International Journal of Clinical Cardiology
Transcatheter Closure of Large Bilateral Coronary Arteriovenous Fistulae using Amplatzer Vascular Plugs
Akika Ando1*, Adnan Bhopalwala2 and Christian Spies2
1Department of Internal Medicine, John A. Burns School of Medicine, University of Hawaii, USA
2Department of Cardiology, University of Hawaii, Honolulu, USA
*Corresponding author: Akika Ando, MD, Department of Medicine, John A. Burns School of Medicine, University of Hawaii, 1356 Lusitana Street, 7th Floor, Honolulu, HI 96813-2427, USA, Tel: (808) 271-0787, E-mail: akika@hawaii.edu
Int J Clin Cardiol, IJCC-3-080, (Volume 3, Issue 1), Case Report; ISSN: 2378-2951
Received: April 16, 2016 | Accepted: June 20, 2016 | Published: June 23, 2016
Citation: Ando A, Bhopalwala A , Spies C (2016) Transcatheter Closure of Large Bilateral Coronary Arteriovenous Fistulae using Amplatzer Vascular Plugs. Int J Clin Cardiol 3:080. 10.23937/2378-2951/1410080
Copyright: © 2016 Ando A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A coronary arteriovenous (AV) fistula is defined as a connection between one or more coronary arteries and a cardiac chamber or great vessel, bypassing the myocardial capillary bed. For symptomatic patients, surgical intervention is the standard treatment plan. Recently, the use of transcatheter vascular plugs for the percutaneous closure of coronary AV fistulae has been reported in a few selected cases. We report the case of a 66-year-old woman with diffusely ectatic right and left coronary AV fistulae that drained into the main pulmonary artery. Using two 8 mm Amplatzer vascular plugs, the large fistulae were successfully closed percutaneously. Transcatheter vascular plugs may be a useful and less invasive treatment alternative to surgery for massive coronary AV fistulae.
Keywords
Coronary arteriovenous fistula, Angina, Percutaneous closure, Transcatheter vascular plug
Introduction
A coronary arteriovenous (AV) fistula is a rare anomaly that involves an abnormal communication between the coronary artery and one of the cardiac chambers or vessels adjacent to the heart [1]. Patients may present with signs of heart failure, arrhythmia, syncope, angina, and, rarely, endocarditis. We present a case of large and extensively tortuous coronary AV fistulae involving the left main and right coronary arteries that was successfully treated with transcatheter vascular plugs.
Case Report
A 66-year-old woman was referred to our clinic for a complaint of angina that was induced by walking one or two level blocks (Canadian class III) [2]. Computed tomography angiography (CTA) and coronary angiography, which had been performed at another hospital, revealed two large AV fistulae that drained into the pulmonary artery; one fistula originated from the left main coronary artery and the other from the right coronary artery (RCA). She was recommended to have open heart surgery, but she opted for a second opinion and consulted our clinic for possible percutaneous treatment.
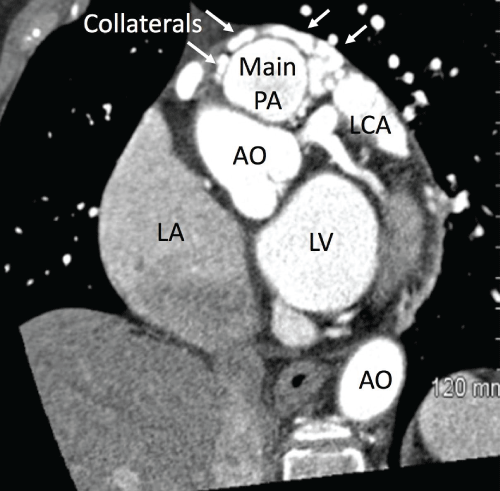
She had a medical history of hypertension, hyperlipidemia, type 2 diabetes mellitus, and mild pulmonary hypertension. On physical examination, there was a grade 3 continuous murmur that was heard best at the left sternal border. Electrocardiography showed normal sinus rhythm without any other changes. Follow-up CTA at our institution, Queens Medical Center, showed diffusely ectatic right and left coronary arteries with large collateral arteries and confirmed an anomalous connection between the coronary arteries and the main pulmonary artery, approximately 10 mm distal to the pulmonic valve, with possible multiple draining sites (Figure 1). Her angina was thought to be secondary to coronary steal phenomenon based on the large size of the fistulae. We decided to attempt occlusion of the fistulae using Amplatzer vascular plugs (St. Jude Medical, Minnesota, USA) because the patient declined surgical treatment.
