International Journal of Clinical Cardiology
Rheumatic Mitral Restenosis with Concomitant Coronary artery Disease
Anupam Dey1*, Ramesh Aggarwal2 and Shridhar Dwivedi3
1Department of Medicine, All India Institute of Medical Sciences, Bhubaneswar, India
2Department of Medicine, Lady Hardinge Medical College and Associated Smt. Sucheta Kriplani Hospital, Dr. Ram Manohar Lohia Hospital, India
3Department of Medicine / Preventive Cardiology, Hamdard Institute of Medical Sciences and Research & HAH Centenary Hospital, Jamia Hamdard, (Hamdard University), India
*Corresponding author: Dr. Anupam Dey, Department of Medicine, AIIMS, Sijua, Bhubaneswar-751019, India, Tel: 919438884202; E-mail: anupamdey.7@gmail.com.
Int J Clin Cardiol, IJCC-1-007, (Volume 1, Issue 2), Letter to Editor; ISSN: 2378-2951
Received: October 21, 2014 | Accepted: November 19, 2014 | Published: November 21, 2014
Citation: Dey A, Aggarwal R, Dwivedi S (2014) Rheumatic Mitral Restenosis with Concomitant Coronary artery Disease.Int J Clin Cardiol 1:007. 10.23937/2378-2951/1410007
Copyright: © 2014 Dey A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Keywords
Coronary, Mitral, Rheumatic, Repair, Stenosis
Rheumatic heart disease (RHD) has practically vanished from developed countries; however one often sees complicated rheumatic valvular disease in elderly individuals, in developing countries. It is not very common to see operated cases of mitral stenosis (MS) coexisting with coronary artery disease (CAD). Studies have reported prevalence of CAD coexisting with rheumatic MS ranging from 1.7% [1] to 28% [2]. We recently had a case of rheumatic MS, who was operated twice, had again developed restenosis, and presented with acute coronary syndrome (ACS) attributed to angiographically documented double vessel disease. Absence of traditional risk factors like smoking, obesity, and diabetes, and the diagnostic and therapeutic issues involved in such condition prompted us to report this case.
A-60-yr-old male presented with sudden onset of severe retrosternal chest pain radiating to left arm, and aggravating on exertion along with anxiety and diaphoresis. He had no history of vomiting or cough or fever. There was a significant history of RHD for the last 40 years. He was diagnosed as severe MS and underwent closed mitral valvotomy (CMV) at age 18 years and was on penicillin prophylaxis and digoxin henceforth. However symptoms recurred and became progressive after next 25 yrs when he developed restenosis, and, he underwent percutaneous transvenous mitral commissurotomy (PTMC) at age 46 years. He was subsequently stable on medications. He is a nonsmoker and nonalcoholic.
His BP was 160/90mmHg and pulse rate 98/min, irregularly irregular. Pedal edema, pallor and cyanosis were absent. BMI was 20.96Kg/sq.m and Waist measured 86cm. CVS examination revealed a loud S1, mid diastolic rumbling murmur. Chest inspection showed a postoperative linear scar extending from anteriorly below nipples through the entire lateral chest wall (Figure-1). Abdomen and CNS were normal. ECG showed ST segment depression in V2 to V6 and limb leads II, III, aVF with atrial fibrillation (AF) and controlled ventricular rate. Troponin T was positive. Chest x-ray showed cardiomegaly and prominence of pulmonary arteries (Figure 2). Blood sugar, serum creatinine, serum lipids and hemogram were all within normal limits. He was diagnosed as CAD with non ST elevation myocardial infarction and managed in hospital. He underwent coronary angiography which showed significant obstruction in mid left anterior descending artery (LAD) and non significant obstruction in right coronary artery (RCA). Echocardiography showed severe mitral stenosis with calcified valves, mitral valve apparatus-0.8 sq. cm, mild mitral regurgitation (MR), trivial aortic regurgitation, dilated left atrium and left ventricle, global hypokinesia with ejection fraction 25%. The important dimensions were LA end systolic(es) 50mm , LVes 40mm, LV end diastolic(ed) 48mm, PW ed 9mm, mitral valve mean diastolic gradient 10mm Hg, and aorta 33mm. There was no clot in left atrium. Right atrium and right ventricle were normal. Later on he successfully underwent mitral valve repair (MVR) along with coronary artery bypass grafting (CABG).
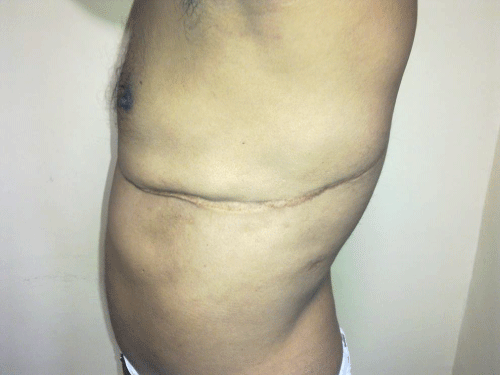
Figure 1: Postoperative scar mark (left lateral chest).
