International Journal of Clinical Cardiology
Cardiac Troponin Assessment Following Atrial Fibrillation Ablation: Implications for Chest Pain Evaluation
Jason C. Rubenstein1, Jason Jacobson2, Jeffrey J. Goldberger3, Rod Passman3, Alan Kadish3 and Michael H. Kim4*
1Division of Cardiology, Department of Medicine, Medical College of Wisconsin, Milwaukee, WI, USA
2Division of Cardiology, Westchester Medical Center, Valhalla, NY, USA
3Division of Cardiology, Feinberg School of Medicine, Northwestern University, Chicago, IL, USA
4Alpert Medical School of Brown University, Providence RI, USA
*Corresponding author: Michael H. Kim, Professor of Medicine, Alpert Medical School of Brown University, Providence RI, USA, Tel: 401-444-7997, Fax: 401-444-4652, E-mail: mkim4@lifespan.org
Int J Clin Cardiol, IJCC-1-011, (Volume 1, Issue 2), Research Article; ISSN: 2378-2951
Received: October 29, 2014 | Accepted: November 22, 2014 | Published: November 25, 2014
Citation: Rubenstein JC, Jacobson J, Goldberger JJ, Passman R, Kadish A, et al. (2014) Cardiac Troponin Assessment Following Atrial Fibrillation Ablation: Implications for Chest Pain Evaluation.Int J Clin Cardiol 1:011. 10.23937/2378-2951/1410011
Copyright: © 2014 Rubenstein JC, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Abstract: The range of elevation of troponin I (tI) that is within expected limits from left atrial radiofrequency ablation for atrial fibrillation (AF) is not well described, though such information may be of clinical value.
Objectives: Identify the expected range of tI values post-atrial fibrillation (AF) ablation.
Methods: 31 patients undergoing AF ablation had a single tI level drawn the day following the procedure. Clinical variables were also collected, such as ablation type and radiofrequency (RF) time.
Results: Paroxysmal AF was present in 23 patients, and 8 had chronic AF. The average RF time was 2627.8 + 737.5 seconds. The mean RF power was 61.7 + 4.3W (range 55-70W). The mean RF temperature limit was 53.6 + 2.00C (range 50-550C). There was no clinical or electrocardiographic evidence of coronary ischemia in this population. The mean tI the following day was 3.21 + 1.5 (range 1.48-8.41). There was no correlation between RF time, ablation type, ablation catheter size, and ablation temperature or ablation power and tI levels.
Conclusions: Troponin I elevation post-ablation was ubiquitous. Knowledge of expected post-ablation tI levels may be helpful in the evaluation of post-procedure chest pain.
Keywords
Atrial fibrillation, Ablation, Troponin, Chest pain
Introduction
Left atrial radiofrequency (RF) ablation is an established procedure for the treatment of atrial fibrillation (AF) [1,2] and is increasingly being applied in the AF population. Cardiac RF ablation causes myocardial necrosis that can be detected through the use of cardiac enzyme markers such as troponin I (tI) [3,4]. Troponin I levels peak at 12 to 16 hours and may remain elevated for up to two weeks after myocardial injury. The range of elevation of tI that is within expected limits due to RF ablation is known immediately post procedure, but the expected levels at longer follow-up times are not well described, though such information may be important both as a marker for the extent of ablation and in the evaluation of post-procedure chest pain [5].
Methods
A prospective cohort of 31 patients undergoing curative AF Ablation had a single tI level (Beckman-Coulter) drawn the day following the procedure. A tI level of < 0.04ng/mL was considered normal by the laboratory, 0.04 ng/mL to < 0.06ng/mL considered suggestive of cardiac damage, and >0.5ng/mL considered consistent with myocardial infarction. The upper reference limit was 0.04ng/mL. Clinical variables were also collected, such as ablation type and radiofrequency (RF) time. Basic demographic information, RF parameters, tI level, and AF ablation outcomes were recorded. Results are expressed as mean + standard deviation, unless otherwise noted. Discrete variables were compared across patient groups using the Chi-Square, Fisher, or Spearman tests where appropriate. Continuous variables were compared with Student's t-test or Mann-Whitney tests, where appropriate. A two-tailed p-value < 0.05 was considered statistically significant. All analysis was performed using SPSS 16.0 (SPSS Inc, Chicago, IL).
Results
The average age in this patient population was 56.9 + 10.9 years. Paroxysmal AF was present in 23 patients, and 8 had chronic AF. Patients were generally healthy with no patients with severe heart failure, LV dysfunction/cardiomyopathy, or renal failure. Patients underwent linear wide-area circumferential ablation (WACA) with additional linear lesions (roof and mitral) (n=18), WACA plus segmental pulmonary vein isolation (PVI) (n=7), or PVI only (n=6). The average RF time was 2627.8 + 737.5 seconds. The mean RF power was 61.7 + 4.3W (range 55-70W). The mean RF temperature limit was 53.6 + 2.00C (range 50-550C). The most commonly used ablation catheter tip size was 8mm (81.2% of cases), with 9.4% cases using standard 4mm tips and 6.2% using both 8mm and 4mm ablation catheters. There was no clinical or electrocardiographic evidence of coronary ischemia in this population. The mean tI the following day was 3.21 + 1.5 (range 1.48-8.41). There was no correlation between RF time (p=0.459), ablation temperature (p=0.888) or ablation power (p=0.275) and tI levels (Figure 1). Ablation type (p=0.431) nor ablation catheter size (p=0.620) was predictive of tI levels.
