International Journal of Clinical Cardiology
Thrombosis and Multiple System Embolization from an on- X Aortic Valve on Clopidogrel- A Review of Pooled Analysis of 2,389 Patient
Kalgi Modi*
Department of Cardiology, LSU Health, USA
*Corresponding author: Kalgi Modi, MD, FACC, Department of Cardiology, LSU Health, 1501 Kings Highway, Shreveport, LA 71106, USA, Tel: 318 675 5941, E-mail: kmodi@lsuhsc.edu
Int J Clin Cardiol, IJCC-2-024, (Volume 2, Issue 2), Case Report; ISSN: 2378-2951
Received: October 21, 2014 | Accepted: March 19, 2015 | Published: March 21, 2015
Citation: Modi K (2015) Thrombosis and Multiple System Embolization from an on- X Aortic Valve on Clopidogrel- A Review of Pooled Analysis of 2,389 Patient. Int J Clin Cardiol 2:024. 10.23937/2378-2951/1410024
Copyright: © 2015 Modi K. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
Thrombosis of a mechanical aortic valve is a rare but life threatening complication and in most cases is caused by inadequate or interrupted anticoagulant treatment. Prosthetic valve thrombosis may cause systemic embolization with clinical manifestation dependent on the organ involved. Multiple systemic embolization resulting from non-infective thrombotic aortic prosthetic valve is a rare occurrence. We present a case of a young woman with a mechanical aortic valve thrombosis manifested as an acute myocardial infarction followed by acute kidney infarction, both of embolic origin.
Case Report
A 32 y/o African American woman was referred to cardiology clinic for evaluation of "dilated aorta" and hypertension diagnosed two years before. On presentation, she reported symptoms of sharp left sided chest pain radiating to the back, grade 3/10, lasting for 3-4 minutes at a frequency of once a month without aggravating or relieving factors and associated with dizziness and dyspnea on exertion. She denied history of smoking, alcohol use, illicit drug use, or significant family history of heart disease.
On examination, there was a 55mmHg systolic blood pressure and 10mmHg diastolic blood pressure difference noted between upper extremities. Her left upper extremity blood pressure was 165/120mmHg and right upper extremity blood pressure was 220/110mmHg. The remainder of the physical examination was unremarkable. Her blood pressure was treated with 0.1 mg Clonidine in the clinic, and she was subsequently sent for emergent transthoracic echocardiogram which revealed dilated aortic root with moderate to severe aortic insufficiency. Because aortic dissection could not be ruled out by transthoracic echocardiogram, an emergent CT angiogram and transesophageal echocardiogram were performed and confirmed fusiform dilatation of ascending thoracic aorta (5.7x 5.8cm) with bovine aortic arch and aortic intimal flap without extension into supra aortic vessels. The patient was immediately admitted to the coronary care unit and started on IV labetalol, IV nitroprusside and Procardia. She underwent Bentall procedure for repair of aortic dissection and received aortic valve replacement with # 25 ON-X- mechanical prosthesis. The pathology of aorta and aortic valve leaflet revealed focal myxoid degeneration. Post operatively, the patient did well and was discharged home on metoprolol, Lisinopril, and Plavix. The patient remained asymptomatic at two-week follow up with CT surgery.
Five months after surgery, the patient presented to an outside facility with new onset of chest pain. EKG at that time was unremarkable with troponin of 3 and CK MB of 100. The patient was transferred to our facility eight hours after initial presentation, and repeat EKG revealed ST segment elevation in lead V1, V2, V3, and V4 with reciprocal depression in inferior leads consistent with anterior STEMI (Figure 1). The patient was hemodynamically stable with unremarkable physical exam. Troponin (122), CK-MB (217.8), and total CK (2718) were all elevated. The remainder of labs was unremarkable. She was taken for emergent cardiac catheterization which confirmed total occlusion of mid LAD and diagonal artery with large burden of thrombus (Figure 2a,2b). Aspiration thrombectomy was performed with V3 and V4 pronto aspiration catheter followed by deployment of 4.0x23 mm bare metal stent in LAD with ASA, Plavix, heparin and Integrillin pharmacotherapy (Figure 3).
