International Journal of Ophthalmology and Clinical Research
Introduction of Basic and Advanced Techniques of Ophthalmic Surgery in Myanmar
Carl-Ludwig Schönfeld1,3*, Chaw Wai Lwin2, Volker Klaub3, San Hlaing2, Thazin Shwe2, Mya Thandar So2, San Myint2, Claudia Klaub4, Tomas Schaal5, Martin Grüterich4 and Tin Win2
1Augenklinik Herzog Carl Theodor, Germany
2Yangon Eye Hospital, Myanmar
3Department of Ophthalmology, University Ludwig Maximilian München, Germany
4Private practice, München, Germany
5Private practice, Bad Tölz, Germany
*Corresponding author: Carl-Ludwig Schönfeld, Augenklinik Herzog Carl Theodor, Nymphenburger Str. 43, 80335 München, Germany, Tel: +49-89-1270930, Fax: +49-89-1290341, E-mail: cb.schoenfeld@gmx.net
Int J Ophthalmol Clin Res, IJOCR-2-035, (Volume 2, Issue 5), Research Article; ISSN: 2378-346X
Received: April 13, 2015 | Accepted: August 25, 2015 | Published: September 01, 2015
Citation: Schönfeld CL, Lwin CW, Klaub V, Hlaing S, Shwe T, et al. (2015) Introduction of Basic and Advanced Techniques of Ophthalmic Surgery in Myanmar. Int J Ophthalmol Clin Res 2:035. 10.23937/2378-346X/1410035
Copyright: © 2015 Schönfeld CL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: We report our first experience with the introduction of an external teaching programme in Myanmar, a country that has only recently opened to the rest of the world.
Methods: 19 eyes in 18 patients were treated by surgical teams comprising a German senior surgeon and a local ophthalmologist. Diagnoses and treatment procedures were recorded, and visual acuity was measured before and 1-7 days after surgery.
Results: Available resources were more appropriate than expected, but supply of consumables and hygienic procedures required improvement. Retinal detachment and vitreous haemorrhages played a dominant role in presenting pathologies. All eligible eyes (n=19) received PPV, frequently combined with other procedures. Despite the short observation period, some improvement of visual acuity could be obtained.
Conclusions: Our programme is in line with the VISION 2020 initiative and yielded tangible benefits for everybody involved. Recommendations for the implementation of such programmes are given.
Keywords
Vitreoretinal surgery, Cataract surgery, Blindness, Myanmar, International cooperation
Introduction
Blindness is one of the oldest and most dreaded health problems of mankind, and most of the underlying diseases are preventable, curable (or at least, controllable) with modern treatment modalities. Whereas avoidable blindness has largely been overcome in developed countries, it continues to represent a major problem up to this day in developing countries and in particular in the-currently 48-'least developed countries' (LDC) of the world [1-3]. The fact that most of the causes of blindness can be removed when sufficient resources are available leads to an extreme worldwide disparity of the prevalence of blindness: Of the officially estimated 37 million blind people in 2002 (best corrected visual acuity of the better eye <3/60)-an approximation that may be way too conservative [1,4] -, a total of 80% lived in developing and least developed countries, respectively [4]. Accordingly, up to 1% of the population in LDC is blind [5]. In the early 1990s, WHO predicted a number of 75 million blind persons by the year 2020 without well-directed measures and initiated a programme ('VISION 2020') in 1999 to reduce this number to 25 million by the year 2020 [6,7]. The goal of this programme is ambitious by any standard, and it definitely overtaxes the means of developing and least developed countries; therefore, foreign cooperation and input of some kind is a certain prerequisite for its accomplishment.
Currently, knowledge about prevalence, incidence and causes of blindness in Myanmar is scanty due to the decade-long seclusion of the country (a MEDLINE search with the key words 'blindness' and 'Myanmar' yielded a mere 19 published articles since filing and indexing began in 1966), but there are some studies-most notably and recently the 'Meiktila Eye Study [8-11]-that provide valuable insights. According to presently published evidence, 40% of the population above 40 years in the rural Meiktila district in Myanmar suffer from significant visual impairment (visual acuity <6/18 in the better eye), and a shocking 8.1% are blind (<3/60) [10]. Approximately 90% of the incident blindness in Myanmar is avoidable [12], with cataract (>50%), glaucoma (~16%) and corneal pathologies (~15%) leading the way in terms of causes. In children specifically, corneal pathologies are a much more important cause of serious visual impairment, and measles keratitis is the single most important identifiable cause [13]. The most prominent reasons for non-treatment of cataract are cost/availability and fear of surgery, respectively [14], i. e. presenting solvable problems in the greater scheme of things.
