International Journal of Clinical Cardiology
Effectiveness of Cardiac Rehabilitation in Increased Left Ventricle Ejection Fraction and Cardiovascular Secondary Prevention
López-Aguilera J1*, Casado-Adam P2, Heredia-Torres MA3, Mazuelos-Bellido F1, Suarez-de-Lezo Jr1, Cano-Lliteras MP4, Mayordomo-Riera FJ3 and Suárez de Lezo J1
1Medical Doctor in Cardiology, Hospital Reina Sofia, Córdoba, Spain
2Medical Area Specialist in Rehabilitation, Hospital Reina Sofia, Córdoba, Spain
3Medical Doctor in Rehabilitation, Hospital Reina Sofia, Córdoba, Spain
4Resident Medical Intern in Rehabilitation, Hospital Reina Sofia, Córdoba, Spain
*Corresponding author: José López Aguilera, Medical Doctor in Cardiology, Hospital Reina Sofia, Córdoba, Spain, Tel: 676613770, E-mail: mircardjla@gmail.com
Int J Clin Cardiol, IJCC-2-065, (Volume 2, Issue 6), Research Article; ISSN: 2378-2951
Received: August 17, 2015 | Accepted: December 05, 2015 | Published: December 10, 2015
Citation: López-Aguilera J, Casado-Adam P, Heredia-Torres MA, Mazuelos-Bellido F, Suarez-de-Lezo Jr, et al. (2015) Effectiveness of Cardiac Rehabilitation in Increased Left Ventricle Ejection Fraction and Cardiovascular Secondary Prevention. Int J Clin Cardiol 2:065. 10.23937/2378-2951/1410065
Copyright: © 2015 López-Aguilera J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: Evaluate effectiveness and predictors in increased left ventricle ejection fraction (LVEF) in patients with ischemic heart disease, after a cardiac rehabilitation program (CRP). Analyze functional capacity and evolution of major cardiovascular risk factors.
Methods: Prospective observational before-after study in the Cardiac Rehabilitation Unit of Córdoba (Spain) between March 2013 and June 2014 during phase 2 of cardiac rehabilitation program (CRP). Demographic variables, LVEF, functional capacity and biochemical parameters were analyzed. Outcome variables at the beginning and end of the treatment were compared using the paired student t-test. In addition, a multiple linear regression analysis was completed to identify the variables related to the increased LVEF.
Results: In this study, 110 patients (98 men and 12 women) were included; 66 low risk patients (60%), moderate 32 (29.1%) and high 12 (10.9%). The mean age of the total sample was 56.6 years. It was obtained statistically significant improvement of: LVEF 3.73 ± 6.99%, functional capacity 2.05 ± 2.25 METs (Metabolic Equivalents), exercise time 1.43 ± 1.56 minutes, LDL cholesterol, HDL cholesterol and glycosylated hemoglobin. The significant predictors of increased LVEF were number of diseased vessels, type of coronary reperfusion and risk group with coefficient of determination of 0.20.
Conclusion: LVEF improvement was determined, being higher in moderate and high risk patients that along with the number of vessels and type of coronary reperfusion were predictors of this increase. Improvement was confirmed in biochemical and functional parameters.
Keywords
Cardiac rehabilitation, Left ventricle ejection fraction, Ischemic heart disease and cardiovascular secondary prevention
Abbreviations
LVEF: Left Ventricle Ejection Fraction, CRP: Cardiac Rehabilitation Program.
Introduction
Ischemic heart disease is a cardiovascular illness of important consequences with a death rate of 45-100/100.000 inhabitants (leading cause of death in adults) in Spain, and with an incidence of 40000-90000 patients/year and a prevalence of approximately 7% in the last years [1]. It is estimated that in next decades, the loss of years of disability- adjusted life increase of 85 million in 1990 to 150 million in 2020 and thus continue to be a major cause of loss of productivity [2]. This pathology is associated with various cardiovascular risk factors largely known such as age, sex, diabetes mellitus, hypertension, dyslipidemia, obesity and smoking habit [3].
The cardiac rehabilitation program aims to: reduce morbidity and mortality [4], improve quality of life, obtain rehabilitation in the family, social and work environment; and decrease secondary disability to cardiovascular disease and improve socio-economic efficiency. In recent years it has been shown that CRP is useful in the secondary prevention of patients who have suffered a cardiovascular event to improve cardiovascular risk factors [5]. It consists of three phases: phase 1 (in-hospital), phase 2 (outpatient) and phase 3 (domiciliary) [6].
