International Journal of Clinical Cardiology
Transient Isolated Right Ventricular Hypertrophy in A Neonate
Muhittin Celik1*, Heybet Tuzun1, Bedri Aldudak2 and Osman Akdeniz2
1Division of Neonatology, Department of Pediatrics,Diyarbakir Children Hospital, Diyarbakir, Turkey
2Division of Pediatric Cardiology, Department of Pediatrics, Diyarbakir Children Hospital, Diyarbakir, Turskey
*Corresponding author: Muhittin Celik, Specialist in Neonatology, Department of Pediatrics, Division of Neonatology, Diyarbakir Children Hospital, Yenisehir Mahallesi Hasteneler Caddesi, Diyarbakir, Turkey, Tel: +90 533 6807376, E-mail: mehdincelik@hotmail.com
Int J Clin Cardiol, IJCC-2-050, (Volume 2, Issue 5), Case Report; ISSN: 2378-2951
Received: June 28, 2015 | Accepted: September 12, 2015 | Published: September 15, 2015
Citation: Celik M, Tuzun H, Aldudak B, Akdeniz O (2015) Transient Isolated Right Ventricular Hypertrophy in A Neonate. Int J Clin Cardiol 2:050. 10.23937/2378-2951/1410050
Copyright: © 2015 Celik M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Transient isolated right ventricular hypertrophy is rarely encountered in neonates. We describe a term neonate in whom right ventricular hypertrophy was detected in the first postnatal day by echocardiography. There are several reasons that cause transient isolated right ventricular hypertrophy such as gestational diabetes, mother's dietary patterns, and certain drugs.
Keywords
Neonate, Perinatal stress, Right ventricular hypertrophy
Introduction
Transient right ventricular hypertrophy is a rare disease of neonates. Metabolic diseases, maternal diabetes mellitus, non-stereoid anti-inflammatory drug use during pregnancy, and dexamethasone use for bronchopulmonary dysplasia in premature infants can induce transient right ventricular hypertrophy [1-7]. Mother's intake of foods with high polyphenol content is also suspected to be responsible for development of right ventricular hypertrophy [1,8]. Prenatal causes apart from maternal diabetes and metabolic diseases are reported to cause fetal distress by leading ductus