International Journal of Pediatric Research
Subacute Metacarpal Osteomyelitis in a Child
Hamdi Kaziz*, Thabet Mouelhi, Walid Osman, Mohamed Amine Triki, Nader Naouar and Mohamed Laziz Ben Ayeche
Department of Orthopaedics, Sahloul University Hospital, Sousse, Tunisia
*Corresponding author: Hamdi Kaziz, Department of Orthopaedics, Sahloul University Hospital, 57 Salem Gardabbou street, 5020 Jemmel Tunisia, Tel: +21698366196, E-mail: hamdi.kaziz@yahoo.fr, hamdi.kaziz@gmail.com
Int J Pediatr Res, IJPR-1-012, (Volume 1, Issue 2), Case Report; ISSN: 2469-5769
Received: October 06, 2015 | Accepted: December 23, 2015 | Published: December 26, 2015
Citation: Kaziz H, Mouelhi T, Osman W, Triki MA, Naouar N, et al. (2015) Subacute Metacarpal Osteomyelitis in a Child. Int J Pediatr Res 1:012. 10.23937/2469-5769/1510012
Copyright: © 2015 Kaziz H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Subacute osteomyelitis is a rare affection. Clinical presentation is often unclear and can lead to a delay in diagnosis. As a matter of fact, subactue