International Journal of Anesthetics and Anesthesiology
Ultrasound-guided Transmuscular Quadratus Lumborum (TQL) Block for Pain Management after Caesarean Section
Nina Mænchen, Christian Kruse Hansen, Mette Dam and Jens Børglum*
Department of Anaesthesia and Intensive Care Medicine, Zealand University Hospital, University of Copenhagen, Denmark
*Corresponding author: Jens Børglum, Department of Anesthesia and Intensive Care Medicine, Zealand University Hospital, University of Copenhagen, Sygehusvej 10, DK-4000 Roskilde, Denmark, Tel: +45-3070 0120, Fax: +45-4732 3601, E-mail: jens.borglum@gmail.com
Int J Anesthetic Anesthesiol, IJAA-3-048, (Volume 3, Issue 2), Case Report; ISSN: 2377-4630
Received: February 08, 2016 | Accepted: June 25, 2016 | Published: June 28, 2016
Citation: Mænchen N, Hansen CK, Dam M, Børglum J (2016) Ultrasound-guided Transmuscular Quadratus Lumborum (TQL) Block for Pain Management after Caesarean Section. Int J Anesthetic Anesthesiol 3:048. 10.23937/2377-4630/3/2/1048
Copyright: © 2016 Mænchen N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The ultrasound-guided transmuscular quadratus lumborum (TQL) block performed in the lumbar paravertebral region exerts its effect by spreading into the thoracic paravertebral space with blockade of both somatosensory and visceral nerves of the abdominal and retroperitoneal region. We discovered an inadequate management of post-operative pain by the conventional analgesic regimen among caesarean section patients in our hospital. In this report we present three cases where the TQL block is demonstrated as an effective tool of opioid sparing, pre-emptive anaesthesia as well as rescue analgesia. We propose the use of TQL block as a safe and reliable alternative to transversus abdominis plane block, paravertebral block and epidural blockade.
Keywords
Transmuscular quadratus lumborum block, Caesarean section, Ultrasound-guided blockade, Pre-emptive analgesia, Post-operative pain management
Introduction
The ultrasound-guided (USG) quadratus lumborum (QL) block was first described in an abstract in 2007 by Dr. Blanco as a modification of the classical landmark based transversus abdominis plane (TAP) block [1]. The specific technique and the endpoint of the injection were not described. However, it was later elucidated that the main advantage of the QL block was an extension of the local anaesthetic beyond the TAP-plane spreading into the thoracic paravertebral space with the provision of both visceral and somatosensory blockade of the abdominal wall [2]. There have been reports of excellent post-operative pain management with the QL block for both abdominal and retroperitoneal surgery [3,4] and a recent double-blinded RCT on the quadratus lumborum block for post-operative pain in caesarean section patients has shown promising results [5]. Børglum et al. [6] further refined the original Blanco block using a transmuscular approach defining the point of administration of the local anaesthetic to the fascial plane between the QL and Psoas Major (PM) muscles. Injection into this fascial plane posterior to the transversalis fascia, ensured a reliable spread into the thoracic paravertebral space and has been corroborated by MRI studies [6,7] that also showed that no redundant spread of the local anaesthetic occurred as could be seen with the original QL block. This transmuscular quadratus lumborum (TQL) block, has been suggested to be a simple and perhaps safer alternative to the anterior approach as was described for the original QL block [8].
A recent retrospective study of caesarean section-patients at our surgical centre assessed their postoperative need of opioids in addition to the standard postoperative analgesic regimen consisting of acetaminophen and ibuprofen. It was discovered that the average opioid amount needed for sufficient pain relief during the first forty-eight postoperative hours following a caesarean section equalled 43.5 ± 30.9 mg calculated in morphine equivalents (ranging from 0 to 175 mg). Even though it is part of the analgesic regime for these patients to receive 10 mg of oral morphine immediately upon arrival in the PACU (post-anaesthesia care unit), we found that > 80% of the patients required additional morphine during their stay in the maternity ward. This indicated a challenge of adequate pain management in this population of new mothers at a crucial point in their lives.