arteriosus construction which results in pulmonary hypertension and right ventricular hypertrophy [1]. Present case was found interesting in terms of detection of right ventricular hypertrophy in first postnatal day in echocardiographic examination and observation of closed ductus arteriosus at first examination.
Case Report
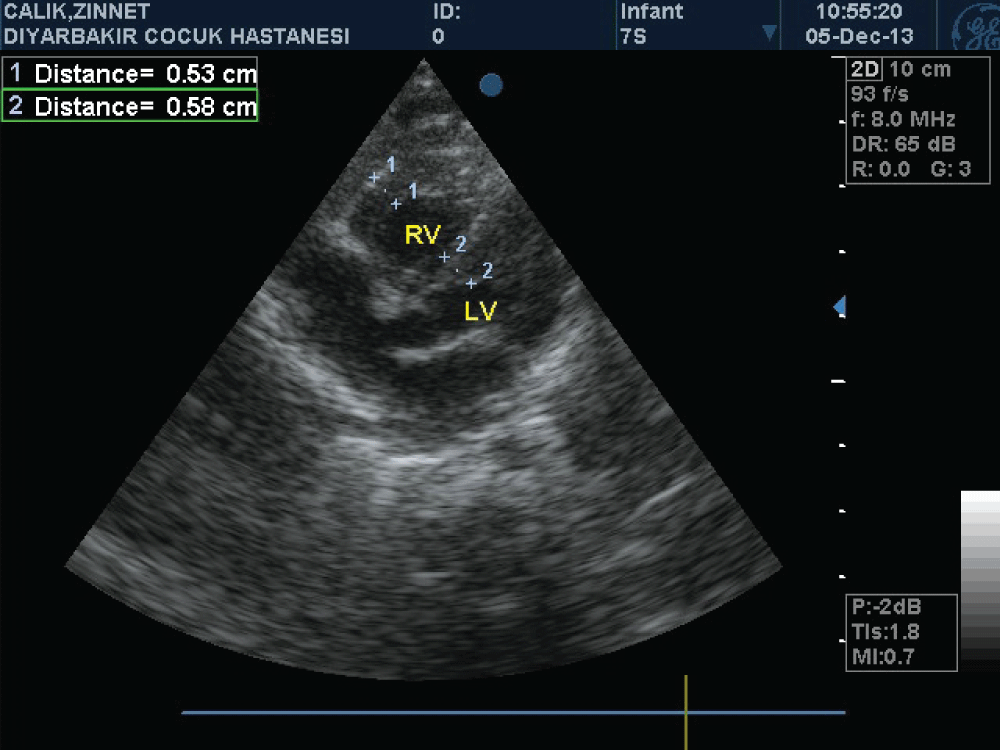
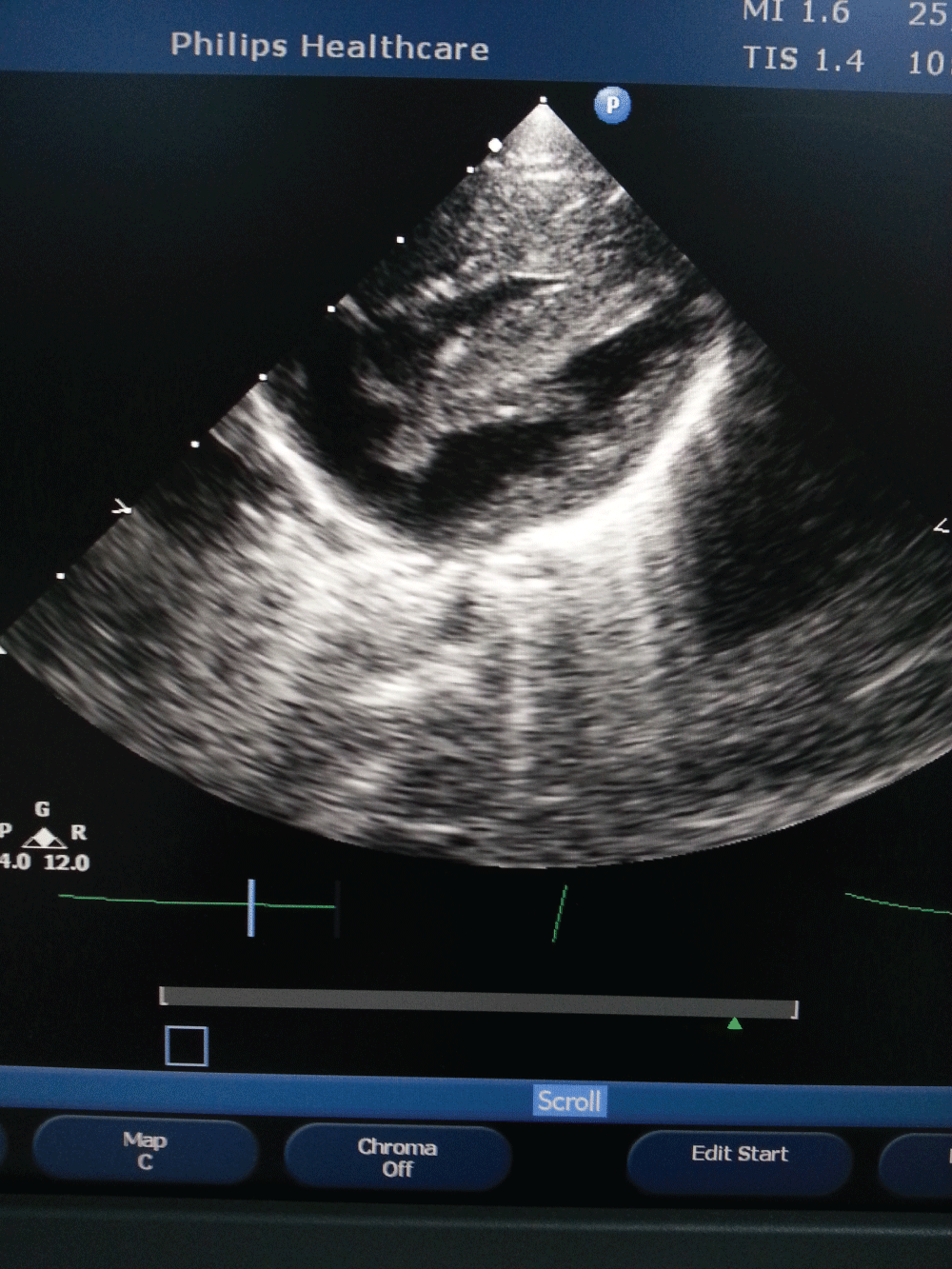
A newborn female patient was admitted to our clinic because of cyanosis. She was born as the first child of non consanguineous healthy parents, via cesarean section due to perinatal stress. Pregnancy was uneventful and family history was unremarkable. There was no history of any medication and gestational diabetes mellitus. Oral glucose tolerance test was normal. Birth weight was 3345 g, and APGAR score at 1 and 5, minute was 6 and 7 respectively. Oxygen saturation on room air was 69%, and was rised to 83% with oxygen supplement. A grade II systolic murmur was present in the tricuspid focus. Transthorasic echocardiographic examination performed at postnatal 6 hour revealed massive hypertrophy in the right ventricle (right ventricular anterior wall thickness was 12 mm, interventricular septum thickness was 12 mm) and grade II tricuspid valve regurgitation (Figure 1). Estimated right ventricular pressure measured through tricuspid regurgitation was 45-50 mmHg. A right to left shunt was observed over a 6 mm diameter secundum type atrial septal defect. The flow in the pulmonary valve was normal and ductus arteriosus was closed. Left ventricular posterior wall thickness was normal (5 mm). There was no coarctation of aorta. Telecardiography was normal. Hemodynamic condition of the patient was thought to be due to the decrease of right ventricular compliance developed secondarily to hypertrophy. To increase right ventricular compliance propranolol was commenced. An oxygen saturation ranged between 83-85% was achieved with the supplementation of 40% oxygen. Saturation values rose up to 90% as of day three and oxygen supplement weaned. The case was discharged