International Journal of Surgery Research and Practice
Precision of Measurements from Computed Tomography (CT), Cone Beam Computed Tomography (CBCT) and their Reformatted Images in Pre-Operative Implant Assessment
Walid Samir Salem *, Mushira M. Dahaba and Sherouk Khalifa
Salman Bin Abdulaziz University, Alkharj- Ryuadh, Saudi Arabia
*Corresponding author: Walid Samir Salem, Salman Bin Abdulaziz University, Alkharj- Ryuadh, Saudi Arabia, Tel: 966501415602, E-mail: dr.walidsalem@yahoo.com
Int J Surg Res Pract, IJSRP-1-004, (Volume 1, Issue 1), Research Article; ISSN: 2378-3397
Received: August 22, 2014 | Accepted: September 20, 2014 | Published: September 23, 2014
Citation: Salem WS, Dahaba MM, Khalifa S et al. (2014) Precision of Measurements from Computed Tomography (CT), Cone Beam Computed Tomography (CBCT) and their Reformatted Images in Pre-Operative Implant Assessment Int J Surg Res Pract 1:004. 10.23937/2378-3397/1410004
Copyright: ©2014 Salem WS. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Preclude the accuracy of dimensional, and linear measurements yielded from CBCT images, panoramic images reformatted from spiral CT, and panoramic images reformatted from CBCT in comparison to the measurements obtained from the cross-sectional CT.
Methods: Twenty patients attending the Oral Maxillofacial Surgery Department, for placement of dental implants in both jaws (10 subjects required mandibular and the other ten required 10 maxillary).
Results: A significant difference between the CT reformatted panoramic and GS results. Meanwhile, a non-significant difference was detected between both CBCT images in relation to the gold standard.
Conclusions: CBCT could be a helpful reliable indispensible tool for pre-surgical planning prior to dental implant insertion in the orofacial region.
Keywords
Dental Implant, Cone- Beam CT, Spiral CT, Digital Panoramic radiograph
Introduction
Radiography has been one of the frequently applied aids in human biometric research. It is essential to check for the accuracy of reproduction with respect to enlargement and projection. Without this accuracy errors can be incorporated into the measurement. Measurement is a vital aspect of interpretation, either of anatomical structures or pathological entities [1].
More recently, an increasing demand for dental implants for rehabilitation of edentulous jaws has raised an interest in the available imaging techniques to perform an accurate preoperative planning. It is essential to measure accurately the height of bone available for implant placement to avoid compromising vital structures such as the inferior alveolar nerve or maxillary sinus during placement of implants [2].
Panoramic imaging provides visualization of many anatomic features and is commonly available. Non-uniform horizontal magnification, the possibility of positioning artifacts and the lack of cross-sectional information are some of the limitations of panoramic radiography in pre-implant assessment [1]. The inherent problems with 2D imaging led to the need for 3D imaging which can overcome the issues of superimposition, blurring and magnification as these factors compromise measurement accuracy to a large extent [3].
Computed tomography which is a 3D imaging modality had long been in use in medical radiology before its use in dental implant imaging. The basic concept of CT includes measurement of attenuation of the x-ray beam through a subject at many positions around the subject and at a sufficient number of angles [3].
With modern multi detector CT imaging, multiple thin axial slices of data are obtained through the area of interest and added together to form a data volume. Cross sectional and panoramic images are reconstructed from this data through the use of softwares. The merits of CT images include uniform magnification, high contrast images with minimum blurring, and simultaneous assessment of multiple implant sites in a single study and multi planar images. The disadvantages include the high cost, the high radiation dose and the metallic streak artifacts if metallic objects such as dental restorations are present [4].
The introduction of Cone Beam Computed Tomography (CBCT) represents a radical change for dental and maxillofacial radiology. CBCT is a technology that provides cross-sectional images without superimposition or blurring [5,6]. And reduces the risk of radiation significantly [7,8]. CBCT provides 3D imaging dedicated to the maxillofacial region at low cost and low dose of radiation [1].