We hypothesized that the use of the bilateral USG TQL block as part of the postoperative multimodal analgesic regimen for caesarean section patients would exert an opioid sparing effect in this population.
We present three cases of planned repeat caesarean section, where two of our patients either had severe postoperative pain with their first delivery or had great troubles tolerating the opioid based pain management regime. All three patients gave verbal and written consent for the publication of their case stories.
Case Descriptions
Three pregnant women with no prior history of alcohol or opioid abuse were planned for repeat caesarean section at our obstetric surgical department. All three had previously had one caesarean section. It is not part of our multimodal analgesic regime to administer any analgesics prior to elective caesarean section. All three patients were anaesthetised with spinal anaesthesia according to local guidelines receiving 2 mL hyperbaric bupivacaine 0.5% supplemented with 2.5 mg sufentanil with a total intratechally administered volume of 2.5 mL. In all cases the surgical procedures were uneventful and without further analgesic requirement in the operating room.
Case 1
A 39-year-old woman was planned for caesarean section due to estimated high weight of the foetus. Post-operative pain management after her previous caesarean section had been without challenges. Following a standard and uncomplicated procedure the patient received the standard multimodal post-operative analgesic regime in the PACU consisting of 10 mg morphine, 1 g acetaminophen and 400 mg ibuprofen before the resolution of the spinal block. Ninety minutes later, with the return of sensory function, the patient experienced intense pain from the incisional wound estimated to 8/10 on the Numerical Rating Scale (NRS) 0-10 with no effect of an additional IV 5 mg of morphine. Feeling drowsy from the morphine the patient refrained from additional opioids and consented to a bilateral TQL-block.
