International Journal of Ophthalmology and Clinical Research
Acute Ophthalmic Artery Occlusion as Initial Manifestation of Acquired Immunodeficiency Syndrome
Gowtham Jonna1, Matthew SJ Katz1, David M Rubaltelli1, David C Gritz1 and Peter L Gehlbach2*
1Department of Ophthalmology, Montefiore Medical Center, Albert Einstein College of Medicine, USA
2The Johns Hopkins Hospital, USA
*Corresponding author: Peter L Gehlbach, M.D., Ph.D., Department of Ophthalmology, Wilmer Eye Institute, The Johns Hopkins University School of Medicine, 600 North Wolfe Street, Maumenee Building #746, Baltimore, Maryland 21287, USA, E-mail: pgelbach@jhmi.edu
Int J Ophthalmol Clin Res, IJOCR-2-028, (Volume 2, Issue 4), Case Report; ISSN: 2378-346X
Received: April 18, 2015 | Accepted: July 17, 2015 | Published: July 20, 2015
Citation: Jonna G, Katz MSJ, Rubaltelli DM, Gritz DC, Gehlbach PL (2015) Acute Ophthalmic Artery Occlusion as Initial Manifestation of Acquired Immunodeficiency Syndrome. Int J Ophthalmol Clin Res 2:028. 10.23937/2378-346X/1410028
Copyright: © 2015 Jonna G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: To report the first case of acute ophthalmic artery occlusion as initial manifestation of Acquired Immunodeficiency Syndrome (AIDS) in context of marked Human Immunodeficiency Virus-1 (HIV-1) viremia and otherwise negative work-up.
Methods: Report of a 25 year-old previously healthy man who presented to a hospital-based tertiary care referral center with acute, monocular vision loss. Complete ophthalmologic examination, fluorescein angiography, and full systemic evaluation were performed.
Results: Ophthalmologic examination revealed no light perception with a relative afferent pupillary defect and evidence of marked, diffuse retinal ischemia in the left eye. Fluorescein angiography confirmed poor perfusion. Systemic evaluation revealed positive testing for human immunodeficiency virus (HIV)-1 antibody with a CD4 count of 35 cells per microliter and an HIV-1 viral load of 556,655 copies/milliliter. Systemic evaluation did not reveal other etiologies.
Conclusions: Various levels of retinal vascular occlusion have been reported in AIDS. This case demonstrates the unusual finding of ophthalmic artery occlusion in a patient with undiagnosed AIDS and marked HIV viremia. High HIV viral loads are associated with hypercoagulable, hypo-fibrinolytic states through activation of endothelial cells with induction of a pro-inflammatory cascade.
Keywords
AIDS, HIV viremia, Hypercoagulable state, Retinal vascular occlusion
Introduction
The overwhelming majority of vascular occlusions in patients infected with HIV are microvascular occlusions with cotton wool spots, with branch, central, and hemi- retinal vein occlusions being common. A much smaller proportion of patients has branch or central retinal artery occlusion [1]. Ophthalmic artery occlusion is even less common. In general, arterial occlusive disease of the retina is related to arteriosclerotic thrombosis, vasculitis, embolic impaction, vasospasm, or systemic hypotension. Over 75% of patients with central retinal arterial occlusion suffer from generalized atheromatous disease, which is frequently associated with hypertension, diabetes mellitus, or both [2]. Arteriosclerotic cardiovascular disease is classically associated with increasing age and a slightly greater male preponderance. In younger patients, one must consider other factors that may be responsible for a clotting diathesis. In the Western World, coagulation disorders, cardiac abnormalities, hemoglobinopathies, and oral contraceptives are cited as the major causes of retinal arterial occlusions [3]. Patients seropositive for HIV frequently have high titers of anti-cardiolipin antibodies, which would theoretically predispose them to thromboembolic disease. However, anti-cardiolipin antibodies are rarely associated with clinically detectable vascular thrombosis in patients with AIDS [4]. Retinal vascular occlusions and occlusive vasculitis have long been reported in acquired immunodeficiency syndrome.
