International Journal of Pediatric Research
Topic: Acute Kidney Injury in Children: 3-Year Data Review from Ghana
Sampson Antwi1,2*, Anima Sarfo2, Abigail Amoah2, Anna Serwaa Appia2 and Esther Obeng2
1School of Medical Sciences, Kwame Nkrumah University of Science and Technology, Ghana
2Komfo Anokye Teaching Hospital, Ghana
*Corresponding author: Sampson Antwi, School of Medical Sciences, Kwame Nkrumah University of Science and Technology, Komfo Anokye Teaching Hospital, Ghana, Tel: +233-206300455, E-mail: kantwisampson@gmail.com
Int J Pediatr Res, IJPR-1-005, (Volume 1, Issue 2), Research Article; ISSN: 2469-5769
Received: August 16, 2015 | Accepted: September 10, 2015 | Published: September 14, 2015
Citation: Antwi S, Sarfo A, Amoah A, Appia AS, Obeng E (2015) Topic: Acute Kidney Injury in Children: 3-Year Data Review from Ghana. Int J Pediatr Res 1:005. 10.23937/2469-5769/1510005
Copyright: © 2015 Antwi S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background/Aims: Acute kidney injury (AKI) is a relatively common condition encountered in everyday paediatric practice. It remains a significant contributor to preventable deaths especially in resource constraint regions of the world largely due to lack of dialysis services.
This 3-year data analysis (2010-2012) was undertaken to determine the aetiology and treatment/mortality outcomes of children with AKI presenting to a Teaching Hospital in Ghana. AKI was defined in this analysis by the RIFLE and KDIGO criteria.
Results: Two hundred and six (206) cases of AKI were recorded over the period out of a total of 664 renal cases.
Haemoglobinuria, obstructive uropathy and tumour infiltration of the kidneys were the leading causes of AKI (37.8%). 9.2% of cases were diarrhoeal-related with glomerulonephritides occurring in 12.1% of cases.
Seventy-one (34.5%) of the 206 AKI cases required dialysis which could only be provided for 25 (35.2%), 16 (64%) of whom survived.
Forty three (20.9%) children died, while 144 (69.9%) survived. Thirty-one (72%) of the patients who died needed dialysis.
Conclusion: In comparison to previous studies across the world, there is huge burden of AKI among hospitalized children in Kumasi, Ghana.
Haemoglobinuria and tumour-related conditions accounted for most cases of AKI more than diarrhoea-associated conditions and postinfectious glomerulonephritis as were previously reported or postulated.
Most AKI deaths were related to lack of dialysis service. In view of the less technical requirements compared with other modalities of renal replacement therapy, peritoneal dialysis should be promoted across Africa to curtail needless deaths from AKI.
Introduction
Acute Kidney Injury (AKI) is any sudden decline in glomerular filtration rate (GFR) expressed clinically as retention of nitrogenous waste products notably urea and creatinine in the blood with or without corresponding reduction in urine output [1]. Kidney Disease Improving Global Outcomes (KDIGO) and RIFLE define AKI as any change in serum creatinine of more than 50% from a baseline value over a period of 48 hours to 7 days and/or urine output of less than 0.5 ml/kg/hour over any period more than 6 hours or a change in absolute creatinine value of 26.5 μmol/l [2,3].
Aetiology of AKI varies widely according to age, geographical region, and clinical setting [4]. Whereas most cases of childhood AKI in developed countries results from severe illness associated with intensive Care setting and haemolytic uraemic syndrome among others, in developing countries, infection-related causes are often cited as the predominant causes particularly gastroenteritis commonly associated with poor sanitation and lack of safe drinking water, and post streptococcal glomerulonephritis [5,6]. AKI remains a significant contributor to the mortality of critically ill children [7]. Mortality outcomes depend on such factors as aetiology, medical setting, co-morbidities, and availability of dialysis therapy [1].
Despite the abundant data on AKI in the literature, only few are from Africa. This data analysis was undertaken to determine the aetiology and treatment/mortality outcomes of children with AKI presenting to a Teaching Hospital in Ghana.