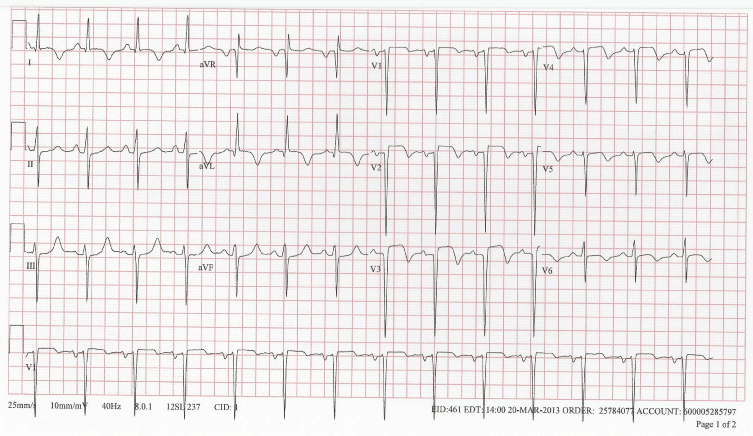
Figure 1: EKG showing ST segment elevation in lead V1, V2, V3, and V4 with reciprocal depression in inferior leads consistent with anterior STEMI.
View Figure 1
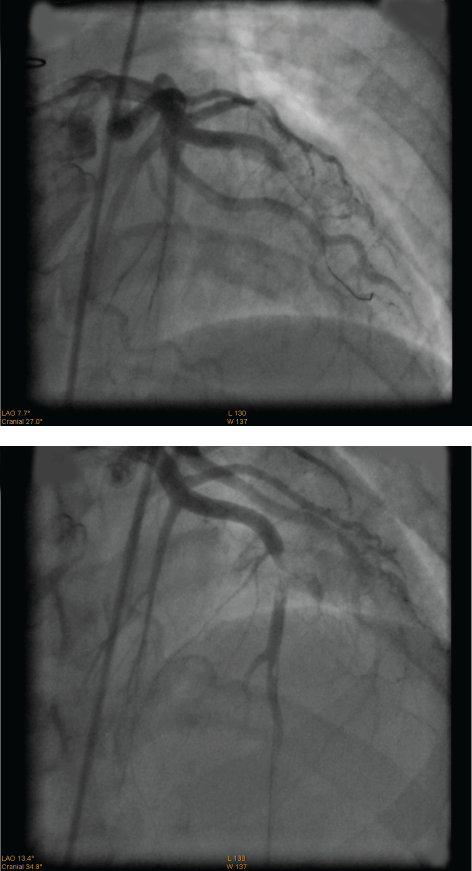
Figure 2: Coronary Angiogram showing total occlusion of mid LAD and
diagonal artery with large thrombus burden.
View Figure 2
Subsequent TEE showed a large 23 x 9 mm thrombus on anterior leaflet of mechanical aortic valve with a mean gradient of 10mmHg (Figure 4) and severely depressed left ventricular systolic function with an EF of 25% associated with anterior and anteroseptal wall hypokinesis. Nonobstructive mechanical valve thrombosis was treated conservatively with therapeutic heparin. Hypercoagulable work up was negative including protein C deficiency, protein S deficiency, anticardiolipin antibodies, anti phosphatidylserine IgG, anti-apolipoprotein antibodies, and anti-thrombin III deficiency. Heparin induced antibodies and RPR were negative as well. On day eight, patient experienced sudden onset left lower quadrant abdominal pain and nausea. An abdominal CT scan showed a well demarcated, hypo dense, wedge-shaped area in the upper pole of the right kidney. There was no mass effect, contrast enhancement or perinephric stranding. The lesion straddles the renal cortico-medullary junction c/w acute infarct of the superior pole of right kidney (Figure 5).
