRWR > 0.8, MELD score > 18, right lobe graft, blood transfusion >10 units and absence of vascular and SFSS complications. On the other hand, there was trends towards survival with the following variables: Less mean recepient age (45.7+8.2 years), more mean actual graft wt (838+166.8 gm), Less mean cold ischemia time (69.7+47.3minutes) and shorter mean operative time (12.7+3.1h) (Table 4, Table 5, Table 6, Figure 2).
![]()
Table 4: Recipients and donors risk factors as predictors of outcome.
View Table 4
![]()
Table 5: Recipients and donors risk factors as predictors of outcome.
View Table 5
![]()
Table 6: Recipients and donors risk factors as predictors of outcome.
View Table 6
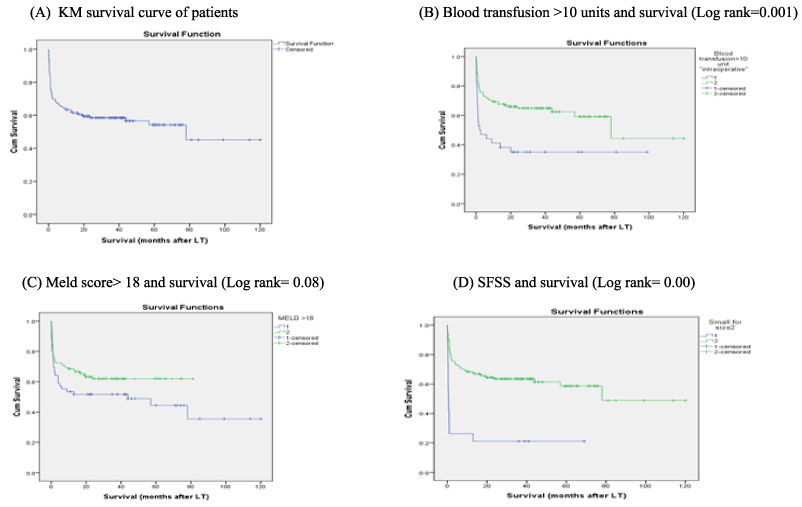
Figure 2: Kaplan-Meier survival curves
View Figure 2
B- On multivariate analysis, male recipients, blood transfusion >10 units and absence of vascular complications were independent predictors (Table 7).
![]()
Table 7: Multinomial logistic regression test.
View Table 7
Discussion
From the first report of A-A LDLT in 1993 by Yamaoka et al, 1993 [11], the cases of A-A LDLT have grown rapidly to address the shortage of livers. Living donor liver transplantation especially A-A LDLT has advantages over deceased donor grafts. Nevertheless, the complicated techniques in the recipient procedure and the potential risks for the donor require careful preoperative evaluation [9].
Researchers have identified several risk factors for graft loss after LDLT, such as donor age [12], MELD score [4,5,13-15], intra-operative blood loss [13,6] and small-for-size syndrome [17-20].
The inverse correlation between recipient age and LT outcome has been reported repeatedly [21-23]. Similarly, it showed statistical significance with survival in The univariate analysis in the (Jin et al, 2012) [24] study and trends towards poor survival in the recent study.
In our study, there was no significant difference between younger and older donors regarding survival. Similarly Kuramitsu et al, 2007 [25] reported no significant difference between selected right lobe donors from aged 60 years or older and younger donors regarding survival. In contrast Yoshizumi et al. 2008 [26], Morioka et al. 2007 [27] and Toshima et al. 2014) [28] have reported donor age to have a negative impact on the outcomes of recipients in LDLT. Similarly Yoshida et al, 2008 [29] found that aged grafts (< 50 years) were observed to have significantly poor outcomes.
Ninety five percent of our patients were given RT lobe graft with significant effect on good survival in univariate analysis; inversely the Tokyo University Group demonstrated that the survival outcomes of AALDLT recipients of non-right-liver grafts were significantly superior to those of recipients of right lobe or extended right lobe grafts [30]. On the other hand in Morioka et al, 2007[27] and Yoshida et al, 2008 [29] studies graft type was not associated with graft failure.
