International Journal of Ophthalmology and Clinical Research
Blue-colored Cystic Mass in Newborn Babies
Titap Yazicioglu1* and Isil Kutluturk2
1Kartal Research and Training Hospital, Eye Clinic, Istanbul, Turkey
2Umraniye Research and Training Hospital, Eye Clinic, Istanbul, Turkey
*Corresponding author: Titap Yazicioglu, Kartal Research and Training Hospital, Eye Clinic, Konaklar mh. Sebboy sok. Petekler sit. G/B D:18, Yenilevent, Istanbul, Turkey, Tel: +905322947119, E-mail: t_yazicioglu@hotmail.com
Int J Ophthalmol Clin Res, IJOCR-3-055, (Volume 3, Issue 2), Research Article; ISSN: 2378-346X
Received: April 09, 2016 | Accepted: May 23, 2016 | Published: May 25, 2016
Citation: Yazicioglu T, Kutluturk I (2016) Blue-Colored Cystic Mass in Newborn Babies. Int J Ophthalmol Clin Res 3:055. 10.23937/2378-346X/1410055
Copyright: © 2016 Yazicioglu T, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To report the clinical findings, and outcomes in newborn infants presented with a cystic mass located inferior to the medial canthus.
Methods: The medical records of twelve newborn infants between 15 days and 3 months of age, with the presence of an unilateral dark-blue mass in the medial canthal region, as soon as after birth, were rewieved retrospectively. The management protocol was consisted of the warm compress and massage over the mass, and antibiotics when dacryocystitis developed. Nasolacrimal duct probing was performed in cases of no spontaneous resolution. Patients age at the time of clinical examination, presence of retrograde outflow from the puncta and development of dacryocystitis were recorded.
Results: A total of twelve newborn infants, age ranged from 15 to 90 days (mean 12 days ), 7 (58.3%) female, and 5 (41.5%) male, with a blue-colored cystic mass over the lacrimal sac, were diagnosed as dacryocystocele. Patients were followed up to 12 months (range, 6 to 24 months). This cystic lesion was unilateral in all cases (100%), with 75% right site involvement. Among these 2 (16.7%) of the patients had spontaneously resolved by systemic antibiotic therapy and massage. Acute dacryocystitis was seen in 10 (83.3%) of the patients, and they were succesfully treated by topical and systemic antibiotic prior to nasolacrimal duct probing.
Conclusion: In order to prevent high incidence of complications such as dacryocystitis and orbital cellulitis, careful observation and treatment should be performed in newborn babies with cystic mass over the lacrimal sac.
Keywords
Dacryocystocele, Amniontocele, Nasolacrimal duct cyst, Lacrimal probing
Introduction
Newborn babies sometimes present with tense visible swelling of the lacrimal sac [1]. This is known as congenital amniontocele or dacryocystocele [1], which is a rare form of congenital nasolacrimal duct obstruction, with an incidence of 0.7% in all infants, 0.02% in newborns, and 0.1% in infants with nasolacrimal duct obstruction [2]. As it is known, the mechanism of this obstruction is due to concomittant upper obstruction of Rosenmuller valve and lower obstruction of the Hasner valve, that causes accumulation of fluid, which is initially filled with mucoid material, in the drainage system [3]. This represents itself as a grey-blue cystic swelling just below the medial canthal ligament, and if it is extend into the nasal cavity, it can cause respiratory distress [1-3]. Although the cystic swelling can be resolved spontaneously with warm compresses and massage within 2 weeks, early surgical intervention, due to the fact that dacryocystoceles have a great tendency to developed dacryocystitis or cellulitis, is recommended [1,4]. So the treatment is still controversial [2]. In this report, we describe 12 congenital dacryocystocel cases, their clinical and surgical outcomes.
Materials and Methods
The records of twelve infants with dacryocystoceles were reviewed retrospectively. The median age at diagnosis was 12 days (range, 15 to 90 days), and 7 (58.3%) of them were female. Parents were complaining about an unilateral dark-blue mass just below the medial canthal region, as soon as after birth. All the infants were the result of full-term pregnancies, and there was no family history of dacryocystocele. Parents were carefully asked about symptoms of nasal congestion, snoring respirations, tachypnea, and breathing difficulty with feeding. Any craniofacial anomalies the lacrimal system, atresia of the lacrimal canaliculi or puncta, or other ocular conditions, such as glaucoma or cataracts were not included in the study.
Infants with non infected dacryocystoceles were initially treated by conservative treatment with warm compress and gentle digital massage of the lacrimal sac by their pediatricians. If they became infected and progress to acute dacryocystitis and lacrimal sac abscess, topical and systemic antibiotics were given. Patients who did not show any improvement with conservative or medical treatment were referred our clinic for further treatment, nasolacrimal duct probing. Nasal examination was found normal in all the patients.
