International Journal of Ophthalmology and Clinical Research
Intravitreal Implant of Dexamethasone for Treatment of Refractory Cystoid Macular Edema Surgically Induced After Pars Plana Vitrectomy
Rino Frisina1* and Barbara Parolini2
1Ophthalmological Unit of Autonomous Province of Trento, Italy
2Department of Ophthalmology, Sant'Anna Hospital, Italy
*Corresponding author: Rino Frisina, Ophthalmological Unit of Autonomous Province of Trento, Italy, Tel: +39-3470652361, Fax: +39-030 3197174, E-mail: frisinarino@gmail.com
Int J Ophthalmol Clin Res, IJOCR-2-041, (Volume 2, Issue 6), Research Article; ISSN: 2378-346X
Received: August 19, 2015 | Accepted: October 19, 2015 | Published: November 02, 2015
Citation: Frisina R, Parolini B (2015) Intravitreal Implant of Dexamethasone for Treatment of Refractory Cystoid Macular Edema Surgically Induced After Pars Plana Vitrectomy. Int J Ophthalmol Clin Res 2:041. 10.23937/2378-346X/1410041
Copyright: © 2015 Frisina R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To evaluate the efficacy and safety of intravitreal implant of Dexamethasone (Ozurdex, Allergan, Irvine, Calif, USA) for the treatment of refractory and chronic cystoid macular edema secondary to PPV and peeling of ERM and internal limiting membrane (ILM) with or without simultaneous cataract surgery.
Methods: Seven eyes of 7 patients affected by chronic and refractory CME for at least 3 months after vitrectomy and peeling of ERM and ILM, were recruited. All patients underwent intravitreal injection of 0.7 mg of Dexamethasone (IVO injection). Demographic data, preoperative and postoperative best corrected visual acuity (BCVA), central foveal thickness (CFT) and intraocular pressure were collected. The follow up was of 6 months.
Results: In all cases, the intraretinal cysts disappeared with an improvement of BCVA. The mean BCVA was 0.87 ± 0.57 at baseline and 0.31 ± 0.27 at 6 months after IVO. The mean CFT was 610.57 ± 200.64 preoperatively and 272.14 ± 73.7, (180-348 microns) at 6 months after IVO.
Conclusions: In this study, the authors noticed an improvement in BCVA, the disappearance of the cysts and the CFT reduction in all patients already at the one month postoperative visit. The effect persisted up to 6 months. The visual recovery after treatment with IVO seems to be related to the duration of edema and to the preoperative visual acuity. CFT reduction does not seem to depend on the duration of the disease. The IVO injection has allowed the treatment of CME without the adverse side effects of systemic steroids.
Keywords
Cystoid macular edema, Pars plana vitrectomy, Epiretinal membrane, Central foveal thickness
Introduction
The purpose of this study was to evaluate the efficacy and safety of intravitreal implant of Dexamethasone (Ozurdex, Allergan, Irvine, Calif, USA) for the treatment of refractory and chronic CME secondary to PPV and peeling of ERM and internal limiting membrane (ILM) with or without simultaneous cataract surgery.
Material and Methods
In 2013, 7 eyes (7 patients), affected by chronic and refractory CME for at least 3 months after vitrectomy and peeling of ERM and ILM, were recruited. All patients underwent intravitreal injection of 0.7 mg of Dexamethasone (IVO injection). All patients signed an informed consent document before the IVO.
The following data were collected:
Demographic data:
• Age (years)
• Gender (female-male)
• Eye (right-left)
• Status of lens (phakic-pseudophakic-aphakic)
• Previous ocular surgery: PPV or PPV+ phacoemulsification and implant of intraocular lens (Phaco + IOL)
• Duration time of CME (months)
• Preoperative data:
• Preoperative BCVA (logMAR)
• Intraocular pressure (mmHg)
• Fluorescein angiography (FA)
• Central foveal thickness (CFT) in micron
Fundus examination was performed in all patients at baseline and during the postoperative follow-up. FA was performed at baseline to exclude neo-vascular diseases and to check for the presence of retinitis associated to CME.
Postoperative data:
• BCVA (logMAR)
• Intraocular pressure (mmHg)
• Central foveal thickness (CFT) in micron
• Intraretinal cysts
The patients were followed-up and visited 1, 3 and 6 months after IVO. CFT and macular morphology (reduction or disappearance of intraretinal cysts) were studied with optical coherence tomography (OCT) preoperatively and at each postoperative visit. The values of CFT was the mean of the values of 6 radial line scans centred on the fovea performed by Spectral OCT scanning laser ophthalmoscopy (SLO) (OPKO OTI Miami, FL).