.
Figure 1: Computed tomography angiogram of the chest showing large collateral arteries (arrows) with an anomalous connection between the coronary arteries and the main pulmonary artery (main PA), at approximately 10 mm distal to the pulmonic valve. AO: aorta; LCA: left coronary artery; LA: left atrium; LV: left ventricle
View Figure 1
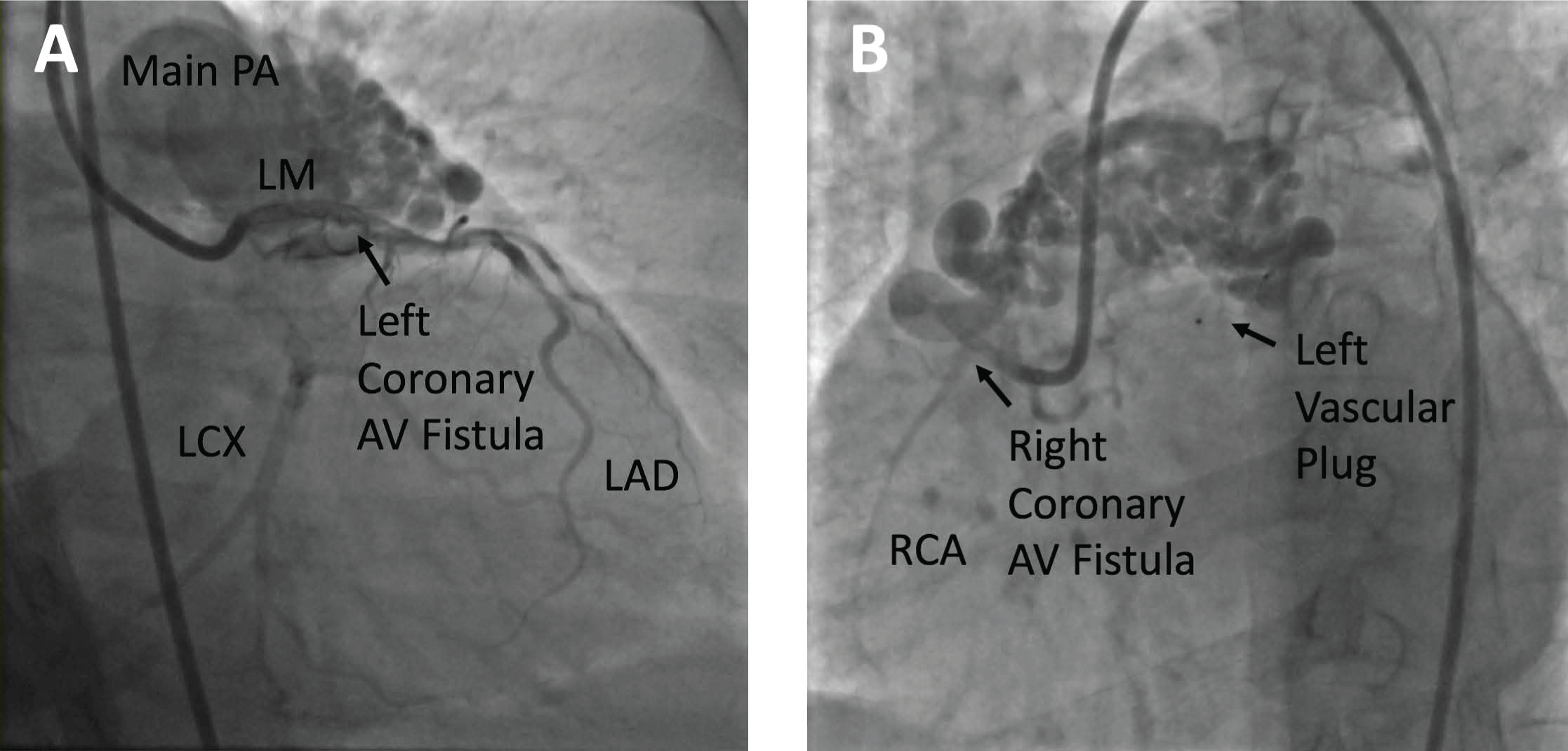
After the administration of local anesthetics, vascular access was attained via the right femoral artery and left femoral vein using 8F and 6F angiography catheters, respectively. Right heart catheterization with a shunt run was first performed. There was an increase in oxygen saturation from the right ventricle (66%) to the main pulmonary artery (72%). In addition, a left-to-right shunt was noted with a Qp/Qs ratio of 1.3/1. Coronary angiography revealed the large and extensively tortuous coronary AV fistulae draining into the main pulmonary artery (Figure 2). The left-to-right shunt was so extensive that the entire pulmonary artery was outlined with coronary injections, and it was difficult to fill the left circumflex artery due to the shunting. One fistula originated from the distal left main/proximal left anterior descending artery (LAD) and the other fistula originated from the proximal RCA.
.
