International Journal of Surgery Research and Practice
Single-Incision Laparoscopic Morgagni Hernia Repair in an Adult
Sharon Monsivais 1,2 Nicole E. Sharp1,2, Hannah Vassaur2 and F. Paul Buckley2*
1College of Medicine, Texas A&M Health Science Center, Temple, Texas, USA
2General Surgery, Scott & White Healthcare, Round Rock, Texas, USA
*Corresponding author: F. Paul Buckley III, Scott & White Healthcare, MS-MB-3.019, 302 University Blvd, Round Rock, TX 78665, Tel: 512-509-0434, Fax: 512-509-8303, E-mail: pbuckley@swmail.sw.org
Int J Surg Res Pract, IJSRP-1-002, (Volume 1, Issue 1), Case report; ISSN: 2378-3397
Received: July 28, 2014 | Accepted: September 05, 2014 | Published: September 07, 2014
Citation: Monsivais S, Sharp NE, Vassaur H, Buckley FP. (2014) Single-Incision Laparoscopic Morgagni Hernia Repair in an Adult. Int J Surg Res Pract 1:002. 10.23937/2378-3397/1410002
Copyright: © 2014 Monsivais S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: This is a case report of a single-incision laparoscopic Morgagni hernia repair. We discuss our initial experience with this technique.
Case Description: A 63-year-old man elected to undergo a single-incision laparoscopic Morgagni hernia repairs after diagnostic imaging showed a large fat containing right diaphragmatic hernia. The patient�s only preoperative symptom was periodic right sided chest pain. The procedure was accomplished through a 2 cm vertical umbilical incision using a Covidien SILS™ port and a combination of straight and articulating laparoscopic instruments. Total operative time was 119 minutes. The patient was discharged home on post-operative day one. The patient tolerated the procedure well without any intraoperative complications or post-operative complications over18 months of follow-up.
Conclusion: Single-incision laparoscopic Morgagni hernia repair is safe and feasible in the hands of experienced laparoscopic surgeons. This technique provides an alternative to open and traditional laparoscopic repair.
Keywords
Minimally Invasive Surgical Procedures, Laparoscopy, Diaphragmatic hernia
Introduction
The foramen of Morgagni lies in the right sternocostal triangle of the anterior diaphragm and allows passage of the superior epigastric arteries and lymphatics. First described in 1761 by Giovanni Battista Morgagni, this muscular defect creates a potential space for herniation of abdominal contents into the thoracic cavity. While rare, some estimate that Morgagni hernias comprise 3-4% of all diaphragmatic hernias [1]. Though more common in the pediatric population, there is a growing collection of case reports and series documenting the occurrence in adults [2]. Due to a lack of classic constellation of symptoms, prompt and accurate diagnosis can be difficult. Patient presentation ranges from asymptomatic, to chest pain or pressure, to pulmonary manifestations [2]. There is not currently a universal protocol for working up a suspected Morgagni hernia, but surgical repair is typically necessary to reduce morbidity associated within carceration [3]. Currently, there are four accepted surgical techniques in the repair of a Morgagni hernia: thoracotomy, thoracoscopy, laparotomy and laparoscopy. While there is clear evidence for the benefits of laparoscopic technique versus open, there are no case reports detailing the repair of a Morgagni hernia through the use of Single-incision Laparoscopic Surgery (SILS) in adults, even with its documented advantages [4-6]. When given the choice of laparoscopic verses SILS, a 65-year-old man with a large Morgagni hernia elected to undergo repair via the SILS approach.
As the field of surgery continues to advance, so too do the surgical techniques and instruments. Procedures traditionally performed open are now accomplished laparoscopically due to well documented advantages, most notably a reduction in post-operative pain and recovery time [7-9]. Subsequently, the application of SILS has evolved as an even less invasive form of laparoscopy. Studies to date have indicated that patients undergoing SILS cholecystectomy and appendectomy had no increase in post-operative complications and are mixed in respect to benefits concerning post-operative pain and recovery [4,5,8]. SILS, however, demonstrated higher patient satisfaction scores with post-operative cosmesis [4,5,10].
Case Summary
A 65-year-old man with a complicated medical history was referred to the general surgery clinic after a Morgagni diaphragmatic hernia was found incidentally during a routine laparoscopic cholecystectomy. A computed tomography (CT) scan was obtained to characterize the hernia in further detail and determine additional management (Figure 1, Figure 2). The scan revealed a 6-7 cm right diaphragmatic defect, and the decision was made to proceed with the surgery. The risks, benefits, and alternatives were discussed with the patient. We also discussed the SILS approach versus traditional multiport laparoscopy. The patient elected for the SILS approach and consented in full.His American Society of Anesthesiologists score was 3 and he had a Body Mass Index (BMI) of 34.8 kg/m2.
