International Journal of Clinical Cardiology
Left Ventricular Assist Device Placement through Left Thoracotomy in Difficult Scenarios
Lyndsay M. Mueller1, Samuel H. Cho1*, Timothy Fritz2 and Asghar Khaghani2
1Michigan State University College of Human Medicine, Grand Rapids, Michigan, USA
2Spectrum Health Frederik Meijer Heart & Vascular Institute, Grand Rapids, Michigan, USA
*Corresponding author: Samuel H. Cho, Michigan State University College of Human Medicine, Grand Rapids, 639 N. Broadway Apt 510, Los Angeles, California USA, 90012, E-mail: sam77cho@gmail.com
Int J Clin Cardiol, IJCC-3-069, (Volume 3, Issue 1), Case Report; ISSN: 2378-2951
Received: September 04, 2015 | Accepted: January 14, 2016 | Published: January 18, 2016
Citation: Mueller LM, Cho SH, Fritz T, Khaghani A (2016) Left Ventricular Assist Device Placement through Left Thoracotomy in Difficult Scenarios. Int J Clin Cardiol 3:069. 10.23937/2378-2951/1410069
Copyright: © 2016 Mueller LM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Standard surgical approach to the implantation of a Left Ventricular Assist Device (LVAD) is through a median sternotomy. The inflow cannula is attached to the apex of the left ventricle, while the outflow graft is usually attached to the ascending aorta. We present 2 patients with prohibitive chest wall abnormalities who underwent left thoracotomy for LVAD placement, and the outflow graft alternatively attached to the descending aorta.
Keywords
LVAD, Left Thoracotomy, Pectus, Heartware
Introduction
Left ventricular assist devices (LVADs) are a common therapy for patients with advanced heart failure as a bridge to transplantation and as a destination therapy. The standard surgical approach for implantation of a LVAD is through a median sternotomy in which the inflow cannula is attached to the apex of the left ventricle, while the outflow graft is attached to the ascending aorta [1]. In a particular subset of patients who present with a chest wall that proves difficult to approach through a median sternotomy, an alternate surgical approach may be taken. The LVAD may be implanted through a left thoracotomy approach, and the outflow graft can be modified so that it can be alternatively attached to the descending aorta.
Case Report 1
A 37 year-old male with a severe form a pectus excavatum (Figure 1), developed end-stage heart failure due to nonischemic dilated cardiomyopathy. The decision was made to place a HeartWare left ventricular assist device as a bridge to transplantation. Surgical approach was complicated by his pectus excavatum, angled sternum, and cardiac structures being shifted entirely to the left half of his chest (Figure 2).
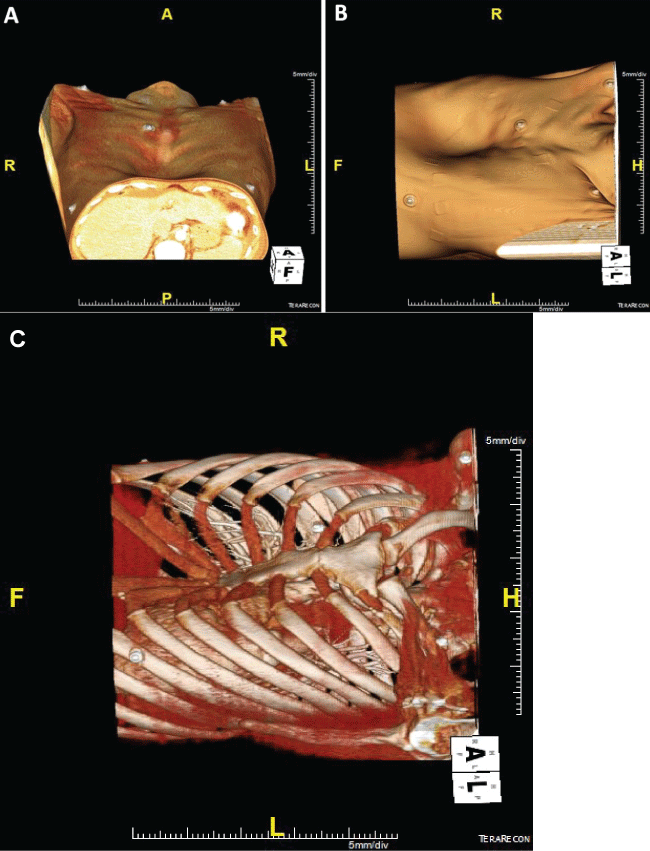
.