Figure 2: A) Prior to treatment, selective left coronary angiogram in the caudal right anterior oblique (RAO) projection shows the left main (LM) coronary artery, the left circumflex (LCX) artery, and a large and extensively tortuous left coronary arteriovenous fistula draining into the main pulmonary artery (main PA); B) Prior to treatment, selective right coronary angiogram in the left anterior oblique (LAO) projection shows a small right coronary artery (RCA) and a large and extensively tortuous RCA AV fistula draining into the main PA. Also seen is the vascular plug on the left side after deployment of the plug.
View Figure 2
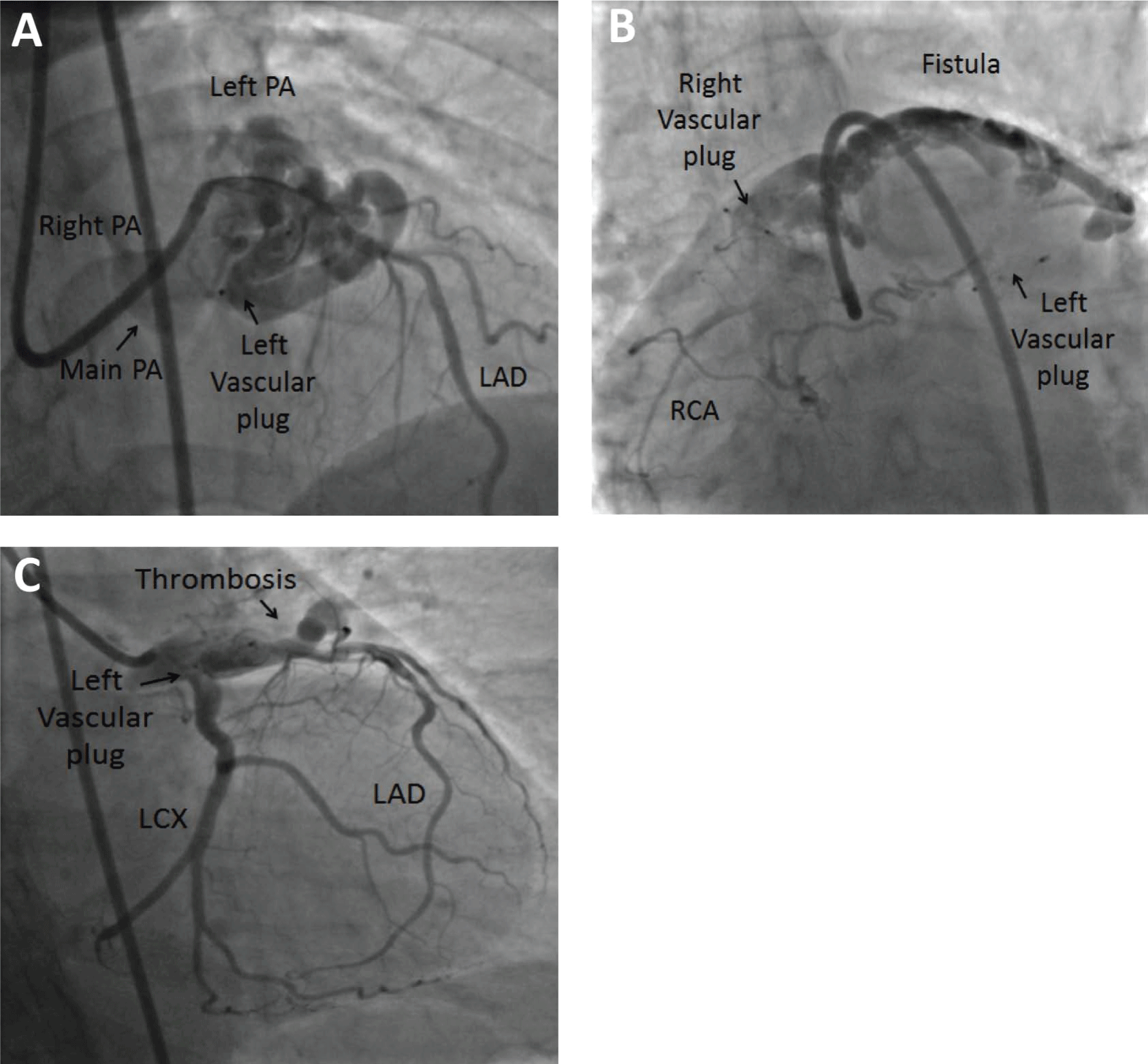
The intention was to use vascular plugs to obliterate each fistula in its narrowest segment. We decided to use an antegrade approach because of the presence of multiple drainage sites in the pulmonary artery. Prior CTA measurements showed an AV fistulous tract with a diameter of 6.5 mm. A Prowater flex wire (Abbott Vascular, CA, USA) was maneuvered into the AV fistula; a Piggyback 0.035-inch wire converter (Vascular solutions, MN, USA) was also advanced into the fistula. Over this wire, a 5F 100 cm JR4 guiding catheter (Medtronic, Ireland) was advanced into the fistula, with subsequent removal of the wire. An 8 mm Amplatzer Vascular Plug 4 was then prepared according to the manufacturer’s recommendation, after which it was advanced and deployed in the proximal portion of the fistula. Several repositioning attempts were made until a stable and occlusive position was reached. After this procedure, coronary angiography confirmed the placement of the plug at approximately 2-3 mm distal to the takeoff of the LAD. The plug was then released, and it remained in a stable position (Figure 3).