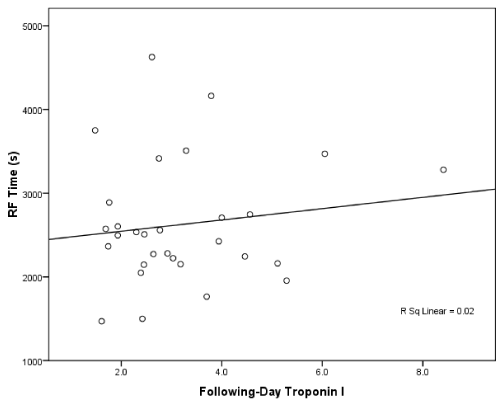 Figure 1: The correlation between RF ablation duration and following-day
troponin I elevation.
View Figure 1
Figure 1: The correlation between RF ablation duration and following-day
troponin I elevation.
View Figure 1
All patients (100 %) had tI levels above both the upper reference limit (0.04ng/mL) and the upper limit of normal in our laboratory (>0.5ng/mL). The lowest recorded tI was more than double the upper limit of normal. The extent of tI elevation was not predictive of AF ablation success rates (CI 0.507-1.418, p=0.53) (Figure 2).
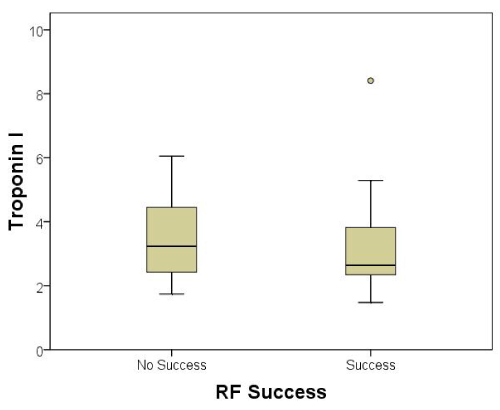 Figure 2: The relationship between the following-day troponin I elevation and
long-term clinical success of the atrial fibrillation ablation.
View Figure 2
Figure 2: The relationship between the following-day troponin I elevation and
long-term clinical success of the atrial fibrillation ablation.
View Figure 2
Discussion
The primary finding of this study is that troponin I elevations in the diagnostic range for myocardial infarction are ubiquitous 1 day after AF ablation, with a mean value of 3.21 (6.4 times the local laboratory cutoff for myocardial infarction). The main value of these data on tI elevations after AF ablation are to provide a reasonable reference range of what may be expected quantitatively in terms of tI. Clinicians assessing a patient with chest pain shortly following an AF ablation may find this of value for medical decision making.
These values were obtained in a younger population of patients typical of an AF ablation cohort without major comorbidities. These values would be inconsistent with any small release of troponin due to recent rapid ventricular rates in AF prior to ablation, which was, not an issue in the study population. None of our patients had severe heart failure or renal failure to account for chronic troponin elevations.
Prior published reports on troponin elevation after AF ablation have only looked at the immediate time period post-ablation. Haegeli et al. [5] examined troponin T levels 4 hrs post-ablation using a 4 mm ablation catheter in 60 patients, and found the mean troponin T to be 0.85ng/mL (5.7 times local laboratory cutoff for myocardial infarction). The degree of elevation did not correlate with common ablation parameters, such as ablation strategy or RF time. Post-ablation chest pain is a common complaint in this patient population, and physicians commonly rely on cardiac enzymes to determine the clinical significance of these symptoms. The time period of 4 hours in Haegeli et al. is likely not long enough to reflect peak levels, and may under-represent the level of troponin that is to be expected following ablation. While our data examined troponin I, the levels found (3.21 + 1.5ng/mL, range 1.48-8.41) were comparably slightly higher. These levels, while elevated, are an expected product of AF ablation and some reference values for clinical management would be of assistance in evaluating patients with chest pain after AF ablation.
Chest pain after AF ablation is generally not associated with ischemia, but for other reasons such as pericarditis. Knowledge of the expected range of troponin elevation following AF ablation should be helpful and may assist clinicians in the evaluation of chest pain shortly after AF ablation. For example, values of troponin markedly more than seen in this study could suggest non-AF ablation-related chest pain such as myocardial ischemia which can occur in left atrial procedures [6].
Limitations
These data are limited by the small sample size and thus may not reflect the full range of values. A larger sample may have provided a greater range. In addition, only a single troponin value was available, so it was not possible to analyze tI values over time or to compare them from baseline. Furthermore, the range of expected values from irrigated tip catheters or cryoballoon ablation may vary and were not assessed in this study.
References
-
Haissaguerre M, Jais P, Shah DC, Takahashi A, Hocini M, et al. (1998) Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med 339: 659-666.
-
Oral H, Pappone C, Chugh A, Good E, Bogun F, et al. (2006) Circumferential pulmonary-vein ablation for chronic atrial fibrillation. N Engl J Med 354: 934-941.
-
Cappato R, Calkins H, Chen SA, Davies W, Iesaka Y, et al. (2005) Worldwide survey on the methods, efficacy, and safety of catheter ablation for human atrial fibrillation. Circulation 111: 1100-1105.
-
Wellens HJ (1999) Catheter ablation of cardiac arrhythmias: usually cure, but complications may occur. Circulation 99: 195-197.
-
Haegeli LM, Kotschet E, Byrne J, Adam DC, Lockwood EE, et al. (2008) Cardiac injury after percutaneous catheter ablation for atrial fibrillation. Europace 10: 273-275.
-
Simon RD, Gill JS (2003) Coronary ischemia induced by radiofrequency ablation in the left atrium. J Cardiovasc Electrophysiol 14: 186-190.