Heart failure of ischemic origin is a factor of poor prognosis due to the increased incidence of death at admission and at six months. It should be also considered the added risks and consequences of other associated diseases which can aggravate the prognosis [6].
Left ventricle ejection fraction (LVEF) is related to: drugs that are prescribed in certain patients with ischemic heart disease such as ivabradine (IF current inhibitor in sinoatrial node that has demonstrated reduction of mortality and readmission in patients with systolic dysfunction) [7] and eplerenone (aldosterone receptor inhibitor with effectiveness and survival increase in coronary heart disease and heart failure) [8]. It is also associated with myocardial contractility by evolutionary improvement of chronotropic competence [9] and with the risk group.
In the literature, there are studies that explain the decreasing in morbidity and mortality in cardiac rehabilitation programs according to their level of risk. So, low-risk patients reduce those values because of changes in endothelial function [10], anti-inflammatory effect [11], modifying the cardiovascular risk profile, increased functional capacity [12]. In patients with a higher risk, in addition to described factors previously that influenced the change of the prognosis, the improvement in survival may be related to the modification of heart functional factors. The improvement of ventricular function produced by exercise can be another mechanism which modified the prognosis of cardiac patients especially if the heart function was affected at the beginning of the program. In patients with depressed left ventricular systolic function, aerobic exercise has showed an increase in exercise capacity and an improvement of data remodeling (ventricular volumes and ejection fraction) [13].
Despite these evidences, few studies have evaluated the increase in the LVEF and the variables related to this [14] and to the increased myocardial contractility [9].
In patients who suffered from heart failure caused by systolic dysfunction with ischemic and non-ischemic etiology, CRP application has shown very positive results in clinical improvement [15].
The main objective of this study was to assess and quantify the increased LVEF and determine the factors related to it. A secondary aim was to analyze the evolution of major cardiovascular risk factors (lipid and glucose profile, abdominal circumference), functional capacity and exercise time.
Methods
A prospective observational study was performed before and after CRP during phase 2 in patients from the cardiac rehabilitation unit of hospital Reina Sofia (Córdoba, Spain) within the routine clinical practice between January 2013 and April 2014. Inclusion criteria were: patients older than 18 years of both sexes who had suffered coronary syndrome and had been assessed in the cardiac rehabilitation unit in phase 2 during the study period, met the criteria for classification of risk (low, moderate or high), referred by the intensive care unit (ICU), cardiology or cardiovascular surgery, with hemodynamic stabilization and ergometry by Bruce Protocol. The exclusion criteria taken into account were: patients with unstabilized coronary syndrome (unstable angina, uncontrolled heart failure and uncontrolled hypertension), severe physical disability which hindered them performing the exercise program, major psychiatric illness, hospitalization during the program for heart disease or other, ergometry by Naughton protocol, phase 1 (in-hospital) and 3 (domiciliary) of the program.
All patients included in the study signed informed consents of exercise test performance and for the inclusion in the cardiac rehabilitation program.
Regarding the study population, 124 patients were selected. 14 were excluded: 4 for being precise ergometry by Naughton protocol, 1 for transfer to another hospital, 2 for not having enough medical scans for inclusion in the study, and 7 for having incidents during the program and hospital admission. The sampling rate was systematic of consecutive cases, from patients referred to the cardiac rehabilitation unit who met inclusion criteria and completed CRP between March 2013 and June 2014. All patients underwent echocardiogram by Acuson CV-70 echocardiograph model to quantify LVEF (%) by the Simpson method, and left ventricular wall motility; and exercise test by ergometer MTM-1500 med Schiller model (exercise time in minutes and functional capacity in METs) at the beginning and end of the program, both tests performed by the cardiologist of the unit.
Prior to commencing the program, it was preceded to the clinical evaluation of patients in consultation. Before requesting participation, they were informed about the content of CRP and characteristics of the study. All patients signed an informed consent for inclusion in this study. Data obtained in the anamnesis were: demographic variables (age and sex), clinical variables that included cardiovascular risk factors (smoking history, diabetes mellitus and arterial hypertension, number of affected coronary vessels, coronary reperfusion treatment and intravenous thrombolysis at admission). As complementary explorations before and after the program: biochemical analysis of LDL cholesterol, HDL cholesterol, triglycerides and glycosylated hemoglobin (mg/dl); abdominal circumference (cm) with measuring tape.
