International Journal of Clinical Cardiology
Intravenous Immunoglobulins in the Management of Parvovirus B19 Induced Fulminant Myocarditis: Case Report
Maysa Saleh1* and Samir Sajwany2
1Pediatric department, Latifa hospital, Dubai Health authority, United Arab Emirates
2Consultant pediatric and Cardiology, Latifa hospital, Dubai Health authority, United Arab Emirates
*Corresponding author:
Maysa Saleh, Pediatric department, Latifa hospital, Dubai Health authority, United Arab Emirates, E-mail: maytawsal@yahoo.com
Int J Clin Cardiol, IJCC-4-094, (Volume 4, Issue 2), Case Report; ISSN: 2378-2951
Received: October 03, 2016 | Accepted: March 29, 2017 | Published: April 01, 2017
Citation: Saleh M, Sajwany S (2017) Intravenous Immunoglobulins in the Management of Parvovirus B19 Induced Fulminant Myocarditis: Case Report. Int J Clin Cardiol 4:094. 10.23937/2378-2951/1410094
Copyright: © 2017 Saleh M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Myocarditis is an inflammatory cardiomyopathy with variable presentations, ranging from mild symptoms with spontaneous recovery, to dilated cardiomyopathy (DCM), severe heart failure or early death [1,2].
Myocarditis may progress to form DCM due to the direct myocardial injury mediated by the virus or secondary to autoimmune process [3]. Hence, the most common viruses, inducing acute myocarditis in developed countries, are parvovirus (PVB19), enteroviruses and human herpes virus 6 [4].
Moreover, parvovirus B19 may induce myocardial injury directly or with secondary autoimmunity through molecular mimicry, where a cross-reaction becomes available between the viral peptides and the antigens intrinsic to the myocardium [5,6].
Here in, we report the two cases, which were presented with parvovirus B19 induced acute myocarditis and have been successfully treated with intravenous immunoglobulins administration during the acute phase of heart failure.
Keywords
Myocarditis, Parvovirus B19, Cardiomyopathy
Case Presentation
Case I
One-year-old boy was admitted to a hospital suffering from acute myocarditis, dilated cardiomyopathy and congestive heart failure. He was experiencing vomiting for 2 days, breathing difficulty and poor oral intake. In view of deterioration of his condition that has required ventilator support, inotropes, anti-failure medications and antibiotics, hence, he was transferred to our hospital.
Regarding his birth history, he was born 31/52 weeks, when he was admitted to NICU for 37 days in view of respiratory distress.
On admission to our hospital, the child was put on ventilator, afebrile. His physical examination demonstrated signs of compromised circulation (cold peripheries and prolonged capillary refill (4 seconds). Heart rate was 134/minutes, blood pressure77/54 mmHg), SpO2 100%. His growth and development were acceptable with weight just above 3rd centile and length 50-90 centile and head circumference < 3rd centile. In addition, cardiovascular examination showed normal heart sound with pan-systolic murmur II/VI at the apex. Meanwhile, Chest: decreased air entry on the right side. Abdomen was soft with liver 4 cm below costal margins. The child was sedated with pupil equal and reactive. Chest x-ray showed consolidation of the right lung associated with right pleural effusion with cardiothoracic ratio; 0.62. ECHO showed severe ventricular dysfunction with FS 15%, and poor contractility. Thorough investigation was done which showed positive Parvovirus IgM and DNA PCR.
Investigations: Laboratory investigations revealed white blood cell (WBC) count 15200/mm3) haemoglobin 8.4, platelet 84000/mm3, C-reactive protein (CRP) 35 mg/dL, disturbed coagulation; Prothrombin time (PT) 18.8 secs, Activated partial thromboplastin time (APTT) 34.8 secs. The cardiac enzymes was elevated CPK 1027 U/L, CKMB 72 u/l, CPK CKMB ratio 7, troponin 0.49 ng/ml. Virology screening (Coxsackie, Epstein Barr, Cytomegalovirus, Echovirus, Enterovirus, Herpes virus 6 & 7, and Adenovirus) were all-negative. Parvovirus IgM as well as Parvovirus B19 DNA PCR were positive. Liver function test revealed normal results.
Chest X-ray showed initially cardiomegaly with cardiothoracic ratio of 0.62, and consolidation of the right lung associated with right pleural effusion. 10 days later, Chest X-ray showed resolution of pneumonia with cardiomegaly was traced with no evidence of edema.