.
Figure 3: A) After deployment of an 8 mm Amplatzer vascular plug, selective left coronary angiogram in the cranial right anterior oblique (RAO) projection shows the occluded AV fistula, LAD, main pulmonary artery (PA), left PA, and right PA; B) After vascular plug deployment, selective right coronary angiogram in the anterior–posterior projection shows partial thrombosis of the fistula; C) Final selective left coronary angiogram in the caudal RAO projection reveals improved flow to the left anterior descending artery (LAD) and left circumflex (LCX) artery because of less steal phenomenon and partial thrombosis of the AV fistula.
View Figure 3
We then treated the RCA fistula with a similar technique. We changed the 5F 100 cm JR4 guiding catheter to an 8F 90 cm AL-1 guiding catheter (Medtronic, MN, USA) for establishing support. An 8 mm Amplatzer vascular plug was placed in the proximal portion of this AV fistula. A stable position was ensured, and the plug was released. Although the fistulae were not completely occluded, final coronary angiography showed unobstructed and improved flow down the coronary arteries, owing to less steal phenomenon and partial thrombosis of the AV fistulae. The patient’s post-procedural recovery was uneventful, and she was discharged from the hospital on the third day. After the procedure, the patient had complete resolution of anginal symptoms and the heart murmur; she was in excellent condition at the 6 month follow-up.
