International Journal of Clinical Cardiology
Use of Statins in an Australian Elderly Population
Svetla Gadzhanova*
Quality Use of Medicines and Pharmacy Research Centre, Sansom Institute, University of South Australia, Australia
*Corresponding author: Svetla Gadzhanova, Quality Use of Medicines and Pharmacy Research Centre, Sansom Institute, University of South Australia, GPO Box 2471, Adelaide SA 5001, Australia, Tel: +61 8 8302 2352; Fax: +61 8 8302 1087; E-mail: svetla.gadzhanova@unisa.edu.au
Int J Clin Cardiol, IJCC-1-016, (Volume 1, Issue 2), Research Article; ISSN: 2378-2951
Received: October 10, 2014 | Accepted: December 25, 2014 | Published: December 28, 2014
Citation: Gadzhanova S, Roughead E, Ilomaki J (2014) Use of Statins in an Australian Elderly Population.Int J Clin Cardiol 1:016. 10.23937/2378-2951/1410016
Copyright: ©2014 Gadzhanova S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Statins are the first drug choice for lowering high cholesterol and are one of the most widely used classes of medicines in Australia. Although well tolerated, some adverse effects are dose and potency dependent to which older people are particularly susceptible.
Objective: The aim of this study was to examine the use of statins in elderly Australians, and how usage had changed over time with respect to dose and potency of statin prescribed.
Methods: A retrospective study was conducted using data from the Australian Government Department of Veterans' Affairs. Monthly utilisation of all statins and by product was established from 2001 to 2012 as a proportion of the overall veteran population. Use by dose and potency of statins as well as dose and potency at time of initiation was investigated. Dose and potency of statins dispensed in December 2012 to the elderly, those in residential aged-care and those with prior cardiovascular (CV) disease were examined using multinomial logistic regression.
Results: Overall use of statins increased from 17% in 2001 to 35% in 2012. Atorvastatin was the most commonly prescribed statin, followed by simvastatin. Statin use shifted from low to high potency with time, with high potency increasing from 35% in 2001 to 71% of all statin use in December 2012. In 2012, around 85% of all statin initiations were with high potency products.
High potency/high dose statins were less likely to be received by those aged 85 and overcompared to those under 85 years (adjusted Odds Ratio (aOR)=0.38, 95% CI 0.37-0.40) and by those living in residential aged care compared to those living in the community(aOR=0.88, 0.83-0.94).
High potency/high dose statin use was higher among secondary prevention patients than among primary prevention patients (aOR=1.88, 1.81-1.95).
Conclusion: Statins were dispensed for around one-third of veteran population in 2012, with majority of statin initiations and use being with high potency statins. While high potency/high dose statins were used less frequently in the very elderly, there were still considerable numbers of older patients using high strength products, which may contribute to increased risk of harm.
Introduction
High blood cholesterol is a risk factor linked to cardiovascular disease (CVD) which is the largest cause of premature death in Australia, accounting for over a third of all deaths in 2007 [1]. HMG CoA Reductase inhibitors (also known as statins) are the first drug choice for lowering high cholesterol and are one of the most widely used classes of medicines in Australia [2]. The efficacy of statinsin secondary prevention of CV events is well established [3,4]. Until recently, there was uncertainty around use of statins for primary prevention of CVD with earlier systematic reviews suggesting insufficient evidence to support their use in adult women and men older than 69 years at low risk [5]. More recent findings by the Cholesterol Treatment Trialists (CTT) Collaboration using individual patient data meta-analysis provide evidence that men and women, old and young all appear to benefit from statin use regardless of baseline risk [6]. However, these findings have been debated with some researchers suggesting only a small gain in reduction of clinical events which has the potential to be offset due to the occurrence of non-adherence and side effects which may be more apparent at higher doses [7].
Even though statins are well tolerated, there are some adverse effectsthat are dose-related and dependent on the potency of the statin [8-10]. Therapy with higher doses or more potent statins is associated with an increased risk of myopathy [9-11] and elevated liver enzymes [11]. Thus, use of low potency and low dosestatins may help to minimise adverse effects.
In Australia, utilisation of statins is higher than in other OECD (Organization for Economic Co-operation and Development)countries [12] and steadily increased from 98 to 162 defined daily dose/1000 population/year from 2001 to 2004 [12], with 16% of the Pharmaceutical Benefits Scheme (PBS) budget spent on statins in 2005 [12,13]. Atorvastatin, rosuvastatin and simvastatin were among the top 10 drugs dispensed in Australian community when expressed either as prescription counts or as defined daily dose/1000 population/day in 2010 [2].
