International Journal of Anesthetics and Anesthesiology
Integrated Pulmonary Index: A New Strategy for Respiratory Patients Evaluation
Guldem Turan*, Yildiz Kuplay, Ceren Karip, Ceren Koksal, Cansu Akin and Nur Akgun
Fatih Sultan Mehmet Teaching and Research Hospital, Intensive Care Unit, Turkey
*Corresponding author: Guldem Turan, Fatih Sultan Mehmet Teaching and Research Hospital, Intensive Care Unit, Turkey, Tel: 9002165783030-5502, Fax: + 9002163360565, E-mail: gturanmd@yahoo.com
Int J Anesthetic Anesthesiol, IJAA-3-042, (Volume 3, Issue 1), Original Article; ISSN: 2377-4630
Received: December 27, 2015 | Accepted: February 10, 2016 | Published: February 13, 2016
Citation: Turan G, Kuplay Y, Karip C, Koksal C, Akin C, et al. (2016) Integrated Pulmonary Index: A New Strategy for Respiratory Patients Evaluation. Int J Anesthetic Anesthesiol 3:042. 10.23937/2377-4630/3/1/1042
Copyright: © 2016 Turan G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Purpose: We presented a study of the importance of integrated pulmonary index (IPI) correlated with arterial blood gas analysis in the respiratory management of the patient (surgical or internal medicine) recovering in intensive care unit.
Methods: The IPI incorporated four real-time respiratory measurements; oxygen saturation (SpO2), the level of carbon dioxide at the end of expiration (ETCO2), respiratory rate (RR), pulse rate (PR). We measured continuosly IPI with repeated arterial blood gas analysis and clinical observations in 100 patients from May/2015 to August/2015 recovered in our intensive care unit. Correlation between measurements was analysed statistically. We analyzed data with SPSS program.
Results: We observed 47 patients in mechanical ventilation support (orotracheal intubation), 8 patients in non invasive ventilation support (NIMV) and 45 patients with venturi mask ventilation. There found to be a correlation between IPI (7.68 ± 1.92) and SpO2 (96.85 ± 3.58), RR (18.96 ± 7.18). Correlations were identified between SpO2 of IPI monitor and arterial blood gas Sat measurements, and between EtCO2 (34,27,66) value and arterial blood gas PaCO2 (38.04 ± 8.07) measurements.
Conclusions: IPI correlates arterial blood gas values and provides a single numerical value for early identification of respiratory failure in intensive care. IPI ensures ease of use by displaying multiple parameters on a single screen and being a bed-side, non-invasive method. Even, it might be a potential candidate to be a more dynamic measurement than arterial blood gas.
Keywords
Integrated Pulmonary Index, Endtidal Carbondioxide, Respiratory Failure, Mechanical Ventilation, Intensive Care Unit
Introduction
There are different monitorisation methods for following patients in intensive care units. Monitorisation of respiratory parameters is also important besides monitorisation of hemodynamic parameters [1,2]. Integrated pulmonary index (IPI) algorithm incorporates four real-time respiratory measurements (end-tidal CO2, respiratory rate, pulse rate and SpO2) into a single value that represents respiratory profile including these parameters. IPI gives an idea to the clinician to determine the need for additional clinical assessment or intervention by assessing respiratory status of the patient quickly [3].
In our study, consistency of IPI use with clinical findings and correlation of IPI with arterial blood gas were evaluated in patients being treated in intensive care unit under invasive, non-invasive mechanical ventilation or followed in spontaneous ventilation.
Materials and Methods
Fatih Sultan Mehmet Hospital Ethics Committee approved the study (FSM EAH KAEK No: 2015/60) and 100 patients whose families had given consent were enrolled in the study. Patients with nasal packing due to any anatomic reason and/or trauma were excluded. APACHE II score of each patient treated in our intensive care unit was recorded. Besides standard monitorisation, follow-up of respiratory parameters with IPI monitor was initiated. IPI monitorisation was performed by collecting expired air sampling with nasal probe in patients with spontaneous ventilation, with an apparatus placed between endotracheal tube and ventilator circuit in intubated patients and with an apparatus placed between mask and ventilator circuit in non-invasive ventilation. And, SpO2 and peripheral pulse count was monitorised through peripheral finger probe of IPI monitor. IPI score is between 1 and 10 [3] (Table 1) .