Methodology
This study was a retrospective analysis of all cases of AKI admitted to the paediatric nephrology unit of Komfo Anokye Teaching Hospital (KATH), Ghana, from January 2010 to December 2012 to determine the aetiology and treatment outcomes. KATH is the second largest Teaching Hospital in Ghana, a 1,000-bedded located in the second largest city, Kumasi, in the middle of Ghana. It receives referrals from the middle and northern half of Ghana and part of the southern half. The paediatric department has 11 subspecialist units and attends to children from birth to 13 years. The paediatric nephrology unit was re-organized with guidelines and protocols in 2010 after receiving a paediatric nephrologist. All children admitted to the nephrology unit are entered into a database.
AKI was defined in this analysis by the pRIFLE criteria as urine output of < 0.5 ml/kg/hour over 8 hours or an increase in serum creatinine of at least 50% from a baseline value within seven days [3].
Treatment of AKI was largely conservative with strict fluid management and diuretics till 2012 when peritoneal dialysis (using manual exchanges) was established as renal replacement therapy modality for AKI. Dialysis for AKI is covered by a National Health Insurance Scheme.
Results
Demographics/Prevalence
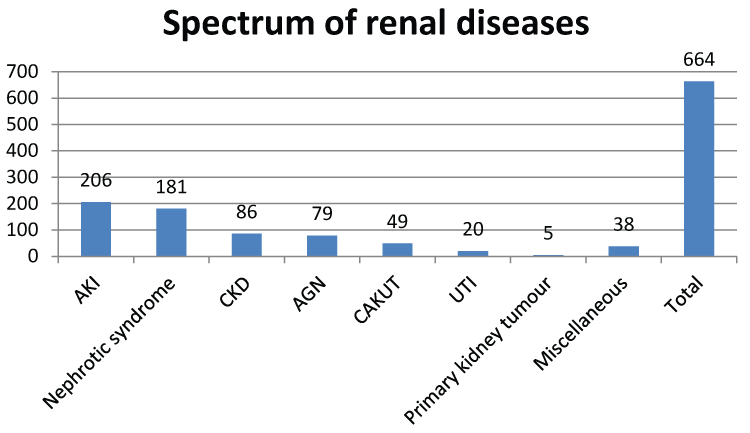
Two hundred and six (206) cases of AKI were recorded over the period out of a total of 664 renal cases. There were 117 (56.8) males. Age range was from 1 day to 13 years (median 5yr 3mo). There were a total of 15, 371 paediatric admissions over the period, giving an AKI prevalence of 1.3%. But among all children with renal diseases admitted over the period, AKI was the commonest presentation (206 of 664 cases, [31%]). Figure 1 summarizes the incidence of all renal diseases recorded over the period.
.
Figure 1: Spectrum of renal diseases recorded over the period of 3 years (2010-2012).
AKI-Acute Kidney Injury, CKD-Chronic Kidney Disease, AGN-Acute Glomerulonephritis, CAKUT-Congenital Anomaly of Kidney and Urinary Tract, UTI-Urinary Tract Infection
View Figure 1
Aetiology/Clinical setting associated with AKI
Primary renal diseases accounted for 38 (18.4%) of all cases of AKI with glomerulonephritides (AGN and nephrotic syndrome) occurring in 25 (12.1%) of cases (Table 1).
![]()
Table 1: Clinical Settings associated with AKI in children
View Table 1
On the contrary, haemoglobinuria from different aetiologies (Table 1), obstructive uropathy (mostly from intra-abdominal tumour) and Burkitt lymphoma of the kidneys were the leading clinical settings associated with AKI. The three conditions accounted for more than a third (37.8%) of all cases of AKI. 9.2% of cases were gastroenteritis-related. Less common clinical settings associated with AKI included HUS (6 cases, [2.9%]), pneumonia with hypoxaemia (5 cases, [2.4%]), bacteria endocarditis and snake bite (2 cases each, [1.0%]). No case of contrast induced AKI was recorded in this analysis.
Dialysis requirement outcomes
One hundred and forty one (68.4%) of the 206 cases of AKI were recorded from 2010-2011, an era when dialysis were not routinely available for children in the hospital. As a result, only 4 of 46 cases that needed dialysis during that period could be dialyzed using chest tube and self constituted dialysis solution as "improvised" peritoneal dialysis 3 (75%) of whom survived. One other child had a session of haemodialysis at the adult haemodialysis unit but died soon after from haemopericardium. Of the remaining 41 cases of AKI in need of dialysis who could not be dialyzed, 31 (75.6%) died but 10 (24.4%) survived on conservative management with strict fluid restriction, high dose frusemide infusion, and aggressive management of hyperkalaemia with salbutamol and kayexalate.