CBCT was developed as an alternative to conventional CT to shorten the time of image acquisition of the entire FOV (Field of View) with a comparatively less expensive radiation detector. The lack of patient translational movement results in improved sharpness of the image which is reduced in conventional CT imaging. The reduced time of acquisition also reduces image distortion that may be caused by internal organ movement [9,10].
For successful bone surgery planning and simulation, it is important that the geometric accuracy of the bone model is known. While the accuracy of bone segmentation has already been studied extensively for MSCT [11-15] so far only a few studies have assessed the accuracy of CBCT [16-19].
CBCT allows 3D visualization of the oral and maxillofacial complex. This imaging modality eliminates the shortcomings of 2D imaging, produces a smaller radiation dose than that of conventional CT and enables clinicians to make more accurate treatment planning decisions, which should lead to more successful surgical procedures. It helps to measure the quantity and the quality of the bone available for the placement of implants [20].
Although the previous studies have shown CBCT to be accurate, some of the accuracy may be due to the increase in contrast when soft tissues are replaced by air, and decreased scatter due to absence of soft tissues. It is important to determine if the accuracy of measurement is maintained with soft tissues intact as this would simulate a clinical situation more closely [20].
Consequently, this study was undertaken in an attempt to demonstrate the validity of measurements yielded from CBCT in assessment of dental implants.
Material and Methods
Study design: This study comprised twenty patients attending the Oral Maxillofacial Surgery Department, Faculty of Oral and Dental Medicine, Cairo University for placement of dental implants in both jaws (10 subject�s required mandibular dental placement and the other ten required 10 maxillary dental placement).
Methods of investigation:
All patients were imaged using the following imaging protocols:-
1. Cone Beam Computed Tomographic scanning (cross sections and reformatted panoramic images were obtained for every case).
2. Low dose MSCT (cross sections and reformatted panoramic images were obtained for every case).
CBCT imaging: CBCT images were performed with an i-CAT unit (Imaging Sciences International, Hatfield, PA). For the CBCT imaging the following settings were used 120 KV; 5 mA; FOV 130mm (mandible and maxilla); orientation landscape; exposure time 4 sec; voxel dimension 0.3 mm with the patient in a seated position
MSCT imaging: CT images were performed using Toshiba Activion�16 multislice CT system. For the MSCT scanning, the following settings were used: tube voltage 120 kV; tube current, 50 mA, 1.5 second, 0.5 mm, and helical pitch 2.5. The reconstruction interval was 1 mm. An acrylic trial denture base was constructed for each patient containing round radiopaque markers (gutta-percha) at the implant site to be used as a reference point during measurements.
Image analysis: I-All images were assessed by three oral radiologists with an experience not less than 10 years in the field of oral and maxillofacial radiology.
II-Dimensional and linear measurements were performed on the three images of every case following the protocol recommended by [21-23].
Then the measurements were performed twice by each observer at two different sessions with a two-week interval in between the two sessions. The measurements were performed in a blind fashion. Results from these two trials were statistically analyzed to reveal the intra-examiner reliability and diagnostic performance (between each observer and himself).
The inter-examiner reliability and diagnostic performance (between the three observers) were also tested between the measurements of the three observers (the repeatability of the measurements).
All the measurement was performed using the software included in each used unit. CBCT measurements were performed using the i-CAT-vision software, and the CT measurements were performed using eFilm Lite software.
III-From the 20 patients, readings for 30 implant sites were recorded in millimeters, a standardized tangent of fixed length drawn to the lower border of the markers at each investigated site was considered as the reference line for all measurements; the measurement were taken as the following:
Maxilla
Anterior area: From the marker to the nasal cavity (M-NC)
Premolar molar area: From the marker to the maxillary sinus (M-MS)
Mandible
Anterior area: From the marker to the inferior border (M-IB)
Premolar area:
� From the marker to the mental foramen (M-MF), &
� From the marker to the inferior border (M-IB)
Molar area
� From the marker to the inferior alveolar canal (M-IAC)
� From the marker to the inferior border (M-IB)
All calculated measurements were recorded along lines drawn perpendicular to the midpoint of that reference line.