The diagnosis of dacryosytocele was made by the presence of an unilateral dark-blue mass in the medial canthal region, as soon as after birth. In order to verify the diagnosis, cardio-spect view with Tc 99m-O4 scopic view of nasolacrimal duct, Computed tomography (CT), B-scan ultrasonography imaging and dacryocystography, were requested to all of the patients but some of the parents were unwilling to do this because of their poor conditions.
The surgical procedure was performed under general anesthesia. After dilatation of the superior lacrimal puncta, a Bowmann 00 probe was passed through the Rosenmuller valve into the lacrimal sac, and then the probe was rotated and directed down the nasolacrimal duct. An obstruction at the Rosenmuller and Hasner valve site was perforated and dense mucopurulent secretion was aspirated from the nasal cavity. Oral and topical antibiotics were given for one week after surgery, and massage was recommended for one month.
The data of the spontaneously resolved dacryocystoceles and persistent dacryocystoceles with previously treated with antibiotics, and massage, and then successfully treated by nasolacrimal duct probing were compared by Pearson's chi-squared test. A value of P < 0.05 was considered statistically significant. As the study consist of low number of patients, the results were given in percentages.
Results
A total of 12 infants, 7 (58.3%) female, and 5 (41.5%) male, with dacryocystocele were included in the study. The median age at diagnosis was 12 days (range, 15 to 90 days). Patients were followed up to 12 months (range, 6 to 24 months). Symptoms were unilateral in 12 patients (100%). The affected side was right in 9 (75%) of cases. In 2 (17%) of them there was also obstruction at the canalicular stage of the nasolacrimal system. The initial clinical characteristics of the patients were shown in table 1.
![]()
Table 1: The initial clinical characteristics of the patients.
View Table 1
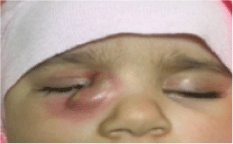
Clinical findings included a blue- colored, soft, well localized cystic mass was seen in 2 (16.7%) of 12 patients (Figure 1), dacryocystitis in 10 (83.3%) of the 12 patients (Figure 2A), and also there was abcess formation and fistulizing sac in one of the 10 dacryocystitits patient (Figure 3). All patients were initially treated conservatively by their pediatrician. Except two, all of the patients had dacryocystitis signs and treated by systemic antibiotic and massage prior to surgery. Among 12 patients only 2 had spontaneous resolution of the cyst. 10 (83.3%) of the them who did not show any improvement with conservative or medical treatment were gone to nasolacrimal duct probing under general anesthesia. In 1 of the dacryocystitis patients, there was also abcess formation and although probing was done successfully under antibiotic treatment, there was recurrence in abcess formation ten days after the operation. Antibiotic treatment was given intravenously, and as soon as the signs and symptoms of inflammation notably subside, not only probing but also exploring the lacrimal sac region was done by making skin insicion. After finding the fistulising site of the lacrimal sac, it was repaired and the patient was completely cured and no recurrence was seen during the follow-up period (Figure 4).
.
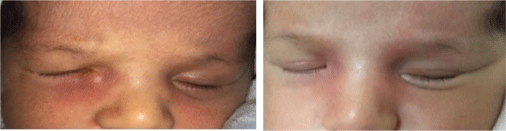
Figure 2: A) Cyctic dilatation and hyperemia on the lacrimal sac region; B) Resolution after probing.
View Figure 2
Spontaneous resolution was seen in 2 (16.7%) of 12 patients with who had mild hyperemic swelling below the medial canthal region and secretion. Nasolacrimal duct probing was found successful in 10 (83.3%) of 12 patients (p = 0.01) (Figure 2B). There was correlation between abcess perforation and age of patient (p = 0.09). But this was an an extreme sample.
.
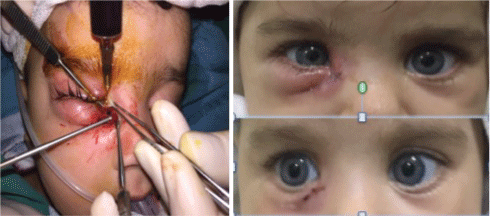
Figure 4: A) Patient was operated again. The site of the fistulizing sac was found and repaired; B) The symptoms were resolved.