The TQL block was performed by placing the patient in the lateral decubitus position, with the side to be anaesthetised facing up (Figure 1). The curved array transducer 6-2 MHz was placed in the midaxillary line in the transverse plane immediately cranial to the iliac spine where the muscular layers of the abdomen can be easily identified. Sliding the probe dorsally the abdominal wall muscles can be observed to attach to the posterior side of the QL muscle. At this point the Shamrock sign can also clearly be identified [9]. The QL is seen as a darker triangular shape attaching to the apex of the transverse process (TP) of L4, and constituting the superior leaf of the Shamrock, while the TP constitutes the stem and the PM and erector spinae muscles make up the anterior and posterior leaves (Figure 2). By using the in plane technique the needle is advanced from the posterior end of the probe, through the QL muscle, and the tip of the needle can be seen to enter the fascial plane between the QL and PM muscles. At this specific location 30 mL ropivacaine 0.375% was deposited bilaterally [10].
.
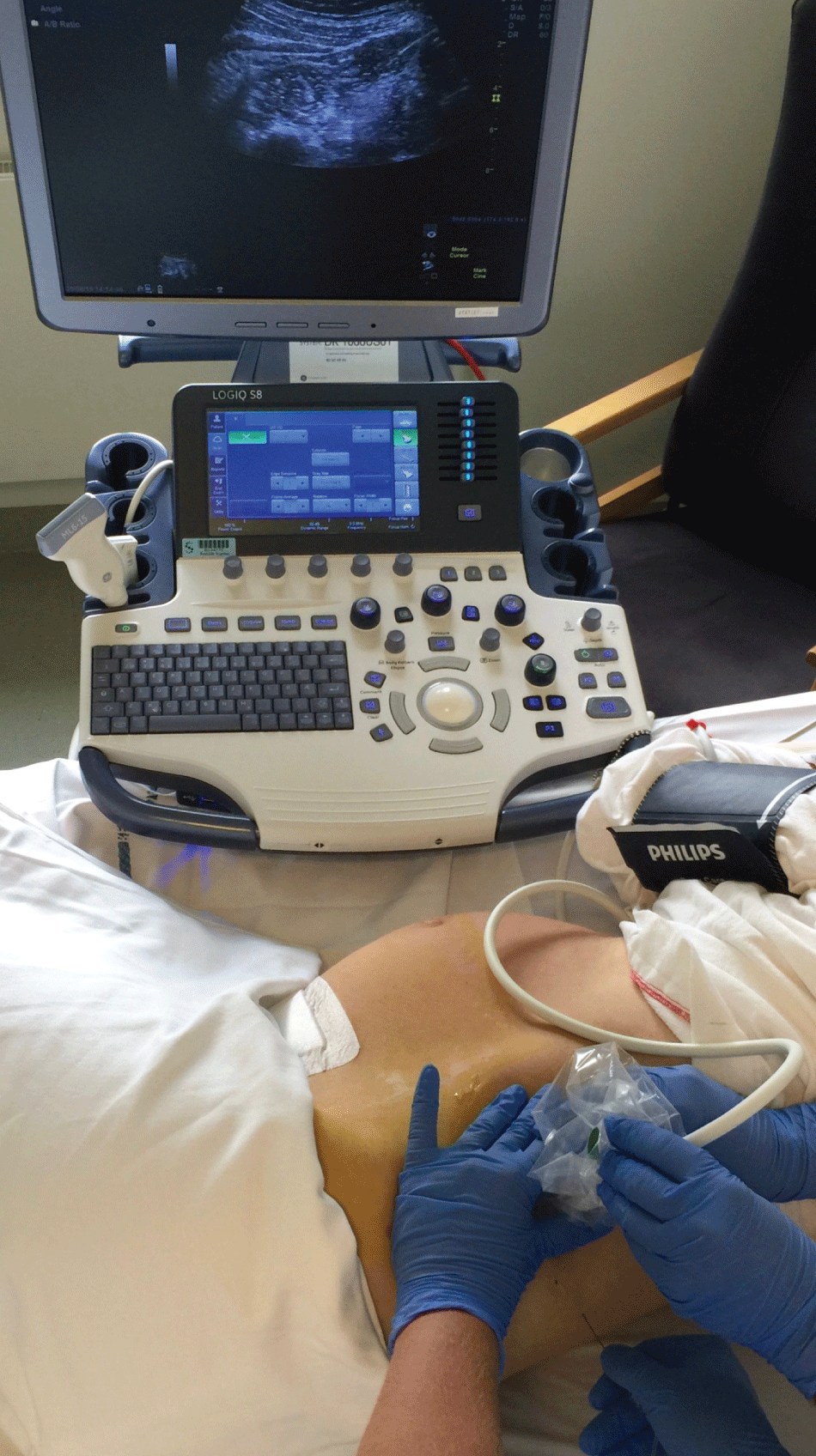
Figure 1: Patient positioning.
The patient is in the right lateral position and the transducer is positioned in the transverse position in the posterior axillary line above the iliac crest.
View Figure 1
.
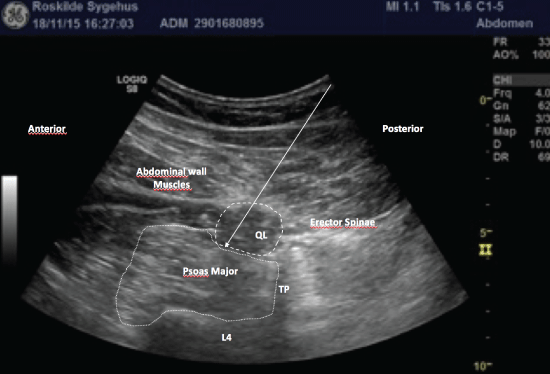
Figure 2: Shamrock sign.
The quadratus lumborum muscle (QL) is seen as a darker triangular shape attaching to the apex of the transverse process (TP) of L4. The three leaves of the Shamrock are composed of the QL, the psoas major and erector spinae muscles while the TP constitutes the stem.
View Figure 2
Cranial spread of the local anaesthesia was confirmed by the visualisation of the injectate advancing along the interfascial compartment and into the thoracic cage by turning the probe 90 degrees in the longitudinal plane (Figure 3).
.
