International Journal of Anesthetics and Anesthesiology
Treatment-Resistant Severe Hypothermia in an Infant Caused by the AirSeal® Insufflator
Kiyotaka Nakagawa1,2*, Kazuo Arakawa1,3, Tomohide Kamiya1,2, Koichi Kataoka1 and Katsuhiro Sakai1,3
1Department of Anesthesia, Kawaguchi Municipal Medical Center, Japan
2Department of Anesthesiology, Jikei University School of Medicine, Japan
3Department of Anesthesiology, Nihon University School of Medicine, Japan
*Corresponding author: Kiyotaka Nakagawa, MD, PhD, Vice-director, Department of Anesthesia, Kawaguchi Municipal Medical Center, 180 Nishi-araijyuku, Kawaguchi-shi, Saitama, 333-0833, Japan, Tel: 81 48 287 2525, Fax: 81 48 280 1566, E-mail: k-n@jikei.ac.jp
Int J Anesthetic Anesthesiol, IJAA-4-056, (Volume 4, Issue 1), Case Report; ISSN: 2377-4630
Received: January 18, 2017 | Accepted: February 27, 2017 | Published: March 02, 2017
Citation: Nakagawa K, Arakawa K, Kamiya T, Kataoka K, Sakai K (2017) Treatment-Resistant Severe Hypothermia in an Infant Caused by the AirSeal® Insufflator. Int J Anesthetic Anesthesiol 4:056. 10.23937/2377-4630/1410056
Copyright: © 2017 Nakagawa K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The valveless trocar system is a novel insufflator that circulates carbon dioxide in the abdominal cavity. Herein, we report an infant with severe hypothermia due to use of this insufflator. An 83-day-old infant (body weight 3862 g) with gastroesophageal reflux underwent laparoscopic Nissen fundoplication. After insufflation was initiated, his body temperature acutely dropped to 34.4 °C. Standard treatments had no effect on the patient's hypothermia. The valveless trocar system can decrease body temperature due to circulated insufflation gas, and this may be especially severe in infants. The valveless trocar system should not be applied to infants without heating and humidifying the insufflation gas.
Keywords
Trocar, Insufflation, Laparoscopic surgery, Hypothermia, Infant
Introduction
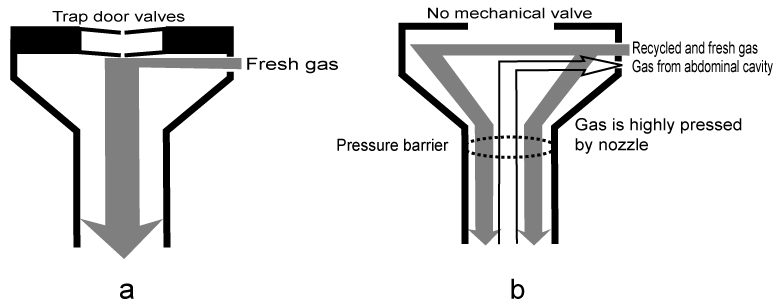
Conventional insufflation systems fill the abdominal cavity, which is sealed with mechanical valves, with carbon dioxide (Figure 1a); however, there are some disadvantages associated with these systems. The insufflation gas often leaks, and insufflation pressure continues to decrease during the exchange of surgical instruments. Furthermore, the valves are smudged by this exchange, and this stains the camera, which then has to be cleaned frequently. Evacuation of surgical smoke is often necessary to obtain a good surgical site, but these results in decreased insufflation pressure. Moreover, refilling lost gas to recover insufflation pressure is a slow process due to intermittent pressure sensing. Thus, disadvantages of conventional systems include time loss and obstruction of the surgical procedure. A novel insufflation system, namely a valveless trocar system (AirSeal® Intelligent Flow System; CONMED, Utica, NY, USA), maintains insufflation pressure by circulating gas in the abdominal cavity, which is sealed by gas downflow in the trocar instead of mechanical valves (Figure 1b). As there are no valves, gas leakage and camera smudge due to the exchange of surgical instruments are generally avoided. Insufflation gas contains surgical smoke, which is continuously eliminated by circulated gas. The returned smoky gas is cleared and re-sent to the abdominal cavity along with fresh gas. Insufflation gas is rapidly refilled as necessary through continuous pressure sensing. Consequently, insufflation pressure is always stably maintained. These advantages are valuable during operations and have been well documented [1]. There have been few previous reports on the harmful effects of this system. However, the valveless trocar system can decrease body temperature by circulating insufflation gas. There has been only one previous case report of this system causing a body temperature decrease of 1.7 °C in a 1.8 kg-infant [2]. The report described the advantages of this system for surgeons performing surgery in an infant, but did not discuss body temperature in detail. Herein, we report an infant with treatment-resistant severe hypothermia due to use of this insufflator system.