Previous experience of combined collaboration and training programmes [15-17] taught us that foreign aid only makes sustainable sense when local surgeons are trained to do the required jobs on their own. Facing the magnitude of the problem of blindness in LDC, there is no way that foreign doctors can solve it all by themselves. This kind of substitution only reaches few people and is far from being sustainable. It may even interfere with local efforts to build eye care programmes. However, our previous experience also taught us that we may encounter unexpected and unprecedented complications, challenges and pitfalls when implementing support programmes. Those problems may pertain to local or national political and bureaucratic peculiarities, tribal issues, and in particular unexpected shortfalls in equipment availability.
Foreign medical aid has been a reality for decades in most parts of the developing world, and therefore it is difficult to distinguish between intrinsic and extrinsic reasons for difficulty or failure. In this regard, the recently emerging opening of Myanmar to the world not only presents a major development demand, but also a unique research opportunity. The fact that Myanmar is practically 'aid-naïve' allows for the unbiased quality control of aid implementation and the analysis of potentials and pitfalls of ophthalmological aid programmes. The aim of the present paper is to objectively analyse our first experience with the teaching programme in vitreoretinal surgery in Myanmar and outline a 'cookbook' for future activities in similarly undersupplied countries or, more importantly, regions.
Methods
Design of the programme
Before onset of the programme, consent was obtained from the responsible local authorities after comprehensive information about scope, participants, and methods. Pertinent approval documents can be obtained from the corresponding author.
Patient examination and treatment took place in the Yangon Eye Hospital (30, Natmauk Road, Tamwe Township, Yangon, Myanmar) between Monday, October 28th and Wednesday, November 6th, 2013.
On the first day of the programme (October 28th, 2013), 38 patients with visual impairment and various retinal pathologies were examined by the author (CLS) and another member of the ophthalmological staff of the hospital. Patients in whom surgery was indicated received an appointment for the operation on Tuesday, October 29th through Tuesday, November 5th. The final evaluation of all patients who underwent surgery took place on Wednesday, November 6th, 2013, i. e. 1-7 days after the operation.
Evaluation
Diagnoses, procedures, and visual acuity were determined upon presentation and on the final day of the programme, respectively. The technical difficulty of the required operation was graded by the author (CLS) in three increments ('easy', 'difficult', 'very difficult').
Results
Resources
With respect to the availability of resources, we found clearly distinguishable situations: The level of education and skill both in surgeons and nursing staff were very high, and surgeons were quite experienced in cataract, albeit not in vitreoretinal, surgery (CSR 1,600/1 million inhabitants). Another area of sufficient resources was that of surgical and optical devices: Operating microscopes, lasers, and surgical systems-even including small incision instruments-were largely up to developed countries' standards. However, most of the more advanced equipment came from unaccompanied donations and was to some extend unused. On the other hand, there was a notable shortage of especially expensive devices (e. g., Binocular Indirect OphthalmoMicroscopes) and consumable tools and materials (i. e., perfluorodecalin, silicone oil, curved laser probes, etc.), and standards of hygiene and sterilization were not matching surgical standards.
Patient profile
Upon presentation, patients were between 10 and 81 (mean, 51.3 ± 18.0) years of age. The presenting diagnoses are shown in table 1; most frequently, the leading cause of visual impairment was retinal detachment (n=12, 31.6%), followed by vitreous haemorrhages (n=6, 15.6%), macular hole, and proliferative diabetic retinopathy (both n=5, 13.2%). The non-assignment to surgical treatment was due to decisions of patients and surgeons, respectively.