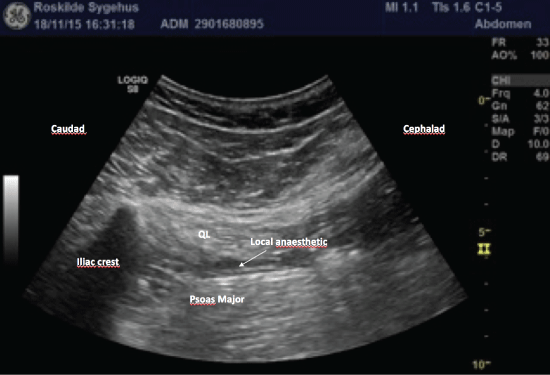
Figure 3: Confirming correct spread of the injectate.
After injection of the local anaesthetic the transducer is rotated 90 degrees in the longitudinal plane. The correct spread of local anaesthetic is confirmed by the clear visualization of injectate advancing along the interfascial compartment from the iliac crest (caudad) towards the diaphragm (cranial) separating the two muscles of quadratus lumborum (QL) and psoas major (PM).
View Figure 3
Within minutes the patient experienced complete pain relief and after ten minutes reported a NRS of 0/10. This patient had no need for additional analgesics for a post-block period of fourteen hours.
Case 2
A 33-year-old woman with a medical history of depression and anxiety was scheduled for her second caesarean section on maternal request. In the postoperative period of her last caesarean section, she experienced severe disability from the incisional pain to the extent of having difficulty sitting and walking despite the standard opioid regimen. Due to the prior difficulties with pain management in this patient, we planned the bilateral TQL block as a supplement to the standard analgesic regimen.
Upon arrival at the PACU she received the standard postoperative regimen consisting of 1 g acetaminophen and 400 mg ibuprofen intentionally omitting the 10 mg of perioral morphine. While the patient still had full effect of the spinal anaesthesia the TQL block was administered bilaterally. Although the motor function had not fully returned she was able to position herself in the lateral position with minimal assistance.
After full regression of the spinal anaesthesia the patient reported a NRS pain score of 0/10 and complete pain relief was experienced for twelve hours after the TQL block without the need for additional analgesia in this period.
Case 3
A 37-year-old fourth time parturient reported severe sedation, nausea and vomiting after pain management with morphine after her prior caesarean section. A wide range of different synthetic opioids had been tried, with the same debilitating side effects and unsatisfactory pain relief. Our aim in the post-operative management of this patient was to completely exclude the need for opioids. In order to accomplish this we hoped to a achieve a prolonged effect of the TQL block by adding dexamethasone to the LA, as perineural dexamethasone has been shown to provide a longer analgesic effect when used in certain types of blockades [11].
The patient arrived to the PACU with a full functioning spinal anaesthesia and without receiving any sort of analgesic we performed a bilateral TQL block with the addition of 4 mg of dexamethasone on each side.
After regression of the spinal anaesthesia the patient was discharged from the PACU with a NRS pain score of 0/10. Five hours after the block-administration the patient experienced a dull pain (NRS 3/10) from the incision when she first got out of bed. Administration of 1 g acetaminophen and 400 mg ibuprofen provided complete pain relief. Similar symptoms returned seventeen hours after block-administration and 1 g acetaminophen was sufficient to the return of a NRS pain score of 0/10. The patient required no additional pain medication during her hospital admission.
Discussion
Our first case is an example of how the TQL block is used successfully as rescue analgesia after the failure of conventional analgesics.
The second and third case demonstrates both the use of the TQL block as an effective tool of pre-emptive analgesia as well as its opioid-sparing effect. In our last case we present the unique example of a caesarean section-patient having managed without opioids as a result of a timely administered TQL block.
