International Journal of Clinical Cardiology
A Case Report of Immediate Extubation Post Primary PCI in STEMI
Sharan Rufus Ponniah1*, Pradeepto Ghosh2, Nagapradeep Nagajothi2, Srinivasa Satti2, Kavitha Nidamanuri2 and Baskar Rajala3
1Department of Internal medicine, Canton medical education foundation, OH, USA
2Department of Cardiology, Aultman Hospital, OH, USA
3Department of Anesthesiology, University of Michigan, MI, USA
*Corresponding author: Sharan Rufus Ponniah, Department of Internal medicine, Canton Medical Education Foundation, 5908 Marzilli St NW Apt A3, Canton, OH, USA, Tel: 6108889502; E-mail: bondsharan@gmail.com
Int J Clin Cardiol, IJCC-1-014, (Volume 1 Issue 2), Case Report; ISSN: 2378-2951
Received: November 16, 2014 | Accepted: December 13, 2014 | Published: December 16, 2014
Citation: Ponniah SR, Ghosh P, Nagajothi N, Satti S, Nidamanuri K, et al. (2014) A Case Report of Immediate Extubation Post Primary PCI in STEMI.Int J Clin Cardiol 1:014. 10.23937/2378-2951/1410014
Copyright: © 2014 Ponniah SR. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
We report a case of immediate extubation following primary percutaneous intervention (PCI) for ST elevation myocardial infarction (STEMI). The optimal timing of extubation following revascularization in STEMI is unclear. Early extubation in this scenario, if feasible has a mortality benefit. Duration of mechanical ventilation following STEMI is a strong predictor of mortality. In this case, we report a scenario of immediate extubation following revascularization, which we believe contributed to the patient’s mortality benefit. We present this case to emphasize the importance of early withdrawal of mechanical support following revascularization in STEMI.
Keywords
ST elevation myocardial infarction, Cardiorespiratory arrest, Mechanical ventilation
Introduction
Cardio-respiratory arrest secondary to STEMI is not uncommon. However, the optimal time to extubation following primary PCI in a cardiac arrest scenario is unclear. Here, we present a case of immediate extubation following primary PCI in a patient presenting with cardio-respiratory failure secondary to STEMI.
Case Description
A 59-year-old Caucasian male with recent history of non-ST elevation myocardial infarction (NSTEMI) 2 weeks ago, presented to the emergency department with complaints of chest pain. Other significant past medical history included chronic obstructive pulmonary disease, bladder cancer receiving chemotherapy, and lung cancer and non-insulin dependent type II diabetes mellitus. During his recent NSTEMI, coronary angiography showed a 95% lesion in the mid-left circumflex artery, which was thought to be the culprit lesion. There was also a 60-70% stenosis in the mid-segment of the right coronary artery and a 60-70% narrowing in the mid and distal left anterior descending artery. The patient underwent successful PCI with a bare metal stent to his left circumflex artery lesion. His discharge medication included Aspirin 325 mg daily, Plavix 75mg daily, metoprololtartrate 12.5mg twice daily, lisinopril 2.5mg daily and atorvastatin20 mg daily. He was compliant with his medications since his discharge.
The patient had been fine since his recent hospital admission until he started experiencing chest pain, which started at rest. The chest pain was 10/10 in intensity, sub sternal in location and non-radiating. It was similar in characteristics to the chest pain he experienced 2 weeks back. The patient was brought to the Emergency department within 45 minutes after onset of chest pain. On arrival to ER he was still complaining of chest pain, 10/10 intensity, not relieved with sublingual nitroglycerine administered by EMS. On arrival his heart rate was 88, blood pressure was 146/82 and respiratory rate of 22/min with a saturation of 98% on 2 liters nasal cannula. Initial labs revealed troponin I of < 0.01ng/ml and normal renal functions with a GFR> 60mls/min. A portable chest X-ray showed hypoventilatory changes with no acute cardio-respiratory pathology discernible on thex-ray.
A 12 lead EKG on arrival revealed sinus rhythm at 92 beats per minute with ST elevation in inferior leads II, III, a VF and reciprocal ST depression in anterior leads consistent with inferior ST elevation myocardial infarction (STEMI) (Figure 1). A STEMI alert was called.