Sixty-five cases of AKI were recorded in 2012. Following the encouraging outcome of the "improvised" peritoneal dialysis in the late 2011, peritoneal dialysis using manual exchanges became available as renal replacement therapy for children with AKI at our center. In that third year (2012), 20 children with AKI out of 25 in need of dialysis received peritoneal dialysis 13 (65%) of whom survived. The remaining 5 who could not be dialyzed were either deemed unstable or had other contraindications to the procedure.
Altogether, 25 cases of our AKI cases had dialysis done on them of whom 16 (64%) survived. The indications for dialysis are summarized in Table 2
![]()
Table 2: Indications for Dialysis
View Table 2
Mortality outcomes
Altogether, 43 (20.9%) out of 206 patients with AKI died, 144 (69.9%) survived. The outcomes of 19 cases (9.2%) were not documented. They might have died, transferred to other units or absconded (i.e. sneaked out of the ward to avoid paying one's hospital bill-a phenomenon common in this part of the world).
Causes of Death
The causes of death for the 43 patients are summarized in Table 3.
![]()
Table 3: Causes of Death among AKI patients
View Table 3
Discussion
The pattern of AKI in this study is at variance with earlier report from the West African subregion [5] and opinion of authors [6] regarding the aetiology of AKI. These Authors reported gastroenteritis and glomerulonephritides as leading clinical settings associated with AKI. It is however in agreement with other studies also from the West African subregion that found low prevalence of gastroenteritis-related AKI [8,9].
In consonance with several other studies from the continent [10-14], haemoglobinuria was identified as the leading clinical setting associated with AKI with obstructive uropathy and tumour infiltration of the kidneys being second and third commonest associated clinical settings. Regarding lymphoma and AKI, another West African study found renal Burkitt lymphoma to account for nearly half (47.2%) of all cases [9].
Haemoglobinuria, extrinsic ureteral obstruction from tumour mass as well as direct tumour infiltration of the kidneys (predominatly from Burkitt lymphoma) are documented clinical settings associated with AKI [1,4,8-11]. Ghana lies in the lymphoma belt of Africa and abdominal Burkitt lymphoma is a common oncologic presentation in children. The kidneys may be primary site for this tumour or the ureters may be compressed by the tumour mass leading to post-renal AKI.
Haemoglobinuria, the passage of free haemoglobin in the urine as opposed to passage of intact red cells (haematuria), often results from intravascular haemolysis from both infectious and non-infectious aetiologies. Originally described as black water fever in association with malaria infection and anti-malarial therapy [10,11], the pathogenesis of haemoglobin-induced pigment nephropathy is complex and may be related to the following: [15,16].
1. Renal vasoconstriction from exhaustive scavenging of nitric oxide and stimulation of endothelin production by haem protein.
2. Direct cytotoxic effect of haem protein on renal tubular epithelial cells. 3. Precipitation of the haem pigment in the tubular lumen.
Haemoglobinuria related AKI might have been overlooked in the past since urine output is often maintained in this form of nephropathy [13,17]. Thus, short of serum urea and creatinine determination, an investigation that is often unavailable in many health facilities in Africa, this form of AKI may escape detection. Most cases of haemoglobinuria reported in the literature were associated with falciparum malaria (black water fever) in conjunction with antimalarial therapy notably quinine among expatriates [10,11]. In this analysis however, the causes of haemoglobinuria could not be determined in more than half of cases. Malaria (7cases), Glucose-6-phosphate dehydrogenase deficiency (5 cases) and sickle cell diseases (3 cases) accounted for the known causes. Table 1
Haemolytic uraemic syndrome, a leading cause of AKI in developed world, was recorded in only 6 (2.9%) cases similar to the 3.3% recorded in another study in West Africa and affirms the long held view that HUS is uncommon in West Africa [4]. Haemolytic uraemic syndrome has however been reported as leading cause of AKI in other parts of Africa mainly in South and Eastern Africa [18,19].