![]()
Table 1: IPI score is between 1 and 10.
View Table 1
In minute 30 following monitorisation practice, arterial blood gas analysis were conducted and IPI, end-tidal CO2, respiratory rate, peripheral oxygen saturation, peripheral pulse rate, arterial blood gas parameters and patient's clinical status were recorded.
While clinical status of the patient was recorded the following were evaluated as stable:
IMV: In intubated mechanical ventilation
NIV: In noninvasive ventilation
MV: Mask ventilation in spontaneous ventilation
IPI's correlation with ETCO2, SPO2, respiratory rate (RR), peripheral pulse rate (PR), arterial blood gas parameters (pH, PO2, PCO2) and IPI means by clinical status were analysed statistically.
Statistical Analysis
For assessing the data obtained in the study, (IBM SPSS) program was used in statistical analysis. Compliance of parameters with normal distribution was assessed by using Shapiro Wilks test in the analysis of the study data. Besides descriptive statistical methods (Mean, Standard deviation, frequency), Kruskal Wallis test was used in comparisons of quantitative data. For investigating relationships between parameters that were in compliance with normal distribution, Pearson correlation analysis was used. For determining compliance between two methods, Bland Altman test was used. Significance was evaluated on the level of p < 0.05.
Results
In the study, totally 100 patients were enrolled providing that 50 patients were female and 50 patients were male. Demographic characteristics of patients and mean values of IPI (7.68 ± 1.92), SPO2, (96.85 ± 3.58), ETCO2 (34,27,66), RR (18.96 ± 7.18), PR (93.42 ± 20.21), blood gas parameters that pH (7.41 ± 0.09), PaCO2 (38.04 ± 8,07), PaO2 (104.09 ± 31.41) and Sat (97.88 ± 2.76) are shown in Table 2.
![]()
Table 2: Demographic Parameters and Mean Values.
View Table 2
While IPI was found to be correlated with SPO2 and RR, it did not correlate with ETCO2 and PR. (Table 3). Mean IPIs by clinical status are shown in Table 4.
![]()
Table 3: IPI correlation with SPO2, ETCO2, RR and PR.
View Table 3
![]()
Table 4: Assessment of the IPI according to clinical status.
View Table 4
Correlations between IPI monitor SPO2 and arterial blood gas Sat and between IPI ETCO2 and arterial blood gas PaCO2 were demonstrated (Graph 1 and Graph 2).
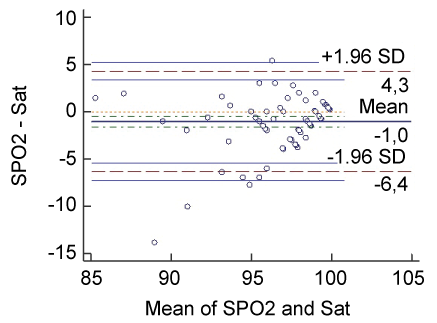
.
Graph 1: Correlation between IPI monitor SPO2 and arterial blood gas Sat (Bland Altman).
View Graph 1
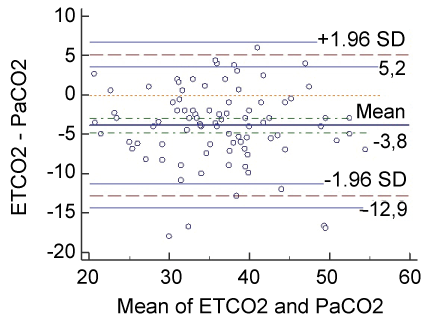
.
Graph 2: Correlation between IPI ETCO2 and arterial blood gas PaCO2 (Bland Altman).