Method of Statistical Analysis
Collected Data were analyzed using the Statistical Program for Social Sciences (SPSS) version 19. Serial numbers (1- 220) was given for each measurement. The technique in each measurement got a numeric value (1-5) relevant to the radiographic technique used.
Descriptive statistics were performed using frequency count and percentages. Independent t-tests were performed to determine the difference between the five studied techniques at the 5% level of significance.
Result
The current study involved twenty patients with 30 sites planned for implant insertion. All patients were subjected to MSCT scanning (cross-sectional and reformatted panoramic) and CBCT scanning ((cross-sectional and reformatted panoramic). According to evidence �based literature, measurements from CT cross-section views are reliably acceptable as being the most accurate radiographic measurements [24,25,26]. Consequently it was chosen as the gold standard measurement in the current work.
According to the edentulous areas examined in every case, every radiologist performed a total of 44 measurements on the different anatomical sites. In total, 220 measurements were made. The normal craniometrical anatomical distribution of the radiographic measurements and the means of the measurements are illustrated in Tables 1 &2.
![]()
Table 1: Summary for the performed measurements according to the normal anatomical radiographic locations
View Table 1
![]()
Table 2: The mean of the jaw measurements recorded by the 3 radiologists for all cases
View Table 2
CT: computed tomography
CBCT: cone beam computed tomography
RPCT: reformatted panoramic radiograph from CT
RPCBCT: reformatted panoramic radiograph from CBCT
Statistical Analysis of Measurements
Statistical analysis of the means of all recorded measurements (whole study sample): A significant difference between the CT reformatted panoramic and GS results. Meanwhile, a non-significant difference was detected between both CBCT images in relation to the gold standard. These results are shown in Figure 1.
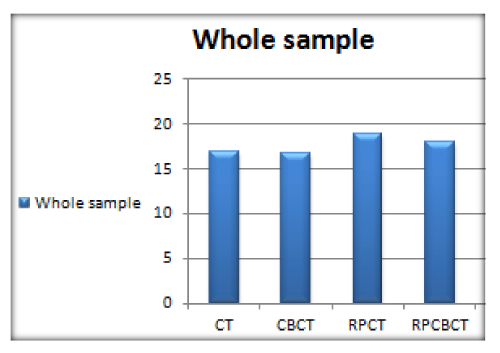 Figure 1: Bar charts comparing the mean measurements of the 3 imaging modalities to the gold standard (CT) in the whole study sample.
View Figure 1
Figure 1: Bar charts comparing the mean measurements of the 3 imaging modalities to the gold standard (CT) in the whole study sample.
View Figure 1
Statistical analysis of the mean maxillary measurements: The same results ass the whole sample was shown in the Maxillary measurements. These results are shown in Figure 2.
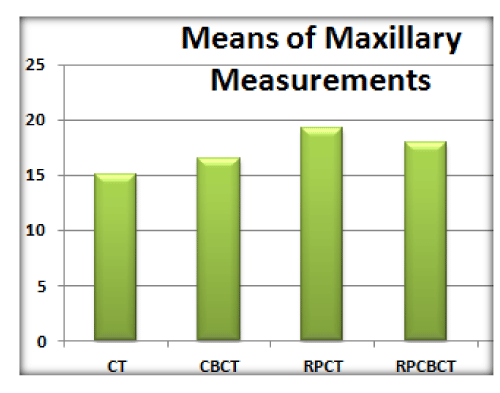 Figure 2: Bar charts comparing the mean measurements of the 4 imaging modalities to the gold standard (CT) in the maxillary arch.
View Figure 2
Figure 2: Bar charts comparing the mean measurements of the 4 imaging modalities to the gold standard (CT) in the maxillary arch.
View Figure 2
Statistical analysis of the mean M and measurements: A non-significant difference was detected between the CBCT and the RPCBCT in relation to the GS. In addition, there was a non-significant difference between the RPCT and the GS; this finding which was only detected in mandibular arch measurements. These results are shown in Figure 3.
