International Journal of Ophthalmology and Clinical Research
Congenital Retinal Macrovessel with Normal Visual Acuity: A Case Report
Harsimran K Bhatia*, Shekhar Sharma and Laxminarayana P
Department of Ophthalmology, ESIC Model Hospital, India
*Corresponding author: Harsimran K Bhatia (MBBS, DNB), Department of Ophthalmology, ESIC Model Hospital, Noida, Uttar Pradesh, India, Tel: +91-9811765926, E-mail: harsimran83@gmail.com
Int J Ophthalmol Clin Res, IJOCR-2-017, (Volume 2, Issue 2), Case Report; ISSN: 2378-346X
Received: February 09, 2015 | Accepted: March 05, 2015 | Published: March 12, 2015
Citation: Bhatia HK, Sharma S, Laxminarayana P (2015) Congenital Retinal Macrovessel with Normal Visual Acuity: A Case Report. Int J Ophthalmol Clin Res 2:017. 10.23937/2378-346X/1410017
Copyright: © 2015 Bhatia HK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Congenital retinal macrovessel is a large aberrant vessel discovered as an incidental finding. These aberrant vessels are mostly single, unilateral veins. CRMs do not affect vision unless there are associated foveolar cysts, foveal ectopia, pigmentary changes at fovea, macular haemorrhage, exudates, serous macular detachment or the macrovessel crosses the fovea. Thorough clinical evaluation and investigations are valuable in diagnosis and follow-up of such cases and aid in timely management of associated complications. In this report, we have discussed a case of CRM with unaffected visual acuity. To the best of our knowledge, such a case of CRM crossing fovea but sparing vision and findings substantiated by Spectral Domain Optical Coherence Tomography (OCT) has not been documented earlier.
Keywords
Congenital retinal macrovessels, Aberrant macrovessels, Visual acuity, Fluorescein angiography, Optical coherence tomography, Retinal thickness, Retinal pigment epithelium, Central macular thickness
Abbreviations
CRM: Congenital Retinal Macrovessel, SD OCT: Spectral Domain Optical Coherence Tomography, FA: Fluorescein Angiography, BCVA: Best Corrected Visual Acuity, RPE: Retinal Pigment Epithelium, CMT: Central Macular Thickness.
Introduction
Congenital retinal macrovessels are a rare finding. They are usually discovered as an incidental finding. The aberrant vessel can be an artery or a vein, the latter being more common [1]. The visual acuity remains unaffected in majority of the cases [1,2]. In this paper we have reported a case of congenital retinal macrovessel crossing the fovea but not affecting the visual acuity.
Case Report
A 16 years old female presented to our clinic for routine ophthalmic evaluation. Best corrected visual acuity (BCVA) in both eyes was 20/20. Anterior segment in both eyes revealed no abnormal findings. Posterior segment evaluation of right eye revealed an aberrant vessel originating at the optic nerve head and traversing temporally across the macula and involving the fovea. The calibre of the macrovessel was comparable to that of the veins and had numerous branches crossing the horizontal raphe. The rest of the fundus findings in both the eyes were normal with cup: disc ratio of 0.4:1 (Figure 1).
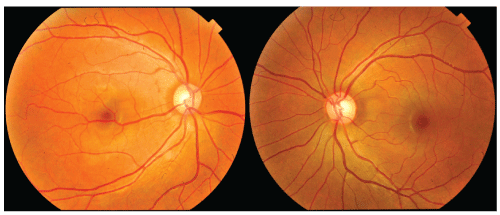
Figure 1: Right e ye - Retinal macrovessel originating at optic nerve head and crossing the fovea just inferior to foveola; Left eye - Normal retinal findings.
View Figure 1
Fluorescein angiography revealed the filling of the macrovessel starting in the arteriovenous phase as laminar flow with complete filling in the venous phase. The filling occurred earlier and emptying later than the rest of the veins. The macrovessel had numerous tributaries spread over the macula but the foveal avascular zone was just spared. There were no arteriovenous anastomoses or abnormal leakage points (Figure 2).