All patients in each group of risk (low, moderate and high) were treated with high potency statins (atorvastatin or rosuvastatin) with the aim of reaching LDL levels < 70 mg/dl. After the program was completed, analytical control was done to verify that values of LDL were desirable. If in the course of the program it found that this objective was not met, it was check the adherence and if the patient was taking the maximum dose, if the treatment was not effective or had intolerance. Reviewed above, if the patient was properly treated without side effects, was added 10 mg ezetimibe.
There are several stratification methods recommended by different societies to classify the cardiologic situation of the patients. All of them focus in evaluating functional capacity, ventricular function, residual ischemia and risk factors. One of the most complete and in which this study has based, has been the guide of the American Association for Cardiovascular and Pulmonary Rehabilitation (AACVPR), according to this guide, there are three risk levels: low, moderate and high [16].
After completing the CRP, 2 months later from the first consultation, patients were given the discharge clinical report and the evolution of the data between these consultations were compared and collected. This process was made by the computer program of the hospital. Histories of all patients were consulted.
The cardiac rehabilitation program developed in phase 2, consisted of groups of 5 patients each who conducted sessions 3 days a week of 1 hour duration for 2 months. It included an initial phase of warm-up with isotonic and isometric exercises and a training phase on treadmill or cycloergometer (30-45 minutes) whose heart frequency of training (by exercise test) should be reached progressively: (75%) in the first month and (85%) in the second month thereof. The entire process was carried out under medical supervision, electrocardiographic monitoring and pressure values, depending on the risk. It ends with a cooling-down phase, relaxation and stretching exercises. During the 2 months, patients attended health education lectures given by all members of the unit.
A descriptive analysis of the total sample was performed; qualitative variables were expressed indicating absolute frequencies and equivalent proportions in each category, and quantitative variables using mean and standard deviation. Increased quantitative variables were analyzed before and after the program by mean difference using the paired Student t-test with significance and confidence intervals. In the case of sample stratification by risk group, in the high risk group (being of 12 patients), normality was analyzed by Shapiro-Wilk test, and if not met, the paired Wilcoxon t-test was performed; in the opposite case, the paired Student t-test was used.
Increase in LVEF post-CRP has been estimated as continuous variable adjusted by baseline ejection fraction and predictors using multiple linear regression (MLR) (Univariate and Multivariate Analysis), being that, the dependent variable of the model. The independent variables considered were: number of vessels, coronary reperfusion therapy (drug-eluting stents, combination of stents, coronary bypass and conventional stents, being the latter the reference), left ventricular asynergy after CRP, eplererone and ivabradine treatment, sex, intravenous thrombolysis, risk group (regrouping moderate and high risk patients due to the low number of the latter), age, diabetes mellitus, smoking, hypertension and number of sessions. Anti-platelet and lipid-lower treatment was not necessary to include it in the multivariate model due to its homogeneity.
All contrasts were bilateral and were considered significant at P less than 0.05. The data were processed and analyzed using SPSS for Windows version 15.
Results
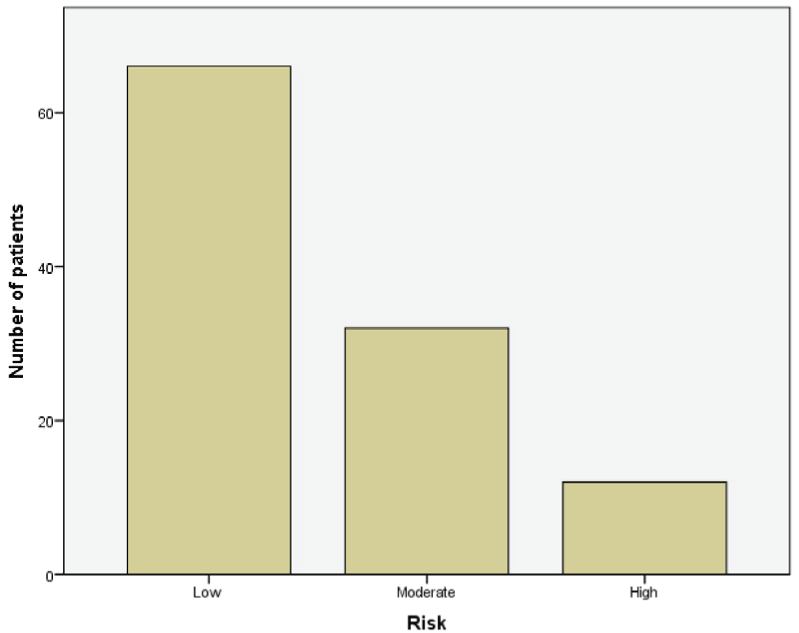
110 patients were included in this study and completed the program. The mean age of the sample was 56.6 ± 8.7 years; Groups of risk are shown in figure 1. Demographic and clinical variables associated with known medical antecedents of the patients described in table 1. The mean duration of the study was 1 year and 6 months.
