International Journal of Ophthalmology and Clinical Research
Incidence of Ocular Hypertension Following Silicone Oil Use after Vitrectomy Surgery
Ashiyana Nariani, Nitasha Khanna, Arthi Chawla, Rominder Momi, Anna Gabrielian and Seenu M. Hariprasad*
Department of Ophthalmology and Visual Science, University of Chicago, USA
*Corresponding author: Seenu M. Hariprasad, M.D., Professor and Director of Clinical Research, Department of Ophthalmology and Visual Science, University of Chicago, 5841 South Maryland, MC 2114 Chicago, IL 60637, USA, E-mail: retina@uchicago.edu
Int J Ophthalmol Clin Res, IJOCR-2-023, (Volume 2, Issue 3), Research Article; ISSN: 2378-346X
Received: February 09, 2015 | Accepted: May 11, 2015 | Published: May 14, 2015
Citation: Nariani A, Khanna N, Chawla A, Momi R, Gabrielian A, et al. (2015) Incidence of Ocular Hypertension Following Silicone Oil Use after Vitrectomy Surgery. Int J Ophthalmol Clin Res 2:023. 10.23937/2378-346X/1410023
Copyright: © 2015 Nariani A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background and objective: Silicone oil (SO) is important in vitreoretinal surgery. The incidence of glaucoma after silicone oil tamponade (SOT) was investigated.
Study design/patients and methods: A retrospective chart review of patients with SOT at the University of Chicago from 2005 to 2008 was conducted to determine the incidence of Silicone Oil Induced Ocular Hypertension (SOIOH). IOP in the SOIOH and SOIOH free groups was compared with the paired t-test.
Results: 45 eyes were evaluated.15 developed SOIOH. Average length of SOT was 10 months in the SOIOH group versus 7.3 months in the SOIOH free group. IOP in the SOIOH group increased by 9.9 ± 1.8mmHg (p=0.0001; CI: 6.13-13.73) and by 0.97 ± 1.0mmHg (p=0.36; CI: -1.15-3.08) in the SOIOH free group.
Conclusions: One-third of patients with SOT developed SOIOH. Given the association between length of SOT and incidence of SOIOH, SO removal should not be delayed.
Keywords
Progressive myopia, Myopia, Hyperopia, Emmetropia, Multivergence hologram, Latent accommodation
Introduction
Silicone oil (SO), also known as polydimethylsiloxane, is a synthetic polymer made of consecutive Si-O units [1]. It was first introduced by Cibis in 1962 for use in retinal detachment surgery [2]. Today, SO is an important adjunct for internal tamponade in a wide variety of vitreoretinal surgeries, especially in eyes with proliferative vitreoretinopathy and diabetic tractional retinal detachments. Silicone oil has unique chemical characteristics that make it a useful tool in intraocular tamponade. These include an effective buoyant force and high surface tension [3]. There are currently two types of SO available to use in vitreoretinal surgery. The two different SO's are differentiated based on viscosity. The 1000cs SO is less viscous and has a lower molecular weight, and the 5000cs SO is more viscous and has a higher molecular weight [4].
Unfortunately, SO has been associated with complications, such as cataract, keratopathy, and glaucoma [5-9]. Secondary glaucoma has been reported to occur at any time in the post-operative period. This secondary glaucoma can manifest with a wide range of IOP's and vision loss [4,5,10]. The true incidence of secondary glaucoma after SO implantation has been difficult to ascertain from the literature because of this variable presentation [4].
The purpose of our study was to assess the incidence of SOIOH at our institution, after 1000cs SO was implanted in patients requiring silicone oil tamponade (SOT) after pars plana vitrectomy (PPV). Additionally, we analyzed each patient's age, family history of glaucoma, length of SOT, and presence of retained SO and changes in IOP, in order to better understand the various factors that contribute to SOIOH.
Patients/Materials and Methods
We did a retrospective chart review of patients with SOT for various etiologies between 2005 and 2008, including tractional retinal detachment, rhegmatogenous retinal detachment, proliferative vitreoretinopathy, and macular hole. A standard three port pars plana vitrectomy with 1000cs SO injection was performed. All patients underwent three consecutive air-fluid exchanges upon SO removal. No patient had SO overfill. As it is customary in our practice, all had small fluid menisci to ensure absence of overfill.
