International Journal of Ophthalmology and Clinical Research
Corticosteroid in the Treatment of Neisseria gonorrhoeae Keratitis
Elizabeth McElnea1*, Sarah Moran2 and Gareth Higgins1
1Department of Ophthalmology, University Hospital Waterford, Ireland
2Department of Ophthalmology, Cork University Hospital, Ireland
*Corresponding author: Elizabeth McElnea, Department of Ophthalmology, University Hospital Waterford Ardkeen, Co. Waterford, Ireland, Tel: 086 8528074, E-mail: mcelneaelizabeth@gmail.com
Int J Ophthalmol Clin Res, IJOCR-2-020, (Volume 2, Issue 2), Case Report; ISSN: 2378-346X
Received: March 07, 2015 | Accepted: March 30, 2015 | Published: April 02, 2015
Citation: McElnea E, Moran S, Higgins G (2015) Corticosteroid in the Treatment of Neisseria gonorrhoeae Keratitis. Int J Ophthalmol Clin Res 2:020. 10.23937/2378-346X/1410020
Copyright: © 2015 McElnea E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Aim: To describe the effective use of corticosteroid in the management of keratitis caused by Neisseria gonorrhoeae.
Methods: Retrospective review of the case of a nineteen year old gentleman who presented with a purulent ocular discharge and in whom peripheral corneal melt occurred.
Results: Neisseria gonorrhoeae was cultured from conjunctival swab. Systemic and topical antibiotics were given. The peripheral corneal melt was unchanged until systemic corticosteroid was prescribed following which the corneal melt resolved promptly.
Conclusions: Neisseria gonorrhoeae keratitis may behave like a peripheral ulcerative keratitis. In such cases topical and/or systemic corticosteroid may be therapeutic despite their usual contraindication in cases of acute infective keratitis.
Keywords
Neisseria gonorrhoea, Keratitis, Corticosteroid, Peripheral ulcerative keratitis
Description
The left eye of a nineteen year old gentleman became red and productive of a purulent discharge. A conjunctival swab was reserved. Presumed to have bacterial conjunctivitis he was treated with topical chloramphenicol and oral flucloxacillin 500mg both four times daily for one week. Neisseria gonorrhoeae was however cultured. He was referred to our service for further management.
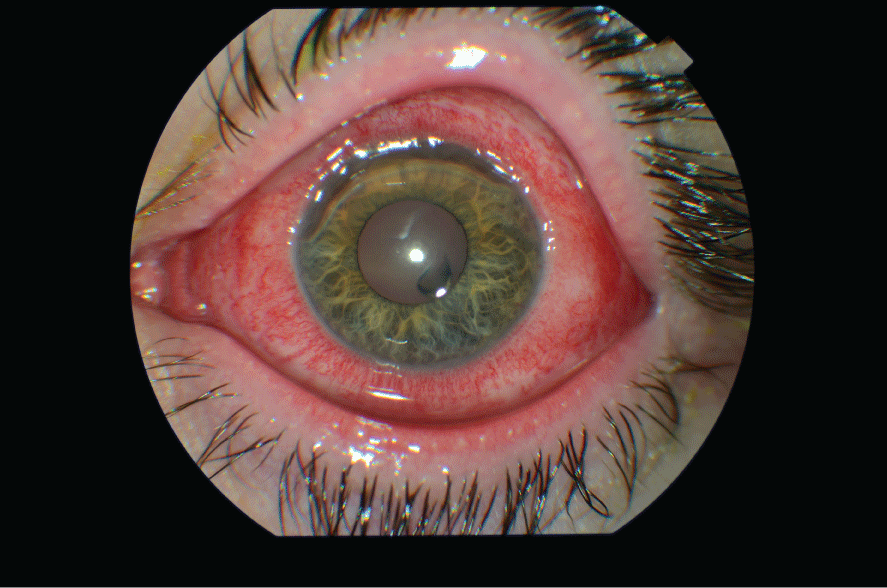
His visual acuity at this time was 6/6 and 6/24 from his right and left eyes respectively. The right eye looked normal. The conjunctiva of the left eye was injected. It was however clear of discharge. A deep gutter extended from the 10 o�clock to the 3 o�clock position in the superior cornea. A smaller para-central area of corneal thinning was also apparent (Figure 1). Treatment with topical exocin and ceftazidime every hour and intravenous ceftriaxone 2g and oral ciprofloxacin 750mg twice daily was commenced. The appearance of this gentleman�s left eye remained unchanged however after five days. Prednisolone 40 mg orally daily was commenced and reduced by 10mg daily every week thereafter. The peripheral corneal melt resolved within two weeks.