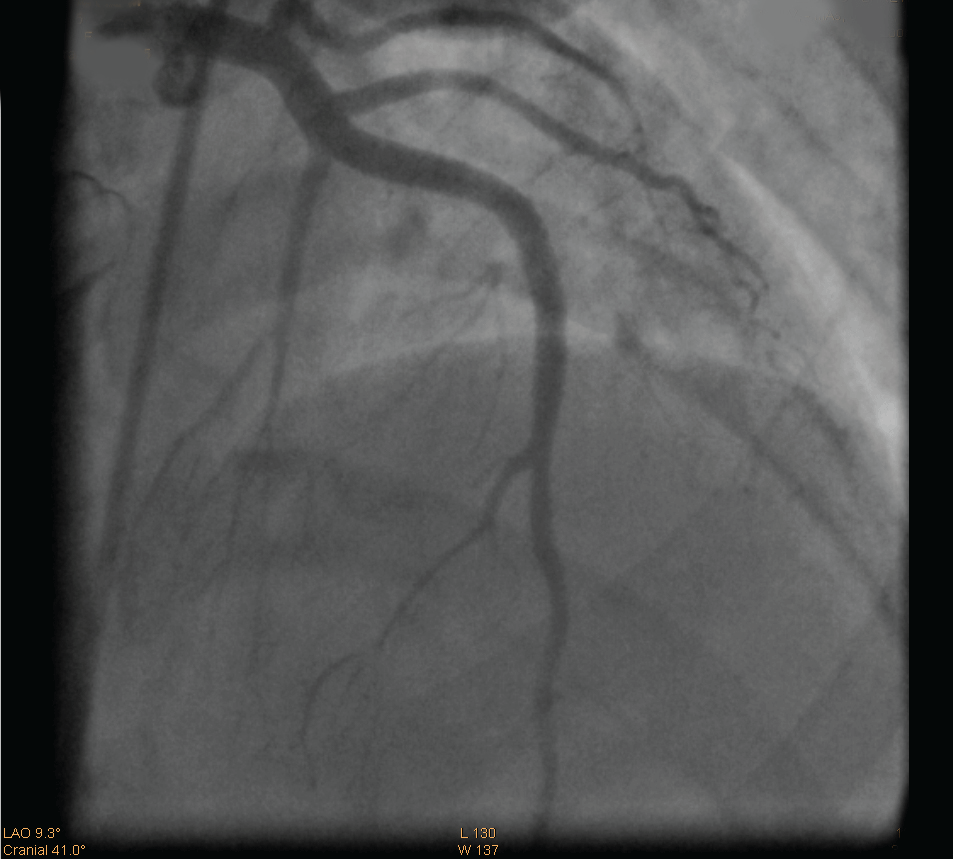
Figure 3: Coronary Angiogram following Aspiration thrombectomy and
deployment of 4.0x23 mm bare metal stent in LAD.
View Figure 3
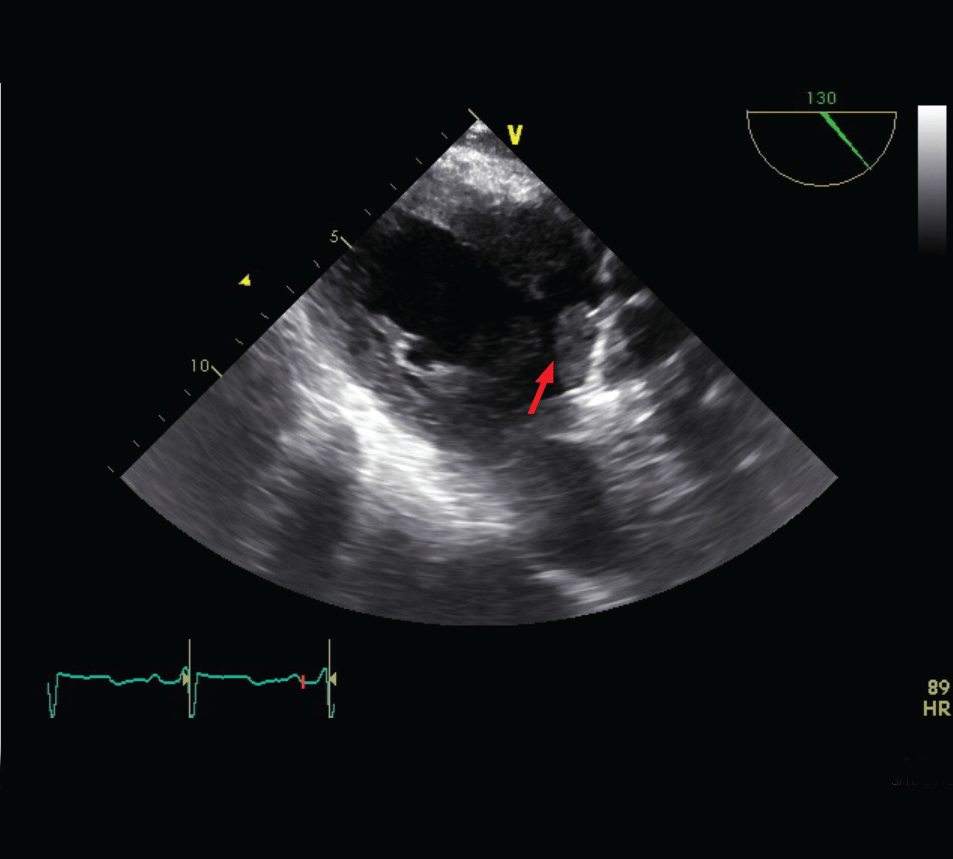
Figure 4: TEE showing a large 23 x 9 mm thrombus on anterior leaflet of
mechanical aortic valve.
View Figure 4
The follow up TEE revealed a 21mm X 21 mm thrombus on mechanical valve (Figure 6). Due to unsuccessful conservative management, patient underwent surgical thrombectomy of aortic valve. Intraoperative thrombus