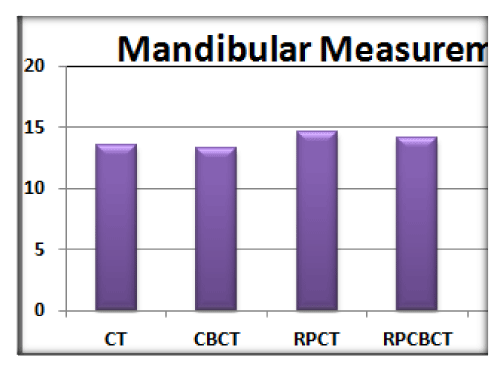 Figure 3: Bar charts comparing the mean measurements of the 4 imaging modalities to the gold standard (CT) in the mandibular arch.
View Figure 3
Figure 3: Bar charts comparing the mean measurements of the 4 imaging modalities to the gold standard (CT) in the mandibular arch.
View Figure 3
Discussion
Discussion of methodology: A preoperative radiographic evaluation aims to identify pathological lesions, assess the quantity and quality of the alveolar bone, identify critical structures at the potential implant sites, and determine the orientation of the implants [25].
The development of computed tomography (CT) enabled three-dimensional (3D) assessment of craniofacial structures. CT has become a widely available mean for head and neck diagnosis [27,28] and various oral surgical procedures [29].
CT equipped with specific software designed for implantology could be used to determine the suitability of bone and specific sites for implant placement, the size of the implant that can be placed, and the need for pre-implantation ridge surgery [29].
Due to all of the previous recommendations for the superiority of the direct CT images in implantology, the measurements obtained from the direct coronal CT cuts were considered the standard gold results and were compared to the data obtained from the other modalities investigated in the present work. However, CT is still not ideal for the particular diagnostic task in dental applications, such as impacted teeth or apical lesions. Excessive radiation exposure, increased cost and limited availability impede the routine use of this technology for dental applications. Cone Beam CT (CBCT) offers a promising alternative approach since it provides sub-millimetre resolution images of high diagnostic quality, with short scanning time and reduced radiation dose up to 15 times lower than Multi-Slice CT scans (MSCT) [9].
Discussion of results: Upon analyzing the calculated data in the current study, a non - significant difference was detected between measurements yielded from MSCT and CBCT cross-section views in either jaw as well as in the whole study sample.
They reported similar results they concluded that the CBCT unit provided satisfactory information about linear distances and volumes [30]. Moreover, [31] assessed dry skulls the distances between anatomic points and reference wires. Measurement accuracy was expressed by average errors of less than 0.6% for dimensional measurement techniques. Again their findings are in agreement with ours.
They worked with two different CBCT units: the New Tom QR DVT 9000 and the Hitachi MercuRay [32]. Measurements were made on human dry skulls using both these units and compared to a gold standard of caliper measurements. They concluded that both the CBCT systems provided highly accurate data with less than 1% relative error.
The current results are also in concordance with those reported by [33] who scanned a dry human mandible with five CBCT systems and one MSCT scanner. From this study, the authors concluded that clinically acceptable results are obtained for both MSCT and CBCT regarding implant planning and placement.
On the other hand, a study was carried to evaluate the images of a dental implant demonstrated that MSCT images had better quality compared with CBCT images. Their findings differed from those of the present study. These differences might be attributed to certain variations between the two study designs; since their study was performed on models lacking hard tissue around the implant in the their study, hence a direct comparison with the present data should be interpreted with caution. Variation in scanning protocol such as voxel size and number of projection images may also influence dimensional accuracy.
When the measurements of the reformatted CT panoramic images were compared to the gold standard data, a significant difference was detected between the maxillary measurements while a non- significant difference was found between the mandibular measurements. These variations in jaw measurements could be the result of the interpretation of the location of vital structures.
On the other hand, the reformatted CBCT panoramic images revealed equivocal data comparable to the gold standard. The accuracy of these measurements could be attributed to the sub-millimeter isotropic voxel for the CBCT which can reform a 2D image with high accuracy.
From the present study, the following conclusions could be conducted: CBCT demonstrated a comparable accuracy in linear measurements in both jaws. Considering these results with low radiation, short scanning time and appropriate image quality, CBCT could be a helpful reliable indispensible tool for pre-surgical planning prior to dental implant insertion in the orofacial region.
