International Journal of Ophthalmology and Clinical Research
Orbital Apex Cavernous Hemangioma Causing a Temporal Visual Field Deficit
Ashley A. Campbell1,2*, Suzanne K. Freitag1,2, Benjamin S. Bleier3,4, Simmons Lessell1,5 and Dean M. Cestari1,5
1Department of Ophthalmology, Harvard Medical School, USA
2Ophthalmic Plastic Surgery Service, Massachusetts Eye and Ear Infirmary, USA
3Department of Otolaryngology - Head and Neck Surgery, Massachusetts Eye and Ear Infirmary, USA
4Department of Otology and Laryngology, Harvard Medical School, USA
5Department of Neuro-ophthalmology, Harvard Medical School, USA
*Corresponding author: Ashley A. Campbell, M.D., Ophthalmic Plastic Surgery Service, Massachusetts Eye and Ear Infirmary, Ophthalmic Education, 243 Charles Street, Boston, MA 02114, USA, Tel: 617-523-7900, E-mail: Ashley_campbell@meei.harvard.edu
Int J Ophthalmol Clin Res, IJOCR-2-026, (Volume 2, Issue 3), Case Report; ISSN: 2378-346X
Received: May 28, 2015 | Accepted: June 19, 2015 | Published: June 23, 2015
Citation: Campbell AA, Freitag SK, Bleier BS, Lessell S, Cestari DM (2015) Orbital Apex Cavernous Hemangioma Causing a Temporal Visual Field Deficit. Int J Ophthalmol Clin Res 2:026. 10.23937/2378-346X/1410026
Copyright: © 2015 Campbell AA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We present a case of compressive optic neuropathy from a small hemangioma in the orbital apex causing a mostly temporal visual field defect with some extension nasally on the pattern deviation plot. Given the visual field defect, the location of this lesion was expected to be in the anterior chiasm or prechiasmal optic nerve. This case supports the hypothesis that the organization of temporal visual field fibers likely occurs at the level of the distal optic nerve prior to entering the anterior chiasm.
Keywords
Visual field defect, Orbital cavernous hemangioma
Introduction
Cavernous hemangiomas are the most common benign tumor of the orbit in adults [1], and are usually discovered incidentally. Because of characteristic findings on computed tomography (CT) and magnetic resonance imaging (MRI), the diagnosis can often be presumed based on imaging studies alone [2]. Radiographic characteristics include a well-defined homogenous mass that is isointense to muscle on the T1-weighted sequence, hyperintense to muscle on the T2-weighted sequence, and demonstrates progressive filling on Gadolinium-enhanced sequences [2]. If symptomatic, findings frequently include proptosis, hyperopic shift, limitation of ductions, decreased visual acuity, and visual field deficit [3,4].
Case Report
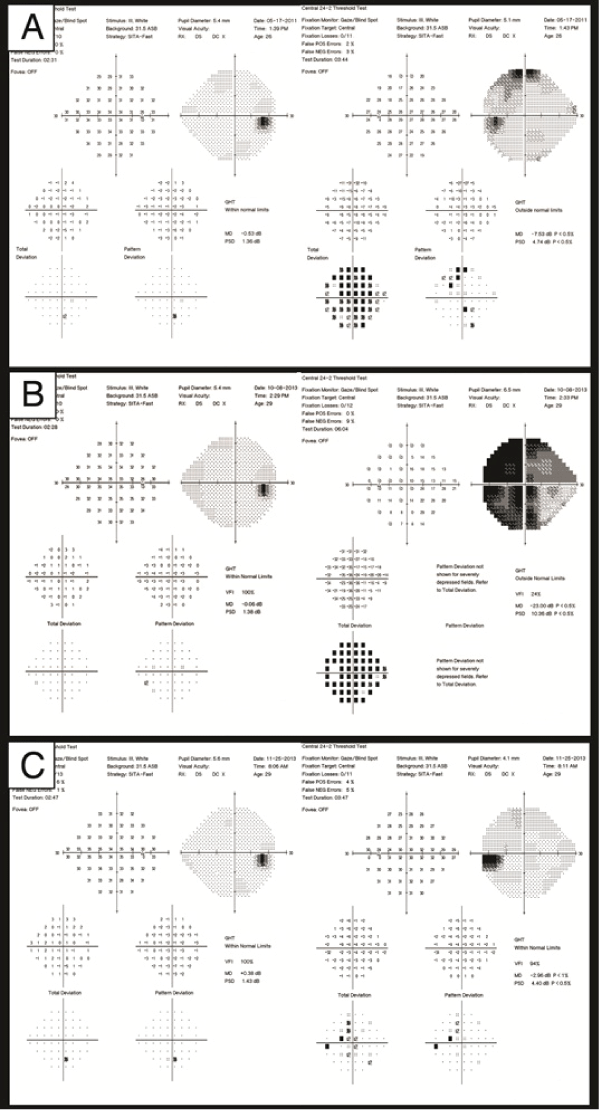
A 29-year-old otherwise healthy man presented to the neuro-ophthalmology service at the Massachusetts Eye & Ear Infirmary with a complaint of decreased vision in his left eye over several months. His visual acuities were 20/15+ OU, and he correctly identified 8 of 8 Ishihara color plates OU. There was no relative afferent pupillary defect. Ductions and versions were full bilaterally, and there was no proptosis. There was questionable left optic nerve temporal pallor. Humphrey visual field testing was performed reliably OU. The visual field of the right eye was normal. There was non-specific decreased sensitivity superotemporally on the pattern deviation plot in the left eye that minimally extended across the vertical meridian (Figure 1a). Goldmann visual field testing demonstrated no vertical step-off on I4e, I3e and 12e. The patient was thought to possibly have a left optic neuropathy and told to follow-up in three months. On his subsequent visit, the findings were unchanged, but the patient was then lost to follow up.