From the foregoing reports, it is clear that there is wide variation regarding the aetiology of AKI in children across different regions of the same continent. Across continents, the aetiological variation of childhood AKI is even greater as summarised in Table 4 below. No case of AKI was recorded among paediatric patients who underwent cardiac surgeries by a visiting Cardiac team; an observation that is at variance with several reports [20-23]. This may largely be due to the skewedness of case selection towards non-complex cardiac cases for these operations in our center.
![]()
Table 4: Clinical settings associated with AKI across geographical regions/continents.
View Table 4
This 3-year analysis, in comparison to other studies [8,9,11,12,14] (also table 4), revealed a huge burden of AKI among hospitalized children in Kumasi recording 206 cases in 3 years. This observation could be due to number of factors: Firstly, the return of a paediatric nephrologist to the unit in 2009 heightened AKI awareness in the unit. Secondly, there has been improvement in case identification of AKI following the introduction of the RIFLE/KDIGO criteria. Thirdly, the center where this study was done is strategically located in Ghana. It serves the whole of the middle and northern part of Ghana and, having one of the only two paediatric nephrologists in a country of 25 million people, it receives referrals from far and near especially after the introduction of dialysis services for children. Fourthly, it may underline the huge burden of AKI in this region of Ghana.
The relatively low prevalence of gastroenteritis as a contributing factor to AKI in this Ghanaian study may be due to the ready availability and widespread use of oral rehydration salt for home treatment of diarrhoeal diseases in Ghana and the modest gain in the economy since the advent of sustained democratic governance.
Most cases of AKI (135, [65.5%]) did not need dialysis and responded well to conservative management. Insertion of nephrostomy tube was life saving intervention for most cases of obstructive uropathy from ureteral compression by abdominal tumour or nephrolithiasis. Lasix infusion (0.25 -1 mg/kg/hr) with or without aminophylline (up to 1 mg/kg q6hrly) equally proved useful conservative treatment method by converting most oliguric AKIs to non-oliguric AKIs and thus prevented complications like pulmonary oedema. Hyperkalaemia was successfully managed with salbutamol nebulisation in most cases sometimes with polysterene sodium (kayexalate).
Thirty-one (72%) of the 43 cases of AKI that died needed dialysis that was non-existent then. Following the introduction of regular dialysis service, case fatality of those in need of dialysis reduced significantly to 36% (9 out of 25 cases).
Conclusion
There is a huge burden of AKI among hospitalised children in Kumasi, Ghana, due in part to improved case detection by the RIFLE/KDIGO criteria and the strategic location of Kumasi. Haemoglobinuria, ureteric compression from abdominal lymphoma and direct tumour infiltration of the kidneys were the predominant clinical settings associated with AKI as previously reported, accounting for more than a third (37.8%) of all cases. Primary renal disease and diarrhoeal-related conditions accounted for just a little over a quarter (27.7%) of all cases of AKI in contrast to long held opinion of their predominance as causes of AKI in developing countries. The findings from this study confirm the observation that the aetiology of AKI may be geographically dependent. It may also point to changing trends in the aetiology of AKI among children in Africa.
Most cases (65.5%) of AKI did not need dialysis and responded well to conservative management. However, among those in need of dialysis, case fatality rate was high (72%) in the absence of this facility which subsequently dropped to 36% with the establishment of renal replacement therapy.
It is recommended that children who present with haemoglobinuria should be considered at risk of AKI and should thus be closely monitored. In tropical Africa where Burkitt lymphoma is endemic, all children presenting with lymphoma should be monitored for AKI.
In view of the less technical competence required for the performance of peritoneal dialysis, this form of renal replacement therapy should be promoted across Africa.
Acknowledgement
We are grateful to Mr Bernard Arhin of the Research and Development unit of Komfo Anokye Teaching Hospital for helping with the data analysis. We are also grateful to the Sustainable Kidney Care Foundation of United States for their support in establishing peritoneal dialysis service for AKI in Ghana.
References
-
Holley JL (2005) Clinical Approach to the Diagnosis of Acute Renal Failure. In: Greenberg A, Primer on kidney diseases. (4th edn) Elsevier Sanders, Philadelphia, 287-292.