.
Figure 1: Sectional schemata of trocars.
a) Conventional trocar: Insufflation gas fills the abdominal cavity, which is sealed by mechanical trap door valves. Gas is suctioned through the insufflation cock or through other trocars' cocks; b) Valveless trocar: A trocar without mechanical valves has a nozzle structure. This structure causes downflow of the insufflation gas, which provides sufficient pressure to seal the abdominal cavity without the use of mechanical valves. Gas is continuously circulated in the abdominal cavity.
View Figure 1
Case Report
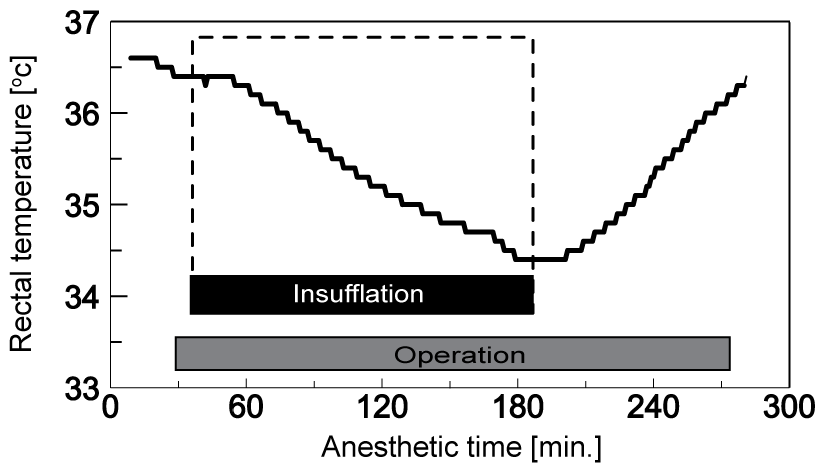
A mechanically ventilated 83-day-old infant (body weight 3862 g) with respiratory failure and gastroesophageal reflux underwent laparoscopic Nissen fundoplication using a valveless trocar system (small open gastrostomy and tracheostomy). This system was used as part of a clinical demonstration with the vendor (Century Medical, Inc. Tokyo, Japan). The patient was administered general anesthesia with sevoflurane, fentanyl, remifentanil, and rocuronium. Crystalloid fluid was continuously administered at a rate of approximately 4 mL/kg/h, and the room temperature was maintained at approximately 29 °C. A heat and moisture exchanger (Gibeck Humid-Vent® Mini; Teleflex Medical, Athlone, Ireland) was used for humidification of the airway. To prevent hypothermia, clothes were placed on the infant and a convective forced-air heater (WarmTouch, Covidien Inc., Mansfield, MA, USA) was used. The patient's rectal temperature just before insufflation was 36.4 °C. However, the rectal temperature began to acutely fall 21 minutes after initiation of insufflation, and 145 minutes after initiation of insufflation, the rectal temperature reached 34.4 °C (Figure 2). A heating lamp and hot packs were utilized while the patient's body temperature dropped. In addition, the temperature settings of the forced-air heater and room air conditioner were increased. However, these treatments had no effect on the patient's hypothermia. After insufflation ended, the rectal temperature began to increase, and 94 minutes after insufflation, the rectal temperature had returned to baseline (before the laparoscopic procedure). Obvious adverse effects of hypothermia were not observed in this patient after the operation.
.
Figure 2: Changes in rectal temperature. Rectal temperature was severely decreased during insufflation. After insufflation, the temperature rapidly increased, and this temperature change corresponded with insufflation.
View Figure 2
Discussion
We observed two important clinical issues in this case. The valveless trocar system can cause treatment-resistant severe hypothermia in infants, and heating and humidifying the insufflation gas is necessary for the use of this system in infants.
First, the valveless trocar system can cause treatment-resistant severe hypothermia in infants. Considering the above-mentioned case report, hypothermia due to the valveless trocar system is not specific to our case [2]. Anesthesia impairs thermoregulatory control; under this condition, body heat is lost in the cool operating room environment, and the heat loss often results in hypothermia [3]. In this case, four factors of heat loss should be considered: the body surface and operation site (except in cases of laparoscopic procedure); the insufflated abdominal cavity; the airway; and the intravenous fluid. Standard measures to protect against heat loss from the body surface were applied in this case. The patient's body temperature decreased slightly immediately after anesthesia was administered, but decreased severely during insufflation; body temperature promptly recovered after insufflation ended. As the temperature changes corresponded with insufflation, it was clear that most heat loss was due to circulated gas produced by the valveless trocar system. Airway evaporation causes loss of body heat [3]. Airway evaporation may be prevented with heated humidification (active humidification) or a heat and moisture exchanger (passive humidification). Passive devices are less effective than active devices in terms of preventing heat loss [4-6]. We used a passive device; nevertheless, because heat loss from the airway does not contribute much to body temperature, heat loss via the airway did not likely contribute to the decrease in body temperature in this case. Hypothermia can also be caused by large volumes of cold intravenous fluid [6]. In our case, the intravenous fluid was warmed before administration but was not continuously warmed. Therefore, the intravenous fluid may have been cold. However, it is unlikely that the low volume of fluid in this case affected the patient's body temperature. Consequently, it is considered that severe hypothermia caused by the valveless trocar system may not respond to standard treatment in infants.