View Graph 2
Discussion
IPI is a new respiratory index that is specific and more accurate then other single respiratory values. According to Resperato et al. [4] correlation between IPI and blood gas values in intensive care unit was investigated. In this study, 21 patients under the support of mechanical ventilation were enrolled. Respiratory status that reflected in arterial blood gas was found to be correlated with IPI. It was demonstrated that there was a moderately inversely proportional correlation between PaCO2 and IPI while there was a directly proportional correlation between SpO2 and IPI; these correlations were statistically significant. Thus, they reported that IPI was a potential candidate for evaluating respiratory status for it was a more dynamic, concurrent measurement than arterial blood gas.
In the study of Garah et al. [5] it was aimed to study the value of IPI monitorisation during pediatric endoscopic procedures. They randomised patients into 3 groups. Five patients were included in Group 1 which used only propofol, 89 patients were included in Group 2 which used propofol and midazolam, and 15 patients were included in Group 3 which used propofol, midazolam and fentanil. IPI values in Group 2 and Group 3 were found to be significantly higher than the values in Group 1. When compared to 7-12 age groups, IPI values were found to be significantly lower than the values in 4-6 age groups. While IPI was alarming in all apnoea and hypoxia episodes, pulse oxymetry could identify only hypoxia episodes.
In the study of Berkenstadt et al. [6] prospective comparison of respiratory pattern to IPI in patients who underwent colonoscopy in sedation was aimed. In low (1-3), moderate (4-6), high (7-10) IPI groups, there found to be no difference with respect to respiratory rate (RR), SpO2, pulse rate (PR), but EtCO2 value was found to be higher in high IPI group. These results are similar to our study's results and it was demonstrated that there was a correlation between IPI and SpO2 and respiratory rate.
Kumar et al. [7] have two different studies of IPI. They followed mean IPI value of 24 obese patients who were under spontaneous ventilation trials. Results of each spontaneous ventilation trial were determined independently by the intensive care team. Records were analysed in order to determine the efficacy of IPI for estimating the results of weaning assessment. Statistical analysis demonstrated that IPI values were higher in successful spontaneous ventilation trials than IPI values in unsuccessful spontaneous ventilation trials. In another study of the same investigators, 43 patients with intubation due to surgical or medical indications and followed in intensive care unit were included in the study. Also in this study, results demonstrated that IPI values were higher in successful spontaneous ventilation trials than IPI values in unsuccessful spontaneous ventilation trials. Sabattani et al. [8] demonstrated that IPI index differed significantly ETCO2 under sedation in 45 patients who went under external cardioversion. It was reported that IPI alone had advantage compared to ETCO2 monitorisation.
Schier et al. [9] in their study stated that IPI was a clinically useful monitorisation. They mentioned that there was a need to conduct further studies in order to determine if IPI was more sensitive to patient factors (tremors in the patient, etc.) than monitors with repeated false alarm which were used commonly in the ward. In our study, we did not experience a problem related to the impact f tremors in IPI monitor. However, in patient whose peripheral temperature was low, we experienced a problem such that the finger probe did not detect data and the data could be obtained after external heating.
In a study conducted by Kuzkov et al. [10] it was aimed to investigate the value of IPI after coronary artery bypass grafting. Twenty-three adult patients who went under elective coronary artery bypass grafting were enrolled in the study. Patients were grouped according to their postoperative IPI values: optimal IPI (IPI > 8, n = 11) and suboptimal (IPI ≤ 8), n = 12). Patients who were smoking were observed to be prone to have low IPI scores after 12 hours of operation. They reported their opinion suggesting that IPI might be a valuable contributor in postoperative monitorisation by facilitating early detection of respiratory problems.
In another study by Kuzkov et al. [11] it was aimed to investigate the role of IPI in the weaning phase after off-pump coronary artery bypass grafting. Seventy-two adults patients were randomised to four groups following elective off-pump coronary artery bypass grafting. Different postoperative ventilation approaches were applied to three groups: CPAP 40 cm H2O for 40 seconds in Group 1, PEEP 15 cm H2O for 5 minutes in Group 2 and increased tidal volume for 40 seconds in order to ensure peak pressure be 40 cm H2O in group 3. When compared to the control group, mechanical ventilation time following off-pump coronary artery bypass grafting was found to be shorter in PEEP 15 cm H2O manoeuvre group (Group 2). They suggested that IPI could estimate postoperative mechanical ventilation and that it might be a valuable contributor in off-pump monitorisation.