metacarpal osteomyelitis is usually missed at the first time, so that some complications may occur like brachymetacarpia or loss of motion. We report a 10 year-old boy, with a subacute metaphyseal osteomyelitis of the second right metacarpal bone. The radiological features can mimic various benign or malignant bone tumours and non-pyogenic infections. Histological confirmation is necessary to avoid a delay in diagnosis. Treatment was based on antibiotics and surgical debridement. No infectious agent was found in bacteriological exams. At 1 year of follow-up, noncompliance was reported with a normal motion of the finger. X-ray views showed a bone reconstruction with a fibrosis of ulnar part of the metaphysis without length discrepancy.
Keywords
Subacute, Metacarpal, Osteomyelitis, Treatment, Complications
Introduction
Subacute metacarpal osteomyelitis in children is a rare affection. Despite the tropism of the acute form to the metaphyseal of long bones especially in lower limb, subacute form doesn't respect to this concept. It is characterized by a particular pathology of occurrence.
The aim of our case report is to reveal the main features of the subacute metacarpal osteomyelitis in children, review the treatment options and the outcome.
Case Report
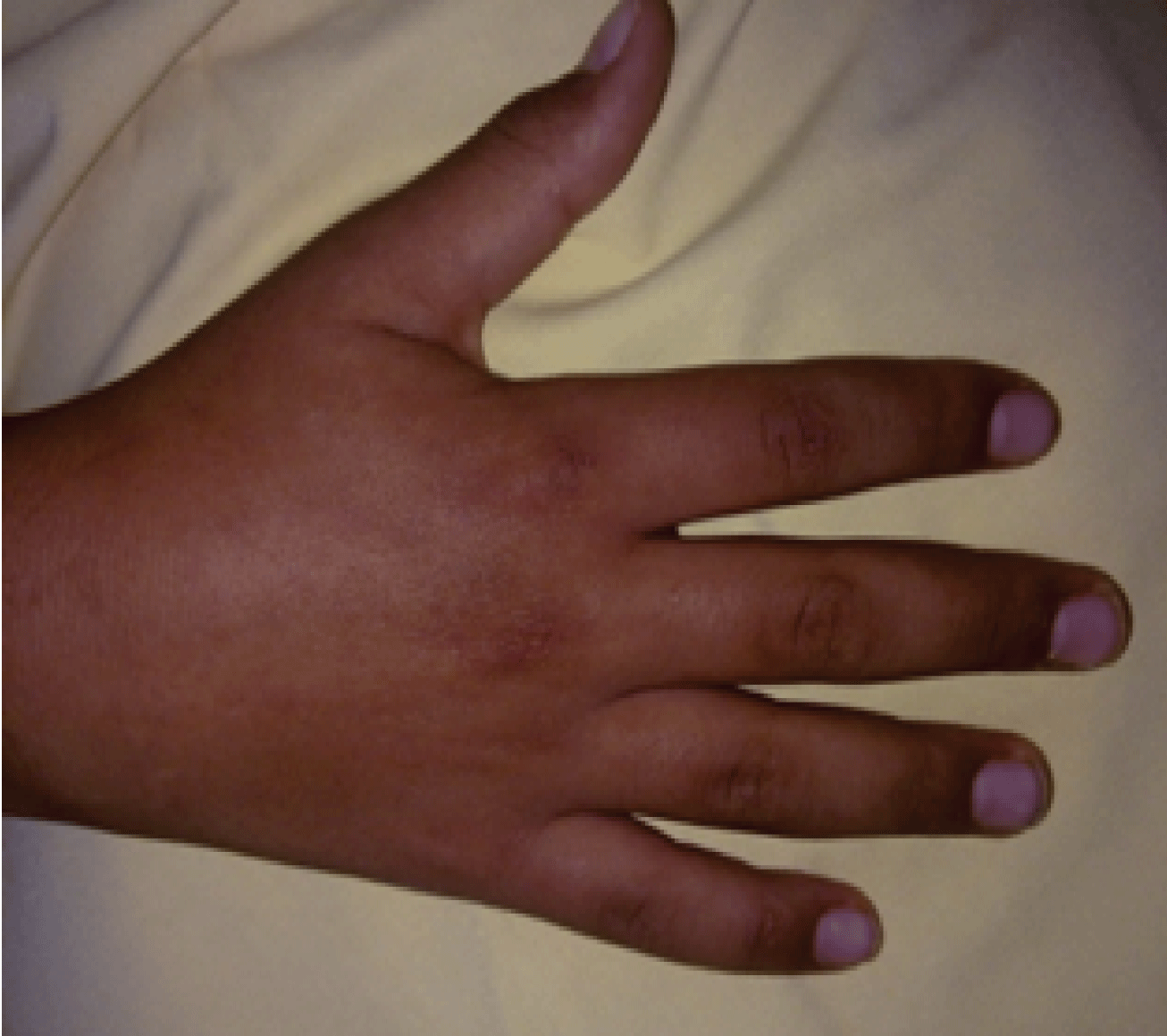
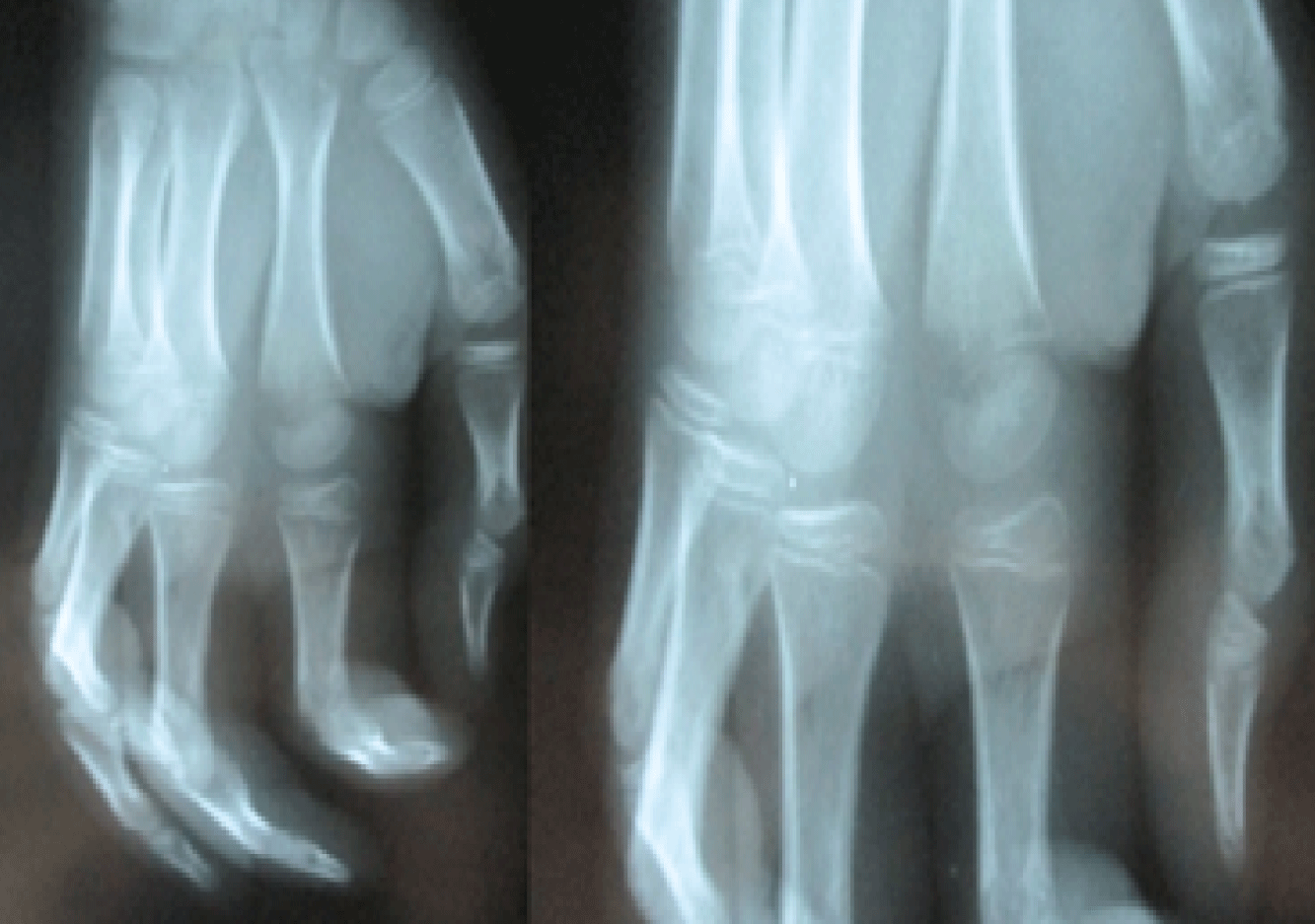
We report a 10 year-old boy, admitted in our department suffering from pain and stiffness of the second metacarpophalangeal joint of his right hand that had been started for two months ago. No fever neither infectious signs were found. Physical examination revealed a little reduction of motion in metacarpophalangeal joint without swelling or injuries signs (Figure 1). Temperature was normal. Lab findings were negative. X-ray views showed a well-defined radiolucent defect in the ulnar part of the metaphysis of the second metacarpal bone associated with a sclerosis in the radial part (Figure 2).
.
Figure 2: X-ray views of the right hand revealing a bone defect on the radial part the metaphysis of the second metacarpal.