was described to be located on pledget beneath aortic valve with excellent excursion. Postoperatively, the patient was started on warfarin and later discharged on it with targeted INR in the range of 2.5-3.5. As of November 2013 six months after discharge the patient has remained compliant and asymptomatic.
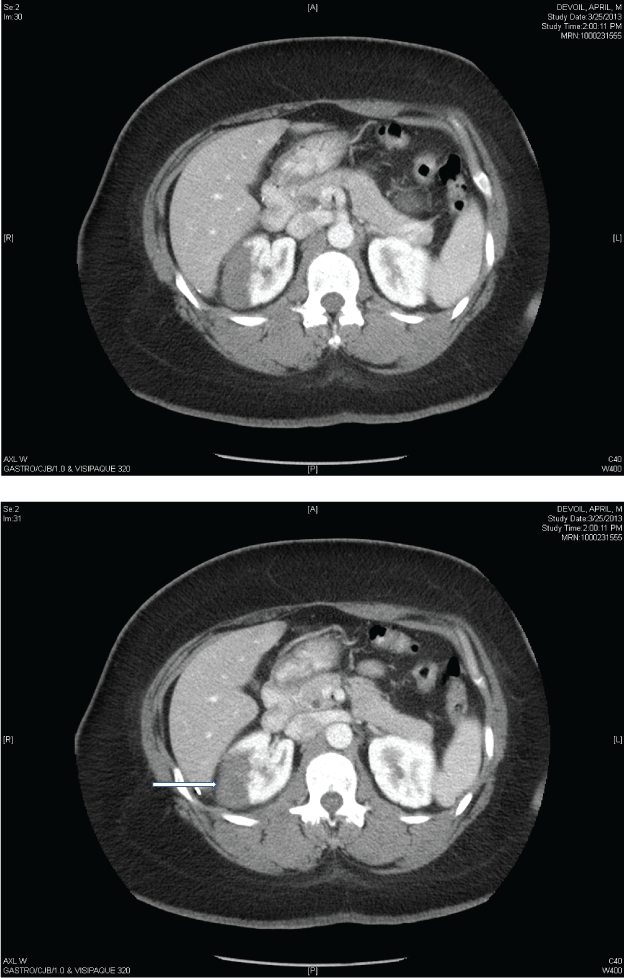
Figure 5: An abdominal CT scan showed well demarcated, hypo dense,
wedge-shaped area in the upper pole of the right kidney c/w acute infarct of
the superior pole of right kidney.