.
Figure 1: A deep gutter extended from the 10 o�clock to the 3 o�clock
position in the superior portion of this gentleman�s cornea. A smaller paracentral
area of corneal thinning was also present.
View Figure 1
Comment
Ocular infection with Neisseria gonorrhoeae is relatively rare. We may be less suspicious of it as a result. Indeed, all four cases of corneal perforation secondary to gonococcal infection described in one case series were originally misdiagnosed as epidemic keratoconjunctivitis [1].
Cases occur in sexually active individuals. Infection results from contact with infected urine and/or genital secretions. Such contact may be direct or by indirect �autoinoculation� wherein infective genital secretions are transferred from their source to the eye�s surface by hand-eye contact.
Genitourinary symptoms of gonococcal infection, if they occur (up to 80% of males and 20% females affected in this regard are asymptomatic) may precede ocular symptoms by one to several weeks. Patients are however unlikely to make a connection between their sexual behaviour, genital and ocular symptoms. Consequently, retrieval of the pertinent patient sexual and genitourinary system history may be invaluable in suggesting a diagnosis of gonococcal keratoconjunctivitis.
Neisseria gonorrhoeae causes a conjunctivitis which typically presents hyper-acutely with usually bilateral but occasionally, as here, unilateral, extreme, conjunctival inflammation and an intensely purulent ocular discharge. The presence of an intensely purulent ocular discharge in a sexually active individual should always raise the suspicion of gonococcal eye infection. Tender eyelid oedema can also occur. Ocular motility may be restricted. Indeed unilateral gonococcal conjunctivitis initially thought to be orbital cellulitis has been described [2].
Common corneal findings include a marginal corneal ulcer or corneal melt, sub-epithelial and/or stromal infiltrates and a discrete oedema of the entire cornea [3]. The first of these may be most common and is thought to be due to the formation of pus filled troughs beneath the eyelids.
Currently, the CDC recommends combination therapy with a single intramuscular dose of ceftriaxone 250mg plus either a single dose of azithromycin 1g orally or doxycycline 100mg orally twice daily for 7 days for the treatment of uncomplicated urogenital, anorectal, and pharyngeal gonorrhea. In instances where ceftriaxone is not available, cefixime 400mg orally, plus either azithromycin 1g orally or doxycycline 100mg orally twice daily for 7 days should be used. For patients allergic to the cephalosporins, the CDC recommends use of a single 2g dose of azithromycin orally. In both of these circumstances, a test of cure for these patients should be carried out one week after treatment [4].
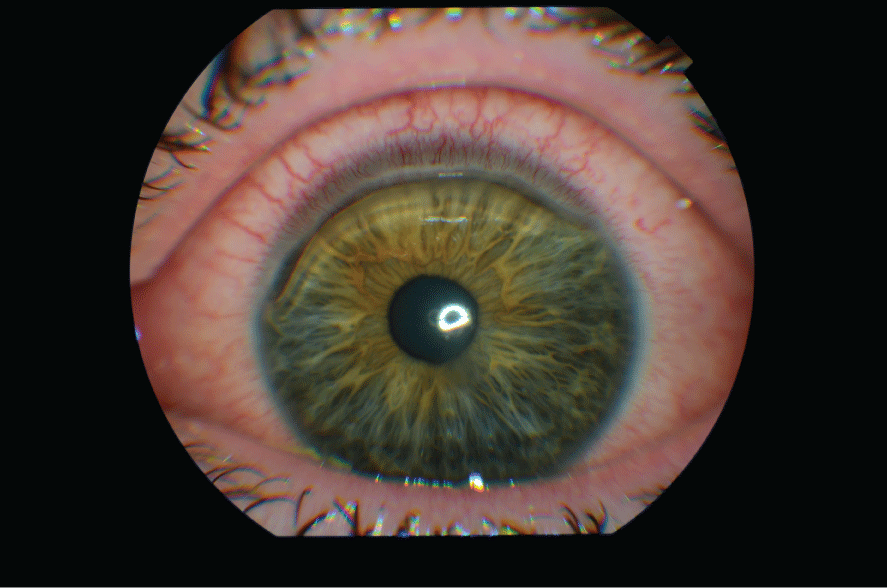
In that particular case of gonococcal keratitis described here the clinical appearance was very similar to an immune mediated peripheral corneal melt. Indeed, we were particularly impressed by the relative lack of stromal disease elsewhere in the cornea beyond the area of ulceration (Figure 2).