The aim of this study was to analyse use of statins in the Australian veteran populationand how usage had changed over time with respect to dose and potency of statin prescribed. The veteran population is predominantly older and analysis of patterns of use of high potency statins may help health professionals to improve prescribing practice in order to reduce the risk of related adverse events in older patients, as advancing age and multiple comorbidities are recognised as characteristics contributing to increased risk of harm.
Methods
Data source
Administrative claims data provided by the Australian Government Department of Veterans' Affairs (DVA) was analysed. The data constitutes de-identified patient level information on all veterans who served in Australian Defence Forces, their spouses and dependants. Medicines subsidised under the Pharmaceutical Benefits Scheme or Repatriation Pharmaceutical Benefits Scheme (medicine dispensed, date of dispensing, quantity supplied, dosage form and strength) as well as patient age, gender, date of death, and residential status are recorded in the dataset. The DVA database also contains details of hospitalisations (dates of admission and discharge and primary diagnosis) provided to veterans for which DVA pay a subsidy.
Trends in statin use (2001-2012)
This study included all statin users in the Australian veteran population during the period of 2001-2012. All statins marketed in Australia were included: simvastatin, pravastatin, fluvastatin, atorvastatin and rosuvastatin (ATC codes: C10AA01, C10AA03, C10AA04, C10AA05, C10AA07) and the combination products (ezetimibe-simvastatin C10BA02 and amlodipine-atorvastatin C10BX03). Cerivastatin, which was withdrawn from the market in August 2001, was not included.
Monthly utilisation trends were established from 2001 to 2012 to determine how statin use changed over time. For each month, the monthly rate was calculated as the number of people who were using specific statin(s) in that month divided by the overall veteran population in that month. Whether a statin was used in a month was determined based on the date of supply and prescription duration. Analysis of time to prescription refill found that 75% of statin users return for their repeat prescription within 35 days. Thus, we assumed prescriptions duration to be 35 days from the date of supply, which is similar to using pack size of 30 days plus 5 days. Participants were followed until death or end of 2012.
Dose and potency of statins at initiation (2001-2012)
All patients who initiated statins between 2001 and 2012were identified. Initiation was defined as first ever dispensing for a given medicine (i.e. no dispensing for that medicine since the beginning of the dataset in 1999). Statin dose was categorised into low and high based on results from a meta-analysis that demonstrated the extent of low density lipoprotein cholesterol (LDL) reduction [14]. Doses that reduced LDL by less than 50% were considered low dose and included any dose of fluvastatin and pravastatin, simvastatin <40mg, atorvastatin <20mg and rosuvastatin <10mg (Table 1).
![]()
Table 1: Categorisation of statins by potency and dose.
View Table 1
The potency of statins was categorised into low and high based on Pharmaceutical Benefits Scheme (PBS) therapeutic relativity [15]. Atorvastatin, rosuvastatin and simvastatin 80mg were considered high potency, as these products have a price premium under the PBS, while simvastatin <40mg, fluvastatin and pravastatin were considered low potency[14] (Table 1).
All veterans who used statin in December 2012 were identified. Whether a statin was used in that month was determined based on the date of supply and prescription duration as described above.
Age and frailty may contribute to risk of adverse events. For this reason we hypothesised that older people (aged 85 years and older)and those living in aged care facilities would be more likely to be dispensed low potency or low dose statins. Differences in the potency or dose of statins used in December 2012 according to age (< 85 vs. >85 years) and residential status (living in a community vs. in residential aged care) were assessed.
To determine if statin potency and dose varied for primary or secondary cardiovascular prevention, we assessed whether use in December 2012 varied in those with a history of cardiovascular events (primary vs. secondary prevention). Cardiovascular diseases were defined based on the date of prior hospitalisation for ischaemic heart diseases (ICD-10 codes I20-I25) or cerebrovascular diseases (ICD-10 codes I60-I69) between 2001 and 2012. Participants with no hospitalisation for cardiovascular diseases before December 2012 were considered the primary prevention population. Patients who had hospitalisation for cardiovascular disease prior to December 2012 were considered as secondary prevention population.
Statistical analyses
The monthly utilisation rates were age-standardised using the veteran population in January 2007 as the standard population in five-year categories. Poisson regression models were used to calculate age-standardised rate ratios (SRR) to compare the rate in one year to the previous year where there was linear trend over time (2001-2012). Pearson's chi square tests were used to compare proportions. Multivariate analysis using multinomial logistic regression was undertaken to assess the independent contribution of age, residential status, and prior cardiovascular event as factors predicting use of statin potency and dose. Sex was not significant predictor and was not considered in the analysis. Analyses were performed using SAS 9.4 statistical package (SAS Institute, Cary NC, USA).