The MELD score, which has been used for allocating liver grafts in DDLT in the United States [31] has been reported to predict death before implementation of LT in patients with end stage liver disease [32]. On the other hand, The studies by Du et al. 2013 [10], Yoshizumi et al. [26], Morioka, et al. [27], Toshima et al. 2014 [28] and Saab et al. 2003 [33] demonstrated that high MELD score could predict post-transplant survival outcomes. Similarly the present study revealed that MELD score < 18 was significant predictor of poor outcome in univariate analysis and in [Yoshida et al. 2008 [29] study, recipients with a high MELD score (< 21) were found to have significantly poor outcomes compared with recipients with a low MELD score (>21). In contrast Hayashi et al. 2003 [34] and Kenneth et al. 2013 [35] reported that the MELD score did not predict the recipient survival in LDLT.
Most studies have shown that a GRWR (considered to be a direct reflection of small for- size syndrome) less than 0.8% increases the opportunity for early graft failure [6,9,36]. Similarly, in our study, GRWR> 0.8 was signifcant predictor of poor outcome in univariate analysis. The clinical significance of this result urges us to emphasize graft-to-recipient matching. On the other hand, Ben-Haim et al. 2001[37] showed that mortality rates among Child�s class B or C patients whose GRWR less than 0.85%, three-fold greater than among those with GRWR greater than 0.85% in Child's class A.
Our data showed that intra-operative transfusion of more than 10 exogenous packed RBC units was independent predictor of poor outcome. Similarly, Chuan et al. 2011 [8], Xu et al. 2011 [9], [Du et al. 2013 [10] and Chung et al. 2013 [38] Found that intra-operative blood loss was significant predictor of poor outcome. However Lee et al. 2004 [6] demonstrated that intraoperative transfusion of more than six exogenous packed RBC units was an independent factor influencing graft survival. They explained this by increase of perioperative cytokine responses (i.e. IL6); that affect graft survival with the increased amount of intra-operative transfusion.
Vascular problems after liver transplantation are among the most serious complications that frequently result in graft failure and patient death (39). In the studies by Sevmis et al. 2011 [40], Steinbr�ck et al. 2011 [41] and Orlandinia et al. 2014 [42] vascular complications had significant effect on survival. Similarly, in our study, there was significant correlation between vascular complications and survival.
Conclusions
The reduction of intraoperative RBC, prevention and treatment of vascular complications, selection (GRWR > 0.8, MELD Score >18, right lobe graft and male recipients) are required to achieve better survival among patients undergoing A-A LDLT.
Declaration:
Forms of support received by each author for this study included good selection of cases, instructive supervision, continuous guidance, valuable suggestions and good instructions. No grant or other financial support was received for this study.
References
-
Ahmed A, Keeffe EB (2007) Current indications and contraindications for liver transplantation. See comment in PubMed Commons below Clin Liver Dis 11: 227-247.
-
Fisher RA, Cotterell AH, Maluf DG, Stravitz RT, Ashworth A, et al. (2009) Adult living donor versus deceased donor liver transplantation: a 10-year prospective single center experience. See comment in PubMed Commons below Ann Hepatol 8: 298-307.
-
Freise CE, Gillespie BW, Koffron AJ, Lok AS, Pruett TL, et al. (2008) Recipient morbidity after living and deceased donor liver transplantation: findings from the A2ALL Retrospective Cohort Study. See comment in PubMed Commons below Am J Transplant 8: 2569-2579.
-
Habib S, Berk B, Chang CC, Demetris AJ, Fontes P, et al. (2006) MELD and prediction of post-liver transplantation survival. See comment in PubMed Commons below Liver Transpl 12: 440-447.
-
Brand�o A, Fuchs SC, Gleisner AL, Marroni C, Zanotelli ML, et al. (2009) MELD and other predictors of survival after liver transplantation. See comment in PubMed Commons below Clin Transplant 23: 220-227.
-
Lee DS, Gil WH, Lee HH, Lee KW, Lee SK, et al. (2004) Factors affecting graft survival after living donor liver transplantation. See comment in PubMed Commons below Transplant Proc 36: 2255-2256.
-
Yoshida R, Iwamoto T, Yagi T, Sato D, Umeda Y, et al. (2008) Preoperative assessment of the risk factors that help to predict the prognosis after living donor liver transplantation. See comment in PubMed Commons below World J Surg 32: 2419-2424.
-
Li C, Wen TF, Yan LN, Li B, Yang JY, et al. (2011) Predictors of patient survival following living donor liver transplantation. See comment in PubMed Commons below Hepatobiliary Pancreat Dis Int 10: 248-253.