As a result of our study, it was observed that IPI statistically significantly correlated with SPO2 and RR, and had a clinical compatibility with ETCO2 and PR. In addition, there found to be a correlation between IPI monitor SPO2 value and arterial blood gas Sat along with IPI monitor ETCO2 value and arterial blood gas PaCO2 measurements. In the light of these results, it may be suggested that IPI monitor which is a continuous and noninvasive measurement method can be opted for arterial blood gas which is an invasive method in monitorising intensive care unit patients.
Conclusion
IPI correlates with arterial blood gas measurements, thus it provides a single numerical value that ensures early detection of respiratory failure in intensive care unit. Features of IPI monitor such as having bedside usage, being a non-invasive method and showing multiple parameters on the same screen makes it easy to use. Even, it may stands for being a more dynamic measurement than arterial blood gas in monitorising patients treated in intensive care units. Particularly, it has been observed that IPI may be an important additional parameter in the monitorisation of critical patients who are in spontaneous ventilation but may require mechanical ventilation and in guiding the physician while making decision about mechanical ventilation indication.
References
-
Arora S, Singh PM, Goudra BG, Sinha AC (2014) Changing trends of hemodynamic monitoring in ICU - from invasive to non-invasive methods: Are we there yet? Int J Crit Illn Inj Sci 4: 168-177.
-
Smallheer BA (2015) Technology and monitoring patients at the bedside. Nurs Clin North Am 50: 257-268.
-
Gozal, D, Gozal, Y (2009) The Integrated Pulmonary Index: Validity, Safety and Application in the Pediatric Population. Proceedings of the 2009 Annual Meeting of the American Society Anesthesiologists A.390.
-
Restrepo RD, Otaibi AA, Wittnebel L, Shammari YA, Ismaeil T (2013) Correlation between ABG parameters and the integrated pulmonary index in a medical-surgical ICU in saudi arabia. Anesthesia and Analgesia 117 (4S Suppl): 54-55.
-
Garah J, Adiv OE, Rosen I, Shaoul R (2015) The value of Integrated Pulmonary Index (IPI) monitoring during endoscopies in children. J Clin Monit Comput 29: 773-778.
-
Berkenstadt H, Ben-Menachem E, Herman A, Dach R (2012) An evaluation of the Integrated Pulmonary Index (IPI) for the detection of respiratory events in sedated patients undergoing colonoscopy. J Clin Monit Comput 26: 177-181.
-
Kumar V, Taft A, Johnson S, Herrington R, Castresana M (2013) Progressive Evaluation of Integrated Pulmonary Index (IPI) During Spontaneous Breathing Trials in Medical and Surgical Patients. Proceedings of the 2013 Annual Meeting of the American Society of Anesthesiologists A 4237.
-
Sabbatani P, Mantovan R (2013) Electrical cardioversion of atrial fibrillation: evaluation of sedation safety with midazolam by means of EtCOâ‚‚ and IPI algorithm analysis. Int J Cardiol 169: 430-432.
-
van der Schier R, Roozekrans M, van Velzen M, Dahan A, Niesters M (2014) Opioid-induced respiratory depression: reversal by non-opioid drugs. F1000Prime Rep 6: 79.
-
Kuzkov VV, Gaidukov KM, Fot EV, Neverova MS, Smetkin AA, et al. (2011) Integrated pulmonary index reflects respiratory function after elective coronary artery bypass grafting: 5AP4-5. European Journal of Anaesthesiology 28 : 78.
-
Kuzkov V, Fot E, Gaidukov K, Neverova M, Kirov M (2012) Integrated pulmonary index (IPI) is associated with duration of postoperative respiratory support after coronary artery bypass grafting and body mass index: 5AP4-6. European Journal of Anaesthesiology 29: 90.