Results
Trends in statin use between 2001 and 2012
Overall, utilisation of statins increased among our elderly Australian population from 17% in January 2001 to 35% in December 2012 (SRR=1.059, 95% CI: 1.055-1.062, p< 0.0001) (Figure 1). Atorvastatin, a high potency statin, was the most commonly used statin. Its use increased steadily from the beginning of 2001, and has been stable since 2010 at approximately 16% (SRR=1.087, 95% CI: 1.082-1.093, p< 0.001) (Figure 1). Use of rosuvastatin, also a high potency statin, was increasing since its marketing in late 2006 and was used by 7% of the population in December 2012 (SRR=1.644, 95% CI: 1.579-1.709, p< 0.001). The use of simvastatin has been declining since 2005; however it was still used inaround 9% of the population at the end of the study period. The low potency pravastatin and fluvastatin were used in less than 5% of the population.
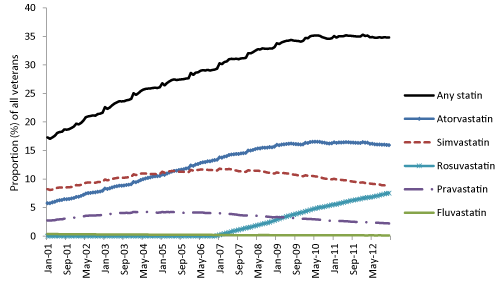
Figure 1: Trends in statin use among the veteran population (2001-2012).
View Figure 1
Figure 2 shows that overall use of statins shifted from low potency to high potency with time. The use of low potency/low dose statins decreased from 65% in January 2001 to 29% in December 2012 (SRR=0.931, 95% CI: 0.928-0.932, p< 0.001), while high potency/high dose use increased from 8% to 35% in the same period (SRR=1.122, 95% CI: 1.116-1.126, p< 0.001) and high potency/low dose - from 27% to 36% (SRR=1.030, 95% CI: 1.028-1.033, p< 0.001). In December 2012, 71% of all statin use was with high potency products.
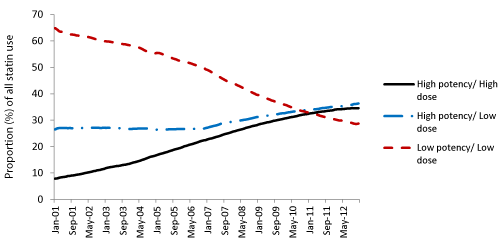
Figure 2: Use of statins by potency and dose (2001-2012).
View Figure 2
Dose and potency of statins at initiation, 2001-2012
Figure 3 presents the potency and dose of statin at initiation and shows that over time participantswere increasingly initiated on higher dose and higher potency products. In 2012, around 85% of all statin initiations were high potency statins. High potency/low dose statins were dispensed at treatment initiation at significantly higher rates (50.6%), compared to high potency/high dose statins (34.1%, chi-square p< 0.001) and to low potency/low dose (15.3%, chi-square p< 0.0001).
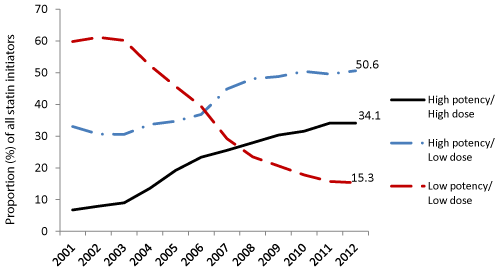
Figure 3: Initiation of statins by potency and dose (2001-2012).
View Figure 3
Statin use by age, in those in residential aged-care and in those with prior cardiovascular disease – snapshot for December 2012
There were 81,110 participants who were dispensed statins in December 2012. Of those, 51% were aged 85 years and over (N=41,596) and the rest were under 85 years (N=39,514).
High potency statinswere commonly used in both age groups; however, there was less use of the high dose products in the older age group (Figure 4). 41% of those aged under 85 years and approximately one in four of those 85 years and older were using high potency/high dose statin.