View Figure 4
Discussion
The nasolacrimal drainage system begins to develope from surface ectoderm [5] at 6 weeks of gestational age and completes its development by 28 months [6]. However, the distal end of the lacrimal drainage system at the level of valve of Hasner may canalize at birth or even later. In this non-patent distal end, the amniotic fluid fills and distends the nasolacrimal duct and the lacrimal sac after the patency of the lacrimal puncta [5]. In the event of the early onset of mucus production by goblet cells, mucinous secretion may lead to distention of the lacrimal drainage system. This then acts as a check-valve system that only permits the fluid to enter into the sac, leading to further distention of the lacrimal sac [5]. As its known proximal obstruction may produce a lacrimal sac mucocele, whereas a more distal blockade may cause nasolacrimal duct mucocele [7]. All mucoseles involving the lacrimal sac present clinically as medial canthal masses, the skin overlying these mucoceles may show a blue discoloration [7], which is often misdiagnosed as a vascular lesion [1]. As the earliest diagnosis can be made in 27th gestational weeks [8], its prenatal detection is important, because it may be seen in numerous syndromes and may serve as their marker [8]. Bilateral cysts have the possibility for intranasal extension and an obstruction to the nasal passages may result in neonatal respiratory distress requiring surgical intervention [8-10]. Unilateral cases are important for the differential diagnosis with serious facial abnormalities [8].
There is a strong female preponderance (73%) and unilateral involvement (88%). The female preponderance is due to having narrow nasolacrimal duct than boys [1]. Our study consist of 12 infants with dacryocystocele, and 7 (58.3%) of them female, and 5 (41.5%) were male. Symptoms were unilateral in 12 patients (100%). The affected side was right in 9 (75%) of cases. This findings are same as it is mentioned in the various studies [1,11].
Several treatment modalities have been proposed for the management of dacryocystocele, including massage, warm compresses, topical or parenteral antibiotics and, when still symptomatic, nasolacrimal probing, intranasal endoscopic cyst marsupialization is recommended [1,2,12]. Parents are teached to do gentle massage [8,13]. Lucarelli et al. reported a case of corneal ectasia with massage of dacryocystocele [14].
Some physicians have recommended early surgical intervation if there is not a rapid response to conservative therapy [1,12]. Bhatia et al. and Lorena et al. You Jin Ha et al. showed complete resolution in their case report with conservative treatment with oral and topical antibioitics and digital massage [1,13,15].
In our study, all of the patients with non infected dacryocystoceles were initially treated by conservative treatment with warm compress and gentle digital massage of the lacrimal sac by their pediatrician. But those patients who had persistent dacryocystocele or a tendency to developed dacryocystitis or cellulitis were referred to our clinic. Among them 2 patients had persistent blue colored cystic mass, and 10 patients had dacryocystitis signs. Topical and systemic antibiotics and gentle massage were given first to dacryocystitis patients. Among them only 2 had spontaneous resolution of the cyst, and 1 had persistent abcess formation in spite of systemic antibioterapy. Patients who did not show any improvement with conservative or medical treatment, were gone to surgery. Nasolacrimal duct probing was performed to 2 patients with persistent dacryocystocel and 10 patients with dacryocystitis, and was found successful in 10 (83.3%) of the patients (p = 0.01). Only in 1 patient with recurrent abcess, not only probing but also repairing the fistula site of the lacrimal sac was needed.
If the cyst left untreated, the fluid-filled sac is at a higher risk of infection, secondary scarring and permanent closure, requiring dacryocystorhinostomy [1,12]. Becker et al. described 27 patients with dacryocystocele and reported their results such as 37.9% were required intravenous antibiotic therapy, and 34.5% were dacryocystitis without cellulitis. They also stated that one or more probings were performed in 26 patients (89.7%), and initial probing was found 100% successful in patients with no lacrimal system infection, and 53% successful in patients who had dacryocystitis with or without cellulitis [15]. In our study we have 83.3% success with initial probing, and 16.7% spontaneous resolution. Abcess formation was observed only in 1 (8%) of the patients who was at 3 months of age. Her history was thought us that, there was a neglection of the cyctic swelling of the lacrimal sac by their parents. There was a resistance to antibioterapy. After the drainage of the abcess and then nasolacrimal duct probing under the antiobiotic treatment, we explored the lacrimal sac region, and found and repaired the fistula site of the lacrimal sac. The symptoms were resolved after than [16].
Surgical intervention is indicated in the event of dacryocystitis, cellulitis, respiratory difficulty caused by a nasal cyst and non- resolution of the cyst after a short trial period of message [3]. Although there is no case which had intranasal cyst in our study, high-prevalence of intranasal cyst has been reported by previous studies [10,17,18]. As the infants are obligate nasal breathers within the first 3 weeks, congenital dacryocystocele may cause dyspnea. Nasal examination should be performed in all cases to exclude the coexistence of a nasal cyst responsible for respiratory distress [3,10]. After the adequate contraction of mucosa of inferior nasal meatus, intranasal cyst should be observed almost all cases of congenital dacryocystocele by using a nasal endoscope. Not only probing but also marsupialization of an intranasal cyst is adequate surgical approach to congenital dacryocystocele.