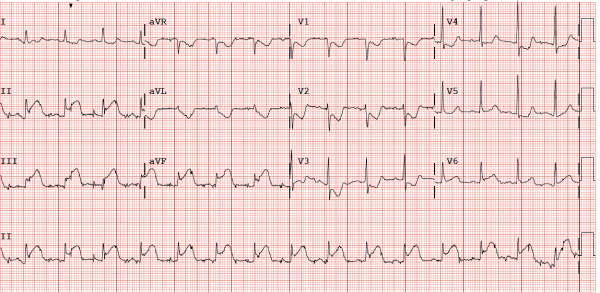 Figure 1: Patient’s electrocardiogram at presentation reveals sinus rhythm
with 4mm ST elevation in leads II, III, aVF and ST depression in leads V1
through V4.
View Figure 1
Figure 1: Patient’s electrocardiogram at presentation reveals sinus rhythm
with 4mm ST elevation in leads II, III, aVF and ST depression in leads V1
through V4.
View Figure 1
Shortly after arrival to emergency department, patient went into ventricular fibrillation and cardiac arrest. CPR was initiated as per ACLS protocol. He had to be defibrillated 9 times within a span of 13 minutes en route to the cardiac catheterization laboratory. Advanced airway was secured with endotracheal tube as part of cardio-respiratory arrest protocol. He regained sinus rhythm with a palpable pulse.
Coronary angiogram revealed 100% in-stent occlusion in the mid portion of left circumflex artery (Figure 2). The patient underwent successful thrombectomy and percutaneous intervention with a drug eluting stent (Figure 3). The patient stabilized hemodynamically post revascularization with resolution of arrhythmia. An intra-aortic balloon pump was therefore not required.
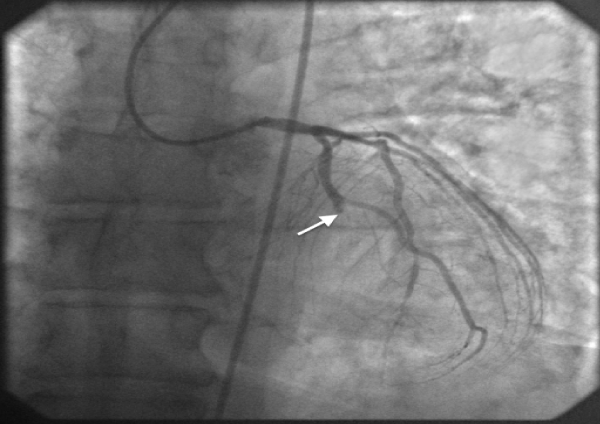 Figure 2: Coronary angiogram at presentation reveals total occlusion in the
mid portion of left circumflex artery.
View Figure 2
Figure 2: Coronary angiogram at presentation reveals total occlusion in the
mid portion of left circumflex artery.
View Figure 2
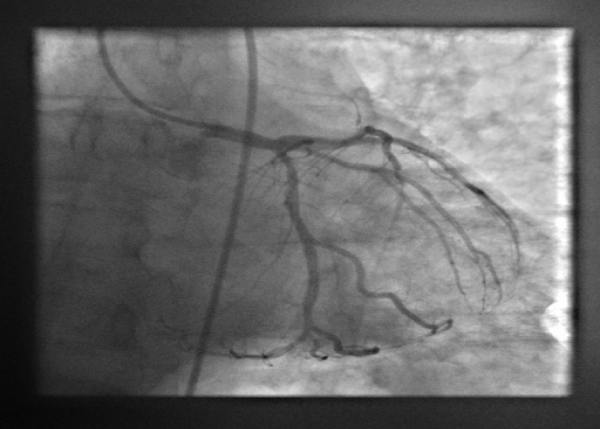 Figure 3: Coronary angiogram post PCI and stent deployment with TIMI 3
flow distally in the left circumflex artery.
View Figure 3
Figure 3: Coronary angiogram post PCI and stent deployment with TIMI 3
flow distally in the left circumflex artery.
View Figure 3
Post-procedure, the patient remained hemodynamically stable, chest pain free, was awake and following commands appropriately. There were no signs of acute congestive heart failure. Due to these reasons, we made the decision to immediately extubate him while in the cardiac catheterization laboratory. The extubation was successful.