Discussion
A coronary AV fistula is defined as a connection between one or more coronary arteries and a cardiac chamber or great vessel, bypassing the myocardial capillary bed. The first pathologic account of this condition was published in 1908 by Maude Abbott [3]. Coronary artery fistulae are occasionally observed during coronary angiography (0.3%-0.8%). Approximately 60% of coronary artery fistulae are from the RCA, 35% are from the left coronary artery (LAD or left circumflex artery), and 5% are bilateral [4,5].
Most coronary artery fistulae are small, usually asymptomatic, can spontaneously resolve, and are clinically undetectable unless echocardiography or coronary arteriography is performed for an unrelated cause. However, larger fistulae are usually three times the size of a normal-caliber coronary artery; these may or may not cause symptoms or complications. Symptoms depend on the amount of shunt and/or the presence of coronary steal phenomenon [6]. Once patients become symptomatic, coronary AV fistulae result in a poor prognosis [7]. Early closure is recommended for symptomatic patients at all ages [8,9]. The surgical ligation of coronary artery fistulae is usually the first-line treatment. However, the transcatheter closure of coronary artery fistulae with coiling and other devices has become an attractive alternative to surgery since the first published report in 1983 [10].
Our case showed large and extensively tortuous coronary AV fistulae involving the left main coronary artery. Occlusion with two 8 mm vascular plugs resulted in the complete resolution of angina and clinical improvement. Armsby et al. reported no further late complications or late deaths at 1 year after transcatheter closure; complete closure of the fistulae was observed in 91% of the analyzed patients [11].
Conclusion
Transcatheter closure of coronary artery fistulae, especially if large, may be a great alternative to surgery in populations such as the elderly who are considered non-surgical candidates because of multiple comorbidities.
References
-
Levin DC, Fellows KE, Abrams HL (1978) Hemodynamically significant primary anomalies of the coronary arteries. Angiographic aspects. Circulation 58: 25-34.
-
Campeau L (1976) Letter: Grading of angina pectoris. Circulation 54: 522-523.
-
De Santis A, Cifarelli A, Violini R (2010) Transcatheter closure of coronary artery fistula using the new Amplatzer vascular plug and a telescoping catheter technique. J Cardiovasc Med (Hagerstown) 11: 605-609.
-
Renard C, Chivot C, Jarry G, Houpe D, Rémond A, et al. (2010) Communicating bilateral coronary artery to pulmonary artery fistula with aneurysm in asymptomatic patient: successful conservative management with selective coil embolization of the aneurysm. Int J Cardiol 150: e107-109.
-
Hoffman J (1995) Congenital anomalies of the coronary vessels and the aortic root. In: Emmanoulides G, Reimenschneider TA, Allen HD, Gutgesell HP, Heart disease in infants, children and adolescents (5th edn), Williams and Wilkins, Baltimore.
-
Testuz A, Roffi M, Bonvini RF (2011) Coronary to pulmonary artery fistulas: an incidental finding with challenging therapeutic options. J Invasive Cardiol 23: E177-180.
-
Sherwood MC, Rockenmacher S, Colan SD, Geva T (1999) Prognostic significance of clinically silent coronary artery fistulas. Am J Cardiol 83: 407-411.
-
Balanescu S, Sangiorgi G, Castelvecchio S, Medda M, Inglese L (2001) Coronary artery fistulas: clinical consequences and methods of closure. A literature review. Ital Heart J 2: 669-676.
-
Latson LA (2007) Coronary artery fistulas: how to manage them. Catheter Cardiovasc Interv 70: 110-116.
-
Reidy JF, Sowton E, Ross DN (1983) Transcatheter occlusion of coronary to bronchial anastomosis by detachable balloon combined with coronary angioplasty at same procedure. Br Heart J 49: 284-287.
-
Armsby LR, Keane JF, Sherwood MC, Forbess JM, Perry SB, et al. (2002) Management of coronary artery fistulae. Patient selection and results of transcatheter closure. J Am Coll Cardiol 39: 1026-1032.