Alternative regional anaesthetic solutions to the TQL block comprise of the transversus abdominis plane (TAP) block, the epidural and the thoracic paravertebral block (TPVB). The bilateral dual-TAP block (a four point injection technique) will anaesthetize the dermatomes Th6-Th12, the anteromedial muscles of the abdominal wall and the underlying parietal peritoneum, but fails to provide visceral pain relief [7] as opposed to the epidural and the TPVB. However the epidural is an invasive and labour-intensive solution with many known adverse effects [12] and both the epidural and the TPVB block present risks of vascular puncture, pneumothorax and excessive sympathetic blockade. Management of the patient after TQL block only requires thirty minutes of post-block monitoring for signs of systemic toxicity [13], which is easily managed in the PACU. No additional training of the maternity ward staff is warranted.
The pain audit at our institution indicated an unsuspected high degree of morphine consumption in this population of new mothers. At a time where the main focus should be on the infant with the initiation of breastfeeding and early bonding, the rather frequent adverse side effects of morphine including nausea, drowsiness, vomiting and dizziness are especially undesirable. Moreover breastfeeding is not recommended at times when the mother is experiencing morphine induced drowsiness [14].
The use of the USG bilateral TQL block as part of multimodal analgesic regimen will have an opioid-sparing effect especially when provided in the early postoperative period, preferably before the resolution of the spinal anaesthesia.
Acknowledgement
None.
References
-
Blanco R (2007) Tap block under ultrasound guidance: the description of a "no pops" technique. Reg Anesth Pain Med 32: 130.
-
Carney J, Finnerty O, Rauf J, Bergin D, Laffey JG, et al. (2011) Studies on the spread of local anaesthetic solution in transversus abdominis plane blocks. Anaesthesia 66: 1023-1030.
-
Chakraborty A, Goswami J, Patro V (2015) Ultrasound-Guided Continuous Quadratus Lumborum Block for Postoperative Analgesia in a Pediatric Patient. A A Case Rep 4: 34-36.
-
Visoiu M, Yakovleva N (2013) Continuous postoperative analgesia via quadratus lumborum block - An alternative to transversus abdominis plane block. Paediatr Anaesth 23: 959-961.
-
Blanco R, Ansari T, Girgis E (2015) Quadratus lumborum block for postoperative pain after caesarean section: A randomised controlled trial. Eur J Anaesthesiol 32: 812-818.
-
Børglum J, Moriggl B, Jensen K, Lönnqvist PA, Christensen AF, et al. (2013) Ultrasound-guided Transmuscular Quadratus Lumborum Blockade. Br J Anaesth.
-
Børglum J, Christensen A, Hoegberg L (2012) 74. Bilateral-dual transversus abdominis plane (BD-TAP) block or thorasic paravertebral block (TPVB)? Distribution patterns, dermatomal anaesthesia and LA pharmacokinetics. Reg Anesth Pain Med 37.
-
Hansen CK, Dam M, Bendtsen TF, Børglum J (2016) Ultrasound-Guided Quadratus Lumborum Blocks: Definition of the Clinical Relevant Endpoint of Injection and the Safest Approach. A A case Rep 15: 39.
-
Sauter AR, Ullensvang K, Niemi G, Lorentzen HT, Bendtsen TF, et al. (2015) The Shamrock lumbar plexus block. A dose-finding study. Eur J Anaesthesiol 32: 764-770.
-
10. Rosenberg PH, Veering BT, Urmey WF (2004) Maximum recommended doses of local anesthetics: A multifactorial concept. Reg Anesth Pain Med 29: 564-575.
-
De Oliveira GS, Alves LJC, Nader A, Kendall MC, Rahangdale R, et al. (2014) Perineural Dexamethasone to Improve Postoperative Analgesia with Peripheral Nerve Blocks: A Meta-Analysis of Randomized Controlled Trials. Pain Res Treat.
-
Rawal N (2012) Epidural technique for postoperative pain: gold standard no more? Reg Anesth Pain Med 37: 310-317.
-
Neal JM, Bernards CM, Butterworth JF, Di Gregorio G, Drasner K, et al. (2010) ASRA practice advisory on local anesthetic systemic toxicity. Reg Anesth Pain Med 35: 152-161.
-
Felsby S, Bækby Houborg K, Lefort Sønderskov M, Bang U (2015) DASAIM: Rekommendation Vedrørende Anæstesi Og Amning.