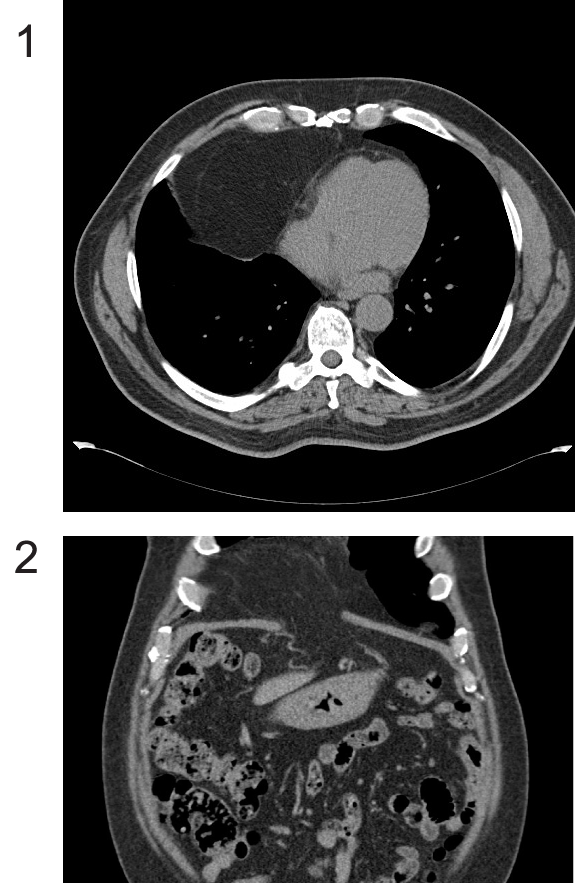 Figure 1: A computed tomography (CT) scan was obtained to characterize
the hernia in further detail and determine additional management.
View Figure 1
Figure 1: A computed tomography (CT) scan was obtained to characterize
the hernia in further detail and determine additional management.
View Figure 1
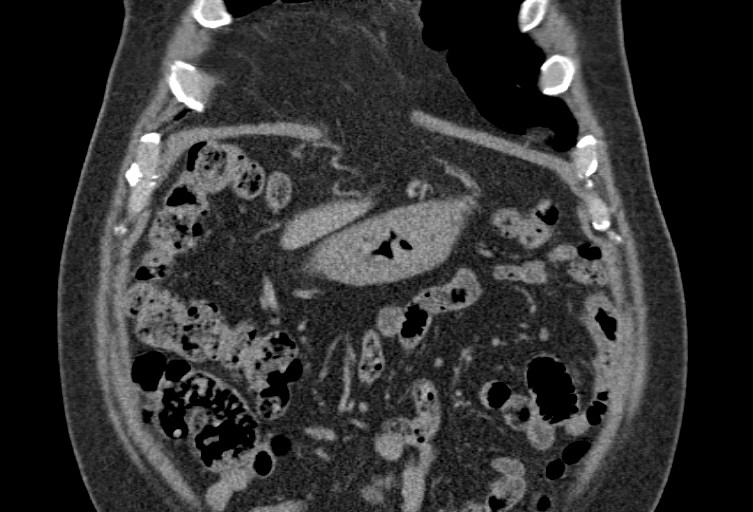 Figure 2: A computed tomography (CT) scan was obtained to characterize
the hernia in further detail and determine additional management.
View Figure 2
Figure 2: A computed tomography (CT) scan was obtained to characterize
the hernia in further detail and determine additional management.
View Figure 2
A single2 cm incision was made in the umbilicus and carried down and through the fascia, at which point a Covidien SILS™ port was placed within the defect. With the patient in steep reverse Trendelenburg, the hernia was visualized, with omentum and colon clearly contained within it. Utilizing traditional and articulating laparoscopic instruments, the hernia contents were reduced. The sac was then excised with a LigaSure™device and extreme caution was exercised to avoid injuring the pericardium or pleural space. The defect was measured to be approximately 7 x 5 cm in size. Parietex™ Composite mesh measuring 20 x 15 cm was used to cover the defect in its entirety. The mesh was secured using a combination of absorbable tacks and interrupted 0-0 braided nylon sutures. Diagnostic laparoscopy did not reveal any additional defects or abnormalities, and the SILS port was removed. The fascial defect was repaired using two 0-0absorbable sutures, both in a figure- of-eight fashion. The skin was closed using a home-made vacuum dressing. Total operative time was 119 minutes.