-
Xu N, Yan LN, Yang JY, Li B, Wen TF, et al. (2011) New prognostic model for adult-to-adult living donor liver transplant recipients. See comment in PubMed Commons below Transplant Proc 43: 1728-1735.
-
Du Z, Wei Y, Chen K, Chen X, Zhang Z, et al. (2013) Risk factors and criteria predicting early graft loss after adult-to-adult living donor liver transplantation. J Surg Res 187: 673-682.
-
Yamaoka Y, Tanaka K, Ozawa K (1993) Liver transplantation from living-related donors. See comment in PubMed Commons below Clin Transpl .
-
Castellv� JM, Xiol X, Guardiola J, Sabat� I, Roca M, et al. (2004) Pretransplantation risk factors for graft loss after liver transplantation in cirrhotic patients; effect of cytomegalovirus serologic status. See comment in PubMed Commons below Transpl Int 17: 131-137.
-
Tsunematsu I, Ogura Y, Inoue K, Koizumi A, Tanigawa N, et al. (2006) Quantitative survival model for short-term survival after adult-to-adult living donor liver transplantation. See comment in PubMed Commons below Liver Transpl 12: 904-911.
-
Ishigami M, Honda T, Okumura A, Ishikawa T, Kobayashi M, et al. (2008) Use of the Model for End-Stage Liver Disease (MELD) score to predict 1-year survival of Japanese patients with cirrhosis and to determine who will benefit from living donor liver transplantation. See comment in PubMed Commons below J Gastroenterol 43: 363-368.
-
Guo Z He X, Wu L, Ju W, Hu A, et al. (2010) Model for end-stage liver disease versus the Child-Pugh score in predicting the post-transplant 3-month and 1-year mortality in a cohort of Chinese recipients. See comment in PubMed Commons below Surg Today 40: 38-45.
-
Mueller AR, Platz KP, Krause P, Kahl A, Rayes N, et al. (2000) Perioperative factors influencing patient outcome after liver transplantation. See comment in PubMed Commons below Transpl Int 13 Suppl 1: S158-161.
-
Kiuchi T, Tanaka K, Ito T, Oike F, Ogura Y, et al. (2003) Small-for-size graft in living donor liver transplantation: how far should we go? See comment in PubMed Commons below Liver Transpl 9: S29-35.
-
Man K, Fan ST, Lo CM, Liu CL, Fung PC, et al. (2003) Graft injury in relation to graft size in right lobe live donor liver transplantation: a study of hepatic sinusoidal injury in correlation with portal hemodynamics and intragraft gene expression. See comment in PubMed Commons below Ann Surg 237: 256-264.
-
Soejima Y, Shimada M, Suehiro T, Hiroshige S, Ninomiya M, et al. (2003) Outcome analysis in adult-to-adult living donor liver transplantation using the left lobe. See comment in PubMed Commons below Liver Transpl 9: 581-586.
-
Dahm F, Georgiev P, Clavien PA (2005) Small-for-size syndrome after partial liver transplantation: definition, mechanisms of disease and clinical implications. Am J Transplant 5: 2605-2610.
-
Wigg AJ, Gunson BK, Mutimer DJ (2005) Outcomes following liver transplantation for seronegative acute liver failure: experience during a 12-year period with more than 100 patients. See comment in PubMed Commons below Liver Transpl 11: 27-34.
-
Barshes NR, Lee TC, Balkrishnan R, Karpen SJ, Carter BA, et al. (2006) Risk stratification of adult patients undergoing orthotopic liver transplantation for fulminant hepatic failure. See comment in PubMed Commons below Transplantation 81: 195-201.
-
Bernal W, Cross TJ, Auzinger G, Sizer E, Heneghan MA, et al. (2009) Outcome after wait-listing for emergency liver transplantation in acute liver failure: a single centre experience. See comment in PubMed Commons below J Hepatol 50: 306-313.
-
Jin YJ, Lim YS, Han S, Lee HC, Hwang S, et al. (2012) Predicting survival after living and deceased donor liver transplantation in adult patients with acute liver failure. See comment in PubMed Commons below J Gastroenterol 47: 1115-1124.
-
Kuramitsu K, Egawa H, Keeffe EB, Kasahara M, Ito T, et al. (2007) Impact of age older than 60 years in living donor liver transplantation. See comment in PubMed Commons below Transplantation 84: 166-172.