oxygen-free and breastfed by the mother on the seventh day. On the day 10 normal saturation values observed and in control echocardiographic examination right ventricular anterior wall thickness measured as 8 mm, while interventricular septum was 6 mm and on the day 40 it was 5.3 and 5.8 mm respectively (Figure 2). Thyroid function tests, Tandem-Mass analysis, and enzyme level for the Pompe's disease were normal.
.
Figure 1: Massive hypertrophy in the right ventricle (right ventricular anterior wall thickness was 12 mm, interventricular septum thickness was 12 mm)
View Figure 1
Discussion
Congenital heart diseases such as, pulmonary stenosis, tetralogy of Fallot, and truncus arteriosus may lead to right ventricular hypertrophy [1]. Other causes of right ventricular hypertrophy are metabolic diseases, maternal diabetes, and early closure of ductus arteriozus [1,3]. Transient right ventricular hypertrophy was associated with acute perinatal stress [1,3,9]. It is well known that mother's intake of aspirin, glucocorticoids, non-stereoid anti-inflammatory drug may cause early closure of ductus arteriosus in neonates. Early closure of ductus arteriosus is suggested to be related with the dietary patterns [1,8]. Vaillant reports 3 hypotheses that can cause right ventricular hypertrophy: a) Mechanic adaptation hypothesis caused by increased pressure or volume overload due to perinatal stress, b) Metabolic hypothesis caused by catecholamine increase, and c) Calcium based ionic derivation hypothesis [3]. Transient right ventricular hypertrophy in the early neonatal phase is an important observation, because it demonstrates that in contrast to adults RVH is still reversible in the perinatal period, when the fetal circulation is significantly altered after birth when the lungs become involved in gas exchange: [I] discontinuation of the placental blood supply, [II] closure of foramen ovale and ductus arteriosus and [III] a dramatic reduction in pulmonary vascular resistance. Did the female patient suffer from pulmonary hypertension in addition to the right to left shunt?