View Figure 5
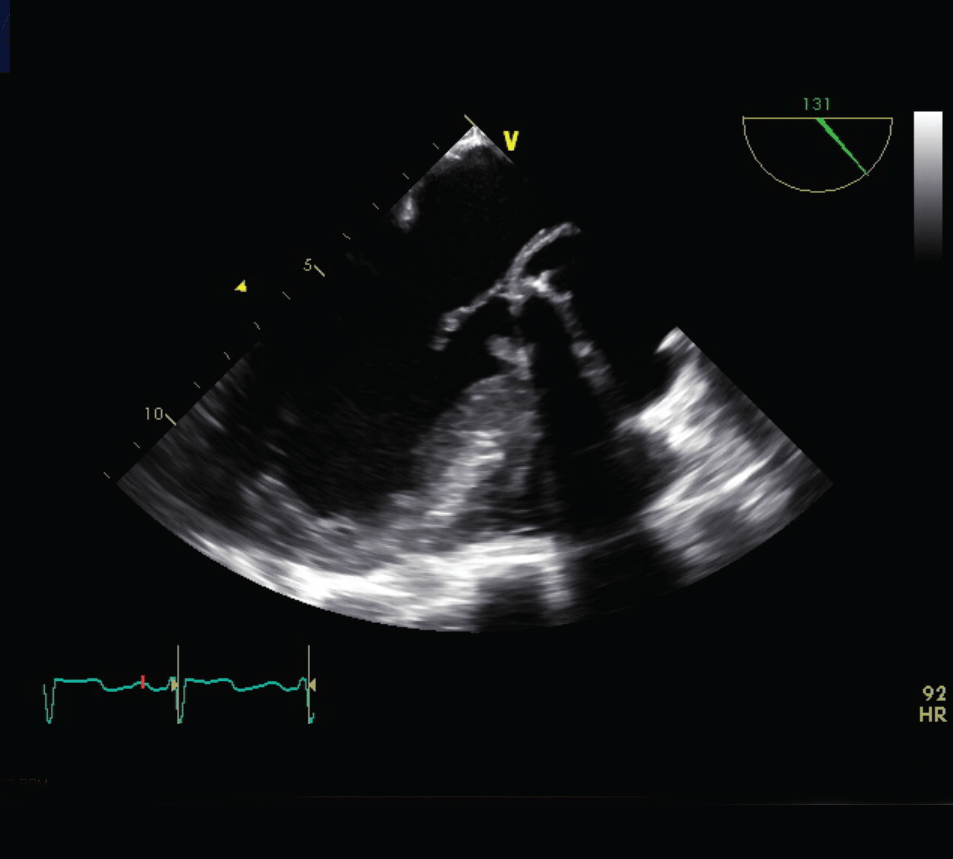
Figure 6: A follow up TEE revealed a 21 X 21 mm thrombus on aortic
mechanical valve.
View Figure 6
Discussion
To our knowledge, this is the first published report of On-X valve thrombosis and multiorgan infarct successfully treated with initial antithrombotic therapy and surgical thrombectomy. Prosthetic valve thrombosis (PVT) is a dreaded complication of valve replacement, and is most frequently seen in patients with suboptimal anticoagulant [1]. The annual incidence of PVT ranges from 0.1 to 6% per patient per year [1]. The risk of thromboembolism depends not only on prosthesis type but also on valve position, patient risk factors, and anticoagulation therapy. Patients with atrial fibrillation, left ventricular dysfunction, left atrial enlargement, previous thromboembolism, and hypercoagulable states are categorized as high risk for thrombus formation. Guidelines recommend anticoagulation with Warfarin to achieve target INR of 2.5-3.5 for mechanical aortic valve with low thrombogenicity [2].
The On-X is a thin bileaflet mechanical valve made with a pure form of isotropic pyrolytic carbon without silicon, has a flared inlet, and an elongated orifice which guides blood through with a laminar flow at a lower pressure gradient than most mechanical valves, preventing damage to the blood [3]. The valve was first implanted in 1996 and became commercially available in the United States in 2002. We reviewed available publications related to On-X aortic valve cases from 1996 to 2014. A total of 2,389 patients had On-X mechanical aortic valve implanted. In these studies implant rate in women ranged from 19-56%. On-X valve was found to have relatively low thrombogenicity (0.6 to 2.67%/ patient �year) compared to other mechanical valves (Table 1) [4-17]. Average follow up time was anywhere from 11 months to 5.2 years. Interestingly, in a poorly anticoagulated community from South Africa, the On-X valve had shown a promising result where a satisfactory anticoagulation was achieved with target INR 1.5-2.5 in 58%, unsatisfactory in 23%, and no anticoagulation in 19% of patients. Even with high number of patients with inadequate anticoagulation (42%), there was 0% thrombosis rate [5].