View Figure 2
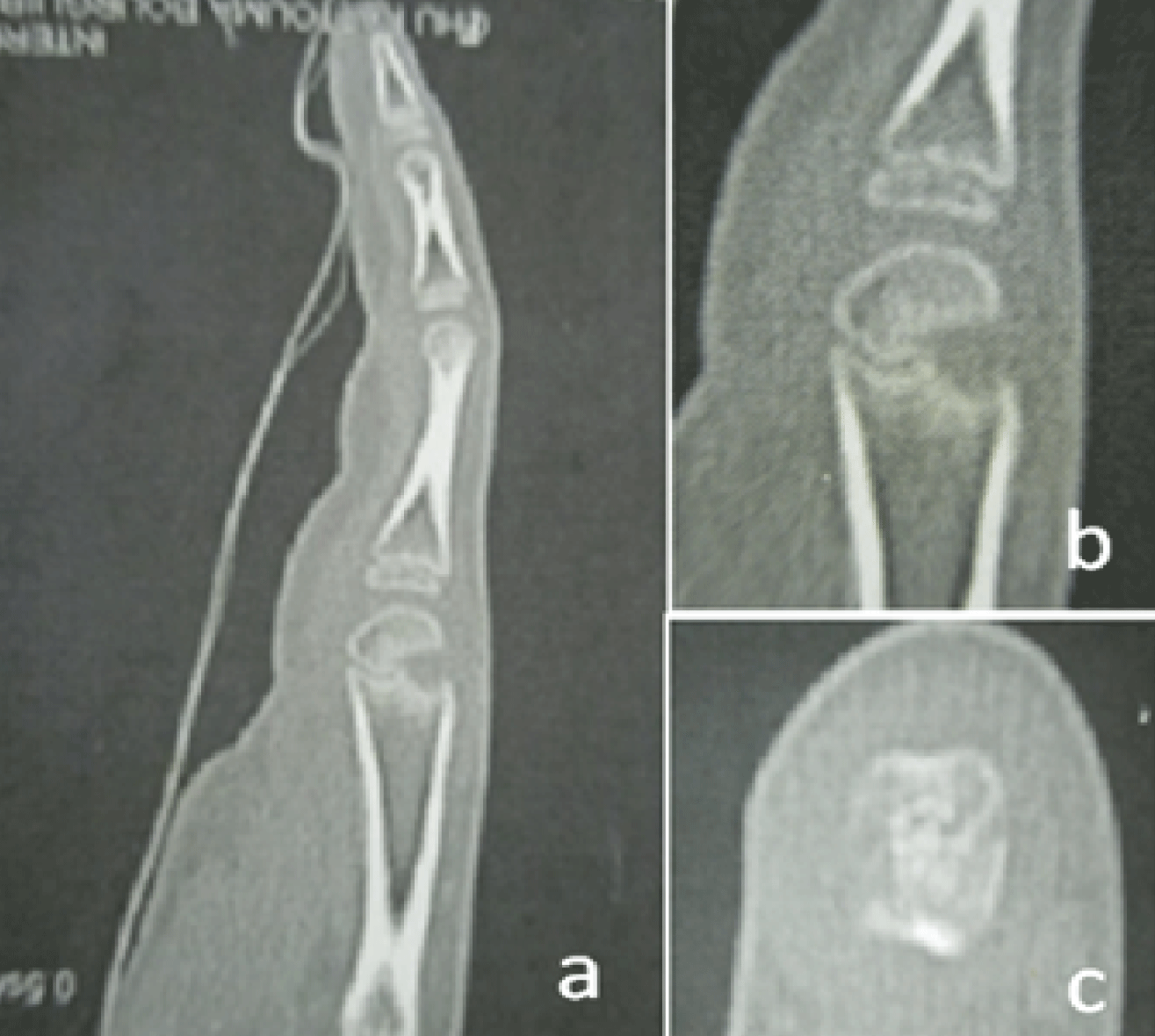
Scan tomography found a radiolucent defect of the metaphyseal part of the carpal bone (Figure 3) advocating an infectious disease. The diagnosis of subacute osteomyelitis was suspected. Hence, intravenous empirical antibiotic therapy based on oxacillin and gantamicin, was started. The daily doses were respectively 1500 mg and 80 mg. Unfortunately, clinical evolution, after 7 days of antibiotic therapy, was unfair with the same stiffness and pain. As a matter of fact, the surgical treatment is advocated and a dorsal approach of the joint was used. Operative exploration found a destruction of both the bone and the metaphyseal cartilage by a local reaction associated to fibrosis and membranous tissues formations without purulent aspect. Surgical debridement of the infected side was undertaken and the hand was immobilized with a plaster splint for 3 weeks. Intravenous antibiotics were continued for one week until results of histological exam which confirmed the infectious origin of the affection without infectious agent in bacteriological findings. Hence, antibiotic therapy based on oxacillin, with a daily dose of 1500 mg, had been continued orally for 3 weeks. During one year of follow, the boy did not report any compliance. The aspect of hand is normal; the second finger regained 260° of total range of motion (TAM) without deformity and abnormalities. The last x-ray views showed a bone reconstruction with a fibrosis of ulnar part of metaphysic (Figure 4).