![]()
Table 1: Leading diagnoses of patients upon presentation
View Table 1
Treatment and outcome
Two operations were performed by the visiting surgeon (CLS) alone, and the remaining 17 procedures by CLS and one of the participating local ophthalmologists. The operations lasted between 40 and 225 minutes (mean, 125.3 ± 45.1 minutes), and the operation theatre was utilized for a total of 57.5 hours over 6 days of surgery. The comparably long duration of surgery is a consequence of the teaching/supervision situation and indicates that this was taken seriously.
Due to the underlying pathology, all patients were treated with a 23-gauge pars plana vitrectomy (ppv). The small-calibre instrument was chosen because it simplifies the surgical procedure (lack of suturing), causes less discomfort, and yields a faster improvement of visual acuity in comparison to 'conventional' 20-gauge instrumentation [18].
In addition to ppv, a variety of procedures were performed according to the individual patient's requirements (Table 2). Most frequently, the vitrectomy was combined with endolaser photocoagulation (n=11, 57.9%) and membrane peeling (n=8, 42.1%). Phacoemulsification and implantation of a posterior chamber intra-ocular lens (PCIOL) was performed in 8 cases (42.1%), and all 12 cases with retinal detachment as the leading diagnosis received a precautionary scleral suture.
![]()
Table 2: Operations
View Table 2
Three of the operations were graded 'easy', two 'difficult', and the remaining 14 operations 'very difficult'.
Despite the short observation period, the visual acuity improved noticably; the median visual acuity after surgery was 1.6 logMAR as compared to 1.9 logMAR before the operations, and the median difference was -0.1 logMAR, equalling one line on visual chart. 11 of the operated eyes (57.9%) showed some degree of improvement of visual acuity, and in three eyes (15.8%) the difference exceeded 1.0 logMAR (Figure 1).
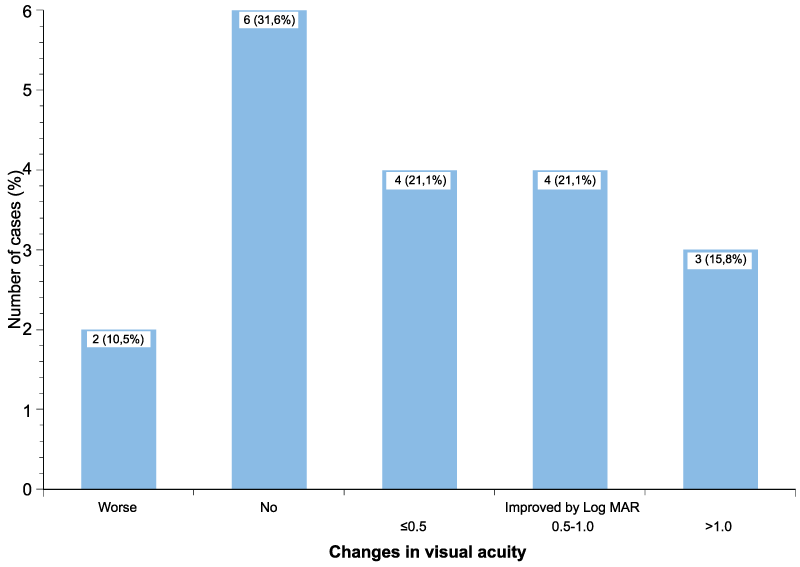
.
Figure 1: Visual acuity 1-7 days after vitreoretinal surgery as compared to baseline
View Figure 1
Discussion
There is a great demand for vitreoretinal surgery in developing countries, and consequently the need for tertiary eye care centres with the required units and equipment as well as appropriate training facilities of vitreoretinal surgeons is eminent. As a result of out long-standing experiences in Kenya, Nepal and Myanmar we can state:
• International cooperation should respond to demand from institutions and/or ophthalmologists in the host country as opposed to being superimposed by foreign countries or NGOs ("paternal philanthropy").
• A long-term perspective with well-defined targets and a clear-cut phasing-out strategy must be defined at the beginning of the partnership.
The improvement of the population's health in poor countries is an immensely demanding and complex task, and the treatment of eye diseases and prevention of blindness are no exception to this rule. While improvements are attainable even under limited funding circumstances [19], they require an integrated approach that homogeneously considers the aspects of availability and affordability of resources, their accessibility for and utilization by the general public, and the quality of delivered care. Evaluations of health care development programmes have shown that substantial funds can be expended without much benefit for the population in impoverished environments; moreover, introduction of treatment facilities without an integrated approach for their utilization may even aggravate poverty due to non-sustainable financial efforts for their accession [20].
