International Journal of Pediatric Research
Clitoral Hair Tourniquet: A Case Report and Review of the Literature
Lindsey N Zimmerman1* and Amy J Wagner2
1Department of Surgery, Medical College of Wisconsin, USA
2Division of Pediatric Surgery, Children's Hospital of Wisconsin; Department of Surgery, Medical College of Wisconsin, USA
*Corresponding author: Lindsey Zimmerman, Department of Surgery, Medical College of Wisconsin, 9200 W. Wisconsin Avenue, Suite 3510, Milwaukee, WI 53226, USA, E-mail: Lindsey.n.zimmerman@gmail.com
Int J Pediatr Res, IJPR-1-007, (Volume 1, Issue 2), Case Report; ISSN: 2469-5769
Received: June 03, 2015 | Accepted: October 07, 2015 | Published: October 10, 2015
Citation: Zimmerman LN, Wagner AJ (2015) Clitoral Hair Tourniquet: A Case Report and Review of the Literature. Int J Pediatr Res 1:007. 10.23937/2469-5769/1510007
Copyright: © 2015 Zimmerman LN, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Hair tourniquets are uncommon occurrences in children that can have devastating consequences. They tend to be found on fingers and toes, but have also been reported to involve the genitalia. We present a case of a hair tourniquet involving the clitoris of a child. A high index of suspicion is necessary in order to facilitate early diagnosis and treatment.
Keywords
Clitoris, Hair, Tourniquet, Genitalia
Introduction
Hair or thread tourniquets are an uncommon occurrence and typically occur in children. Hair tourniquet syndrome is a phenomenon originally described in 1612 by Guillemeau with the first published case report being in 1832 in The Lancet [1-4]. The most common sites of occurrence are toes and fingers; genitals have been also involved, more commonly the penis than female external genitalia [2,5,6]. Given complications that can arise, it is important for physicians to be aware of this process and to conduct a thorough history and physical examination when a patient presents with pain, irritability or abnormal gait.
Case
A five-year-old girl presented to the emergency department (ED) with swelling overlying her clitoris. The mother noted a "pimple" near the child's genitalia, and upon closer inspection the mother found and removed a hair. Following this, the area became painful and swollen. She presented to her pediatrician who referred her to the ED due to concern for a hair tourniquet. The area was difficult to examine given the patient's pain and anxiety, but it was noted that there was a 0.5 cm red nodule near her clitoris.
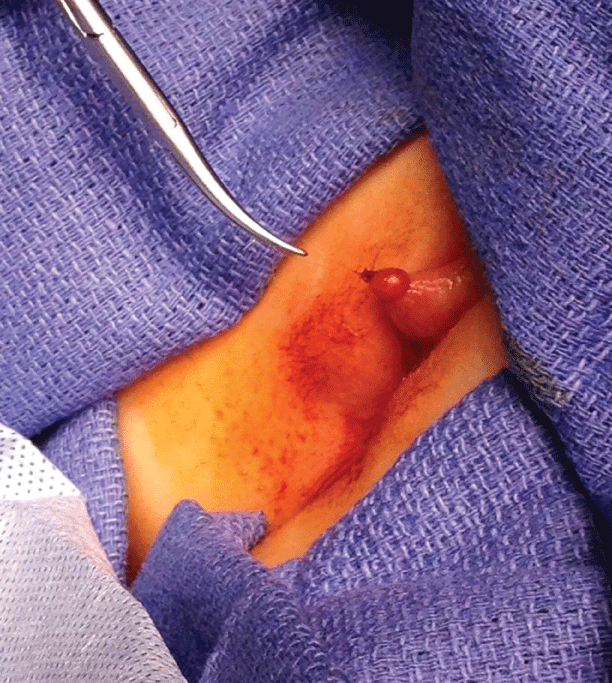
Due to the history obtained and concern for hair tourniquet, the patient was taken to the operating room for examination under anesthesia and removal (Figure 1). Upon closer inspection, the clitoris was edematous and a hair tourniquet, which was the same color and texture as the child's hair, was present on the distal aspect. Her genitalia were otherwise normal with good hygiene. It was removed and the patient had an uncomplicated postoperative course.
Discussion
Presentation
Hair tourniquets tend to occur in young children, but can also occur in older patients. When digits are involved, patients typically range from a few days to two years of age [5-9]. Cases in the literature involving genitalia tend to occur in older ages; male genitalia cases range from four months to six years of age [2,5,7-9]. Cases involving female genitalia, including labia majora, labia minora, and clitoris can extend into adolescent ages [3,6,10]. The median age of hair tourniquet of the clitoris is eight years [1,6]; however, there is a single case report as young as four years of age [11].
Parents tend to bring children in with complaints of pain or occasionally swelling, although the only symptom may be irritability. Symptoms may be subtle, such as decreased use of a hand with an affected digit or a wide-based gait when the tourniquet is present in the genital area [12]. On physical examination, the distal area to the tourniquet is erythematous and edematous. It is possible for the hair or thread causing the syndrome to be obscured; this can be due to the surrounding soft tissue edema or even reepithelialization of the overlying skin [4,13-15]. If constriction with surrounding edema is noted, exploration is warranted even if a foreign body cannot be visualized [9,14]. Other etiologies for these findings should also be considered. The differential diagnosis of hair tourniquet also includes infection, dermatitis, insect bites, ainhum, trauma, and sexual abuse [4,5,7,12,13]. In infants, one must also consider congenital amniotic band syndrome [4] or congenital adrenal hyperplasia if clitoromegaly is present. As patients are older and develop pubic hair, one should also consider folliculitis.