.
Figure 1a: Humphrey visual field 24-2 on initial presentation shows non-specific decreased sensitivity super temporally on the pattern deviation plot OS.
Figure 1b: Humphrey visual field 24-2 two years later demonstrates a dense temporal defect OS that respects the vertical meridian with slight extension into the superonasal quadrant.
Figure 1c: Humphrey visual field 24-2 after endoscopic transnasal resection of apical orbital hemangioma demonstrating significant improvement of the temporal field defect OS.
View Figure 1
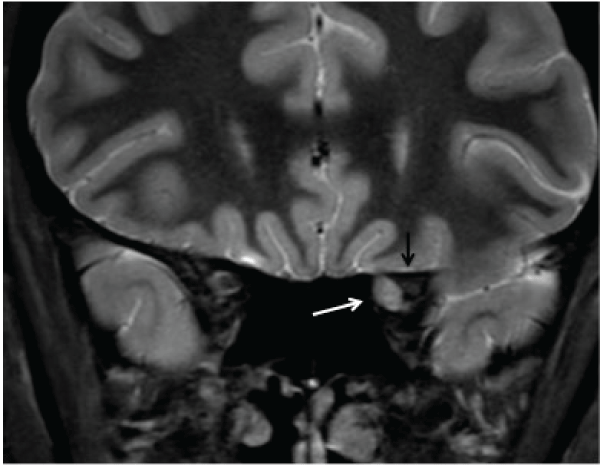
Two years after initial presentation, the patient returned complaining of worsening vision OS over 2 months. His visual acuities were 20/15 OD and 20/300 OS, and he identified 0 of 8 Ishihara color plates OS. There was a left relative afferent pupillary defect, and left optic nerve pallor. Humphrey perimetry demonstrated a diffuse visual field defect most dense temporally OS (mean deviation -23.00 dB) (Figure 1b). MRI Brain with and without contrast revealed an approximately 7mm T1 and T2 isointense well-defined nodular lesion adjacent to the medial posterior aspect of the left optic nerve at the orbital apex that appears to be displacing at the optic nerve superolaterally with adjacent bony remodeling (Figure 2a,2b). The imaging was felt to be most consistent with a diagnosis of cavernous hemangioma. He underwent transnasal endoscopic excision of the mass, and pathology confirmed the diagnosis of cavernous hemangioma.
.
Figure 2A: Pre-operative MRI of the orbit. Coronal Stir image shows an approximately 7mm well-circumscribed hyperintense mass (white arrow) nasal to the left optic nerve (black arrow) at the orbital apex which extends into the optic canal.
View Figure 2A
.
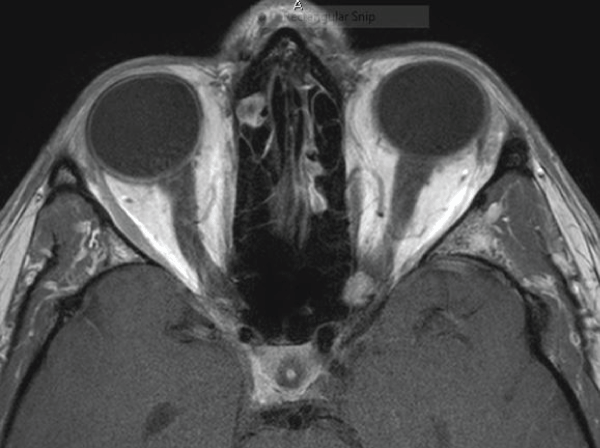
Figure 2B: Pre-operative MRI of the orbit. Axial T1-weighted post-gadolinium image demonstrating the mass nasal to the left optic nerve at the orbital apex which extends into the optic canal.