![]()
Table 1: Pooled data from 2002 to 2014 on On-X valve.
View Table 1
Although a number of individuals are still working on a mechanical valve that does not need anticoagulation, success is unlikely. This is because mechanical valves cause platelet activation and thrombosis not because of materials that induce blood clotting, but because of the fact that they are hard, rigid structures. When the valve leaflets close, at the point of contact there is immediate rebound. This collision and rebound is a very violent event � so violent that cavitation was induced in some early heart valve designs. Even when cavitation does not occur, the shear stress induced in the vicinity of the closing and rebounding leaflets is extremely high. This activates platelets and leads to thrombosis and to thromboembolism downstream of the valve.
In a study conducted by Garcia et al, there was 0% valve thrombosis (135 patients) rate of mechanical aortic valve on aspirin and clopidogrel as anticoagulation, although they recommended that patient should undergo routine testing of platelet reactivity [18]. The CAPTA study (clopidogrel and aspirin in the prevention of thromboembolic complications after mechanical valve placement) was stopped due to one death in anti-platelet arm [19]. Based on the relative success of its South African trial in a poorly anticoagulation population of indigents, a US clinical trial (PROACT) has been initiated in which low risk aortic valve patients will be anticoagulated with only Plavix and aspirin; high risk aortic valve patients will be anticoagulated with Coumadin to INR levels of between 1.5 and 2.0. The preliminary data suggest that selected low-risk AVR patients can be managed without warfarin on dual antiplatelet therapy [16].
The present case was characterized by sudden onset of multiple embolizations in the absence of endocarditis, hypercoagulability, or atrial fibrillation. Specifically, coronary and renal embolization with myocardial and renal infarct is reported for the first time as consequence of On-X valve nonobstructive thrombosis. Acute ST elevation myocardial infarction in our patient was very likely provoked by embolization from mechanical valve thrombus near the left coronary cusp. In our case, first line therapy was medical management with IV heparin due to concern of a high risk of cerebral or systemic embolization and is considered appropriate therapy in the absence of valve obstruction or congestive heart failure. The On-X valve is a relatively new prosthesis that boasts improved hemodynamic characteristics and reduced need for anticoagulation. However, our patient experienced PVT and multiorgan infarct likely secondary to inadequate anticoagulation, suggesting that dual antiplatelet therapy with ASA and Plavix may not be sufficient to prevent PVT and systemic thromboembolic in patients with mechanical On-X aortic valve. Inadequate systemic anticoagulation at the time of thrombosis in 45% of patients:(27% for medical reason and 17% because of poor patient compliance) has been the most frequently related risk factor for prosthetic valve thrombosis [20]. Similarly, the rate of subtherapeutic anticoagulation was 39% among patients with PVT in a recent review.
References
-
Paci AM, Lattanzi F, Cabani E, Conti U, DeTommasi SM (2007) Non-obstructive prosthetic aortic valve thrombosis presenting with acute myocardial infarciton and stroke in a patient with inadequate low-molecular-weight heparin treatment. The unlucky patient and the (pseudo) prudent physician. J Cardiovasc Med (Hagerstown) 8: 277-280.
-
Pibarot P, Dumesnil JG (2009) Prosthetic heart valves: selection of the optimal prosthesis and long-term management. Circulation 119: 1034-1048.
-
Birnbaum D, Laczkovics A, Heidt M, Oelert H, Laufer G, et al. (2000) Examination of hemolytic potential with the On-X(R) prosthetic heart valve. J Heart Valve Dis 9: 142-145.
-
Chambers JB, Pomar JL, Mestres CA, Palatianos GM (2013) Clinical event rates with the On-X bileaflet mechanical heart valve: a multicenter experience with follow-up to 12 years. J Thorac Cardiovasc Surg 145: 420-424.