The main outcome was the development of SOIOH in the operated eye. SOIOH was defined as IOP greater than 20mmHg after post-operative week #3 requiring therapy. Patients who developed SOIOH were compared to those who did not (SOIOH free group), in terms of age, family history, length of SOT, presence of retained SO, and IOP outcomes. IOP values in the SOIOH, SOIOH free and the combined groups were compared with the paired t-test.
Patients with SO overfill or IOP spikes on post-operative days 1-21 were excluded. Additionally, patients with glaucoma, ocular hypertension, glaucoma suspects and those on IOP lowering agents were also excluded.
Results
Forty-five patients that met the criteria were evaluated. The demographics of the SOIOH free group and the SOIOH group are given in Table 1. The average age of all the patients was 43.5 years (range 2-76). The mean follow-up was 21 months (range 6-60). The average length of SOT was 8.2 months (range 4-38). Average pre- and post-operative IOP for the combined group was 13.6 ± 4.6mmHg and 17.5 ± 7.9mmHg respectively. IOP increased by 3.6mmHg (±1.1mmHg; p=0.0009; 95% CI: 1.74-6.17) overall post-operatively for the combined group.
![]()
Table 1: Characteristics of SOIG and SOIG free patients
View Table 1
Fifteen of forty-five patients (33.3%) developed SOIOH. SOIOH group had an average IOP of 12.7 ± 3.8mmHg pre-operatively and 22.6 ± 8.4mmHg post-operatively. Average IOP in the SOIOH group increased by 9.9mmHg (±1.8mmHg; p=0.0001; 95% CI: 6.13 to 13.73) (Table 2).
![]()
Table 2: Results
View Table 2
The SOIOH free group had an average pre-operative IOP of 14.0 ± 4.84mmHg and a post-operative IOP of 15.0 ± 6.2mmHg. Overall there was an increase in the IOP by 0.97mmHg (±1.0mmHg; p=0.36; 95% CI: -1.15 to 3.08) post operatively.
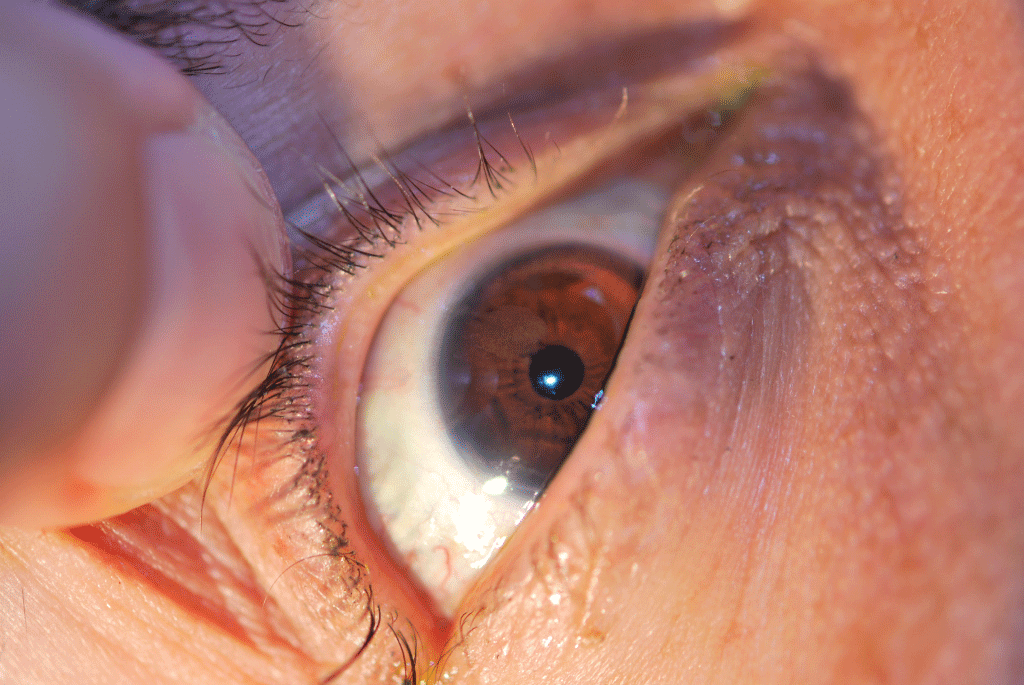
Six of thirty (20%) patients in the SOIOH free group and 5 of 15 (33%) in the SOIOH group had retained silicone oil in anterior chamber after SO removal (Figure 1). Of the 6 patients with retained SO in the SOIOH free group 5 were phakic and one had a posterior chamber intraocular lens (PCIOL). In the SOIOH group 2 out of 5 patient with retained SO were phakic, 1 had a PCIOL and 2 were aphakic. All 11 patients with retained silicone oil in anterior chamber had oil visible in the anterior chamber. Two of the eleven patients (1 from each group) had silicone bubbles in the anterior chamber and angle.