View Figure 2B
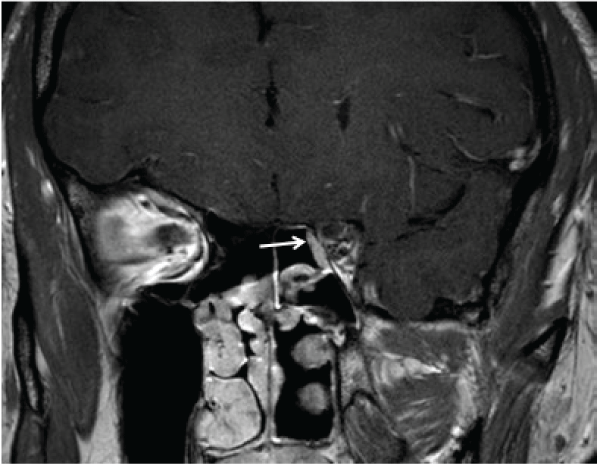
One month after surgery, his visual acuity had improved to 20/15 OS, he correctly identified 8 of 8 Ishihara color plates, and the afferent pupillary defect had resolved. Humphrey perimetry demonstrated significant improvement of the temporal field defect with a mean deviation of -2.96 dB (Figure 1c). A post-operative MRI was obtained and shown in Figure 3.
.
Figure 3: Post-operative MRI of the orbit. Post-gadolinium T1-weighted coronal image of the orbital apex demonstrating absence of the lesion. The arrow indicates the nasoseptal flap reconstruction of the orbital wall defect through which the tumor was removed.
View Figure 3
Discussion
Given the retinotopic organization of the visual pathways, lesions to specific portions of the afferent visual pathway result in fairly reproducible visual field defects. Although there are variations in the visual field defects caused by damage to the optic chiasm, the essential feature is some type of unilateral or bitemporal defect that respects the vertical meridian. Lesions that affect the chiasm can be thought of as occurring in the anterior angle of the chiasm, the body of the chiasm, or the posterior angle of the chiasm. Typically, a lesion at the anterior angle of the optic chiasm creates a "junctional scotoma," initially described by Traquair in 1949 [5]. Additionally, there is a small upper temporal defect in the field of the contralateral eye because of the separation of the nasal crossed and temporal uncrossed fibers. In 1993, Hershenfeld and Sharpe published a case series of 24 patients with monocular temporal hemianopia. In this series, 15 had pituitary adenomas, 2 had tuberculum sella menigiomas, 2 had optic disc dysversion, 2 were non-organic, and 3 had an astrocytoma, craniopharyngioma, and optic neuritis respectively. The presence of a relative afferent pupillary defect, with or without optic disc pallor, on the side of monocular temporal field loss was thought to further localize the lesion to the optic nerve at its junction with the chiasm [6].
Herein, we report a case with a monocular visual field defect mostly affecting the temporal visual field of the left eye with some extension nasally caused by a hemangioma compressing the medial side of the optic nerve in the orbital apex and optic canal but sparing the chiasm. We think this case demonstrates the relationship between compression of the optic nerve nasally in the posterior orbit and optic canal and a mostly temporal visual field deficit. We acknowledge that the visual field defect does not perfectly respect the vertical meridian and suspect this is due to disruption of some of the temporal fibers against the bony optic canal due to displacement of the nerve from a nasal tumor, as would be expected based on a more proximal organization of the fibers in the posterior optic nerve.
In 1980, Unsold and Hoyt demonstrated in a pathologic specimen that a lesion destroying nerve fibers at the temporal side of the optic nerve between the optic canal and chiasm will affect the nasal field of vision [7]. They postulated that a lesion affecting the nerve fibers at the nasal side of the optic nerve would only affect the temporal field of vision. The findings in this case, although not perfect, seem to validate their postulate. Here, the hemangioma compresses the optic nerve nasally within the orbital apex and optic canal producing a visual field defect that is most dense temporally.
References
-
Garrity JA, Henderson JW, Cameron JD (2007) Henderson's Orbital Tumors. (4th edn). Philadelphia, Lippincott Williams & Wilkins, USA.
-
Thorn-Kany M, Arru� P, Delisle MB, Lacroix F, Lagarrigue J, et al. (1999) Cavernous hemangiomas of the orbit: MR imaging. J Neuroradiol 26: 79-86.
-
Harris GJ, Jakobiec FA (1979) Cavernous hemangioma of the orbit.J Neurosurg 51: 219-228.
-
Harris GJ, Jakobiec FA (1978) Cavernous hemangioma of the orbit: A clinicopathologic analysis of sixty-six cases. In: Jakobiec FA. Ocular and Adnexal Tumors. Birmingham: Aesculapius: 741-781.
-
Traquair HM (1949) An Introduction to Clinical Perimetry. (6th edn). Henry Kimpton, Kimpton.
-
Hershenfeld SA, Sharpe JA (1993) Monocular temporal hemianopia.Br J Ophthalmol 77: 424-427.
-
Uns�ld R, Hoyt WF (1980) Band atrophy of the optic nerve. The histology of temporal hemianopsia. Arch Ophthalmol 98: 1637-1638.