References
-
Cavalcanti MG, Haller JW, Vannier MW (1999) Three-dimensional computed tomography landmark measurement in craniofacial surgical planning: experimental validation in vitro. J Oral Maxillofac Surg 57: 690-694.
-
Tyndall DA, Brooks SL (2000) Selection criteria for dental implant site imaging: a position paper of the American Academy of Oral and Maxillofacial radiology. See comment in PubMed Commons below Oral Surg Oral Med Oral Pathol Oral Radiol Endod 89: 630-637.
-
Goldman LW (2007) Principles of CT and CT technology. See comment in PubMed Commons below J Nucl Med Technol 35: 115-128.
-
Rothman SL, Chaftez N, Rhodes ML, Schwarz MS (1988) CT in the preoperative assessment of the mandible and maxilla for endosseous implant surgery. Work in progress. See comment in PubMed Commons below Radiology 168: 171-175.
-
Mozzo P, Procacci C, Tacconi A, Martini PT, Andreis IA (1998) A new volumetric CT machine for dental imaging based on the cone-beam technique: preliminary results. See comment in PubMed Commons below Eur Radiol 8: 1558-1564.
-
Arai Y, Tammisalo E, Iwai K, Hashimoto K, Shinoda K (1999) Development of a compact computed tomographic apparatus for dental use. See comment in PubMed Commons below Dentomaxillofac Radiol 28: 245-248.
-
Hashimoto K, Arai Y, Iwai K, Araki M, Kawashima S, et al. (2003) A comparison of a new limited cone beam computed tomography machine for dental use with a multidetector row helical CT machine. See comment in PubMed Commons below Oral Surg Oral Med Oral Pathol Oral Radiol Endod 95: 371-377.
-
Ludlow JB, Davies-Ludlow LE, Brooks SL (2003) Dosimetry of two extraoral direct digital imaging devices: NewTom cone beam CT and Orthophos Plus DS panoramic unit. See comment in PubMed Commons below Dentomaxillofac Radiol 32: 229-234.
-
Scarfe WC, Farman AG (2008) What is cone-beam CT and how does it work? See comment in PubMed Commons below Dent Clin North Am 52: 707-730.
-
Farman AG, Scarfe WS (2009) The basic of Maxillofacial cone beam computed tomography. Seminars in Orthodontics 15: 2-13.
-
Aamodt A, Kvistad KA, Andersen E, Lund-Larsen J, Eine J, et al. (1999) Determination of Hounsfield value for CT-based design of custom femoral stems. See comment in PubMed Commons below J Bone Joint Surg Br 81: 143-147.
-
Kang Y, Engelke K, Kalender WA (2003) A new accurate and precise 3-D segmentation method for skeletal structures in volumetric CT data. See comment in PubMed Commons below IEEE Trans Med Imaging 22: 586-598.
-
Egger G, Korb W, Welzel T, Da�ber S, Marmulla R, et al. (2005) The accuracy of CT based craniofacial models for robotic surgery, Proceedings Surgetica 399-405.
-
De Vos W, Casselman J, Swennen GR (2009) Cone-beam computerized tomography (CBCT) imaging of the oral and maxillofacial region: a systematic review of the literature. See comment in PubMed Commons below Int J Oral Maxillofac Surg 38: 609-625.
-
Munetaka Naitoh, Kino Nakahara, Yutaka Suenaga, Kenichi Gotoh, Shintaro Kondo, et al. (2010) Comparison between cone-beam and multislice computed tomography depicting mandibular neurovascular canal structures. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology e25-e31.
-
Kobayashi K, Shimoda S, Nakagawa Y, Yamamoto A (2004) Accuracy in measurement of distance using limited cone-beam computerized tomography. See comment in PubMed Commons below Int J Oral Maxillofac Implants 19: 228-231.
-
Lascala CA, Panella J, Marques MM (2004) Analysis of the accuracy of linear measurements obtained by cone beam computed tomography (CBCT-NewTom). See comment in PubMed Commons below Dentomaxillofac Radiol 33: 291-294.