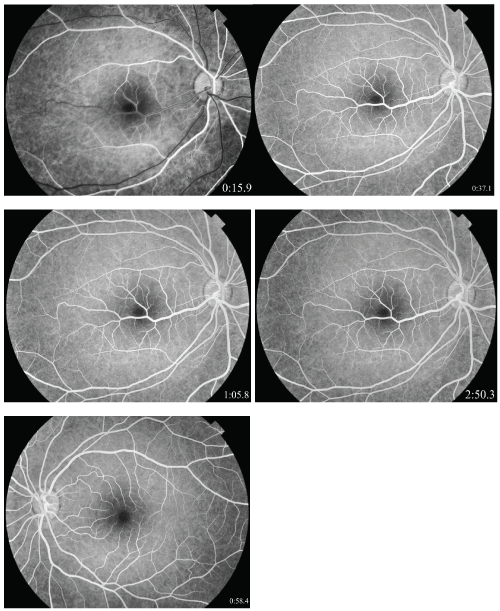
Figure 2: Fluorescein angiographs of right eye showing early filling of CRM with laminar flow and delayed emptying; no leakage, no arteriovenous anastomoses. Left eye shows normal findings.
View Figure 2
RTVue spectral domain OCT (Optovue Inc., Fremont, California, USA) analysis of the right eye revealed normal foveal contour in the radial scan. There was attenuation of signals in deeper retinal layers inferior to the fovea due to the hyper-reflective aberrant vessel. The retinal thickness maps of both the eyes revealed thickness within normal range. There was no evidence of foveal cysts, submacular detachment (Figure 3). Over 4 months of follow-up no changes have been noticed.
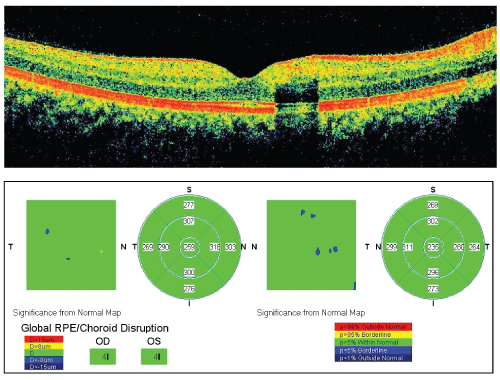
Figure 3: Above: RTVue SD OCT radial scan of right eye showing normal foveal contour, attenuation of signals in deeper retinal layers due to hyper-reflective CRM. Below: Retinal thickness map of both eyes showing normal retinal thickness.
View Figure 3
Discussion
Congenital retinal macrovessels (CRM) were first described by Mauthner in 1869 [3]. A century later in1969, Ashton explained the formation of congenital retinal macrovessels [4]. These vessels are of mesenchymal origin and develop around 15-16 weeks of gestation when differentiation of arteries and veins occurs. If foveal hypoxia occurs, vascular proliferation may reach foveola. CRM was defined by Brown in 1982 as the large aberrant vessel that crossed the horizontal raphe without affecting the visual acuity [1].
CRMs are mostly unilateral, single veins [1,5]. These vessels may supply or drain blood from both inferior and superior retina. In the case in discussion, the macrovessel was of venous origin as seen clinically and suggested by the laminar flow and complete filling in the venous phase on fluorescein angiography. Fewer cases have been reported of arteriolar origin of CRM. There have been reports of anomalous retinal arteries with leaking macroaneurysms causing macular oedema, haemorrhage and exudates and hence decreased vision [6,7]. A case of congenital retinal arterial macrovessel associated with congenital simple hamartoma of retinal pigment epithelium has also been reported [8].
Most of the cases of CRM that have come up so far have been associated with normal visual acuity [1,9,10]. Visual status tends to remain stable over long follow up periods [9-11]. Brown et al first reported 7 eyes with CRM all having normal vision [11]. de Crecchio et al have followed a case with impaired but stable visual acuity over 14 years [11]. The current case presented with normal visual acuity which has remained stable over 4 months of follow-up.