.
Figure 3: Tomography scan of the finger: a,b: sagittal views of the finger showing the bone defect, c: transverse axial view revealing the defect on the radial part of the metaphysic.
View Figure 3
.
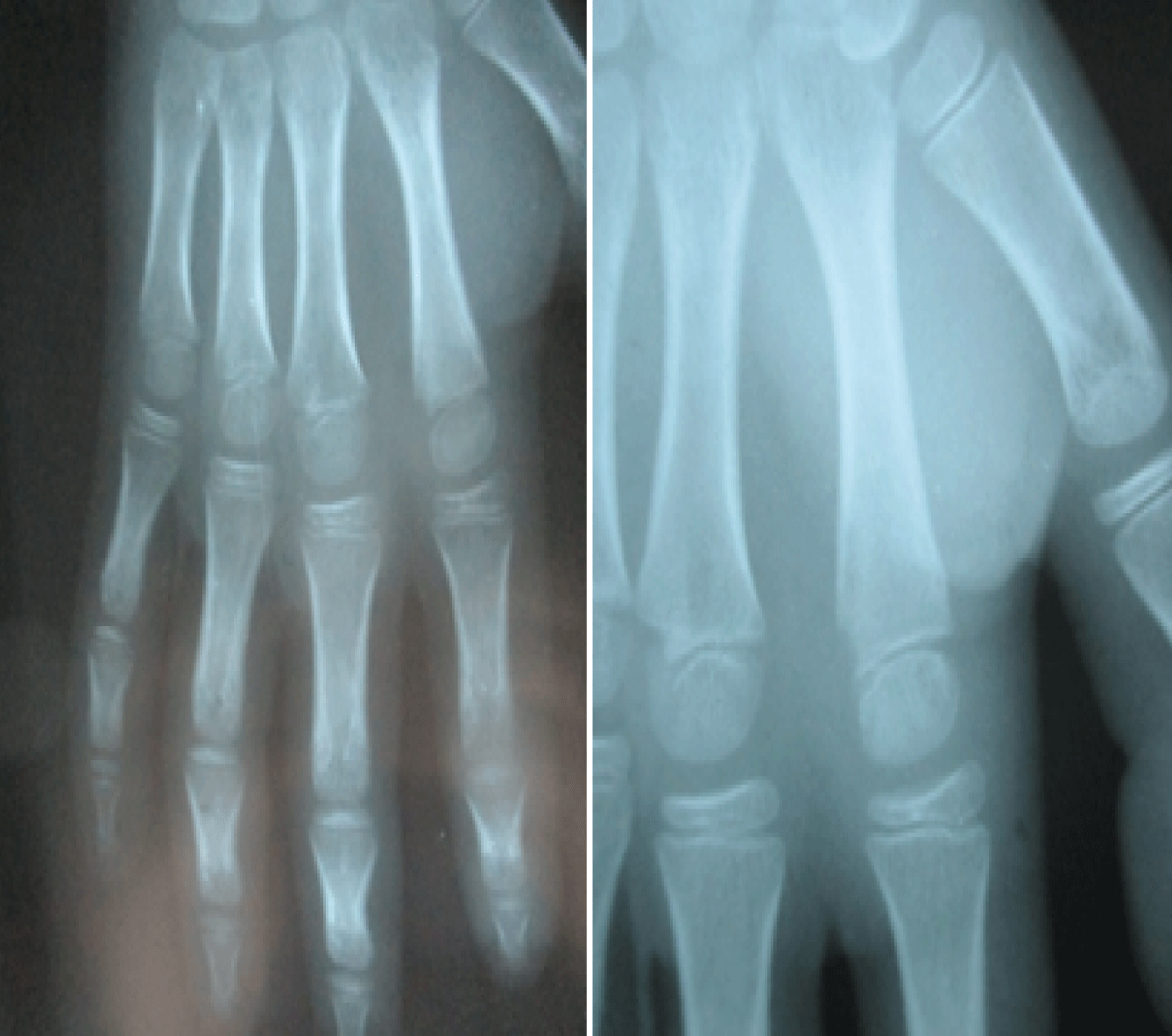
Figure 4: The last X-ray views of the right hand obtained after one year from surgical debridement with a bone reconstruction and a little fibrosis in the infection site.