Chest ultrasound was done on admission, which showed moderate right side pleural effusion which was repeated after 3 days and no effusion were seen.
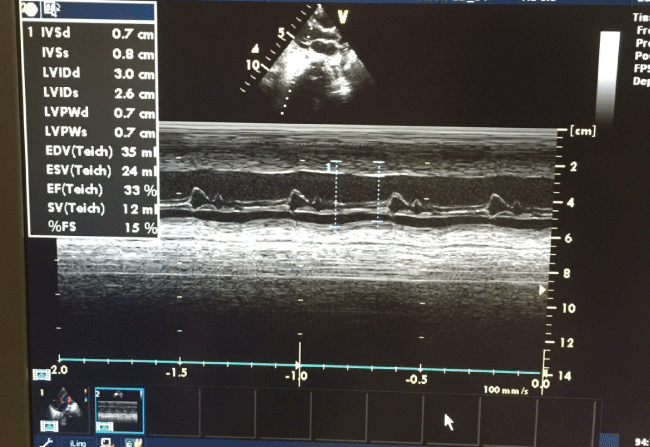
ECG showed low voltage. Besides, an echocardiogram (ECHO) noted severe ventricular dysfunction with FS 15%, and poor contractility (Figure 1a), which were improved on follow up.
Treatment: The child continued on two inotropes (dopamine and dobutamine) infusion in addition to furosemide, and ceftriaxone. Accordingly, he received packed red blood cells transfusion and one dose of intravenous immunoglobulins (2 g/kg). After three days, dopamine was replaced with Milrinone along with captopril.
Outcome and follow up: The child's case had been stabilized and extubated after 7 days. His general condition gradually improved. Repeated ECHO showed improving myocarditis, FS 22%. Milirinone was gradually tappered. Fifteen days later, the child was discharged from hospital on furosemide and captopril.
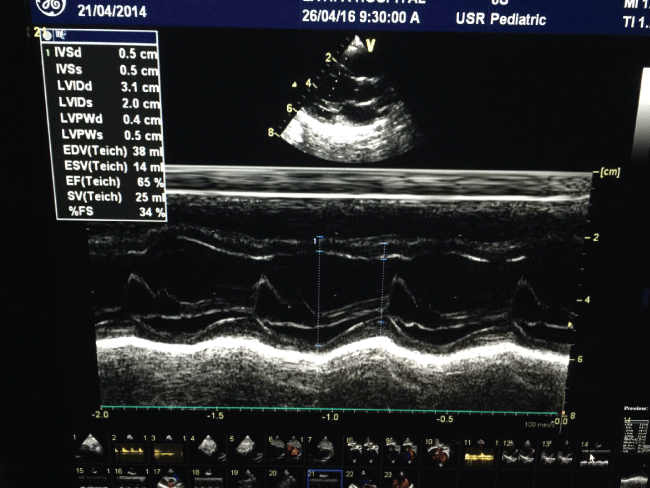
At 1-month follow-up, the patient remained asymptomatic and with ECHO reflected an improved cardiac function, FS 27%. Six months later, repeated ECHO showed improved myocarditis with FS 34% (Figure 1b), he was advised to continue on having captopril and furosemide.
Case II
9-months-old girl, previously healthy, was presented with vomiting and drowsiness after head trauma 5 days prior to admission; however, CT scan brain was normal. She had History of viral illness 9 days back. Upon admission, she was conscious, alert, mildly distressed, dehydrated, with normal systemic examination. Chest x-ray was initially normal. Two days later, she became more distressed with abdominal distention, still vomiting. In view of deterioration of general condition and being tachypneic and distressed, ECHO was done which showed myocarditis with ejection fraction of 14%. A repeated chest X-ray showed bilateral pleural effusion-more on the right side. The child shifted to the PICU. She was hooked to mechanical ventilation, started on milrinone, Furosemide, IV ceftriaxone with fluid restriction. Intravenous immunoglobulin was given in dose of 2 gm/kg once. She improved gradually, captopril was added and milrinone tapered. She was gradually weaned off ventilator (5 days).