All cases of CME secondary to the following pathologies were excluded from the study:
• Retinal and choroid inflammation
• Vascular occlusion
• Ocular trauma
• Diabetes mellitus
• Subretinal neovascularization
Results
Seven eyes (5 right and 2 left) of 6 patients (2 female and 5 male) were affected by chronic and refractory cystoid macular edema.
The average age of the patients was 73.71 ± 12.53 years (range 58 - 89).
Five eyes were pseudophakic and 2 eyes were phakic.
In all cases CME appeared after PPV and peeling of ERM and ILM.
Among the 5 pseudophakic patients, in 3 cases was performed only PPV, in 2 cases PPV with Phaco IOL.
The mean duration of CME was 17.14 ± 19.26 months (range 3 - 45).
The details of demographic and preoperative clinical characteristics for each eye are summarized in table 1.
![]()
Table 1: Demographic and preinjection IVO clinical characteristics of patients.
View Table 1
CME had appeared between 1 and 3 months post-op in all cases.
In 3 cases CME had been treated first with non-steroid-anti-inflammatory (NSAID) topical therapy. One case had been treated with steroid and NSAID topic therapy. Another one had been treated with systemic steroid therapy and then with steroid and NSAID topic therapy. One case did not receive previous therapy. In all cases no reduction of CME had been obtained.
The mean BCVA was 0.87 ± 0.57 (range 0.4 - 2 logMAR) at baseline; 0.44 ± 0.28 (0.3 - 1 logMAR) at 1 month; 0.36 ± 0.24 (0 - 0.7 logMAR) at 3 months; 0.31 ± 0.27 (0 - 0.7 logMAR) at 6 months.
The mean CFT was 610.57 ± 200.64 (range 290 - 800 microns) pre-operatively, 343 ± 93.15, (190 - 479 microns) at 1 month; 283.14 ± 104.77 (190 - 446 microns) at 3 months; 272.14 ± 73.7, (180 - 348 microns) at 6 months.
The patterns of BCVA and CFT, during the follow up for each eye, are reported in table 2.
![]()
Table 2: Pattern of BCVA and CFT.
View Table 2
The mean IOP was 13.8 ± 1.48, (range 12 - 16 mmHg) pre-operatively; 13.6 ± 1.03, (12 - 16 mmHg) at 1 month; 13.6 ± 1.57, (12 - 16 mmHg) at 3 months; 14.6 ± 2.02, (12 - 16 mmHg) at 6 months. No side effects were reported.
In all cases, the intra-retinal cysts disappeared with an improvement of BCVA.
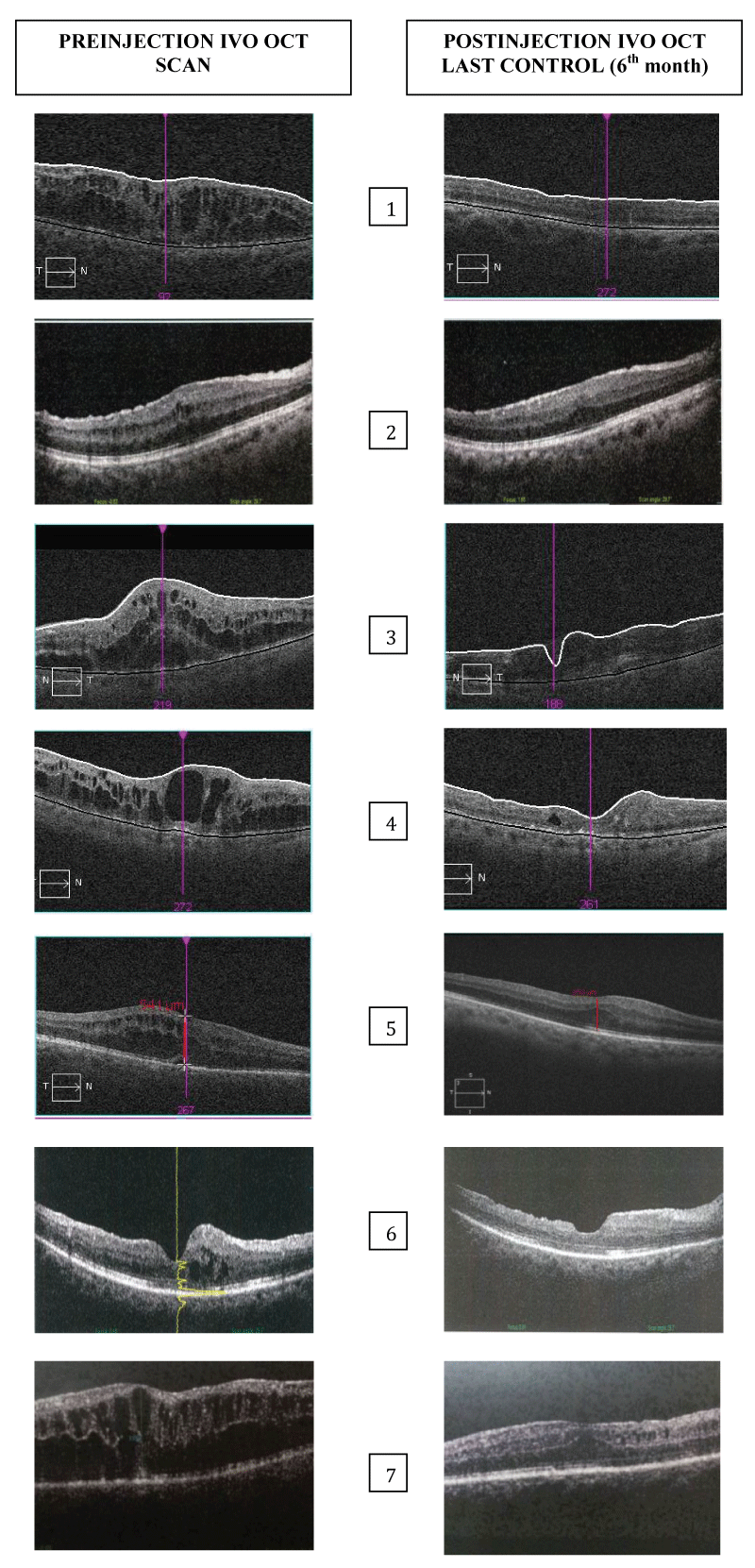
The functional and anatomical improvement was observed at the 1 - month postoperative visit and was maintained to the end of the follow up. Figure 1 shows the preoperative OCT scan and the postoperative OCT scan at the last control (6th month) of the whole group of patients (Figure 1).
.