View Figure 4
Discussion
Subacute metacarpal osteomyelitis in children is a scarce disease [1]. A few published cases were about the acute form [2,3]. Although, the primary acute haematogenous osteomyelitis in childhood is commonly localized in the metaphysis of long bone, subacute form doesn't have the same characteristics and can affect diaphysis [4]. The most affected metaphysis in subacute osteomyelitis is the tibia [4]. Metaphyseal localization in the hand bones are possible but have never been described. Several studies showed that subacute osteomyelitis occurs each time there is a decreased bacterial virulence and an increased host resistance [5-7]. Moreover, early antibiotic therapy in acute form seems to have a rule in occurrence of subacute form since it decreases the virulence of infectious agents [4,5]. Subacute metacarpal osteomyelitis may occur in metaphysis but also in both diaphysis and epiphysis and can be described in radiological findings according to Roberts's classification [7]. The main difficulty in the management of subacute metacarpal osteomyelitis is making the diagnosis [8]. In this form, physical examination doesn't reveal abnormalities and a little reduction of motion and a mild pain are often seen without any systemic manifestations, so that the infectious origin is usually missed at the first examination [7,8]. In spite of the benignity of this affection, other benign and malignant affections must be advocated in the differential diagnosis, including eosinophilic granuloma, osteoid osteoma, chondroblastoma, tuberculosis, fungal infection, osteosarcoma, Ewing's sarcoma, leukaemia and round cell tumours [9-11]. Actually, studies of the subacute osteomyelitis showed the important value of MRI in diagnosing osteomyelitis in children also pointing to gadolinium-enhanced imaging as the most sensitive [4,12,13]. MRI exploration helps to localize the affection of the bone and provide an objective control of the lesion extent [10,14]. However, X-ray views may underestimate the bone destruction and remain normal until the step of irreversible progression of the infection [15,16].
Treatment of this affection is controversial [17]. The recommended treatment for subacute osteomyelitis with a lucent lesion or nidus has been curettage, biopsy and culture followed by immobilization and antibiotics [7,10,17]. In diaphyseal lesions with a periosteal reaction a core of bone should be taken which includes periosteum, cortex and medullary contents [18]. The diagnosis is usually confirmed by histological examination which shows an inflammatory component with scattered lymphocytes, plasma cells and granulation tissue [11,17,18]. Staphylococcus aureus is regarded as the causative organism by most authors. It is, however, difficult to identify. [17-19]. Several studies concluded that antibiotics alone may be adequate and surgery should be reserved for "aggressive lesions" and those which do not respond to antibiotics [18,19]. Cloxacillin is the antibiotic of choice in the treatment of subacute osteomyelitis and is given orally for six weeks after an initial intravenous course for up to five days [19]. Subacute metaphyseal osteomyelitis has been shown to disturb the growth plate and compromise the joint [19,20].
In our case report, subacute osteomyelitis of metacarpal bone had been showed to have a satisfied functional and radiological outcomes comparing to the other forms of infectious bone diseases. Antibiotic therapy indicated for five weeks with only two weeks of intravenous treatment seems to be curative and enough.
It is important to re-emphasize that subacute form is a clinical entity which is distinct from the acute form and from those types in which the clinical presentation has been modified by the administration of antibiotics. These lesions are frequently confused with a variety of benign and malignant bone tumours and non-pyogenic infections.
Acknowledgment
We, authors of these papers certify that there is no conflict of interest.