-
Yoshizumi T, Taketomi A, Soejima Y, Uchiyama H, Ikegami T, et al. (2008) Impact of donor age and recipient status on left-lobe graft for living donor adult liver transplantation. See comment in PubMed Commons below Transpl Int 21: 81-88.
-
Morioka D, Egawa H, Kasahara M, Ito T, Haga H, et al. (2007) Outcomes of adult-to-adult living donor liver transplantation: a single institution's experience with 335 consecutive cases. See comment in PubMed Commons below Ann Surg 245: 315-325.
-
Toshima T, Ikegami T, Kimura K, Harimoto N, Yamashita Y, et al. (2014) Application of Postoperative Model for End-Stage Liver Disease Scoring System for Evaluating Liver Graft Function After Living Donor Liver Transplantation. Transplant Proc 46: 81-86.
-
Yoshida R, Iwamoto T, Yagi T, Sato D, Umeda Y, et al. (2008) Preoperative assessment of the risk factors that help to predict the prognosis after living donor liver transplantation. See comment in PubMed Commons below World J Surg 32: 2419-2424.
-
Kokudo N, Sugawara Y, Imamura H, Sano K, Makuuchi M (2005) Tailoring the type of donor hepatectomy for adult living donor liver transplantation. See comment in PubMed Commons below Am J Transplant 5: 1694-1703.
-
Amin MG, Wolf MP, TenBrook JA Jr, Freeman RB Jr, Cheng SJ, et al. (2004) Expanded criteria donor grafts for deceased donor liver transplantation under the MELD system: a decision analysis. See comment in PubMed Commons below Liver Transpl 10: 1468-1475.
-
Heuman DM, Abou-Assi SG, Habib A, Williams LM, Stravitz RT, et al. (2004) Persistent ascites and low serum sodium identify patients with cirrhosis and low MELD scores who are at high risk for early death. See comment in PubMed Commons below Hepatology 40: 802-810.
-
Saab S, Wang V, Ibrahim AB, Durazo F, Han S, et al. (2003) MELD score predicts 1-year patient survival post-orthotopic liver transplantation. See comment in PubMed Commons below Liver Transpl 9: 473-476.
-
Hayashi PH, Forman L, Steinberg T, Bak T, Wachs M, et al. (2003) Model for End-Stage Liver Disease score does not predict patient or graft survival in living donor liver transplant recipients. See comment in PubMed Commons below Liver Transpl 9: 737-740.
-
Chok KS, Chan SC, Fung JY, Cheung TT, Chan AC, et al. (2013) Survival outcomes of right-lobe living donor liver transplantation for patients with high Model for End-stage Liver Disease scores. See comment in PubMed Commons below Hepatobiliary Pancreat Dis Int 12: 256-262.
-
Bernal W, Wendon J, Rela M, Heaton N, Williams R (1998) Use and outcome of liver transplantation in acetaminophen-induced acute liver failure. See comment in PubMed Commons below Hepatology 27: 1050-1055.
-
Ben-Haim M, Emre S, Fishbein TM, Sheiner PA, Bodian CA, et al. (2001) Critical graft size in adult-to-adult living donor liver transplantation: impact of the recipient's disease. See comment in PubMed Commons below Liver Transpl 7: 948-953.
-
Chung HS, Jung DH, Park CS (2013) Intraoperative predictors of short-term mortality in living donor liver transplantation due to acute liver failure. See comment in PubMed Commons below Transplant Proc 45: 236-240.
-
Khalaf H (2010) Vascular Complications After Deceased and Living Donor Liver Transplantation: A Single-Center Experience. Transplant Proc 42: 865-870.
-
Sevmis S, Karakayali H, Tutar NU, Boyvat F, Ozcay F, et al. (2011) Management of Early Hepatic Arterial Thrombosis After Pediatric Living-Donor Liver Transplantation. Transplant Proc 43: 605-608.
-
Steinbr�ck K, Enne M, Fernandes R, Martinho JM, Balbi E, et al. (2011) Vascular Complications After Living Donor Liver Transplantation: A Brazilian, Single-Center Experience. Transplant Proc 43: 196-198.
-
Orlandini M, Feier FH, Jaeger B, Kieling C, Vieira SG, et al. (2014) Frequency of and factors associated with vascular complications after pediatric liver transplantation. See comment in PubMed Commons below J Pediatr (Rio J) 90: 169-175.