Visual acuity when affected can be attributed to the macrovessel crossing the foveola, foveolar cyst, foveal ectopia, pigmentary changes at fovea, macular haemorrhage, exudates or serous macular detachment [1-5,9,12,13]. In our patient, foveola was surrounded but not traversed by the macrovessel and its tributary and none of the above associations were noticed. Other proposed causes of decreased vision include macular thickening and distorted foveal architecture as seen on SD OCT [14,15]. Visual field analyses have revealed relative angioscotomas caused by decreased retinal sensitivity in the area crossed by the macrovessel [15,16]. In our subject, OCT revealed the shadow effect of the hyper-reflective vessel with normal foveal contour and no intraretinal or subretinal fluid. The macular thickness was within normal range in both the eyes.
Few authors have reported the occurrence of central serous chorioretinopathy in such cases [17-20]. The decompensation of an otherwise stable macrovessel has been associated with the alteration of pressure (Valsalva manoeuvre) or gravitational forces (roller-coaster rides or bungee jumping) [21,22]. Branch retinal artery occlusion occurring as a result of ischemic decompensation of CRM has also been discussed recently [23]. Amblyopia can occur in children by these vessels crossing fovea [24].
Fluorescein angiography reveals certain characteristic findings of CRMs which may include early filling and delayed emptying of the vessel, arteriovenous anastomoses, capillary non perfusion, hyperfluorescence associated with RPE alterations and vascular leakage [1,2,5]. Except the early filling and delayed emptying, none of the other findings were seen in the case in discussion.
CRMs can mimic certain vascular anomalies like capillary hemangiomas, racemose angiomas, retinal venous collaterals following venous occlusions and tumours like malignant melanoma and retinoblastoma [1,3,6]. Cavernous hemangiomas have also been found to coexist with such macrovessels [25]. Microvascular anomalies with CRMs have been reported in a case of neurofibromatosis-I [26]. In our case no anomalies were noted in the retinal vasculature. There also exists a possibility of brain vascular anomalies like Wyburn-Masson syndrome so neurological studies should be considered [1,3,5].
The limitation in our case was the visual field analysis, though performed by the young subject could not fetch us useful results due to highly unreliable indices. The follow-up period of 4 months is too short and it would be interesting to look for any new developments over a longer duration.
Conclusion
CRMs are a rare and incidental finding. Thorough clinical examination, fluorescein angiography and OCT are essential in the diagnosis and management of such cases. Although a rare occurrence, visual acuity may remain unaffected even with the macrovessel crossing the fovea. Regular follow-up is an important aspect to appropriately manage cases developing complications associated with CRMs.
Acknowledgement
I am grateful to Dr. Mohit Bhatia for providing assistance in writing and editing this manuscript.
References
-
Brown GC, Donoso LA, Magargal LE, Goldberg RE, Sarin LK (1982) Congenital retinal macrovessels. Arch Ophthalmol 100: 1430-1436.
-
VOLK D (1956) Visual function studies in a case of large aberrant vessels in the macula. AMA Arch Ophthalmol 55: 119-122.
-
Mauthner L (1869) Lehrbuch der Ophthalmoscopie. Vienna: Tendler, Co: 249.
-
Ashton N (1970) Retinal angiogenesis in the human embryo. Br Med Bull 26: 103-106.
-
de Crecchio G, Mastursi B, Alfieri MC, Pignalosa B (1986) Congenital retinal macrovessel. Ophthalmologica 193: 143-145.
-
Chalam KV, Gupta SK, Vinjamaram S, Shah VA (2003) Clinicopathologic reports, case reports, and small case series: congenital anomalous retinal artery associated with a leaking macroaneurysm. Arch Ophthalmol 121: 409-410.