-
(2012) KDIGO Clinical Practice Guideline for acute kidney injury. Kidney International Supplements 2.
-
Mak RH (2008) Acute kidney injury in children: the dawn of a new era. Pediatr Nephrol 23: 2147-2149.
-
Devarajan P, Goldstein SL (2006) Acute renal failure. In: Kher KK, Schnaper HW, Makker SP, Clinical Pediatric Nephrology. (2nd edn) Informa Healthcare, London, 363-376.
-
Anochie IC, Eke FU (2005) Acute renal failure in Nigerian children: Port Harcourt experience. Pediatr Nephrol 20: 1610-1614.
-
Gbadegesin R, Srivastava R (2003) Paediatric nephrology in developing countries. In: Webb JAN, Postlethwaite JR, Clinical Paediatric Nephrology. (3rd edn) Oxford University Press, New York, 483-492.
-
Goldstein SL (2006) Pediatric acute kidney injury: it's time for real progress. Pediatr Nephrol 21: 891-895.
-
Esezobor CI, Ladapo TA, Osinaike B, Lesi FE (2012) Paediatric acute kidney injury in a tertiary hospital in Nigeria: prevalence, causes and mortality rate. PLoS One 7: e51229.
-
Olowu WA, Adelusola KA (2004) Pediatric acute renal failure in southwestern Nigeria. Kidney Int 66: 1541-1548.
-
Mate-Kole MO, Yeboah ED, Affram RK, Adu D (1996) Blackwater fever and acute renal failure in expatriates in Africa. Ren Fail 18: 525-531.
-
Bruneel F, Gachot B, Wolff M, Régnier B, Danis M, et al. (2001) Resurgence of blackwater fever in long-term European expatriates in Africa: report of 21 cases and review. Clin Infect Dis 32: 1133-1140.
-
Aloni MN, Nsibu CN, Meeko-Mimaniye M, Ekulu PM, Bodi JM (2012) Acute renal failure in Congolese children: a tertiary institution experience. Acta Paediatr 101: e514-518.
-
Gobbi F, Audagnotto S, Trentini L, Nkurunziza I, Corachan M, et al. (2005) Blackwater fever in children, Burundi. Emerg Infect Dis 11: 1118-1120.
-
Adu D, Anim-Addo Y, Yeboah ED, Blankson JM, Annobil SH (1984) Acute renal failure in Ghanaian children. J Trop Pediatr 30: 36-39.
-
Murali SN, Nath KA (2005) Myoglobinuric and Haemoglobinuric Acute Renal Failure. In: Greenberg A, Primer on kidney diseases. (4th edn) Elsevier Sanders, Philadelphia 310-311.
-
Andreoli SP (2009) Clinical evaluation of Acute Kidney Injury in Children. In: Avner ED, Harmon WE. Niaudet P, Pediatric Nephrology. (6th edn) Springer-Verlag, Berlin Heidelberg,1603-1618.
-
Warrel DA (2002) Clinical features of malaria. In: Warrel DA, Gilles HM, Essential malariology. (4th edn) Arnold, London, 191-205.
-
Shimelis D, Tadesse Y (2004) Clinical profile of acute renal failure in children admitted to the department of pediatrics, Tikur Anbessa Hospital. Ethiop Med J 42: 17-22.
-
Van Biljon G (2008) Causes, prognostic factors and treatment results of acute renal failure in children treated in a tertiary hospital in South Africa. J Trop Pediatr 54: 233-237.
-
Debra M, Williams, Sue S, Sreedhar, John J, et al. (2002) Acute Kidney Failure: A Pediatric Experience Over 20 Years. Arch Pediatr Adolesc Med 156: 893-900.
-
Prayong Vachvanichsanong, Pornsak Dissaneewate, Apiradee Lim, Edward McNeil (2006) Childhood Acute Renal Failure: 22-Year Experience in a University Hospital in Southern Thailand. Pediatrics 118.
-
Ball EF, Kara T (2008) Epidemiology and outcome of acute kidney injury in New Zealand children. J Paediatr Child Health 44: 642-646.
-
Shaheen IS, Watson AR, Harvey B (2006) Acute renal failure in children: etiology, treatment and outcome. Saudi J Kidney Dis Transpl 17: 153-158.





