International Journal of Anesthetics and Anesthesiology
The Effect of Perioperative Restrictive Fluid Therapy on Postoperative Edema and Ecchymosis in Rhinoplasty
Erden V1, Sever E2, Dağdelen Ş1, Güler C1*, Kirgezen T1, Toprak N1 and Yiğit Ö2
1Anesthesiology and Reanimation Department, İstanbul Research and Education Hospital, Turkey
2Otorhinolaryngology Department, İstanbul Research and Education Hospital, Turkey
*Corresponding author: Güler C, Anesthesiology and Reanimation Department İstanbul Research and Education Hospital, Turkey, KasapIlyas district Org. Abdurrahman Nafiz Gurman Street Postal code: 34098 Fatih/Istanbul Turkey, Tel: +902124596160, E-mail: cianguler@gmail.com
Int J Anesthetic Anesthesiol, IJAA-2-038, (Volume 2, Issue 4), Original Research; ISSN: 2377-4630
Received: September 15, 2015 | Accepted: December 19, 2015 | Published: December 22, 2015
Citation: Erden V, Sever E, Dağ delen Ş, Güler C, Kirgezen T, et al. (2015) The Effect of Perioperative Restrictive Fluid Therapy on Postoperative Edema and Ecchymosis in Rhinoplasty. Int J Anesthetic Anesthesiol 2:038. 10.23937/2377-4630/2/4/1038
Copyright: © 2015 Erden V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Objective: The aim of our study is perioperative restrictive fluid administration in rhinoplasty whether contribute to decreased postoperative edema and ecchymosis.
Background: Prolonged periorbital ecchymosis and severe edema may cause a delay in healing and affect the result of surgery and influence the satisfaction of patient and surgeon.
Methods: The study designed as a prospective, blinded, randomised study. Fifty patients, ASA physical status 1 aged 18-46 years planning to undergo rhinoplasty as an elective surgery were randomly divided into two groups; standard fluid administration ( group S) and restrictive fluid administration (group R). Operation time, mean arterial pressure and total fluid volume were recorded.
Results: Periorbital ecchymosis was significantly decreased in the group R at 4 hours postoperatively. When comparing between two groups' ecchymosis scores were no statistically significant difference at 24 hours and 7 days postoperatively.
Conclusion: Postoperative edema and ecchymosis are the main morbidities which were not affected from perioperative restrictive fluid regimen in patients undergoing rhinoplasty.
Keywords
Fluid Regimen, Rhinoplasty, Edema, Ecchymosis
Introduction
Postoperative edema and ecchymosis can usually occur after rhinoplasty and can cause disgruntled results which influence the satisfaction of patient and surgeon. Prolonged periorbital ecchymosis and severe edema may cause a delay in healing and affect the result of surgery. Many of agents have been used to reduce the influence of edema and ecchymosis developing around the eyes after rhinoplasty, such as corticosteroids, lidocaine and adrenaline combination, melilotus extract [1-5].
The physiological stress due to surgery induced inflammation, catabolism and fluid retention initiated by inflammatory factors that increasing around the surgical area. Vascular permeability is affected by the increasing size of the surgical area, inducing distribution of fluid between intravascular and interstitial space. Together with that the perioperative patient has a tendency for fluid retention, since administered fluids are not readily excreted, which may cause to postoperative fluid overload and accumulation of fluid in peripheral tissues.
There is no information on the impact perioperative fluid management on postoperative edema and ecchymosis following rhinoplasty surgery. Therefore we studied that a perioperative restrictive fluid regimen seen in rhinoplasty whether contribute to decreased postoperative edema and ecchymosis.
Methods
After institutional review board approval and informed consent 50 patients, ASA physical status 1 aged 18-46 years planning to undergo rhinoplasty as an elective surgery were enrolled in this study. Patients having coagulation disorder, morbid obesity and corticosteroid usage were excluded.
The subjects were randomly divided into two groups; standard fluid administration (group S, n: 25) and restrictive fluid administration (group R, n: 25). No pre-anaesthetic administration was performed on the day of the operation. After arriving at the operation room, peripheral venous access was established and standard monitorization was performed using electrocardiogram, pulse oximetry and non-invasive blood pressure monitoring. In all groups anesthesia was induced with propofol 2 mg/kg and muscle relaxation with rocuronium 0.5 mg/kg. The remifentanil was given to all groups intravenously as a bolus 0.5 mcg/kg-1 min-1 (minimum 30 seconds) before induction of anaesthesia and 0.5-1 mcg/kg-1 min-1 continuous intravenous infusion during the operation. Anaesthesia was maintained with sevoflurane and 50% nitrous oxide in oxygen both two groups. Standard fluid regimen in group S shown in table 1. Restrictive fluid regime in group R; administration of crystalloid fluid ( 0.9 % NaCI) 4 ml per kg per hour for the first 10 kg, 2 ml per kg per hour for the second 10 kg and 1 ml per hour for each additional kilogram body weight. Fluid administration was stopped at the end of the surgery in both groups.