Figure 1: Preinjection IVO e OCT scan and postinjection IVO OCT scan at the last control (6th month) of the whole group of patients.
View Figure 1
Discussion
Surgically induced cystoid macular edema (CME) is a complication that can occur after intraocular surgery. In 1953, Irvine noticed a syndrome that occurs after cataract extraction [1]. In 1966, Gass and Norton described the angiographic features of this syndrome in aphakic eyes and called it Irvine Gass syndrome [2]. However, CME can occur after various types of intra-ocular surgery procedures. CME is observed after the operations of glaucoma, iridotomies penetrating keratoplasty and scleral buckling [3-5]. The incidence of CME is higher when surgical procedures are combined in a single operation [6]. There are several articles documenting that CME may complicate the recovery of vision after anterior segment surgery. However, in literature, only the following papers document the incidence of CME secondary to PPV. In a recent study, Frisina et al. noticed an incidence of 10.04% of CME in a group of 242 patients that underwent PPV for treatment of epiretinal membrane (ERM) [7]. On the other hand, Eric Sigler et al. published that the occurrence of CME after PPV was of 1% in a group of 768 patients that underwent vitrectomy for treatment of ERM [8]. The difference of incidence of CME has been discussed by Frisina and could be due to several factors: calibres of instrumentations (25 or 23 gauge), methods of staining, surgical procedures (application of endolaser), length of follow up, combination with phacoemulsification, definition of CME [7].
There are reports of angiographic cystoid macular edema (CME) where there is visible pooling on the fluorescein angiography (FA), but the patient is asymptomatic. CME is clinically significant if the patient has a reduction of visual acuity. If clinically significant CME persists for more than six months, it may be defined as chronic [9]. CME occurs between the first and third month after surgery [7]. It results in a delay or lack in the recovery of vision. In patients affected by CME secondary to anterior segment surgery, spontaneous resolution with subsequent visual improvement may occur within 3 to 12 months in 80% of cases [10]. In more severe cases, the treatment with the most common anti-inflammatory topical therapies can often lead to complete resolution of edema and visual recovery. It has been observed that CME secondary to PPV, however, could be refractory to standard treatments and could frequently become chronic.