Results
A 65-year-old male presented with an incidental finding of a Morgagni hernia, which was repaired through a 2 cm incision using SILS technique and standard laparoscopic instruments. After successful repair of the diaphragmatic hernia, the patient was discharged home on post-operative day one. He had no intra-operative or post-operative complications and had minimal post-operative pain at his 1 week follow-up visit.
Discussion
Morgagni was the first to describe abdominal content herniation occurring through a right sided retrosternal muscular diaphragmatic defect. However, in 1829 Dominique Larrey described the left sternocostal triangle as a means to access the heart during a pericardial tamponade. Therefore, the right sternocostal hiatus has been referred to by some as the �foramina of Morgagni� and the left sternocostal hiatus as the foramina of Larrey [11]. In terms of embryology, however, both foramina were formed in the same manner.
Diaphragmatic development is a complex process and primarily occurs between weeks four and 12 of gestation [2]. Four embryologic structures comprise the diaphragm, with formation beginning in a rostral fashion and descending. The diaphragm�s components include the septum transversum (also called the central tendon), the pleuroperitoneal membranes, the dorsal esophageal mesentery, and the muscular components derived from the dorsal and lateral body wall. While these components are coalescing and migrating caudally, the sternum also fuses together, and abdominal organogenesis rapidly continues [11]. When the anterior pleura peritoneal membrane fails to fuse with the sternum and costal cartilage, there is a potential defect for a Morgagni hernia to occur [9].
Given that Morgagni hernias are uncommon, there is no universal protocol to follow during work up, and initial detection usually requires strong clinical suspicion[11]. Further complicating diagnosis, several case studies and retrospective studies have demonstrated a wide array of symptoms, ranging from asymptomatic to pulmonary complaints, chest pain, or dysphagia [2]. Several risk factors have been recognized by investigators, including trauma, obesity, pregnancy and chronic cough, with increased intra-abdominal pressure identified as the likely common factor. The majority of diaphragmatic hernias have been documented as right sided, and contents of the hernia sac have been seen to include omentum, small intestine, colon, or stomach [2,3].
Even without consensus guidelines, there have been case studies compiling data about the optimal method to visualize the hernia. Chest x-ray is usually the first technique employed, and may show an anterior mass or loops of bowel within the chest [9]. It has been suggested that insertion of a nasogastric tube can be utilized prior to imaging to determine if there is stomach within the chest, but most clinicians opt to further characterize the abnormality via CT scan. Other cases have used barium swallows or enemas to confirm the diagnosis [9].
The imaging studies reveal a diagnosis, surgical management is strongly recommended due to the risk of incarceration [3,9]. Further, elective cases can be managed with more minimally invasive options, and laparotomyis only recommended in emergent surgical repair [2]. Like common laparoscopic surgeries including cholecystectomy and appendectomy, the benefits of laparoscopic Morgagni hernia repair are well established when compared to open laparotomy [3,4,10-12]. The reduction of invasiveness with the laparoscopic approach raises the question of potential benefits for an even more minimally invasive technique. While the SILS technique has already been applied to cholecystectomy, appendectomy, and colectomy, the question remains whether it can reasonably be applied to less common and potentially more complicated laparoscopic procedures. One case reportindicates a successfulrepair of a Morgagni hernia in a pediatric patient via the SILS approach, but there have been no published reportsconcerning SILS Morgagni hernia repair in an adult until now [13].
Surgical techniques have progressed dramatically in the last few decades, and the trend towards the minimization and refinement of laparoscopic techniques continues. It is widely accepted that traditional multi-port laparoscopy has replaced open procedures due to reduced post-operative pain, faster return to daily functioning and fewer complications [9]. As methods develop to advance minimally invasive surgery, SILS has grown in popularity. In addition to increased patient satisfaction relative to cosmetic outcome, recent publications have also indicated possible reduction in post-operative pain, reduced likelihood of infection, and reduced risk of herniation and bleeding [4,10,13,14-16]. While results have been promising, larger studies should be conducted in the form of randomized controlled trials to better support these possible differences.
Disadvantages of a single-incision laparoscopy are mostly due to the learning curve associated with adoption of a new surgical technique. Surgeon difficulty may arise from decreased ease of trocar manipulation in a narrow working space as well as difficulty with triangulation [14-16]. However, there have been recent advances in surgical tools which help the surgeon adapt, such as articulating and reticulating instruments [16]. Though longer operative times have been documented in early SILS studies, many authors acknowledge that few SILS procedures had been conducted prior to study intiation [4,10]. As surgeons continue to pursue proficiency in the technique, they will no doubt overcome the learning curve that may exist with its implementation.