![]()
Table 1: Fluid Management
View Table 1
All patients with similar nasal deformities, skin types were choose and were operated with external approach by same surgical team. All patients underwent septoplasty, dorsal hump resection, nasal tip reshaping and median-oblique and lateral osteotomies with 2 to 3 millimetres endonasal micro osteotomy applied. A local anaesthetic infiltration of 2% lidocaine and 1:100.000 adrenaline was administered 15 minutes before surgery. Postoperatively, nasal pacing was applied for 24 hours for all patients. A nasal splint (Rhino fix, Istanbul, Turkey) was left over the nasal dorsum for 1 week. All patients were hospitalized for 24 hours after surgery and they were called for a control examination on postoperative day 7. Degree of eyelid edema was recorded at 4 and 24 hours and on postoperative day 7 by 2 investigators who were blinded which fluid regime was administered. In each patient, edema and ecchymosis extended from medial to lateral and from inferior to superior. Severity of edema was rated in terms of the degree of closure of eyelids on a scale of 0 to 4 [6]. (Table 2) The extension of upper and lower eyelid ecchymosis was evaluated separately using a scale of 0 to 5 [4]. (Table 2) We used for post-operative analgesia diclofenac sodium 75 mg tablets. Operation time, mean arterial pressure and total fluid volume were recorded.
![]()
Table 2: Scoring system for parameters
View Table 2
Statistics
Data analysis was performed using SPSS v.16.0 software. The student T-test used to analyse the demographic data and mean arterial pressure between groups. Mann-Whitney U test was used to compare for ecchymosis and edema between groups. P value of less than 0.05 was considered as statistically significant.
Result
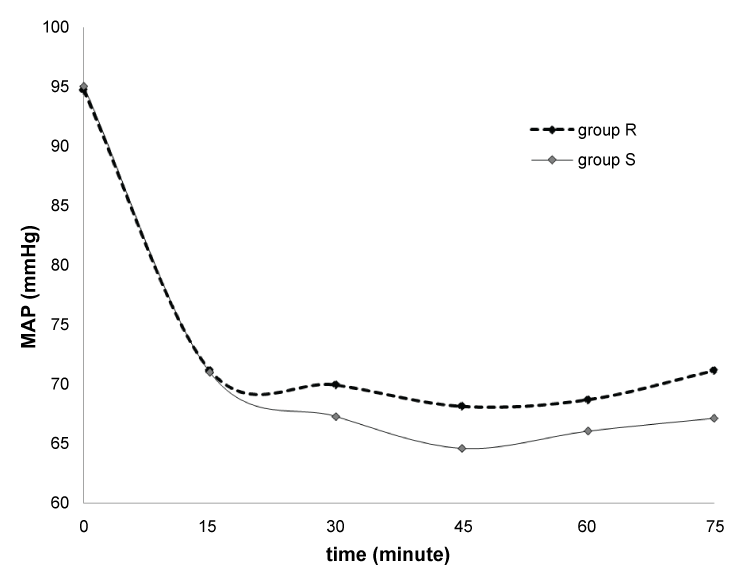
The demographic data, duration of anesthesia and total fluid volume were given in table 3. No significant differences were found in age, body mass index or duration of anesthesia between two groups. Mean arterial pressure values were shown at Graphic 1. No statistically difference was observed at minutes 0, 15, 30, 45, 60 and 75 between groups .(P: respectively 0.97, 0.45, 0.31, 0.14, 0.13, 0.11) When comparing between two groups edema scores were no statistically significant difference at 4, 24 hours and 7 days postoperatively.
![]()
Table 3: Scoring system for parameters
View Table 3
(P: respectively 0.06, 0.14, 1.0) (Table 4) Periorbital ecchymosis was significantly decreased in the group R at 4 hours postoperatively. (P = 0.039) When comparing between two groups ecchymosis scores were no statistically significant difference at 24 hours and 7 days postoperatively (P: respectively 0.11, 0.21) (Table 5)
![]()
Table 4: Eyelid Edema Scores
View Table 4
![]()
Table 5: Eyelid Edema Scores
View Table 5
Discussion
We performed a prospective study of fluid management regimen, postoperative evaluation of ecchymosis and edema in patients undergoing rhinoplasty. We found that restrictive fluid intervention decreased the 4 hours post-operative period ecchymosis. First and seventh day postoperative scores of ecchymosis and edema degrees was not affected by restrictive and standard fluid regimens.
Perioperative fluid intervention has been a matter of debate and still continues today. Conventional practice large crystalloid volumes were given to all patients perioperatively. This was based on the perioperative patient was hypovolemia due to prolonged fasting and insensible fluid loss during the surgical exposure. In addition; hypotension during general and neuraxial anaesthesia often covered by liberal intravenous fluid administration. On the other hand there is no association between anaesthesia related hypotension and fluid loading [7,8]. Anaesthesia related hypotension should more properly be treated with vasopressor therapy [9].