Case
A 25 year-old man with a past medical history of treated Chlamydia sexually transmitted infection and no past ocular history, presented to Montefiore Medical Center Emergency Department with acute-onset vision loss of the left eye of less than 24 hours duration. The patient noted dimming of vision in the left eye while going to sleep. He awoke the following morning with painless loss of all vision in the left eye. No similar episodes preceded this event. Pertinent positives included associated weight loss, night sweats, rash (1-week history), odynophagia, and watery diarrhea. No associated fever, chills, headache, chest pain, arthralgias, myalgias, temporal artery tenderness, nausea, or vomiting were noted. There was no recent trauma, travel, sick contacts, or known arthropod-borne infections. The patient reported no use of prescribed, over-the-counter, or illicit drugs other than marijuana.
There is a family history of diabetes mellitus and hypertension but no family history of stroke, coronary artery disease, bleeding disorder, clotting disorder, or autoimmune disease. The patient had a history of 16 ounces of daily alcohol use for several years but more recently, had been drinking two or fewer drinks per week. He reported smoking 2 cigarettes per day for several years but quit 3 weeks prior to presentation. He is bisexual and reports 3-4 lifetime partners. He has engaged in oral sex and stated that he uses condoms with male partners.
Ophthalmologic examination of the right eye was within normal limits with visual acuity of 20/20. Examination of the left eye revealed no light perception with a marked relative afferent pupillary defect and normal anterior segment. Intraocular pressure was 14 and 15 millimeters of mercury in the left and right eyes respectively. Funduscopic examination of the left eye demonstrated evidence of marked optic disc and nerve fiber layer edema most dense in the posterior pole but extending beyond the posterior pole, peri-foveal macular edema, diffuse retinal whitening, attenuation of vessels, box-car segmentation of blood flow in vessels, and sclerosis of vessels. There was no "cherry red spot" present with foveal coloration being brown. There was no evidence of cilioretinal artery perfusion. There was no intraretinal hemorrhage present, as may be associated with a combined central retinal artery and vein occlusion.
The patient's blood pressure was within normal limits. Electrocardiography revealed no evidence of arrhythmia. Hematologic evaluation revealed a mildly elevated erythrocyte sedimentation rate (31mm/hr, 24mm/hr; reference: <16mm/hr), normal C-reactive protein (0.3mg/dL, 0mg/dL; reference: <0.9mg/dL), leukopenia (2.5K/mcL, 2.6K/mcL; reference: 4.8-10.8K/mcL), and thrombocytopenia (100K/mcL, 91K/mcL; reference: 150-400K/mcL) with giant platelets on peripheral smear. Urgent carotid sonography and computerized tomographic scan of the brain were within normal limits. Given that the patient presented approximately 20 hours after onset of symptoms, thrombolytic therapy was not administered. The patient did receive 500 milligrams of intravenous acetazolamide to lower intraocular pressure and treatment-dose heparin was begun by the admitting medicine team.
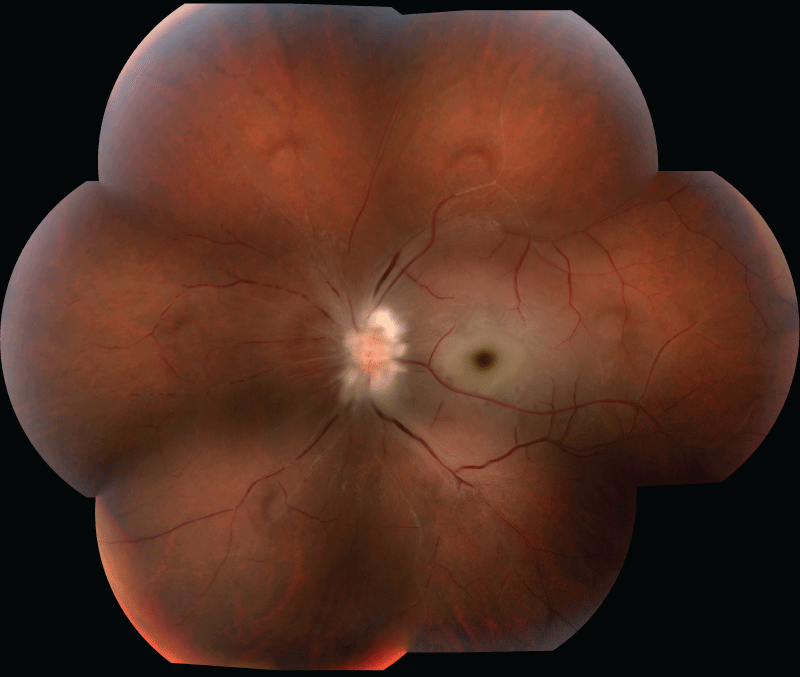
Figure 1 is a composite montage of the ischemic retina of the left eye. Fluorescein angiography confirmed normal perfusion of the right eye and markedly asymmetric, poor choroidal perfusion with essentially no retinal perfusion of the left eye evident (Figure 2a,2b).