Investigations: Laboratory investigations revealed; white blood cell (WBC) count 25.3 × 10^3/uL (N: 6.0-18.0) haemoglobin 9.1 (N: 11.1-14.1), Red blood cells: 4.35 × 10^6/uL ( N: 4.10-5.30 ), platelet 490 × 10^3/uL (N: 200-550) , Absolute neutrophil 10.4 c 10^3/uL (N: 1.0-7.0), absolute lymphocytes 13.4 × 10^3/uL (N: 4.0-10.0), absolute monocytes 1.2 × 10^3/uL (N: 0.2-1.2 ), absolute eosinophils 0.1 × 10^3/uL (N: 0.1-1.0).
C-reactive protein (CRP) 35 mg/dL (N: < 5), disturbed coagulation; Prothrombin time 19.6 secs (N:, Activated partial thromboplastin time 27.9 secs. INR: 1.78. The cardiac enzymes was elevated CPK 288 U/L (N: 0-228), CKMB 155 u/l , CPK CKMB ratio 54% (N: < 6), troponin 1.42 ng/ml. lactic acid: 2.6 mmol/l (N: 0.5-2.2).
Virology screening (Coxsackie, Epstein Barr, Cytomegalovirus, Echovirus, Enterovirus, Herpes virus 6&7, and adenovirus) was negative. Parvovirus IgM as well as Parvovirus B19 DNA PCR were positive. Liver function test was normal.
Radiological examination: Chest X-ray initially normal. One day later, it revealed bilateral pleural effusion-more on the right side. Resolution of the effusion has been notedwithin one week.
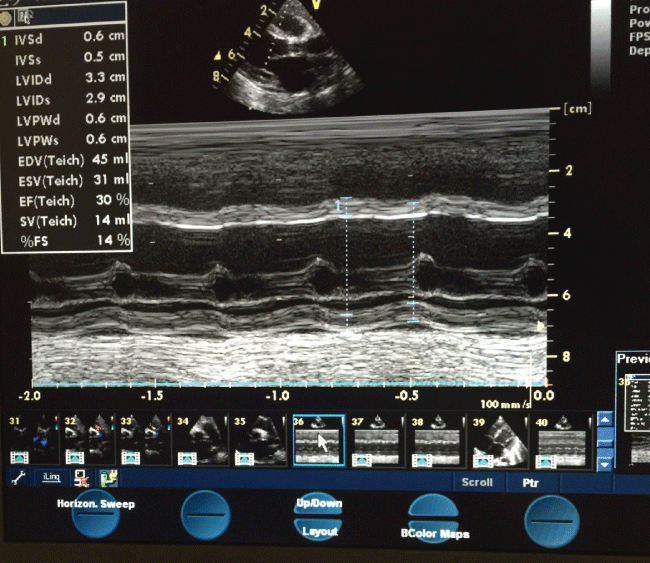
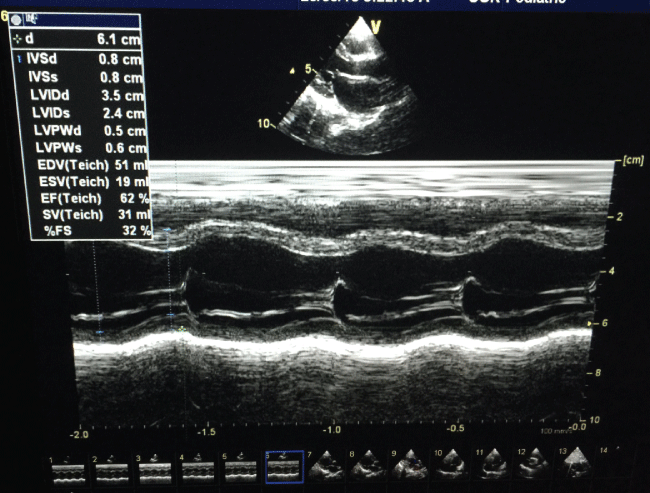
Initial ECHO showed severe left ventricular dysfunction with poor contractility, with dilated right ventricle, myocarditis, moderate mitral and tricuspid regurge, FS 14% (Figure 2a). Three weeks later, Myocarditis was improved with normal heart function. FS 38%. Six months follow up showed normal left ventricle function, no mitral regurge, FS 32%, EF 63% (Figure 2b).
Discussion
This report has illustrated PVB19-induced myocarditis leading to severe cardiac dysfunction. The peculiarity of this report was due to the effectiveness of immunoglobulin administration in high dose in two infants who suffered parvovirus induced severe myocarditis, dilated cardiomyopathy and severe heart failure. Immunoglobulin therapy (single high dose) in addition to conventional heart failure therapy and ventilatory support has been able to improve cardiac function in these patients.