![]()
Table 1: Demographic characteristics and initial clinical of patients included in the study.
View Table 1
In the paired Student T-test, in the total sample, it was obtained statistically significant improvement of LVEF, functional capacity, exercise time, LDL cholesterol, HDL cholesterol and glycosylated hemoglobin. Decreased abdominal circumference and increased triglycerides were not significant (Table 2). The results of increased echocardiographic and functional variables of the sample stratified by risk groups are shown in table 3. Statistical differences were found between groups of risk in variation of LVEF by the Bonferroni test.
![]()
Table 2: Monitoring variables result before and after CRP by Student T test for paired data.
View Table 2
![]()
Table 3: Mean differences in ejection fraction evolution, functional capacity before and after the program according to/depending on the risk group.
View Table 3
In the multiple linear regression analysis were found as predictors of increased LVEF (%) after completing the CRP: number of vessels, type of coronary reperfusion and risk group. Linear regression model is represented in table 4. The coefficient of determination (R2) was 0.20. All the assumptions of the regression model were met, except normality of the residuals. No significant interaction, confounding or removed variables that provide additional information were found.
![]()
Table 4: Linear regression: predictors of increased LVEF.
View Table 4
Discussion
The findings of this research established increased LVEF before and after CRP and related predictor factors. It was also obtained improvement in biochemical parameters of lipid, glycemic profiles and stress test values. The main variable was LVEF, due to the presence of the association of ischemic heart disease with heart failure, present in a significant number of patients referred to the unit.
It is considered appropriate stratify the sample by risk groups to analyze increase in LVEF, functional capacity and exercise time. The proportion of low risk patients in the present study has been numerically representative. A slight, but significant LVEF increase was obtained in this group, being higher in moderate and high risk patients. Unlike previous studies that considered either the total sample or the high risk group, in this group, it was expected that the improvement was greater, as Vasheghani-Farahani et al. [17] analyzed.
An important finding was increased functional capacity in the total sample (2.01 METs), considering Kavanagh et al. [12] conclusions in which for every 1 ml/kg/min of exercise capacity, was supposed a prognosis improvement in life of 9% (2.6 years more).
In functional capacity, an increase directly proportional to the risk group was produced, but in LVEF, the increase is greater in the moderate risk group, which could be explained by the difference in sample size in the three risk groups (high risk = 12 patients) as well as the comorbidity which sometimes can be associated with high risk patients, as can be the intermittent claudication which hinders the physical training.
In our study, we observed the improvement in lipid profile, which could be more associated with the pharmacological effects, so the objectives of treatment of dyslipidemia in LDL-cholesterol were too high (LDL-cholesterol < 70 mg/dL). However, the cardiac rehabilitation programs have the advantage of closer monitoring of treatment, awareness of the subject of the condition being treated, in addition the known benefits of physical exercise. As well as, the health education lecture offered cardiac rehabilitation programs, including cardiovascular risk factors, the importance of lipids in prevention, the role of diet and how to adjust it were explained.
With regard to the assessment of abdominal circumference before and after the treatment, in our research was not significant, because it was thought that there was not specific care performed by a nutritionist and many patients initiate the smoking cessation at the beginning of the program, so that the weight reduction was more difficult. Body mass index has had a slight relationship with cardiovascular risk, although it has been considered that weight distribution of adipose tissue was more important than the total bodily weight. The gluteofemoral region (gynoid obesity) was not as dangerous as in the abdominal (android), which has been directly related to cardiovascular risk. Several studies have shown that the measurement of waist circumference is associated independently with mortality from all causes [18,19]. For these reasons, body mass index was not analyzed, it was preferred abdominal circumference.
In the regression model, it was expected that pharmacological treatment with eplerenone [8] or ivabradine [7] could be confounding factor or interaction, due to the known increase of LVEF.