.
Figure 1: Composite montage of the retina of the left eye 2-3 days post-presentation demonstrated marked optic disc and nerve fiber layer edema, peri-foveal macular edema, diffuse retinal whitening, attenuation of vessels, box-car segmentation of blood flow in vessels, and sclerosis of vessels.
View Figure 1
.
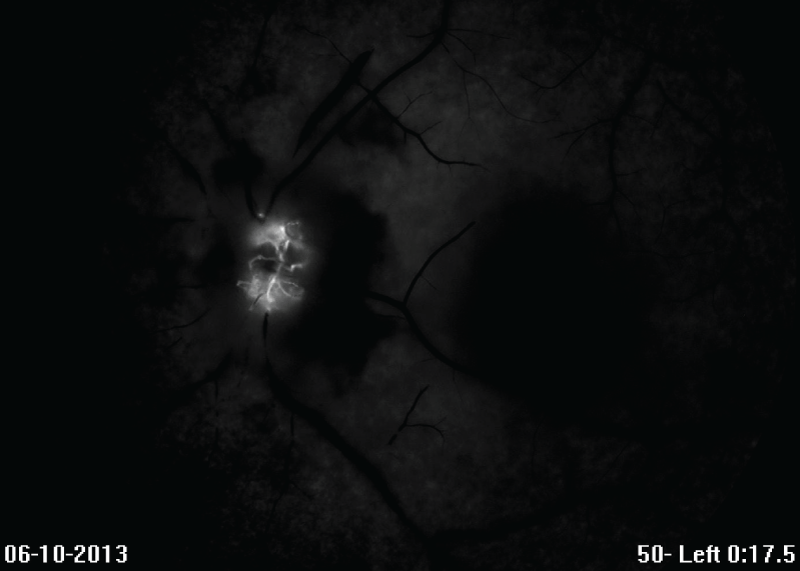
Figure 2A: 2-3 days post-presentation, this early-phase fluorescein angiogram of the left eye at 17.5 seconds post-injection demonstrated choroidal hypoperfusion and a lack of retinal perfusion, as evidenced by lack of arteriole filling.
View Figure 2A
.
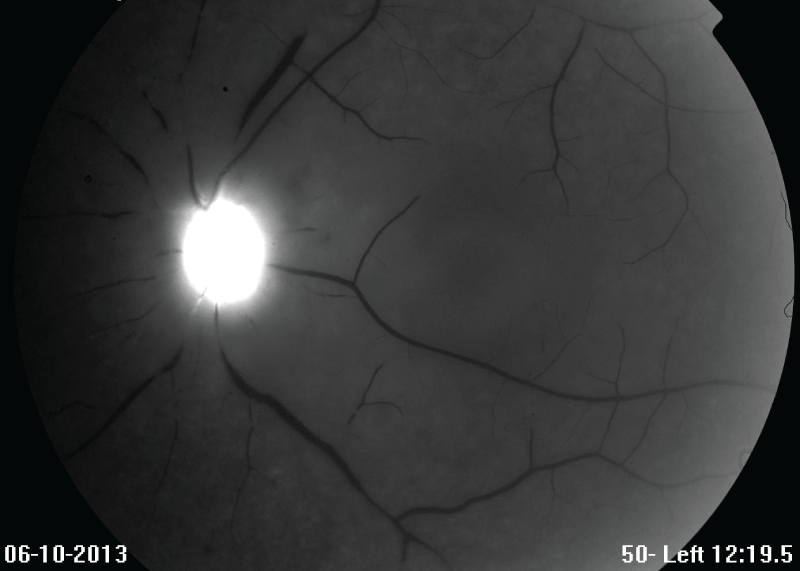
Figure 2B: 2-3 days post-presentation, this late-phase fluorescein angiogram of the left eye at 12 minutes 20 seconds demonstrated a lack of retinal perfusion.