Given the potential advantages of single-incision approach over traditional laparoscopy when performed by an experienced surgeon, the surgeon in this case opted to attempt repair with the use of the single-incision laparoscopic port. Adequate reduction of the hernia, excision of the sac, and placement of mesh over the diaphragmatic defect was accomplished through a 2 cm incision well hidden in the patient�s umbilicus. Additionally, operative length was within the timeframe reported in a small case series of traditional laparoscopic Morgagni hernia repair [3]. The surgery was performed in a reasonable timeframe and with good post-operative and clinical outcomes.
This case report illustrates that the SILS technique may safely be applied to this rare surgical diagnosis. The continuing addition of case studies, retrospective reviews, and prospective trials to the literature has begun to elucidate the benefits of the single port technique. They have also served to highlight several challenges that have slowed universal acceptance. Larger randomized controlled trials may provide more conclusive evidence regarding the benefits and disadvantages of the SILS approach versus traditional laparoscopy for abdominal surgeries. This case serves to illustratethat the single-incision laparoscopic correction of a Morgagni hernia in an adult can be successfully and safely performed by a surgeon experienced in the SILS technique.
References
-
Pfannschmidt J, Hoffmann H, Dienemann H (2004) Morgagni hernia in adults: results in 7 patients. See comment in PubMed Commons below Scand J Surg 93: 77-81.
-
Horton JD1, Hofmann LJ, Hetz SP (2008) Presentation and management of Morgagni hernias in adults: a review of 298 cases. See comment in PubMed Commons below Surg Endosc 22: 1413-1420.
-
Durak EG, Gur S, CokmezA, Atahn K, Zahtz E, et al. (2007) Laparoscopic repair of Morgagni Hernia. Hernia 11:265-270.
-
Markar SR, Karthikesalingam A, Thrumurthy S, Muirhead L, Kinross J, et al. (2012) Single-incision laparoscopic surgery (SILS) vs. conventional multiport cholecystectomy: systematic review and meta-analysis. See comment in PubMed Commons below Surg Endosc 26: 1205-1213.
-
Kim HO, Yoo CH, Lee SR, Son BH, Park YL, et al. (2012) Pain after laparoscopic appendectomy: a comparison of transumbilical single-port and conventional laparoscopic surgery. See comment in PubMed Commons below J Korean Surg Soc 82: 172-178.
-
Udwadia TE (2011) Single-incision laparoscopic surgery: An overview. J Minim Access Surg 7: 1-2.
-
Calland JF, Tanaka K, Foley E, et al. (2001) Outpatient laparoscopic cholecystectomy: patient outcomes after implementation of a clinical pathway. Ann Surg 233:704-715.
-
Shea JA, Berlin JA, Bachwich DR, Staroscik RN, Malet PF, et al. (1998) Indications for and outcomes of cholecystectomy: a comparison of the pre and postlaparoscopic eras. See comment in PubMed Commons below Ann Surg 227: 343-350.
-
Kesieme EB, Kesieme CN (2011) Congenital diaphragmatic hernia: review of current concept in surgical management. See comment in PubMed Commons below ISRN Surg 2011: 974041.
-
St Peter SD, Adibe OO, Juang D, Sharp SW, Garey CL, et al. (2011) Single incision versus standard 3-port laparoscopic appendectomy: a prospective randomized trial. See comment in PubMed Commons below Ann Surg 254: 586-590.
-
Arr�ez-Aybar LA, Gonz�lez-G�mez CC, Torres-Garc�a AJ (2009) Morgagni-Larrey parasternal diaphragmatic hernia in the adult. See comment in PubMed Commons below Rev Esp Enferm Dig 101: 357-366.
-
Pironi D, Palazzini G, Arcieri S, Candioli S, Manigrasso A, et al. (2008) Laparoscopic diagnosis and treatment of diaphragmatic Morgagni hernia. Case report and review of the literature. See comment in PubMed Commons below Ann Ital Chir 79: 29-36.
-
Danielson PD, Chandler NM (2010) Single Port laparoscopic repair of a Morgagni diaphragmatic hernia in a pediatric patient: advancement in single port technology allows effective intracorporeal suturing. J Pediatr Surg 45: E21-E24.
-
Greaves N, Nicholson J (2011) Single incision laparoscopic surgery in general surgery: a review. See comment in PubMed Commons below Ann R Coll Surg Engl 93: 437-440.
-
Tsimoyiannis EC, Tsimogiannis KE, Pappas-Gogos G, et al (2010) Different pain scores in single transumbilical incision laparoscopic cholecystectomy versus classic laparoscopic cholecystectomy: a randomized controlled trial. Surg Endosc 24:1842-1848.
-
Rao PP, Rao PP, Bhagwat S (2011) Single-incision laparoscopic surgery - current status and controversies. See comment in PubMed Commons below J Minim Access Surg 7: 6-16.