PPV, peeling of ERM and ILM combined or not with phacoemulsification, can determine an inflammatory process that may result in changes of the blood-retinal barrier (BRB) with the consequent alteration of the permeability of endothelial capillary network. Several studies have shown changes in the retinal foveal profile after peeling of the ILM, but there are no studies evaluating the incidence of CME after PPV.
The inflammation causes a breakdown of retinal barrier (BRB) and a diffusion of proteins in the thickness of the neuro-retina. The osmotic gradient causes the accumulation of fluid in the extracellular space. The inflammation can worsen retinal endothelial damage causing chronic macular edema. The most important target for the treatment of CME, is the inflammation. The most common treatments are topical and systemic steroids, topical and systemic non-steroidal anti-inflammatory agents and topical carbonic anhydrase inhibitors. Despite these treatment modalities, CME secondary to PPV may persist.
We decided to use intravitreal steroids for the following reasons. Steroids inhibit the formation of prostaglandins and leukotrienes. At the local level, their vasoconstrictor properties decrease the intracellular and extracellular edema. Steroids inhibit the activity of macrophages, and decrease the production of lymphokines [11]. The IVO injection has allowed the treatment of CME without the adverse side effects of systemic steroids. IVO injection penetrates the BRB allowing a significant concentration of drug and for a long period of time. In our study, we noticed an improvement in BCVA, the disappearance of the cysts and the CFT reduction in all patients already at the one month postoperative visit. The effect persisted up to 6 months.
The study group was limited in number. However, we can confirm what other studies have shown: every case experience a reduction in CFT but not every case experience a parallel improvement in BCVA. The visual recovery after treatment with IVO in our study seems to be related to the duration of edema and to the preoperative visual acuity. The same observation has been made by others [12]. CFT reduction does not seem to depend on the duration of the disease.
Further studies are needed to understand the factors that play a role in the formation and persistence of CME. There are unknown reasons why CME may occur, recur or respond differently to various treatments. However, the IVO proved to be an effective and safe treatment in reducing the CME and limiting the damage to photoreceptors, that occurs for the persistence of fluid in the foveal region.
References
-
Irvine SR (1953) A newly defined vitreous syndrome following cataract surgery. Am J Ophthalmol 36: 599-619.
-
Gass JDM, Norton EWD (1966) Cystoid macular edema and papilledema following cataract extration: A fluorescein funduscopic and angiographic study. Arch Ophthalmol 76: 646-661.
-
Choplin NT, Bene CH (1983) Cystoid macular edema following laser iridotomy. Ann Ophthalmol 15: 172-173.
-
Nirankari VS, Karesh JW (1986) Cystoid macular edema following penetrating keratoplasty: incidence and prognosis. Ophthalmic Surg 17: 404-407.
-
Lobes LA Jr, Grand MG (1980) Incidence of cystoid macular edema following scleral buckling procedure. Arch Ophthalmol 98: 1230-1232.
-
Tso MO (1982) Pathology of cystoid macular edema. Ophthalmology 89: 902-915.
-
Frisina R, Pinackatt SJ, Sartore M, Monfardini A, Baldi A, et al. (2015) Cystoid macular edema after pars plana vitrectomy for idiopathic epiretinal membrane. Graefes Arch Clin Exp Ophthalmol 253: 47-56.
-
Sigler EJ, Randolph JC, Charles S (2013) Delayed on set inner nuclear layer cystic changes following internal limiting membrane removal for epimacular membrane. Graefes Arch Clin Exp Ophthalmol 25: 1679-1685.
-
Gass JD, Anderson DR, Davis EB (1985) A clinical, fluorescein angiographic, and electron microscopic correlation of cystoid macular edema. Am J Ophthalmol 100: 82-86.
-
Bonnet S (1995) Repercussions of cataract surgery on the development of cystoid macular edema in the diabetic patient. Bull Soc Belge Ophtalmol 256: 127-129.
-
Abe T, Hayasaka S, Nagaki Y, Kadoi C, Matsumoto M, et al. (1999) Pseudophakic cystoid macular edema treated with high-dose intravenous methylprednisolone. J Cataract Refract Surg 25: 1286-1288.
-
Wei-Shi Yeh, Julia A. Haller, Paolo Lanzetta, Baruch D. Kuppermann, Tien Yin Wong, et al. (2012) Effect of the Duration of Macular Edema on Clinical Outcomes in Retinal Vein Occlusion Treated with Dexamethasone Intravitreal Implant. Ophthalmology 119: 1190-1198.