View Figure 2B
In routine evaluation of the presenting leukopenia, a positive result for human immunodeficiency virus (HIV)-1 antibody with a CD4 count of 35 cells per microliter and an HIV-1 viral load of 556,655 copies/milliliter was discovered.
Hypercoagulable work-up revealed moderate protein S deficiency (functional: 37%, reference: 48-136%; antigen: 65%, reference: 70-130%) and mildly elevated anti-cardiolipin IgA (28.8 units, reference: 15-39.9 units weakly positive, >80 units strongly positive) and antiphospholipid IgG (23.3 ASP units, reference: <20 units) antibodies. Patient was found to have elevated transaminases (ALT 97U/L, reference: 5-40U/L; AST 65U/L, reference: 9-48U/L) with positive serum anti-smooth muscle antibodies. Ultrasonography revealed mild hepatomegaly with echogenicity of the liver and mild splenomegaly. Dermatopathologic evaluation revealed herpes simplex virus-related gluteal cleft ulcer, tinea cruris, and spongiotic dermatitis of trunk and extremities. Patient was found to have low Rocky Mountain spotted fever antibody titers. Neuroimaging of brain and orbit and magnetic resonance angiography of the head and neck were all within normal limits. Echocardiography revealed a patent foramen ovale but no evidence of cardiac neoplasm, thrombosis or endocarditis; there was no atrial fibrillation or akinetic wall areas present. Heparin was discontinued after five days of treatment, as there was no clear cause for thrombophilia aside from HIV viremia.
Six weeks after presentation, the patient developed 2+ conjunctival injection, 1-2+ anterior chamber cells with 1+ flare, neovascularization of the iris (NVI), and neovascularization of the angle (NVA) with peripheral anterior synechiae (PAS) of the left eye. Intravitreal bevacizumab injection was administered into the left eye. Eight weeks after initial presentation, the anterior chamber reaction resolved. The fibrotic PAS persisted but the vascular NVI and NVA regressed post-bevacizumab injection. The patient was on highly active anti-retroviral therapy by this point in time. Fundus photography of the left eye (Figure 3a) revealed ischemic retina with diffuse pallor of the optic nerve, reddish-brown foveal pigmentation, retinal pigment epithelium granularity of the macula, and sclerotic retinal vasculature with some areas of sheathing changes. Optical coherent tomography (OCT) of the macula showed normal central macular thickness and foveal contour of the right eye whereas OCT of the macula of the left eye demonstrated diffuse thinning of retinal layers (Figure 3b). Two weeks later, pan-retinal photocoagulation of the left eye was able to be performed.
.
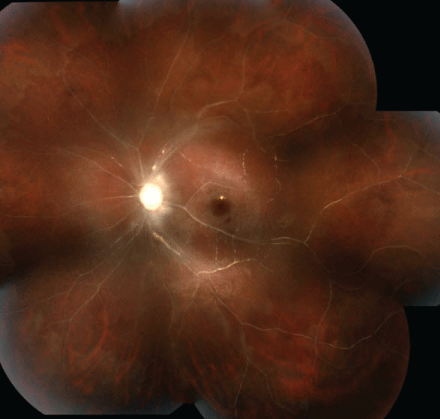
Figure 3A: Composite montage of the retina of the left eye 2 months post-presentation demonstrated ischemic retina with marked optic disc pallor, reddish-brown pigmentation of the fovea, retinal pigment epithelium granularity, and thread-like, sclerotic retinal vasculature with some areas of sheathing changes.
View Figure 3A
.