.
Figure 2: In this gentleman�s case the clinical appearance was very similar
to an immune mediated peripheral corneal melt. Note the relative lack of
stromal disease elsewhere in the cornea beyond the area of ulceration
superiorly.
View Figure 2
The influence of inflammatory cells and their enzymatic products in stromal destruction in auto-immune peripheral corneal melt is already well established [5]. The polymorphonuclear (PMN) cell is thought to be most important. Since the migration of PMN cells is from the limbal vasculature into the corneal stroma most immune mediated tissue damage is limbal. Neisseria gonorrhoea was not cultured from the cornea of eyes with severe gonococcal keratitis which were enucleated as might be expected were corneal penetration secondary to active bacterial replication [6]. Similarly, in our case, though an aggressive, extensive peripheral corneal melt persisted following the administration of antibiotics, we were unable to demonstrate the presence of organisms in specimens taken at conjunctival swab and corneal scrape. The relative role of the enzymatic products of the PMN cell in the pathogenesis of gonococcal keratitis is unknown but given the appearance of the cornea in the case we describe here we postulate that it is relatively great. Indeed the peripheral corneal ulceration resolved only when systemic corticosteroids were administered.
The successful use of topical corticosteroid in the treatment of a case of Neisseria gonorrhoeae keratitis which was associated with diffuse lamellar keratitis three years after laser in situ keratomileusis has already been described [7].
Rapid progression of an ulcerative keratitis to corneal perforation can reportedly occur within 24 h of infection with Neisseria gonorrhoeae [8]. Further, the outcome of this infection depends upon its severity when appropriate therapy is commenced [9]. �Appropriate� therapy in some cases may thus include topical and/or systemic corticosteroid despite their usual contraindication in cases of acute infective keratitis.
Conclusion
We hope this report will serve as a reminder of both the occurrence and indeed the potential severity of gonococcal eye disease. A sexual and genitourinary system history should be obtained from all those with a purulent ocular discharge. Severe gonococcal keratitis may be unilateral. This may behave like a peripheral corneal melt. Consequently topical and/or systemic steroid may be therapeutic.
References
-
Kawashima M, Kawakita T, Den S, Tomita M, Shimazaki J (2009) Surgical management of corneal perforation secondary to gonococcal keratoconjunctivitis. Eye (Lond) 23: 339-344.
-
Hegde V, Smith G, Choi J, Pagliarini S (2005) A case of gonococcal kerato-conjunctivitis mimicking orbital cellulitis. Acta Ophthalmol Scand 83: 511-512.
-
Wan WL, Farkas GC, May WN, Robin JB (1986) The clinical characteristics and course of adult gonococcal conjunctivitis. Am J Ophthalmol 102: 575-583.
-
Centers for Disease Control and Prevention (CDC) (2012) Update to CDC's Sexually transmitted diseases treatment guidelines, 2010: oral cephalosporins no longer a recommended treatment for gonococcal infections. MMWR Morb Mortal Wkly Rep 61: 590-594.
-
Kenyon KR (1985) Inflammatory mechanisms in corneal ulceration. Trans Am Ophthalmol Soc 83: 610-663.
-
Ullman S, Roussel TJ, Culbertson WW, Forster RK, Alfonso E, et al. (1987) Neisseria gonorrhoeae keratoconjunctivitis. Ophthalmology 94: 525-531.
-
Symes RJ, Catt CJ, Males JJ (2007) Diffuse lamellar keratitis associated with gonococcal keratoconjunctivitis 3 years after laser in situ keratomileusis. J Cataract Refract Surg 33: 323-325.
-
Duke-Elder S (1965) Diseases of the outer eye. In: System of Ophthalmology Vol. 8. Part 1.St. Louis: CV Mosby Co, USA.
-
Lee JS, Choi HY, Lee JE, Lee SH, Oum BS (2002) Gonococcal keratoconjunctivitis in adults. Eye (Lond) 16: 646-649.