Figure 1: (A) Patient in supine position with view of chest wall; (B) Patient in left lateral position with view of chest wall; (C) Patient's bony structures including deep pectus excavatum.
View Figure 1
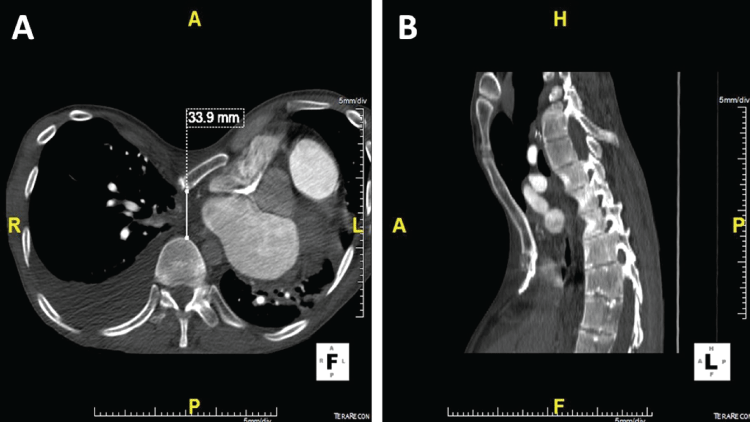
.
Figure 2: (A) Axial CT view of pectus excavatum, angled sternum, and chest contents; (B) Lateral CT view of patient's thorax.
View Figure 2
A left posterolateral thoracotomy was performed through the 5th intercostal space, and the pericardium was opened about 1.5 cm anterior to the left phrenic nerve. The heart was then delivered outside the pericardial cavity, and a venous line was inserted through the left femoral vein to the SVC with TEE guidance. An aortic line was then inserted to the mid descending aorta for cardiopulmonary bypass return. The HeartWare LVAD sewing ring was attached to apex of the left ventricle using 2-0 Prolene, and a hole was created in the apex. After examination of the apex, no thrombus was found. The HeartWare device was then inserted into the ventricle through the hole and fixed into place. At this point, the LVAD was turned on to a low pump speed.
The outflow graft of the HeartWare device was shortened so that it could be attached to the descending aorta instead of the ascending aorta. It was anastomosed to the upper portion of the descending aorta near the subclavian artery using 5-0 Prolene.
The drive line of the LVAD was tunneled through the chest wall between the attachment of the diaphragm to the rib cage, behind the abdominal muscles, and out through the left side of the abdominal wall. Cardiopulmonary bypass was gradually stopped, and the LVAD was turned up to optimal pump speed. 2 chest drains were placed, and the patient was closed in the usual manner with 2 pericostal sutures.
Case Report 2
A 67 year-old male with past medical history significant for coronary artery bypass surgery in 1999 with post-operative development of MRSA mediastinitis and subsequent sternotomy and bilateral pectoral flap placement (Figure 3) developed progressive left ventricular failure refractory to medical management. His treatment team decided to place a Heartmate II left ventricular assist device. Surgical approach for implantation of the device would be impossible through a standard approach, and the decision was made to implant the LVAD through a left thoracotomy approach.
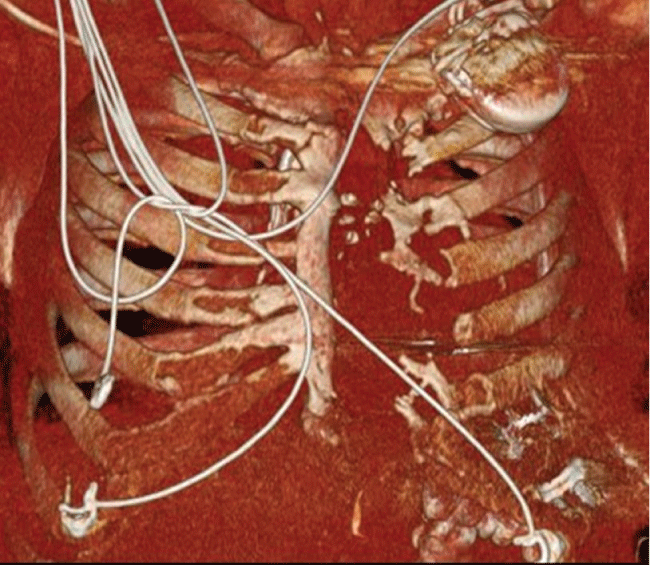
.
Figure 3: Bony structures of patient status post sternectomy and pectoral flap placement.