Consequently, it is not beneficial (and may even be detrimental) to simply purchase and deliver machinery for modern treatment without making sure that the ultimate goal-improvement of a population's health status-is being met. On the contrary, our Myanmar experience shows that the availability of technical equipment as such is one of the areas with relatively low deficiencies, but that the utilization of advanced equipment requires local education and training.
Overall, the assessment of the one-week training programme was very positive from the side of the participants and the instructors, respectively. In the meantime, one of the participants (CWL) has spent 6 months at the Department of Ophthalmology, University Ludwig Maximilian Munich, and an upcoming programme in Myanmar is scheduled for May, 2014.
The first lesson to be learned from the first implementation of the programme is the high standard of surgical skill already present; the cataract surgical rate (CSR) in Myanmar was 1,600/1,000,000, indicating a fairly high penetration of ocular surgery in comparison to other LDC and developing countries [21,22]. Although this didn't pertain to the more complex-and technically demanding-vitreoretinal procedures, it did indeed facilitate the teaching and made the one-week instruction/supervision programme all the more worthwhile. As a matter of fact, in retrospect the very good standards in basic ophthalmological surgery were a precaution of success of the fairly short period of teaching. Based on this experience, short-term residencies of Myanmar colleagues in high-volume tertiary eye care centres in developed countries would be an excellent method of stepwise qualification; unfortunately, Myanmar's current system of postgraduate education requires 12-month periods of abroad residency to be spent in a single country, which is less than ideal from this point of view.
A definite positive is the generous approval of foreign surgeons' teaching and operating by the Myanmar government; this facilitates sandwich programmes that allow foreign surgeons to gather practical experience and provide substantial benefits for all involved, first and foremost including the patients afflicted by vision-threatening or -destroying eye disorders.
While the initial situation in terms of human resources and technical appliances was better than expected (and a more than adequate basis for the teaching programme), we identified two distinct areas with deficiencies: Hygiene and sterilization standards on the one, and supply of consumable tools and materials on the other hand. The former issue is theoretically relatively easy to address, but nevertheless represents a pressing global concern: Health-care associated infections-being a major problem in industrialized countries as well-are 5 to 25 times more frequent in developing and LDC, and post-surgical infection rates frequently exceed 25% [23]. In recognition of this issue, the WHO has launched the ‚World Alliance for Patient Safety' in October 2004, emphasizing hand hygiene in healthcare as the key method for improvement [24,25]. The Hippocratic principle of non-maleficence ('primum non nocere' [first, do no harm]) dictates that this issue should be taken seriously, and our observation of room for improvement underlines its importance especially in a resource-replete environment.
A rapid and substantial improvement of the hygienic standards in the Yangon Eye Hospital is certainly attainable without any extra expenditure, but it requires a distinct and targeted educational effort. Just as in teaching surgical skills, short-term residencies in European, North American, Australian, or Singaporean eye care centres would prove to be extremely helpful for the obtainment of appropriate techniques and procedures.
The shortage of consumables reflects a structural problem that we consider typical for developing and least-developed countries based on previous experience in countries like Kenia [15,17,26] and Nepal [27], respectively: Due to the relatively slow turnover, the local distributors have no particular interest in stocking the very expensive and perishable goods because they fear financial losses if they are not sold before their date of expiry. In LDC the majority of patients can contribute nothing or little to the cost of surgery-"cost sharing" -, but models from India and Nepal demonstrated that even in poorer rural populations a significant financial contribution can be achieved [28]. Primarily, the supply of consumables is the local government's responsibility and should only become foreign governments' or NGOs' duty in serious crises.
Whereas the method of examination, discharge and re-admission for surgery did not impose serious logistical problems in the urban Yangon area, it would have complicated patients' access to the programme in more rural regions where transportation can represent an insurmountable obstacle. For the future, it would be preferable to integrate diagnosis and treatment into one hospital visit.