The remainder of his hospital stay was uneventful. His cardiac troponin I peaked at 86.8mg/dl and an echocardiogram done 48 hours after the event revealed normal left ventricular systolic and diastolic function with no other abnormalities. He was maintained on dual anti-platelet therapy with Aspirin 81mg daily and Ticagrelor 90mg twice daily. He was discharged home after 4 days of hospitalization.
Discussion
Stent thrombosis is an uncommon but serious complication with an incidence of less than 1% [1]. Most cases of stent thrombosis present with ST elevation myocardial infarction [2]. Emergency PCI after stent thrombosis effectively restores vessel patency and flow [3]. It is not uncommon to find cardiorespiratory instability in patients presenting with STEMI. Cardiorespiratory instability prior to PCI is an independent risk factor for increased mortality [4]. Electrical instability of the myocardium during an acute coronary event can predispose to ventricular arrhythmias, especially ventricular fibrillation [5]. Most of these patients presenting with cardiac arrest require cardio-respiratory support in the form of mechanical ventilation. The need for mechanical ventilation during the early management of STEMI is a strong prognostic indicator of mortality both at short and long term [6]. The need for mechanical ventilation is also a predictor of depressed left ventricular function [5]. The duration of mechanical ventilation is associated with long-term mortality [4]. There are no standardized protocols to assess weaning in patients who undergo primary PCI.
Our patient needed ventilatory support due to cardiorespiratory collapse secondary to ventricular fibrillation from myocardialischemia. This was reversed with coronary re-vascularization. We feel that early extubation if possible is beneficial, considering that the duration of mechanical ventilation following STEMI strongly correlates with long-term mortality [4].The decision to extubate was made as per the recommended clinical criteria [7].
Conclusion
The duration of mechanical ventilation in patients presenting with STEMI is an independent predictor of long-term mortality. Patients who have undergone successful re-vascularization after STEMI with resolution of cardio-respiratory collapse should be assessed for extubation as soon as possible. We believe this will lead to a significant mortality benefit in these patients. Further studies are needed in this regard.
References
-
Cutlip DE, Baim DS, Ho KK, Popma JJ, Lansky AJ, et al. (2001) Stent thrombosis in the modern era: a pooled analysis of multicenter coronary stent clinical trials. Circulation 103: 1967-1971.
-
Armstrong EJ, Feldman DN, Wang TY, Kaltenbach LA, Yeo KK, et al. (2012) Clinical presentation, management, and outcomes of angiographically documented early, late, and very late stent thrombosis. JACC Cardiovasc Interv 5: 131-140.
-
Wenaweser P, Rey C, Eberli FR, Togni M, Tüller D, et al. (2005) Stent thrombosis following bare-metal stent implantation: success of emergency percutaneous coronary intervention and predictors of adverse outcome. Eur Heart J 26: 1180-1187.
-
Brener SJ, Brodie BR, Guerchicoff A, Witzenbichler B, Guagliumi G, et al. (2014) Impact of Pre-Procedural Cardiopulmonary Instability in Patients With Acute Myocardial Infarction Undergoing Primary Percutaneous Coronary intervention (from the Harmonizing Outcomes With Revascularization and Stents in Acute Myocardial Infarction Trial). Am J Cardiol 114: 962-967.
-
Volpi A, Cavalli A, Santoro L, Negri E (1998) Incidence and prognosis of early primary ventricular fibrillation in acute myocardial infarction--results of the Gruppo Italiano per lo Studio della Sopravvivenza nell'Infarto Miocardico (GISSI-2) database. Am J Cardiol 82: 265-271.
-
Lazzeri C, Valente S, Chiostri M, Attanà P, Mattesini A, et al. (2013) Mechanical ventilation in the early phase of ST elevation myocardial infarction treated with mechanical revascularization. Cardiol J 20: 612-617.
-
MacIntyre NR, Cook DJ, Ely EW Jr, Epstein SK, Fink JB, et al. (2001) Evidence-based guidelines for weaning and discontinuing ventilatory support: a collective task force facilitated by the American College of Chest Physicians; the American Association for Respiratory Care; and the American College of Critical Care Medicine. Chest 120: 375S-395S.