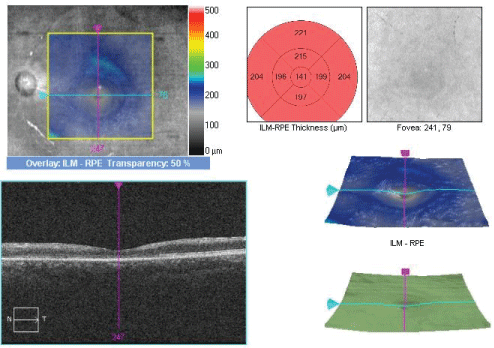
Figure 3B: Optical coherence tomography of the macula of the left eye 2 months post-presentation demonstrated diffuse thinning of retinal layers.
View Figure 3B
Discussion
To our knowledge, this is the first case of acute ophthalmic artery occlusion as a presenting sign of AIDS. In this case, the ophthalmic artery thrombosis is associated with marked HIV viremia and hematology consultation indicates insufficient evidence to support anti-phospholipid antibody syndrome or protein S deficiency as probable etiologies. Though histopathologic evaluation of the ophthalmic artery would be most definitive, the clinical presentation, no light perception visual acuity, funduscopic appearance at presentation and two months later, lack of retinal and choroidal perfusion, and development of anterior segment neovascularization, collectively support a diagnosis of ophthalmic artery occlusion rather than isolated central retinal artery occlusion [5].
Retinal microangiopathy is associated with higher plasma HIV-1 viral loads and lower CD4 cell counts [6]. This case epitomizes these two associations with a CD4 count of 35 cells/microliter and a very high viral load of 556,655 copies/milliliter. Patients with venous thromboembolic (VTE) disease have been shown to have significantly lower CD4 counts, higher HIV viral loads, and lower hemoglobin concentrations than those without VTE. High HIV viral loads are associated with a hypercoagulable, hypo-fibrinolytic state through activation of endothelial cells and induction of a pro-inflammatory cascade [7]. The same theory may apply in other vascular beds of the body, specifically the retinal circulation.
Conclusion
In conclusion, ophthalmic artery occlusion is rare in the young. Given the documented propensity for retinal vascular occlusion in HIV/AIDS and in consideration of this first report of ophthalmic artery occlusion associated with HIV/AIDS, it is reasonable to consider HIV/AIDS in the differential diagnosis of ophthalmic artery occlusion presenting in young patients. Such awareness will help to avoid untoward outcomes and optimize health with prompt and appropriate disease-modifying therapy.
Acknowledgements
The study is supported by an unrestricted grant from the Research to Prevent Blindness foundation. We sincerely acknowledge Kenneth Boyd for his unwavering assistance with ophthalmic photography.
References
-
Dunn JP, Yamashita A, Kempen JH, Jabs DA (2005) Retinal vascular occlusion in patients infected with human immunodeficiency virus. Retina 25: 759-766.
-
Beatty S, Au Eong KG (2000) Acute occlusion of the retinal arteries: current concepts and recent advances in diagnosis and management. J Accid Emerg Med 17: 324-329.
-
Ratra D, Dhupper M (2012) Retinal arterial occlusions in the young: systemic associations in Indian population. Indian J Ophthalmol 60: 95-100.
-
Cappell MS, Simon T, Tiku M (1993) Splenic infarction associated with anticardiolipin antibodies in a patient with acquired immunodeficiency syndrome. Dig Dis Sci 38: 1152-1155.
-
Roth DB, McCabe CM, Davis JL (1999) HIV-related occlusive vasculitis. Arch Ophthalmol 117: 696-698.
-
Furrer H, Barloggio A, Egger M, Garweg JG, and the Swiss HIV Cohort Study (2003) Retinal Microangiopathy in Human Immunodeficiency Virus Infection is Related to Higher Human Immunodeficiency Virus-1 Load in Plasma. Ophthalmology 110: 432-436.
-
Aboulafia DM (2010) An Update on HIV-associated Venous Thromboembolism in the Era of Highly Active Antiretroviral Therapy. J Coagul Disord 2: 1-8.