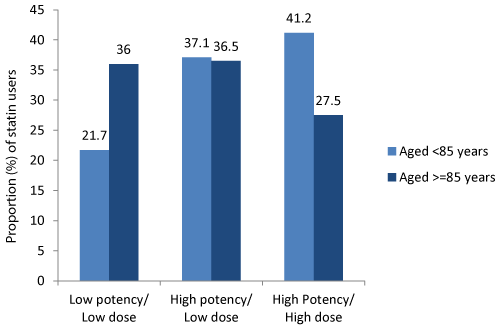
Figure 4: Statin potency and dose by age inDecember 2012 (N=81,110).
View Figure 4
The majority of patients on statins in December 2012 were living in the community (N=73,605, 91% of all). Figure 5 shows that high potency statins were used by 65% of those who were living in residential aged care and 72% of those living in the community. 29% ofpatients living in residential aged care and 35% of those living in the community were using high potency/high dose statins.
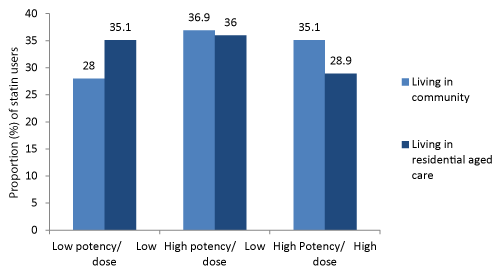
Figure 5: Use of statins in December 2012 by dose/potency and domicile (N=81,110).
View Figure 5
Of statin users in December 2012, 68% (N=54904) had no prior CV hospitalisation, and 32% (N=26206) had prior CV hospital admission. The prevalence of high potency/high dose statins was higher among secondary prevention patients than among primary prevention patients (Table 2). Overall, 30% of those with no prior CV hospitalisation and 44% of those with prior CV hospitalisation were dispensed high potency/high dose statins. Age stratification showed that approximately one in three patients aged < 85 years and one in five aged >85 were using high potency/high dose statins for primary prevention (Table 2). The high potency/high dose statins were used at higher proportions for secondary prevention in both age groups (54% in aged >85 and 36% in aged < 85).
![]()
Table 2: Statin potency and dose in primary and secondary prevention of cardiovascular diseases by age group in December 2012 (N=81,110).
View Table 2
Multivariate analysis
Multivariate analyses adjusted for age, residential status, and prior cardiovascular event shows that those aged >85 years were less likely to be using high potency/high dose statin compared to those aged less than 85 years (Table 3). Those living in residential aged care wereless likely to receive high potency/high dose statins than those living the community. Older people with prior cardiovascular events were more likely to use high potency/high dosestatins compared to those with no history of cardiovascular disease.
![]()
Table 3: Factors associated with statin potency and dose use in December
2012(low potency/low dose is used as a reference group).
View Table 3
Discussion
We found that the use of statins in veteran population increased from 2001 to 2012 with around one third using those medicines in 2012. We found increasing use of high dose and high potency products overall and at initiation. While therapy with higher doses or more potent statins lead to greater reduction in LDL cholesterol reducing further the risk of myocardial infarction and stroke [11,16], intense thera[8-11,17] and elevated liver enzymes[11,17]. Recognising that more than 80% of the LDL-lowering effect of any statin may be achieved with 50% of its maximum dose, it is recommended to start people with or without CV disease on a statin with moderate LDL-lowering effect [18]. Intensive lipid management should be reserved for patients with high CV risk after failing to achieve optimal lipid levels on lower doses and when benefits are expected to outweigh potential risks [19]. We found that 85% of all statin initiations in 2012 were on high potency statins, with one in three patients initiated on high potency/high dose statin. Statin use shifted from low to high potency with time, with high potency reaching 71% of all statin use in December 2012. The prevalence of high potency/high dose statins was higher among secondary prevention patients than among primary prevention patients (44% vs 30% in December 2012) consistent with guideline recommendations [19].
Administration of potent statins and statins at high doses in older population may increase the risk of statin related adverse events, as advancing age and multiple comorbidities are recognised as characteristics contributing to the increase of risk of side effects [20-22]. Our snapshot of statin use in December 2012 showed that people aged >85 years were less likely to be using high potency/high dose statin compared to younger patients aged< 85 years (28% vs 41%) which is in accord with the expected practice. People living in residential aged care are frailer and with multiple comorbidities – as expected we found that they were less likely to receive high potency/high dose statins than those living in the community (29% vs 35%). However, there was still significant use of high dose and high potency products in these patients groups which may increase the risk of side effects.