In conclusion, the following aspects should be considered in planning and execution of future programmes for teaching and training of vitreoretinal surgery in LDCs:
• The surgical skill of local ophthalmologists can be unexpectedly high; the cataract surgical rate CSR provides a good 'rule-of-thumb' assessment method.
• In countries with a low CSR, development of basic surgical skills and implementation of safe cataract surgery should be implemented before the more complex procedures. This 'staggered' approach yields faster and more population benefits because up to 75% of blindness worldwide is caused by cataract [29].
• Development programmes must be preceded by an analysis of locally available resources and adapted to its results. This should include a photographic documentation of available facilities that can be electronically submitted to the visiting consultant to allow for demand-adapted planning.
• A working infrastructure for the continuous supply of consumables and the obtainment of expensive equipment needs to be established. Since device and consumable acquisition is often a subject of bureaucratic approval, it may help to lend expensive devices like the BIOM for the teaching period and later negotiate acquisition with the background of a demonstrable benefit.
• Novel surgical techniques, e. g. 23/25-gauge ppv, can and should be taught and implemented within the training programme. This also applies to complex procedures: For instance, the combination of phacoemulsification, PCIOL and ppv is beneficial in terms of completeness of vitreous removal and consequently postoperative convalescence; however, the slightly longer duration requires careful maintenance of intra-ocular pressure, and mastery of the appropriate techniques requires some skill.
• Implementation of sandwich training programmes creates an enticing win-win situation with substantial benefits for every involved stakeholder.
• Along with teaching and training of ophthalmological surgeons, it is paramount that nursing staff in operating theatres, emergency rooms and wards receives equivalent attention with special respect to the issues of hygiene and asepsis. This should include short-term residencies abroad and certifications for obtained qualifications.
• The aforementioned 'staggered' approach equally applies to regional penetration of available methods. Without any reasonable doubt, a development programme for vitreoretinal surgery in Myanmar has to originate in Yangon, but must not end there. In a country with roughly 60 million inhabitants, sufficient supply of only the capital region (with about 10% of the population) merely scratches the surface of the underlying issue that must not be forgot: Prevention of global blindness.
It should be noted that this 'cookbook' is mostly based on personal experience and does not claim completeness. However, said experience spans over 14 years and three countries on two continents, so we are fairly confident that it is comprehensive.
Acknowledgements
There was no relevant funding. Hartmut Buhck assisted the authors in data analysis and manuscript preparation.
References
-
Dandona L, Dandona R (2006) What is the global burden of visual impairment? BMC Med 4: 6.
-
Resnikoff S, Pascolini D, Etya'ale D, Kocur I, Pararajasegaram R, et al. (2004) Global data on visual impairment in the year 2002. Bull World Health Organ 82: 844-851.
-
Resnikoff S, Pascolini D, Mariotti SP, Pokharel GP (2008) Global magnitude of visual impairment caused by uncorrected refractive errors in 2004. Bull World Health Organ 86: 63-70.
-
Pizzarello L, Abiose A, Ffytche T, Duerksen R, Thulasiraj R, et al. (2004) VISION 2020: The Right to Sight: a global initiative to eliminate avoidable blindness. Arch Ophthalmol 122: 615-620.
-
Lewallen S, Courtright P (2001) Blindness in Africa: present situation and future needs. Br J Ophthalmol 85: 897-903.
-
World Health Organization: What is "VISION 2020: The Right to Sight"?
-
Yorston D (1999) The global initiative vison 2020: the right to sight childhood blindness. Community Eye Health 12: 44-45.
-
Abdul-Rahman AM, Casson RJ, Newland HS, Muecke J, McGovern S, et al. (2008) Pseudoexfoliation in a rural Burmese population: the Meiktila Eye Study. Br J Ophthalmol 92: 1325-1328.
-
Casson RJ, Newland HS, Muecke J, McGovern S, Abraham L, et al. (2007) Prevalence of glaucoma in rural Myanmar: the Meiktila Eye Study. Br J Ophthalmol 91: 710-714.
-
Casson RJ, Newland HS, Muecke J, McGovern S, Durkin S, et al. (2007) Prevalence and causes of visual impairment in rural myanmar: the Meiktila Eye Study. Ophthalmology 114: 2302-2308.