References
-
Rasool MN (2001) Primary subacute haematogenous osteomyelitis in children. J Bone Joint Surg Br 83: 93-98.
-
Keret D, Giladi M, Kletter Y, Wientroub S (1998) Cat-scratch disease osteomyelitis from a dog scratch. J Bone Joint Surg Br 80: 766-767.
-
Aebi C, Ramilo O (1998) Metacarpal osteomyelitis complicating varicella-associated cellulitis of the hand: report of 2 cases. Scand J Infect Dis 30: 306-309.
-
Hempfing A, Placzek R, Gottsche T, Meiss AL (2003) Primary subacute epiphyseal and metaphyseal osteomyelitis in children. Diagnosis and treatment guided by MRI. J Bone Joint Surg Br 85: 559-564.
-
Mhuircheartaigh JN, Lin YC, Wu JS (2014) Bone tumor mimickers: A pictorial essay. Indian J Radiol Imaging 24: 225-236.
-
Shekhar A, Korlhalli S, Murgod G (2015) Ewing's sarcoma of proximal phalanx of the hand with skip metastases to metacarpals. Indian J Orthop 49: 365-368.
-
Ezra E, Wientroub S (1997) Primary subacute haematogenous osteomyelitis of the tarsal bones in children. J Bone Joint Surg Br 79: 983-986.
-
Macnicol M (2001) Patterns of musculoskeletal infection in childhood. J Bone Joint Surg Br 83: 1-2.
-
Cottias P, Tomeno B, Anract P, Vinh TS, Forest M (1997) Subacute osteomyelitis presenting as a bone tumour. A review of 21 cases. Int Orthop 21: 243-248.
-
Calhoun JH, Manring MM, Shirtliff M (2009) Osteomyelitis of the long bones. Semin Plast Surg 23: 59-72.
-
Chow LT, Wong SK (2014) Primary osseous inflammatory malignant fibrous histiocytoma masquerading as chronic osteomyelitis. Orthopedics 37: 940-945.
-
Merlini L, Anooshiravani M, Ceroni D (2015) Concomitant septic arthritis and osteomyelitis of the hip in young children; a new pathophysiological hypothesis suggested by MRI enhancement pattern. BMC Med Imaging 15: 17.
-
von Kalle T, Heim N, Hospach T, Langendörfer M, Winkler P, et al. (2013) Typical patterns of bone involvement in whole-body MRI of patients with chronic recurrent multifocal osteomyelitis (CRMO). Rofo 185: 655-661.
-
Howe BM, Wenger DE, Mandrekar J, Collins MS (2013) T1-weighted MRI imaging features of pathologically proven non-pedal osteomyelitis. Acad Radiol 20: 108-114.
-
Godley DR (2015) Managing musculoskeletal infections in children in the era of increasing bacterial resistance. JAAPA 28: 24-29.
-
Bires AM, Kerr B, George L (2015) Osteomyelitis: an overview of imaging modalities. Crit Care Nurs Q 38: 154-164.
-
Ceroni D, Belaieff W, Cherkaoui A, Lascombes P, Schrenzel J, et al. (2014) Primary epiphyseal or apophyseal subacute osteomyelitis in the pediatric population: a report of fourteen cases and a systematic review of the literature. J Bone Joint Surg Am 96: 1570-1575.
-
Dartnell J, Ramachandran M, Katchburian M (2012) Haematogenous acute and subacute paediatric osteomyelitis: a systematic review of the literature. J Bone Joint Surg Br 94: 584-595.
-
Shah TT, Chin KF, Noorani A, Nairn D (2012) Subacute physeal abscess: case report to illustrate treatment with a minimally invasive incision and drainage technique. Ann R Coll Surg Engl 94: 51-54.
-
Lietzau M, Rehage J, Heppelmann M (2015) Therapeutic procedure of a complicated septic epiphyseal osteomyelitis in a heifer. A case report. Tierarztl Prax Ausg G Grosstiere Nutztiere 43: 159-164.