The average time to develop SOIOH was 9.7 months (range 1-38). Thirteen of fifteen eyes (87%) had persistent SOIOH even after SO removal. SOIOH resolved after SO removal in 2 of the 15 patients with SOIOH. In one patient SOIOH resolved after having an additional trip to the operating room to remove persistent SO droplets from the anterior chamber by washout. The rest of the SOIOH patients were managed medically.
Discussion
The development of SOIOH can be categorized according to the postoperative time of onset. SOIOH that develops early in the postoperative period has a different pathogenesis than intermediate-and late onset SOIOH. There are many proposed mechanisms of pathogenesis responsible for early onset SOIOH. These include: 1) pupillary block 2) inflammation 3) pre-existing glaucoma, and 4) migration of silicone oil into the anterior chamber with subsequent mechanical obstruction to filtration [4]. This contrasts with the possible mechanisms for intermediate and late-onset SOIOH, which are: 1) infiltration of trabecular meshwork by SO bubbles 2) chronic inflammation 3) synechial angle closure 4) rubeosis iridis 5) migration of SO (emulsified and non) into anterior chamber [4]. It is difficult to ascertain the relative contribution of these individual factors to the development of SOIOH. This could be because the exact timing of early, intermediate and late onset of SOIOH are poorly defined in the literature.
In our study, SOT with 1000cs SO after PPV seemed to be associated with the development of SOIOH in 33.3% of patients. Literature review shows that the true incidence of glaucoma after SOT is difficult to establish, with averages from previous studies (1979 to 2007) ranging from 0-56% [4].
We excluded patients with acutely elevated IOP in order to investigate a more homogenous group of patients. These included patients who had non-sustained IOP spikes in postoperative days 1-21 and patients with SO overfill. SO overfill can lead to acute glaucoma with shallowing of the anterior chamber and oil displacement into anterior chamber [3]. As a result, all patients had a small meniscus of silicone oil to ensure the absence of overfill. Additionally, as is customary in our practice, all underwent three consecutive air-fluid exchanges upon SO removal to ensure that all oil had been removed.
Age and family history of glaucoma had a positive correlation with the development of SOIOH. This is consistent with the tendency of glaucoma to be an age-related disease. One third of patients with SOIOH had a positive history of glaucoma, which supports our knowledge that genetic predisposition is an important part of the multi-factorial nature of glaucoma, and has important implications for patients undergoing SOT.
The length of SOT was associated with increased incidence of SOIOH. This suggests that SO should be removed as soon as there is no further need for it. Unfortunately, the majority of patients with SOIOH had persistence of the disease, even after SO removal. This could imply that the pathogenesis of SOIOH includes irreversible damage to the angle structures. Additionally, small silicone bubbles could have persisted in the trabecular meshwork, even after oil removal. Patients with SOIOH were 1.7 times more likely to have retained SO in the anterior segment. Retained SO in the anterior segment could increase the risk of developing SOIOH. Patients in the SOIOH group had a 10 fold higher increase in average post-operative IOP.
In our study the incidence of retained silicone oil was 20% and 33%, in the disease free and SOIOH groups respectively. Even though data on incidence of retained silicone oil is limited in literature, a recent study found that 17% of patients retain silicone oil in the anterior chamber after repair of complex retinal detachments with silicone oil tamponade [11]. Patients with SOIOH were 1.7 times more likely to have retained SO in the anterior segment. Retained SO in the anterior segment could increase the risk of developing SOIOH. Notably, there is potentially a correlation between lens status and retained SO. 5 of 6 (83.3%) in the SOIOH free group with retained SO where phakic. 2 of 5 (40%) in the SOIOH group with retained SO where phakic. Another 2 of 5 (40%) in the SOIOH group with retained SO were aphakic. All patients undergoing SOT had increased IOP post-operative, with SOIOH group having a nearly 10 fold higher increase in IOP.