-
Durkin SR, Casson RJ, Newland HS, Aung TH, Shein WK, et al. (2007) Prevalence of trachoma-related trichiasis and corneal opacity in rural Myanmar: the Meiktila Eye Study. Ophthalmology 114: e7-11.
-
Nemet AY, Nemet P, Cohn G, Sutton G, Sutton G, et al. (2009) Causes of blindness in rural Myanmar (Burma): Mount Popa Taung-Kalat Blindness Prevention Project. Clin Ophthalmol 3: 413-421.
-
Muecke J, Hammerton M, Aung YY, Warrier S, Kong A, et al. (2009) A survey of visual impairment and blindness in children attending seven schools for the blind in Myanmar. Ophthalmic Epidemiol 16: 370-377.
-
Athanasiov PA, Casson RJ, Newland HS, Shein WK, Muecke JS, et al. (2008) Cataract surgical coverage and self-reported barriers to cataract surgery in a rural Myanmar population. Clin Experiment Ophthalmol 36: 521-525.
-
Schönfeld CL, Kollmann M, Nyaga P, Onyango O, Klauss V, et al. (2013) 11 Years of experience in vitreoretinal surgery training in Nairobi, Kenya, from 2000 to 2010. Can J Ophthalmol 48: 324-330.
-
Schönfeld CL, Kollmann M, Nyaga P, Onyango OM, Klauss V, et al. (2008) [Training program for vitreoretinal surgery in Nairobi, Kenya from 2000 - 2006]. Klin Monbl Augenheilkd 225: 857-862.
-
Schönfeld CL, Nyaga P, Onyango OM, Klauss V, Kampik A, et al. (2012) Benefits, limitations and outcomes of vitreoretinal surgery, Nairobi, Kenya: 8-year experience. Acta Ophthalmol 90: e244-245.
-
Recchia FM, Scott IU, Brown GC, Brown MM, Ho AC, et al. (2010) Small-gauge pars plana vitrectomy: a report by the American Academy of Ophthalmology. Ophthalmology 117: 1851-1857.
-
Balabanova D, Mills A, Conteh L, Akkazieva B, Banteyerga H, et al. (2013) Good Health at Low Cost 25 years on: lessons for the future of health systems strengthening. Lancet 381: 2118-2133.
-
Haddad S, Nougtara A, Fournier P (2006) Learning from health system reforms: lessons from Burkina Faso. Trop Med Int Health 11: 1889-1897.
-
Habtamu E, Eshete Z, Burton MJ (2013) Cataract surgery in Southern Ethiopia: distribution, rates and determinants of service provision. BMC Health Serv Res 13: 480.
-
Rao GN, Khanna R, Payal A (2011) The global burden of cataract. Curr Opin Ophthalmol 22: 4-9.
-
Pittet D, Allegranzi B, Storr J, Bagheri Nejad S, Dziekan G, et al. (2008) Infection control as a major World Health Organization priority for developing countries. J Hosp Infect 68: 285-292.
-
WHO Guidelines for Safe Surgery 2009: Safe Surgery Saves Lives. Geneva, World Health Organization, 2009.
-
Allegranzi B, Storr J, Dziekan G, Leotsakos A, Donaldson L, et al. (2007) The First Global Patient Safety Challenge "Clean Care is Safer Care": from launch to current progress and achievements. J Hosp Infect 65: 115-123.
-
Schönfeld CL, Kollmann M, Nyaga P, Onyango O, Klauss V, et al. (2010) New approach in training in East Africa: vitreo-retinal surgery from 2000 to 2007 in Kenya. Br J Ophthalmol 94: 1402.
-
Schönfeld CL, Hennig A (2013) Restoration of severely impaired eyesight in an adolescent with Down syndrome and bilateral cataract in South Asia. Case Rep Ophthalmol 4: 184-187.
-
Muralikrishnan R, Venkatesh R, Prajna NV, Frick KD (2004) Economic cost of cataract surgery procedures in an established eye care centre in Southern India. Ophthalmic Epidemiol 11: 369-380.
-
Tabin G, Chen M, Espandar L (2008) Cataract surgery for the developing world. Curr Opin Ophthalmol 19: 55-59