Based in Schrauwen-Hinderling et al. [14], it was not added LDL-cholesterol, HDL-cholesterol and glycemic values, because in this article it was concluded that there was not relationship between glycemic or lipids values and functional cardiac results, including LVEF.
Besides, gender was not considered because of the little quantity of women (12 in the total sample). It was considered the moderate and high risk group reunification because of the little quantity of this latter group, to show more representative results.
It was not considered the anti-platelet treatment in the regression model because all the patients had two anti-platelet drugs in the moment of the study: Aspirin and prasugrel, as all the patients completed CRP in phase 2, with an average of evaluation 3 months after acute myocardial infarction at the unit.
There were not any influences at the results because of the socioeconomic status despite the heterogeneity in the occupations of the patients (lawyers, administrative assistants, agriculturalist, housewives....). CRP was performed in the phase 2 at hospital, consequently, all the patients who completed the program, received the same sanitary attention, because of the Spanish health public system. This result could influence more at phase 3 (domiciliary) where is more dependent on care and social/family components.
During CRP there was not any event of mortality in the duration of the study (phase 2). Phase 3 (domiciliary) was not analyzed because it was not the objective of the study. However, it was reported that 3 months after finishing the CRP 1 patient died at his residence (phase 3).
In echocardiography, performed within routine clinical practice, LVEF, wall motion and presence of myocardial alterations by Simpson method were considered, although in other studies volumes, diameters and other indices [20] were taken into account, as well as the assessment of these parameters with another more sensitive measuring instrument as magnetic resonance imaging (Schrauwen-Hinderling et al. [14]). Although, it was known that the best non-invasive and gold standard method for evaluating volumes and systolic function of left ventricle was cardiac magnetic resonance at the present time, it was not used in this study because it was out of our reach and it was not present in our routine clinical practice.
In the linear regression, Mather et al. [21] mentioned that the predictor of final LVEF at three months after an acute myocardial infarction was LVEF in the first week after primary percutaneous angioplasty. In Frengley et al. [22], LVEF was considered significant predictor of survival. However, no studies have been found in which the dependent variable is LVEF after CRP to analyze the predictors that might influence the variation thereof.
A number of limitations need to be considered. A lack of a control group because the number of patients who performed the domiciliary treatment was insufficient, in order to obtain higher homogeneity of the sample, the number of patients with moderate and high risk was greater, especially the latter; in the variable number of vessels would also be convenient to determine the location of the coronary artery that has been affected but it was difficult because of its statistical difficulty.
It would be interesting for future studies to perform a longitudinal research with the same group of patients in phase 3, where the increase of LVEF after CRP and the evolution of mortality rate were proved as well as the possibility of comparing variables with controls to assess the increase and significance in both groups, as Belardineli et al. [9].
Conclusions
This study has shown improvement of LVEF in patients who performed the CRP. Predictors associated with increased LVEF were moderate/high risk, number of affected vessels and type of coronary reperfusion. Improvement in risk factors and FC were confirmed.
Conflict of Interest
All authors have read and approved of the manuscript and declare no conflict of interest.
Acknowledgments
The authors thank all patients and the members of the Cardiac Rehabilitation Unit (especially Mr. Francisco Navas and Milagros Ramos) for participating in this study, Mónica Martín and Tania Seoane for their recommendations in cardiology, Enrique Gómez for his assessment in statistical analysis and Pilar Torres for her translation.
References
-
Ferreira-González I (2014) Epidemiología de la enfermedad coronaria. Rev Esp Cardiol 67: 139-144.
-
Scottish intercollegiate guidelines network (SIGN) (2007) Risk estimation and the prevention of cardiovascular disease. A national clinical guideline, Report no 97.
-
Perk J, De Backer G, Gohlke H, Graham I, Reiner Z, et al. (2012) Guía europea sobre prevención de la enfermedad cardiovascular en la práctica clínica (versión 2012). Rev Esp Cardiol 65: 937.e1-66.
-
García-Porrero E, Andrade-Ruiz M, Sosa-Rodríguez V (2011) Rehabilitación de los pacientes después de la colocación de una endoprótesis coronaria. Rev Esp Cardiol 11: 50-56.
-
Lawler PR, Filion KB, Eisenberg MJ (2011) Efficacy of exercise-based cardiac rehabilitation post-myocardial infarction: A systematic review and meta-analysis of randomized controlled trials. Am Heart J 162: 571-584.