View Figure 1
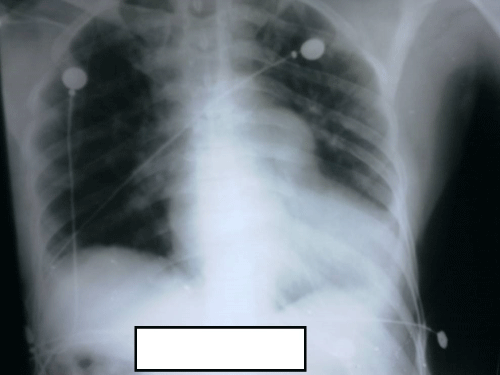
Figure 2: Chest radiograph showing cardiomegaly and prominence of
pulmonary arteries.
View Figure 2
RHD is fairly prevalent in South East Asia. The predominant cause of MS is rheumatic fever. About 25% of all patients with RHD have isolated MS, and about 40% have combined MS and MR. Cases of CAD occurring in patients with preexisting RHD are known, but there is relatively lesser literature in India. Jose VJ had shown the prevalence of coronary artery disease in patients with rheumatic heart disease undergoing valve surgery in India as 12.2% and more in aortic than mitral valve disease [3]. Manjumnath CN et al. in their study in Indian subjects have shown that coronary artery disease is relatively uncommon in patients with rheumatic valvular heart disease (4.9%), and its prevalence is highest in degenerative aortic valve disease (23.4%) [4]. Although the possibility of coronary arteritis secondary to rheumatic fever has been discussed, but any association of RHD with CAD has not been proven. CAD may coexist silently with severe MS, as angina pectoris is often a poor predictor of CAD [2]. Mattina CJ et al. [2] showed coexistent CAD in 28 % patients of MS over the age of 40 years. They pointed out that coronary artery sclerosis is common in this population and it can be clinically silent. Alexopoulos D et al. [5] found the prevalence of CAD higher in non-rheumatic valvular heart disease as compared to rheumatic etiology, and that there is predominance of the male sex and older age.
It is interesting to note that the risk factors for CAD in this patient were his advancing age and hypertension. However he was nontobacco user had reasonably normal weight and normal lipids and sugar. Kruczan et al. [6] from Brasil found that the variables most strongly associated to CAD in patients with valvular heart disease, were typical chest pain, diabetes mellitus and dyslipidemia.
Preoperative coronary angiography before valvular surgery, can demonstrate coronary artery disease. Moreover the coronary angiography is indicated as a routine procedure in the preoperative assessment of patients with valvular heart disease in males aged = 35 years, pre-menopausal females aged = 35 years with cardiovascular risk factors and post-menopausal females [7].
Mitral valve repair (commissurotomy) is the preferred surgical treatment for severe MS in elderly, but mitral valve replacement is often necessary as the valvular morphology in elderly adults is usually unfavorable due to extensive calcification, rigidity and retraction of valve components. Since our patient had already undergone corrective procedures twice, hence valve replacement was desirable. With significant involvement of his left anterior descending artery along with non-significant right coronary involvement, CABG was the better choice since it can prolong life and can be performed in the same setting as the valvular replacement.
References
-
Chu PH, Chiang CW, Hsu LA, Lin KH, Cheng NJ, et al. (2001)Low prevalence of coronary arterial disease in Chinese adults with mitral stenosis.Chang Gung Med J 24: 97-102.
-
Mattina CJ, Green SJ, Tortolani AJ, Padmanabhan VT, Ong LY, et al.(1986) Frequency of angiographically significant coronary arterial narrowing in mitral stenosis. Am J Cardiol57: 802-805.
-
Jose VJ, Gupta SN, Joseph G, Chandy ST, George OK, et al. (2004) Prevalence of coronary artery disease in patients with rheumatic heart disease in the current era. Indian Heart J56:129-131.
-
Manjunath CN, Agarwal A, Bhat P, Ravindranath KS, Ananthakrishna R, et al. (2014) Coronary artery disease in patients undergoing cardiac surgery for non-coronary lesions in a tertiary care centre.Indian Heart J 66:52-56.
-
Alexopoulos D, Kolovou G, Kyriakidis M, Antonopoulos A, Adamopavlos S, et al. (1993) Angina and coronary artery disease in patients with aortic valvular disease. Angiology 44: 707-711.
-
Kruczan DD, Silva NA, Pereira Bde B, Rom�o VA, Correa Filho WB, et al. (2008) Coronary Artery Disease in Patients with Rheumatic and Non-Rheumatic Valvular Heart Disease Treated at a Public Hospital in Rio de Janeiro. Arq Bras Cardiol90: 217-223.
-
Bonow RO, Carabello BA, Chattergee K, de Leon AC Jr, Faxon DP, et al. (2006) ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/AHA Task Force on Practice guidelines. J Am Coll Cardiol 48: 1-148.