Treatment
The offending hair or thread needs to be removed as soon as possible in order to prevent serious complications, including necrosis or autoamputation [2,3,10,13]. The fiber can be removed by manual unwrapping or excision with a scissors or scalpel. Using a depilatory cream has been described, but this is only an option if a hair is the cause and not a thread or other foreign fiber; it also should not be used in close proximity to mucus membranes [16,17]. It is important to be sure to remove the entire tourniquet in order to prevent chronic or recurrent symptoms [10,15].
Pathophysiology
The mechanism of injury begins with lymphatic occlusion, which causes impaired venous drainage; the subsequent edema then leads to obstruction of arterial flow and necrosis [2-4,6,15]. Hair is the ideal fiber to cause these symptoms due to its inherent properties. It stretches when wet and then constricts as it dries [3]. The high tensile strength allows it to remain secure and causes difficulty in removal [3,8,13].
Etiology
The etiology of the hair must be carefully considered as intentional application for cultural beliefs or child abuse has been associated in addition to inadvertent or accidental hair tourniquets [6,11,13]. This reiterates the need for a thorough history and physical examination. In our case, there was no suspicion of abuse.
Hair tourniquets have also been suggested to be associated with telogen effluvium, when mothers have increased hair shedding for 2-6 months postpartum. During this time, there is a higher risk of hair tourniquets to the child [12]. This was not the timeframe in for the patient presented, but must be considered for others.
Conclusion
Our patient is at the low end of age range that has presented in the literature with a clitoral hair tourniquet [1,11,13]. Although a hair was unable to be seen on initial physical examination, an exam under anesthesia was warranted for further evaluation and treatment. This shows the importance of maintaining a high index of suspicion when patients present in unexplained distress. Clinicians need to be aware of hair tourniquets and the uncommon presentations they can have, in both a variety of ages and locations. This highlights the importance of a thorough physical exam in order to evaluate for this potentially serious condition.
Ethical Statement
Informed consent for photo documentation was obtained prior to the procedure. Per local Institutional Review Board policy, no review or research consent is required for describing single case reports.
Conflict of Interest
The authors declare that there is no conflict of interest.
References
-
Golshevsky J, Chuen J, Tung PH (2005) Hair-thread tourniquet syndrome. J Paediatr Child Health 41: 154-155.
-
Hussain HM (2008) A hair tourniquet resulting in strangulation and amputation of penis: case report and literature review. J Paediatr Child Health 44: 606-607.
-
Kuo JH, Smith LM, Berkowitz CD (2002) A hair tourniquet resulting in strangulation and amputation of the clitoris. Obstet Gynecol 99: 939-941.
-
Barton DJ, Sloan GM, Nichter LS, Reinisch JF (1988) Hair-thread tourniquet syndrome. Pediatrics 82: 925-928.
-
Bacon JL, Burgis JT (2005) Hair thread tourniquet syndrome in adolescents: a presentation and review of the literature. J Pediatr Adolesc Gynecol 18: 155-156.
-
Mat Saad AZ, Purcell E, McCann JJ (2006) Hair-thread tourniquet syndrome in an infant with bony erosion. Ann Plast Surg 57: 447-452.
-
Alpert JJ, Filler R, Glaser HH (1965) Strangulation of an appendage by hair wrapping. N Engl J Med 273: 866-867.
-
Garcia-Mata S, Hidalgo-Ovejero A (2009) Hair tourniquet syndrome of the toe: report of 2 new cases. J Pediatr Orthop 29: 860-864.
-
Kerry RL, Chapman DD (1973) Strangulation of appendages by hair and thread. J Pediatr Surg 8: 23-27.
-
Dua A, Jamshidi R, Lal DR (2013) Labial hair tourniquet: unusual complication of an unrepaired genital laceration. Pediatr Emerg Care 29: 829-830.
-
Serour F, Gorenstein A, Dan M (2007) Tourniquet syndrome of the clitoris in a 4-year-old girl. J Emerg Med 33: 283-284.
-
Sivathasan N, Vijayarajan (2012) Hair-thread tourniquet syndrome: a case report and literature review. Case Rep Med 2012: 171368.
-
Rich MA, Keating MA (1999) Hair tourniquet syndrome of the clitoris. J Urol 162: 190-191.
-
Alvarez-Perez A, Mateo S, Fernandez-Redondo V, Toribio J (2013) Hair-thread tourniquet syndrome: a hidden hazard. Pediatr Dermatol 30: 61-62.
-
Sylwestrzak MS, Fischer BF, Fischer H (2000) Recurrent clitoral tourniquet syndrome. Pediatrics 105: 866-867.
-
O'Gorman A, Ratnapalan S (2011) Hair tourniquet management. Pediatr Emerg Care 27: 203-204.
-
Bean JF, Hebal F, Hunter CJ (2015) A single center retrospective review of hair tourniquet syndrome and a proposed treatment algorithm. J Pediatr Surg 50: 1583-1585.