-
Williams MA, Crause L, Van Riet S (2004) A comparison of mechanical valve performance in a poorly anticoagulated community. J Card Surg 19: 410-414.
-
Moidl R, Simon P, Wolner E; On-X Prosthesis Heart Valve Trial (2002) The On-X prosthetic heart valve at five years. Ann Thorac Surg 74: S1312-1317.
-
Ozyurda U, Akar AR, Uymaz O, Oguz M, Ozkan M, et al. (2005) Early clinical experience with the On-X prosthetic heart valve. Interact Cardiovasc Thorac Surg 4: 588-594.
-
Palatianos GM, Laczkovics AM, Simon P, Pomar JL, Birnbaum DE, et al. (2007) Multicentered European study on safety and effectiveness of the On-X prosthetic heart valve: intermediate follow-up. Ann Thorac Surg 83: 40-46.
-
Chan V, Jamieson WR, Lam BK, Ruel M, Ling H, et al. (2010) Influence of the On-X mechanical prosthesis on intermediate-term major thromboembolism and hemorrhage: a prospective multicenter study. J Thorac Cardiovasc Surg 140: 1053-1058.
-
McNicholas KW, Ivey TD, Metras J, Szentpetery S, Marra SW, et al. (2006) North American multicenter experience with the On-X prosthetic heart valve. J Heart Valve Dis 15: 73-78.
-
Sasaki T, Takahashi Y, Ando M, Wada N (2007) Repair of recoarctation and aortic valve replacement with the On-X valve in a pediatric patient: a case report. J Nippon Med Sch 74: 173-176.
-
Tossios P, Reber D, Oustria M, Holland-Letz T, Germing A, et al. (2007) Single-center experience with the On-X prosthetic heart valve between 1996 and 2005. J Heart Valve Dis 16: 551-557.
-
Chambers J, Roxburgh J, Blauth C, O�Riordan J, Hodson F, et al. (2005) A Randomized Comparison of the MCRI On-X and CarboMedics Top Hat Bileaflet Mechanical Replacement Aortic Valves: Early Postoperative Hemodynamic Function and Clinical Events. J Thorac Cardiovasc Surg 130: 759-764.
-
Laczkovics A, Heidt M, Oelert H, Laufer G, Greve H, et al. (2001) Early clinical experience with the On-X prosthetic heart valve. J Heart Valve Dis 10: 94-99.
-
Dohmen G, Prufer D, Dahm M, Guth S, Moersig W, et al. (2008) Clinical and Hemodynamic Performance of the On-X Bileaflet Heart Valve. European Journal of Cardiac Interventions 8: 111-114.
-
Puskas J, Gerdisch M, Nichols D, Quinn R, Anderson C, et al. (2014) Reduced anticoagulation after mechanical aortic valve replacement: interim results from the prospective randomized on-X valve anticoagulation clinical trial randomized Food and Drug Administration investigational device exemption trial. J Thorac Cardiovasc Surg 147: 1202-1210
-
Williams MA, van Riet S (2006) The On-X heart valve: mid-term results in a poorly anticoagulated population. J Heart Valve Dis 15: 80-86.
-
Garcia-Rinaldi R, Carro-Pagan C, Schaff HV, McKellar SH, Thompson JL 3rd, et al. (2009) Initial Experience with Dual Antiplatelet Thromboprophylaxis Using Clopidogrel and Aspirin in Patients with Mechanical Aortic Prostheses. J Heart Valve Dis 18: 617-625.
-
Schlitt A, von Bardeleban RS, Ehrlich A, Eimermacher A, Peetz D, et al. (2003) Clopidogrel and Aspirin in the Prevention of Thromboembolic Complications after Mechanical Aortic Valve Replacement (CAPTA). Thromb Res 109: 131-135.
-
D�rrleman N, Pellerin M, Bouchard D, H�bert Y, Cartier R, et al. (2004) Prosthetic valve thrombosis: twenty-year experience at the Montreal Heart Institute. J Thorac Cardiovasc Surg 127: 1388-1392.