-
Marmulla R, W�rtche R, M�hling J, Hassfeld S (2005) Geometric accuracy of the NewTom 9000 Cone Beam CT. See comment in PubMed Commons below Dentomaxillofac Radiol 34: 28-31.
-
Miet Loubele, Frederik Maes, Filip Schutyser, Guy Marchal, Reinhilde Jacobs, et al. (2006) Assessment of bone segmentation quality of cone-beam CT versus multislice spiral CT: a pilot study. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology 225-234.
-
Howerton WB Jr, Mora MA (2008) Advancements in digital imaging: what is new and on the horizon? See comment in PubMed Commons below J Am Dent Assoc 139 Suppl: 20S-24S.
-
Simon JH, Enciso R, Malfaz JM, Roges R, Bailey-Perry M, et al. (2006) Differential diagnosis of large periapical lesions using cone-beam computed tomography measurements and biopsy. See comment in PubMed Commons below J Endod 32: 833-837.
-
Stavropoulos A, Wenzel A (2007) Accuracy of cone beam dental CT, intraoral digital and conventional film radiography for the detection of periapical lesions. An ex vivo study in pig jaws. See comment in PubMed Commons below Clin Oral Investig 11: 101-106.
-
Liu DG, Zhang WL, Zhang ZY, Wu YT, Ma XC (2008) Localization of impacted maxillary canines and observation of adjacent incisor resorption with cone-beam computed tomography. See comment in PubMed Commons below Oral Surg Oral Med Oral Pathol Oral Radiol Endod 105: 91-98.
-
Andersson L, Kurol M (1987) CT scan prior to installation of osseointegrated implants in the maxilla. See comment in PubMed Commons below Int J Oral Maxillofac Surg 16: 50-55.
-
Schwarz MS, Rothman SL, Chafetz N, Stauts B (1990) Preoperative diagnostic radiology for the tissue-integrated prosthesis. In: Laney WR, Tolman DE, editors. Tissue integration in oral, orthopedic, and maxillofacial reconstruction. Chicago, Quintessence 68-79.
-
Shui-Cheong Siu Adam, Frederick Cho-Shun Chu, Thomas Ka-Lun Li, Tak-Wah Chow, Fei-Long Deng (2010) Imaging modalities for preoperative assessment in dental implant therapy: an overview. Hong Kong Dent J 7: 23-30.
-
Fuchs T, Kachelriess M, Kalender WA (2000) Technical advances in multi-slice spiral CT. See comment in PubMed Commons below Eur J Radiol 36: 69-73.
-
Bou Serhal C, Jacobs R, Flygare L, Quirynen M, van Steenberghe D (2002) Perioperative validation of localisation of the mental foramen. See comment in PubMed Commons below Dentomaxillofac Radiol 31: 39-43.
-
Sarment DP, Sukovic P, Clinthorne N (2003) Accuracy of implant placement with a stereolithographic surgical guide. See comment in PubMed Commons below Int J Oral Maxillofac Implants 18: 571-577.
-
Mischkowski RA, Pulsfort R, Ritter L, Neugebauer J, Brochhagen HG, et al. (2007) Geometric accuracy of a newly developed cone-beam device for maxillofacial imaging. See comment in PubMed Commons below Oral Surg Oral Med Oral Pathol Oral Radiol Endod 104: 551-559.
-
Ludlow JB, Laster WS, See M, Bailey LJ, Hershey HG (2007) Accuracy of measurements of mandibular anatomy in cone beam computed tomography images. See comment in PubMed Commons below Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103: 534-542.
-
Stratemann SA, Huang JC, Maki K, Miller AJ, Hatcher DC (2008) Comparison of cone beam computed tomography imaging with physical measures. See comment in PubMed Commons below Dentomaxillofac Radiol 37: 80-93.
-
Xin Lianga, Reinhilde Jacobsa, Bassam Hassan, Limin Li, Ruben Pauwels, (2010) A comparative evaluation of Cone Beam Computed Tomography (CBCT) and Multi-Slice CT (MSCT) Part I. On subjective image quality. European Journal of Radiology 75: 265-269.