Conclusion
Congenital dacryocystocele is an uncommon unilateral condition of predominantly neonatal females. Although one-third of the cases are successfully managed with conservative treatment alone, most patients need surgical intervention in order to reduce the incidence of dacryocystitis and cellulitis.
So the patients with congenital dacryocystocele, should have probing on an urgent basis as early in life as possible, unless the lacrimal sac decompresses into the nose at the time of the initial examination.
Declaration
The authors alone are responsible for the content and writing of the paper.
Conflicts of Interest
No conflicting relationship exists for any author.
Acknowledgement
Institution at which the study was conducted Kartal Research and Training Hospital, Eye Clinic, Istanbul.
References
-
Bhatia J, Rahman N, Varghese M (2007) Uncommon presentation of congenital lacrimal duct obstruction a case report of congenital amniontocele. Oman Med J 22: 60-61.
-
Mimura M, Ueki M, Oku H, Sato B, Ikeda T (2014) Process of spontaneous resolution in the conservative management of congenital dacryocystocele. Clin Ophthalmol 8: 465-469.
-
Cavazza S, Laffi GL, Lodi L, Tassinari G, Dall'Olio D (2008) Congenital dacryocystocele: diagnosis and treatment. Acta Otorhinolaryngol Ital 28: 298-301.
-
Brodkiewicz A, Zakowska A, Peregud-Pogorzelski J, Gizewska M, Burak M, et al. (2010) Congenital nasolacrimal duct mucocele--a case report. Turk J Pediatr 52: 194-197.
-
Kim YH, Lee YJ, Song MJ, Han BH, Lee YH, et al. (2015) Dacryocystocele on prenatal ultrasonography: diagnosis and postnatal outcomes. Ultrasonography 34: 51-57.
-
Gupta H, Kane S, Balasubramaniam V (2014) Bilateral dacryoceles associated with bilateral alacrimia with punctal and canalicular agenesis. Saudi J Ophthalmol 28: 72-75.
-
Castillo M, Merten DF, Weissler MC (1993) Bilateral nasolacrimal duct mucocele, a rare cause of respiratory distress: CT findings in two newborns. AJNR Am J Neuroradiol 14: 1011-1013.
-
Bingol B, Basgul A, Guducu N, Isci H, Dunder I (2011) Prenatal early diagnosis of dacryocystocele, a case report and review of literature. J Turk Ger Gynecol Assoc 12: 259-262.
-
Roy D, Guevara N, Santini J, Castillo L (2002) Endoscopic marsupialization of congenital nasolacrimal duct cyst with dacryocoele. Clin Otolaryngol Allied Sci 27: 167-170.
-
Hochang K, Jongyeop P, Jaeho J, Junwoo C (2014) Urgent Bilateral Endoscopic Marsupialization for Respiratory Distress due to bilateral Dacryocystitis in a Newborn. J Craniofac Surg 25: 292-293.
-
Shekunov J, Griepentrog GJ, Diehl NN, Mohney BG (2010) Prevalence and clinical characteristics of congenital dacryocystocele. J AAPOS 14: 417-420.
-
Lueder GT (2012) The association of neonatal dacryocystoceles and infantile dacryocystitis with nasolacrimal duct cysts (An American Ophthalmological Society Thesis). Trans Am Ophthalmol Soc 110: 74-93
-
You JH, Hae YC, Ki BM, You WC (2010) A case of Congenital Dacryocystocele. Ann Dermatol 22: 54-56.
-
Lucarelli MJ, DeBry P (2002) Corneal ectasia associated with massage of dacryocystoceles. Cornea 21: 419-420.
-
Lorena SHT, Gonçalves ED, Silva JAF (2014) Congenital dacryocystocele: case report and treatment. Rev Bras Oftalmol 73: 243-245.
-
Becker BB (2006) The treatment of congenital dacryocystocele. Am J Ophthalmol 142: 835-838.
-
Roy D, Guevara N, Santini J, Castillo L (2002) Endoscopic marsupialization of congenital nasolacrimal duct cyst with dacryocoele. Clin Otolaryngol Allied Sci 27: 167-170.
-
Shashy RG, Durairaj VD, Holmes JM, Hohberger GG, Thompson DM, et al. (2003) Congenital dacryocystocele associated with intranasal cysts: diagnosis and management. Laryngoscope 113: 37-40.