According to the World Health Organization/International Society and Federation of Cardiology, myocarditis is a disease of the heart muscle with an inflammatory process [7]. Though, numerous infectious agents are accused to be the primary cause of its evolution, yet autoimmune disease, hypersensitivity or toxins may also play a role. The diagnosis of myocarditis is established by histological, immunological as well as inflammatory criteria [8].
The use of IVIG in cases of viral myocarditis in children is still a controversy. However, its use is widely spread. A systematic review was done in 2005 to evaluate the use of IVIG in acute myocarditis. There was inconclusive evidence about the use of IVIG in those children [9,10]. Furthermore, a single center [8] and multicenter studies [11] of acute myocarditis in children were discerned about the benefits of using IVIG therapy for them.
However, based on the direct and the secondary autoimmune effect of PVB19 on the myocardium, it is beneficial to try IVIG to block the evolution of end stage form of DCM early in the management of viral induced myocarditis in pediatric age group.
Conclusion
In our case report, the children have been markedly improved with single high dose of IVIG. Thesetwo cases illustrate PVB19-induced myocarditis leading to severe cardiac dysfunction. Parvovirus B19 infection could lead to direct myocardial injury, and could trigger a severe autoimmune reaction of the myocardium. Immunoglobulin therapy in addition to conventional heart failure therapy is able to improve cardiac function in patients to perform the same treatment modality obtaining an early improvement in left ventricular performance. The peculiarity of these two cases is specifically the effectiveness of immunoglobulin administration in the acute phase of heart failure induced by Parvovirus.
Learning Points/Recommendations
According to this report, it is now time to intensify the diagnostic tools in order to get an early etiologic diagnosis of myocarditis and to perform dedicated treatment options that could promptly restore an acute cardiac impairment and block the possible evolution towards end-stage forms of dilated cardiomyopathy. We also stress on having more research regarding the use of high dose intravenous immunoglobulins for early management of viral induced myocarditis in children.
References
-
Aretz HT, Billingham ME, Edwards WD, Factor SM, Fallon JT, et al. (1987) Myocarditis. A histopathologic definition and classification. Am J Cardiovasc Pathol 1: 3-14.
-
Lieberman EB, Hutchins GM, Herskowitz A, Rose NR, Baughman KL (1991) Clinicopathologic description of myocarditis. J Am Coll Cardiol 18: 1617-1626.
-
Afanasyeva M, Georgakopoulos D, Rose NR (2004) Autoimmune myocarditis: cellular mediators of cardiac dysfunction. Autoimmun Rev 3: 476-486.
-
Dennert R, Crijns HJ, Heymans S (2008) Acute viral myocarditis. Eur Heart J 29: 2073-2082.
-
Lunardi C, Tinazzi E, Bason C, Dolcino M, Corrocher R, et al. (2008) Human parvovirus B19 infection and autoimmunity. Autoimmun Rev 8: 116-120.
-
Kuhl U, Pauschinger M, Seeberg B, Lassner D, Noutsias M, et al. (2005) Viral persistence in the myocardium is associated with progressive cardiac dysfunction. Circulation 112: 1965-1970.
-
Richardson P, McKenna W, Bristow M, Maisch B, Mautner B, et al. (1996) Report of the 1995 World Health Organization/International Society and Federation of Cardiology Task Force on the Definition and Classification of Cardiomyopathies. Circulation 93: 841-842.
-
Canter CE, Simpson KE (2014) Diagnosis and Treatment of Myocarditis in Children in the Current Era. Circulation 129: 115-128.
-
English RF, Janosky JE, Ettedgui JA, Webber SA (2004) Outcomes for children with acute myocarditis. Cardiol Young 14: 488-493.
-
Joan L Robinson, Lisa Hartling, Ellen Crumley, Ben Vandermeer, Terry P Klassen (2005) A systematic review of intravenous gamma globulin for therapy of acute myocarditis. BMC Cardiovasc Disord 5: 12.
-
Klugman D, Berger JT, Sable CA, He J, Khandelwal SG, et al. (2010) Pediatric patients hospitalized with myocarditis: a multi-institutional analysis. Pediatr Cardiol 31: 222-228.