Anterior chamber washout was done in one patient with retained SO in the anterior chamber after SO removal due to persistently elevated IOP despite maximum medical management. This resulted in successful resolution of SOIOH. The remaining patients with SOIOH were managed medically. No patient required surgical management of SOIOH. Given the success of anterior chamber washout in resolving SOIOH, it should be attempted in all patients with persistently elevated IOP and visible SO in the anterior segment.
There is conflicting data regarding the development of SOIOH after the use of the 1000cs or 5000cs SO. For example, one study suggested the 1000cs is more likely to cause an elevated IOP [12], but another study did not find such a difference [13]. Therefore, it would be plausible to investigate 1000cs compared to 5000cs SOT in a prospective, randomized controlled study, in order to determine if there is a significant difference between the two oils in causing SOIOH. This could potentially lead us to modify our use of silicone oil by selecting the "safer" oil for SOT in the near future. Additionally, the issue of ocular hypertension with the current management of SOT, may be overcome through the development of a non-SO vitreous substitute in the future.
Our study was limited by its retrospective nature and a relatively small number of patients. We defined SOIOH to be a persistent elevation of IOP after post-operative week #3. Were this a prospective study, we would have included visual field and pachymetry testing to define the SOIOH group with more accuracy. Despite these limitations, however, our follow-up suggested that over one third of patients with SOT develop SOIOH, with length of SOT being associated with an increased incidence of SOIOH. Since the majority of patients continue to have persistent SOIOH even after SO removal, SOT should be minimized as much as possible, without compromising the success of the surgery.
References
-
Kreiner CF (1987) Chemical and physical aspects of clinically applied silicones. Dev Ophthalmol 14: 11-19.
-
CIBIS PA, BECKER B, OKUN E, CANAAN S (1962) The use of liquid silicone in retinal detachment surgery. Arch Ophthalmol 68: 590-599.
-
Gallemore RP, McCuen BW (2006) Silicone oil in vitreoretinal surgery. In: Ryan SJ ed. Retina, (4th edn). St Louis: Mosby: 2211-2234.
-
Ichhpujani P, Jindal A, Jay Katz L (2009) Silicone oil induced glaucoma: a review. Graefes Arch Clin Exp Ophthalmol 247: 1585-1593.
-
Barr CC, Lai MY, Lean JS, Linton KL, Trese M, et al. (1993) Postoperative intraocular pressure abnormalities in the Silicone Study. Silicone Study Report 4. Ophthalmology 100: 1629-1635.
-
Chan C, Okun E (1986) The question of ocular tolerance to intravitreal liquid silicone. A long-term analysis. Ophthalmology 93: 651-660.
-
Federman JL, Schubert HD (1988) Complications associated with the use of silicone oil in 150 eyes after retina-vitreous surgery. Ophthalmology 95: 870-876.
-
Leaver PK, Grey RH, Garner A (1979) Silicone oil injection in the treatment of massive preretinal retraction. II. Late complications in 93 eyes. Br J Ophthalmol 63: 361-367.
-
Nguyen QH, Lloyd MA, Heuer DK, Baerveldt G, Minckler DS, et al. (1992) Incidence and management of glaucoma after intravitreal silicone oil injection for complicated retinal detachments. Ophthalmology 99: 1520-1526.
-
Zborowski-Gutman L, Treister G, Naveh N, Chen V, Blumenthal M (1987) Acute glaucoma following vitrectomy and silicone oil injection. Br J Ophthalmol 71: 903-906.
-
Ozdek S, Yuksel N, Gurelik G, Hasanreisoglu B (2011) High-density silicone oil as an intraocular tamponade in complex retinal detachments. Can J Ophthalmol 46: 51-55.
-
Petersen J, Ritzau-Tondrow U (1988) Chronic glaucoma following silicone oil implantation: a comparison of 2 oils of differing viscosity. Fortschr Ophthalmol 85: 632-634.
-
Stinson WG, Small KW (1994) Glaucoma after surgery on the retina and vitreous. Semin Ophthalmol 9: 258-265.