Second, when the valveless trocar system is used on infants, it is necessary to heat and humidify the insufflation gas. Many studies have reported that heating and humidifying insufflation gas prevents decreases in body temperature, while the effect of only heating, not humidifying, insufflation gas is controversial [7]. The valveless trocar system recycles gas, which is heated and humidified by living tissue. Recycled gas is cooled as it passes through the insufflation tube. Fresh gas, which is not heated and humidified, is added at a rate of approximately 3-15 L/min. Consequently, cool, dry gas at a flow rate of more than 3 L/min is continuously circulated in the abdominal cavity at all times. This cool, dry gas might not affect body temperature in adults; however, hypothermia in children may be avoided by warming the insufflating gas and/or by maintaining a flow rate of less than 2 L/min [8]. Our case suggests that circulating cool and dry gas with use of the valveless trocar system may seriously affect the body temperature of infants. Moreover, hypothermia in this case strongly resisted standard treatment. Therefore, this system must not be used on infants, unless the apparatus is equipped to heat and humidify gas.
In conclusion, the valveless trocar system can cause treatment-resistant severe hypothermia in infants and thus would require heating and humidifying the insufflation gas for infant use. While the previous operator's manual for the valveless trocar system (ver. 1.5, 2012) included a warning to warm the insufflation gas to avoid hypothermia, the more recent manual (Revision 09/2015-06/ama, 2015) does not include this warning. Nevertheless, the valveless trocar system should not be applied to infants without heating and humidifying the insufflation gas.
Acknowledgements
We thank the neonatal pediatrician, Dr. Asami Shinbo at Kawaguchi Municipal Medical Center, for her support with this report.
This work is from Kawaguchi Municipal Medical Center. There is no conflict of interest. This report was solely supported by our departmental foundation (Department of Anesthesia, Kawaguchi Municipal Medical Center).
Part of this case was presented in Japanese at the 55th Annual Meeting of Japanese Society of Anesthesiologists Tokyo-Kanto Region on September 5, 2015.
Ethical Statement
The patient's mother provided written informed consent for publication of this report, and the institutional ethics committee of Kawaguchi Municipal Medical Center permitted publication of this report.
References
-
Horstmann M, Horton K, Kurz M, Padevit C, John H (2013) Prospective comparison between the AirSeal® System valve-less Trocar and a standard Versaport™ Plus V2 Trocar in robotic-assisted radical prostatectomy. J Endourol 27: 579-582.
-
Miyano G, Morita K, Kaneshiro M, Miyake H, Nouso H, et al. (2015) Laparoscopic Toupet Fundoplication using an Air Seal Intelligent Flow System and Anchor Port in a 1.8-kg infant: A Technical Report. Asian J Endosc Surg 8: 357-560.
-
Luginbuehl I, Bissonnette B, Davis PJ (2011) Thermoregulation: Physiology and Perioperative Disturbances. In: Davis PJ, Cladis FP and Motoyama EK, Smith's Anesthesia for Infants and Children. (8th edn), Elsevier Mosby, Philadelphia, 157-178.
-
Bissonnette B, Sessler DI, LaFlamme P (1989) Passive and active inspired gas humidification in infants and children. Anesthesiology 71: 350-354.
-
Bissonnette B, Sessler DI (1989) Passive or active inspired gas humidification increases thermal steady-state temperatures in anesthetized infants. Anesth Analg 69: 783-787.
-
Sessler DI (2015) Temperature Regulation and Monitoring. In: Miller RD, Miller's Anesthesia. (8th edn), Elsevier Saunders, Philadelphia, 1622-1646.
-
Binda MM (2015) Humidification during laparoscopic surgery: overview of the clinical benefits of using humidified gas during laparoscopic surgery. Arch Gynecol Obstet 292: 955-971.
-
Hammer G, Hall S, Davis PJ (2011) Anesthesia for General Abdominal, Thoracic, Urologic, and Bariatric Surgery. In: Davis PJ, Cladis FP and Motoyama EK, Smith's Anesthesia for Infants and Children. (8th edn), Elsevier Mosby, Philadelphia, 745-785.