-
Musadiq M, Gibson JM (2010) Spontaneously resolved macroaneurysm associated with a congenital anomalous retinal artery. Retin Cases Brief Rep 4: 70-72.
-
Souissi K, E Afrit MA, Kraiem A (2006) Congenital retinal arterial macrovessel and congenital hamartoma of the retinal pigment epithelium. J Pediatr Ophthalmol Strabismus 43: 181-182.
-
Chronister CL, Nyman NN, Meccariello AF (1991) Congenital retinal macrovessel. Optom Vis Sci 68: 747-749.
-
Petropoulos IK, Petkou D, Theoulakis PE, Kordelou A, Pournaras CJ, et al. (2008) Congenital retinal macrovessels: description of three cases and review of the literature. Klin Monbl Augenheilkd 225: 469-472.
-
de Crecchio G, Pacente L, Alfieri MC, Pignalosa G, Greco GM (1999) Congenital retinal macrovessels: a "low visual acuity" case report with a 14-year follow-up. Acta Ophthalmol Scand 77: 474-475.
-
Gurwood AS, Bailey JT, Pelino CJ (2001) Congenital retinal macrovessel: a case report. Optometry 72: 597-602.
-
Polk TD, Park D, Sindt CW, Heffron ET (1997) Congenital retinal macrovessel. Arch Ophthalmol 115: 290-291.
-
de Crecchio G, Pappalardo G, Pascotto F, Forte R (2006) Aberrant congenital macular vessel crossing the fovea: evaluation with optical coherence tomography. Eye (Lond) 20: 1464-1466.
-
Ceylan OM, Gullulu G, Akin T, Bilen H (2011) Congenital retinal macrovessel: atypical presentation using optical coherence tomography. Int Ophthalmol 31: 55-58.
-
Shah VA, Chalam KV (2004) Congenital retinal macrovessel causes reduced retinal sensitivity at the macula. Eur J Ophthalmol 14: 341-344.
-
Arai J, Kasuga Y, Koketsu M, Yoshimura N (2000) Development and spontaneous resolution of serous retinal detachment in a patient with a congenital retinal macrovessel. Retina 20: 674-676.
-
Kumar V, Ghosh B, Raina U, Goel N (2009) Central serous chorioretinopathy in a patient with congenital retinal macrovessel. Can J Ophthalmol 44: e57.
-
Laktaoui A, Louaya S, Zerrouk R, Fiqhi A, Bouia Y, et al. (2010) [Congenital retinal macrovessel associated with central serous retinopathy]. J Fr Ophtalmol 33: 573.
-
Ascaso FJ (2011) Spontaneous resolution of central serous chorioretinopathy in a patient with congenital retinal macrovessel. Circulation 124: e904-905.
-
de Crecchio G, Pacente L, Alfieri MC, Greco GM (2000) Valsalva retinopathy associated with a congenital retinal macrovessel. Arch Ophthalmol 118: 146-147.
-
Beatty S, Goodall K, Radford R, Lavin MJ (2000) Decompensation of a congenital retinal macrovessel with arteriovenous communications induced by repetitive rollercoaster rides. Am J Ophthalmol 130: 527-528.
-
Goel N, Kumar V, Seth A, Ghosh B (2014) Branch retinal artery occlusion associated with congenital retinal macrovessel. Oman J Ophthalmol 7: 96-97.
-
P�rez-Carro G, Miranda-Roll�n M, Junceda-Moreno C, Alvarez-S�nchez M, Junceda-Moreno J (2008) [Congenital retinal macrovessels: a discovery by chance]. Arch Soc Esp Oftalmol 83: 273-276.
-
Bru� C, Vance SK, Yannuzzi LA, Freund KB (2011) Cavernous hemangioma associated with retinal macrovessels. Retin Cases Brief Rep 5: 323-325.
-
Makino S, Endoh K, Tampo H (2013) Retinal microvascular abnormalities in neurofibromatosis type 1 associated with congenital retinal macrovessels. Case Rep Ophthalmol Med 2013: 604191.