Conclusion
Statins were dispensed for around one-third of veteran population in 2012, withmajority of statin initiations and use being with high potency statins. Approximately one in threepatients living in residential aged care were using high potency/high dose statins. Their use was also common among people with no prior cardiovascular event (30%). While high potency/high dose statins were used less frequently in the very elderly; there werestill considerable numbers of older patients using high strength products, which may contribute to increased risk of harm.
References
-
AIHW (2010) Australia's health 2010. Australia's health no.12. Cat. no. AUS 122.
-
Australian Government Department of Health and Ageing (2011) Australian Statistics on Medicines 2010.
-
National Institute for Health and Clinical Excellence (2006) Statins for the prevention of cardiovascular events. [http://www.nice.org.uk/nicemedia/pdf/TA094guidance.pdf]
-
Naci H, Brugts JJ, Fleurence R, Tsoi B, Toor H, et al. (2013) Comparative benefits of statins in the primary and secondary prevention of major coronary events and all-cause mortality: a network meta-analysis of placebo-controlled and active-comparator trials. Eur J Prev Cardiol 20: 641-657.
-
Abramson J, Wright JM (2007) Are lipid-lowering guidelines evidence-based? Lancet 369: 168-169.
-
Cholesterol Treatment Trialists' (CTT) Collaborators, Mihaylova B, Emberson J, Blackwell L, Keech A, et al. (2012) The effects of lowering LDL cholesterol with statin therapy in people at low risk of vascular disease: meta-analysis of individual data from 27 randomised trials. Lancet 380: 581-590.
-
Sniderman A, Thanassoulis G, Couture P, Williams K, Alam A, et al. (2012) Is lower and lower better and better? A re-evaluation of the evidence from the Cholesterol Treatment Trialists' Collaboration meta-analysis for low-density lipoprotein lowering. J Clin Lipidology 6: 303-309.
-
Preiss D, Seshasai SR, Welsh P, Murphy SA, Ho JE, et al. (2011) Risk of incident diabetes with intensive-dose compared with moderate-dose statin therapy: a meta-analysis. JAMA 305: 2556-2564.
-
Holbrook A, Wright M, Sung M, Ribic C, Baker S (2011) Statin-associated rhabdomyolysis: is there a dose-response relationship? Can J Cardiol 27: 146-151.
-
Cham S, Evans MA, Denenberg JO, Golomb BA (2010) Statin-associated muscle-related adverse effects: a case series of 354 patients. Pharmacotherapy 30: 541-553.
-
Josan K1, Majumdar SR, McAlister FA (2008) The efficacy and safety of intensive statin therapy: a meta-analysis of randomized trials. CMAJ 178: 576-584.
-
Senes S, Penm E (2007) Medicines for cardiovascular health: are they used appropriately? Canberra, ACT: Australian Institute of Health and Welfare.
-
Stocks N, Ryan P, Allan J, Williams S, Willson K (2009) Gender, socioeconomic status, need or access? Differences in statin prescribing across urban, rural and remote Australia. Aust J Rural Health 17: 92-96.
-
Weng TC, Yang YH, Lin SJ, Tai SH (2010) A systematic review and meta-analysis on the therapeutic equivalence of statins. J Clin Pharm Ther 35: 139-151.
-
Australian Government Department of Health and Ageing (2012) Therapeutic relativity sheet. [http://www.pbs.gov.au/info/industry/pricing/pbs-items/therapeutic-relativity-sheets]
-
Law M, Wald N, Rudnicka A (2003) Quantifying effect of statins on low density lipoprotein cholesterol, ischaemic heart disease, and stroke: systematic review and meta-analysis. BMJ 326: 1423-1427.
-
Alsheikh-Ali AA1, Maddukuri PV, Han H, Karas RH (2007) Effect of the magnitude of lipid lowering on risk of elevated liver enzymes, rhabdomyolysis, and cancer: insights from large randomized statin trials. J Am Coll Cardiol 50: 409-418.
-
NPS Medicine Wise (2011) Managing lipids – reducing cardiovascular disease risk. NPS News.
-
Therapeutic Guidelines: Cardiovascular. Version 6, 2012. Melbourne: The Therapeutic Guidelines Ltd.
-
Maroo BP, Lavie CJ, Milani RV (2008) Efficacy and safety of intensive statin therapy in the elderly. Am J Geriatr Cardiol 17: 92-100.
-
Escobar C, Echarri R, Barrios V (2008) Relative safety profiles of high dose statin regimens. Vasc Health Risk Manag 4: 525-533.
-
Davidson MH, Robinson JG (2007) Safety of aggressive lipid management. J Am Coll Cardiol 49: 1753-1762.