View Figure 3
A left thoracotomy was created in the mid chest, and the LV apex and descending aorta were exposed. Using TEE guidance, a wire was placed through the left common femoral to the SVC. The drive line tract was then created into the left midepigastrium.
The Heartmate II inflow ring was positioned near the apex. The outflow graft site was selected on the descending aorta instead of the ascending aorta. The graft was then measured and trimmed to fit, and the descending aorta was cannulated. Cardiopulmonary bypass was started.
The apex was examined then cored out, and the inflow cannula was placed in the LV apex using pledgeted sutures and zip ties. The D-ring device was connected, and the pump was allowed to fill (Figure 4 and Figure 5).
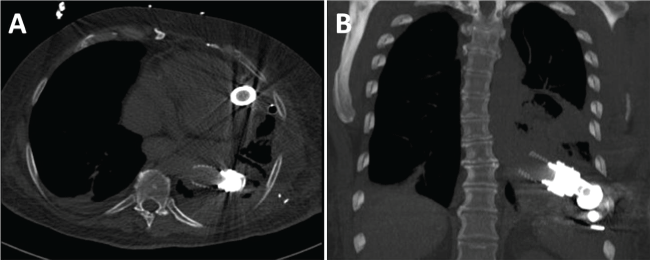
.
Figure 4: (A) Axial CT view showing LVAD inflow from L ventricle and outflow cannula into Descending Aorta; (B) Anterior CT view of LVAD placement.
View Figure 4
.
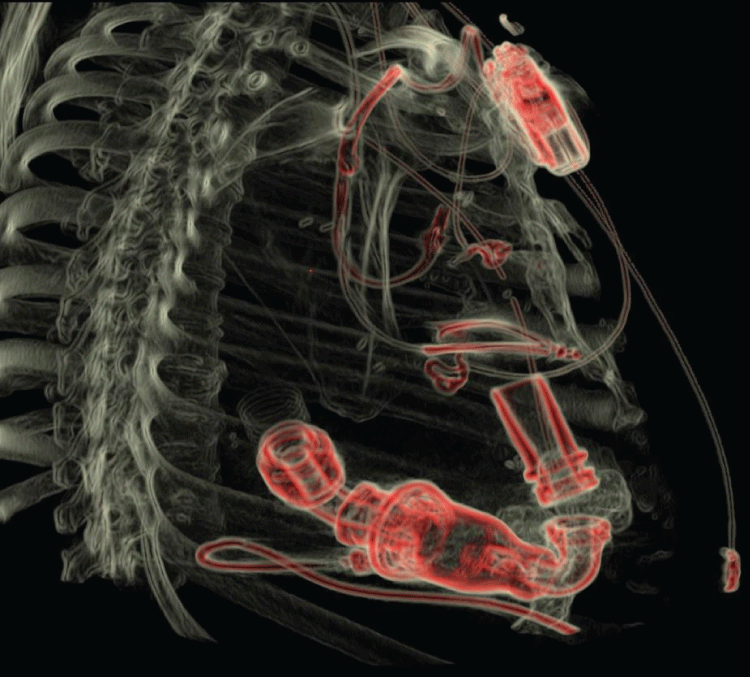
Figure 5: 3D Imaging showing LVAD placement with outflow from L ventricle and inflow into Descending Aorta.s
View Figure 5
The device was turned on to a low pump speed and gradually increased. A single Prolene was utilized to secure the pump so that it would not rotate. The patient was gradually separated from cardiopulmonary bypass as the LVAD pump speed was increased. Angled and straight chest tubes were placed, and the patient was closed in the usual manner.
Conclusion
Many end stage heart failure patients requiring Left Ventricular Assist Device implantation will require a repeat thoracotomy. The recognized major complications of a redo sternal approach include major hemorrhage with entry into the right ventricle, inadvertent lysis of an Internal Mammary Artery or Saphenous Vein graft, graft embolization from manipulation, and dense pericardial adhesions [2].
We present 2 patients with prohibitive chest walls who required novel approach to LVAD implantation through left thoracotomy. This approach may be used to prevent the complications of redo sternotomy for heart transplantation in other patients.
Conflict of Interest
The authors declare that there is no conflict of interests regarding the publication of this article.
References
-
Molina E, Boyce S (2013) Current status of left ventricular assist device technology. Semin Thorc Cardiovasc Surg 25: 56-63.
-
Elahi M, Dhannapuneni R, Firmin R, Hickey M (2005) Direct complications of repeat median sternotomy in adults. Asian Cardiovasc Thorac Ann 13: 135-138.