This observation suggests that (pulmonary hypertension-induced) RVH can be treated effectively in the early neonatal period, in which the immature lung and developing heart are probably more susceptible to effective treatment. This observation confirms data found in neonatal rats, in which directly after birth the right ventricular free wall is relatively thick compared to the left ventricular free wall and hyperoxia-induced RVH can be completely reversed by pharmacological intervention in the early neonatal period.
In present case echocardiography was excluded structural causes. Spontaneous regression, normal metabolic screening test results and normal enzyme analysis excluded the metabolic causes and Pompe's disease. Normal oral glucose tolerance test during pregnancy, normal birth weight, and absence of postnatal hypoglycemia were excluded gestational diabetes mellitus.
To our knowledge present case is the first case in which right ventricular hypertrophy was detected on the first postnatal day. Two cases reported by Tomar et al. [9] were diganosed on the 3. Postnatal day, three cases reported by Vaillant et al. [3] were diagnosed between the days 2-7, and Karatas et al. [1] reported a case diagnosed on the third day. In general, cardiac hypertrophy is known to be developed during postnatal period [3]. Our case was delivered via cesarean section due to perinatal stress, and presence of the pronounced hypertrophy 6 hours after delivery suggested antenatal development of the process. Closed ductus arteriosus confirmed the role of early closure of ductus arteriosus on the etiology of right ventricular hypertrophy [10-12]. It is known that cardiac hypertrophy due to hypoxic injury, as similar in diabetic mother's babies, is a benign process and regresses within as 1-5 months spontaneously [3,9]. Effect of propranolol on the regression of hypertrophy and its use as a therapeutic option, as we commenced to repair the right ventricular compliance in our case, still remains controversial.
Financial Support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
References
-
Karatas Z, Sap F, Karaaslan S, Alp H, Altin H, et al. (2013) Transient Isolated Right Ventricular Hypertrophy in a Neonate. Turkish Journal of Pediatric Disease 7: 44-46.
-
Towbin JA, Lipshultz SE (1999) Genetics of neonatal cardiomyopathy. Curr Opin Cardiol 14: 250-262.
-
Vaillant MC, Chantepie A, Casasoprana A, Chamboux C, Suc AL, et al. (1997) Transient hypertrophic cardiomyopathy in neonates after acute fetal distress. Pediatr Cardiol 18: 52-56.
-
Werner JC, Sicard RE, Hansen TW, Solomon E, Cowett RM, et al. (1992) Hypertrophic cardiomyopathy associated with dexamethasone therapy for bronchopulmonary dysplasia. J Pediatr 120: 286-291.
-
Akcoral A, Oran B, Tavli V, Oren H, Cevik NT (1996) Transient right sided hypertrophic cardiomyopathy in an infant born to a diabetic mother. Indian J Pediatr 63: 700-703.
-
Gill AW, Warner G, Bull L (1996) Iatrogenic neonatal hypertrophic cardiomyopathy. Pediatr Cardiol 17: 335-339.
-
Mazzoleni S, Policicchio G, Piovesana P, Pantaleoni A, Bacolla G, et al. (1992) [A case of transient hypertrophic cardiomyopathy in a twin infant of a diabetic mother]. Pediatr Med Chir 14: 95-98.
-
Zielinsky P, Piccoli AL Jr, Manica JL, Nicoloso LH (2010) New insights on fetal ductal constriction: role of maternal ingestion of polyphenol-rich foods. Expert Rev Cardiovasc Ther 8: 291-298.
-
Tomar M, Radhakrishnan S, Shrivastava S (2003) Transient severe isolated right ventricular hypertrophy in neonates. Cardiol Young 13: 384-386.
-
Gao Y, Raj JU (2010) Regulation of the pulmonary circulation in the fetus and newborn. Physiol Rev 90: 1291-1335.
-
de Visser YP, Walther FJ, Laghmani el H, Steendijk P, Middeldorp M, et al. (2012) Phosphodiesterase 4 inhibition attenuates persistent heart and lung injury by neonatal hyperoxia in rats. Am J Physiol Lung Cell Mol Physiol 302: L56-67.
-
Del Pasqua A, Iadanza A, Pierli C (2007) Unexplained severe transient hypertrophy of the right ventricle in a newborn. J Cardiovasc Med 8: 311-312.