-
Pleguezuelos Cobo E, Miranda Calderón G, Gómez González A, Capellas Sans L (2011) Rehabilitación cardíaca en el síndrome coronario agudo. In: Principios de Rehabilitación cardíaca. (1st edn) Madrid, Panamericana 171-181.
-
González Juanatey JR, Anguita Sánchez M, Raposeiras Roubín S, Castillo Domínguez JC (2012) Estudio SHIFT: papel de la ivabradina en la insuficiencia cardiaca y su importancia en la práctica clínica. Rev Esp Cardiol Supl 12: 8-13.
-
Rossignol P, Ménard, J, Fay R, Gustafsson F, Pitt B, et al. (2011) Eplerenone Survival Benefits in Heart Failure Patients Post-Myocardial Infarction Are Independent From its Diuretic and Potassium-Sparing Effects Insights From an EPHESUS (Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study) Substudy. Heart Failure 58: 1958-1966.
-
Belardinelli R, Georgiou D, Ginzton L, Cianci G, Purcaro A (1998) Effects of moderate exercise training on thallium uptake and contractile response to low-dose dobutamine of dysfunctional myocardium in patients with ischemic cardiomyopathy. Circulation 97: 553-561.
-
Vona M, Rossi A, Capodaglio P, Rizzo S, Servi P, et al. (2004) Impact of physical training and detraining on endothelium-dependent vasodilation inpatients with recent acute myocardial infarction. Am Heart J 147: 1039-1046.
-
Abramson JL, Vaccarino V (2002) Relationship between physical activity and inflammation among apparently healthy middle-aged and older US adults. Arch Intern Med 162: 1286-1292.
-
Kavanagh T, Mertens DJ, Hamm LF, Beyene J, Kennedy J, et al. (2002) Prediction of long-term prognosis in 12 169 men referred for cardiac rehabilitation. Circulation 106: 666-671.
-
Haykowsky MJ, Liang Y, Pechter D, Jones LW, McAlister FA, et al. (2007) A meta-analysis of the effect of exercise training on left ventricular remodeling in heart failure patients: the benefit depends on the type of training performed. J Am Coll Cardiol 49: 2329-2336.
-
Schrauwen-Hinderling VB, Meex RC, Hesselink MK, van de Weijer T, Leiner T, et al. (2011) Cardiac lipid content is unresponsive to a physical activity training intervention in type 2 diabetic patients, despite improved ejection fraction. Cardiovasc Diabetol 10: 47-53.
-
Belardinelli R, Georgiou D, Cianci G, Purcaro A (2012) 10-year exercise training in chronic heart failure: a randomized controlled trial. J Am Coll Cardiol 60: 1521-1528.
-
Rehabilitation AACVPR (American association of cardiovascular and pulmonary) (2013) Guidelines for cardiac rehabilitation and Secondary prevention programs, 5th edn.
-
Vasheghani-Farahani A, Asef-Kabiri L, Masoudkabir F, Davoodi G, Nejatian M, et al. (2011) Effect of exercise- based cardiac rehabilitation following coronary artery bypass surgery on ventricular repolarization indices. J Cardiopulm Rehabil Prev 31: 239-244.
-
López-Jiménez F, Cortés-Bergoderi M (2011) Update: systemic diseases and the cardiovascular system (i): obesity and the heart. Rev Esp Cardiol 64: 140-149.
-
Aranceta J, Foz M, Gil B, E Jover, T Mantilla, et al. (2003) Documento de consenso: obesidad y riesgo cardiovascular. Clinical Invest Arterioscl 15: 196-233.
-
Kim C, Kim DY, Woo Lee D (2011) The Impact of Early Regular Cardiac Rehabilitation Program on Myocardial Function after Acute Myocardial Infarction. Ann Rehabil Med 35: 535-540.
-
Mather AN, Fairbairn TA, Artis NJ, Greenwood JP, Plein S (2011) Timing of cardiovascular MR imaging after acute myocardial infarction: effect on estimates of infarct characteristics and prediction of late ventricular remodeling. Radiology 261: 116-26.
-
Frengley JD, Sansone GR, Alba A, Uppal K, Kleinfeld J (2011) Influence of age on rehabilitation outcomes and survival in post-acute inpatient cardiac rehabilitation. J Cardiopulm Rehabil Prev 31: 230-238.