Perioperative fluid loading seem to have important side effects in several organ systems such as the cardiovascular system, the possibility of developing myocardial ischemia due to the potential impairment of left ventricular stroke volume [10]. Pulmonary system may be impaired by accumulation of interstitial fluid, which may cause pulmonary edema, atelectasis and respiratory failure [10]. The occurring decreased tissue oxygenation may contribute to impaired wound healing [10]. Studies has shown that in patients undergoing major abdominal surgery, fluid restrictive regimen during perioperative period have several benefits such as shorter length of hospital stay and reduced post-operative complications [11-14]. However, the others found no change for complication rate post-operatively [15-17]. In our study we found that restrictive fluid regimen has no effect on edema and ecchymosis postoperatively. One study showed that infusion rates of between 2 and 18.5 ml kg-1 h-1 surgery of duration < 3 hours did not cause significant interstitial edema [18]. In elective major surgery indicate that administration of > 5 litres fluid (primarily crystalloid) without specific indication may increase morbidity [19]. In 12 healthy volunteers, mimicking the perioperative set-up for laparoscopic cholecystectomy, but without surgery being performed, where infusion of 40 ml kg-1 (~ 3 litres) ringer lactate over 3 hours led to decrease pulmonary function and in addition a significant weight gain lasting 24 hours [20]. In our study patients undergoing rhinoplasty which is minor surgery so perioperative fluid shifts are small and organ dysfunctions minor. In standard fluid administration group was given nearly 1400 ml crystalloid fluid and mean operation duration was about 2 hours. Therefore in standard group given total fluid volume was less than 3 litres and duration of operation was less than 3 hours may not cause to increase edema and ecchymosis.
Several factors are related to eyelid edema and ecchymosis such as osteotomy technique, skin type, perioperative blood pressure and corticosteroid usage. Many trials have focused on the effect of osteotomy techniques on edema and ecchymosis in patients undergoing rhinoplasty operation. They found conflicting results. One of them reported external osteotomy is better on the other a study showed that there was no difference between internal and external approach [21-23]. Therefore we performed similar osteotomy techniques in all patients. Controlled hypotension is usually used to reduce bleeding and established more proper operative field especially for head and neck surgery [24]. Controlled hypotension in rhinoplasty reduce edema and ecchymosis postoperatively [25,26]. In our study mean arterial pressure was maintained between 65-75 mmHg with remifentanyl infusion for controlled hypotension.
Conclusion
There is some benefit in perioperative fluid restriction with related to reduce morbidity in major surgery. However; in our study we found that ecchymosis and edema degrees was not affected by restrictive and standard fluid regimens except the decreased 4 hours post-operative period ecchymosis in restrictive group. These findings, specific to patients undergoing rhinoplasty, are the main comorbidities such as postoperative edema and ecchymosis were not affected from perioperative restrictive fluid regimen.
References
-
Youssef TA, Elibiary H, Amish KF (2013) Role of steroids in reducing postoperative edema in rhinoplasty: a meta-analytic study. Eur Arch Otorhinolaryngol 270: 1189-1193.
-
Gurlek A, Fariz A, Aydogan H, Ersoz-Ozturk A, Eren AT (2006) Effects of different corticosteroids on edema and ecchymosis in open rhinoplasty. Aesthetic Plast Surg 30: 150-154.
-
Gürlek A, Fariz A, Aydoğ an H, Ersöz-Oztürk A, Evans GR (2009) Effects of high dose corticosteroids in open rhinoplasty. J Plast Reconstr Aesthet Surg 62: 650-655.
-
Totonchi A, Guyuron B (2007) A randomized, controlled comparison between arnica and steroids in the management of postrhinoplasty ecchymosis and edema. Plast Reconstr Surg 120: 271-274.
-
Xu F, Zeng W, Mao X, Fan GK. (2008) The efficacy of melilotus extract in the management of postoperative ecchymosis and edema after simultaneous rhinoplasty and blepharoplasty. Aesthetic Plast Surg 32: 599-603.
-
Hoffmann DF, Cook TA, Quatela VC, Wang TD, Brownrigg PJ, et al. (1991) Steroids and rhinoplasty. A double-blind study. Arch Otolaryngol Head Neck Surg 117: 990-993.
-
Jackson R, Reid JA, Thorburn J (1995) Volume preloading is not essential to prevent spinal-induced hypotension at caesarean section. Br J Anaesth 75: 262-265.
-
Norberg A, Hahn RG, Li H, Olsson J, Prough DS, et al. (2007) Population volume kinetics predicts retention of 0.9% saline infused in awake and isoflurane-anesthetized volunteers. Anesthesiology 107: 24-32.
-
Jacob M, Chappell D, Conzen P, Finsterer U, Rehm M (2008) Blood volume is normal after pre-operative overnight fasting. Acta Anaesthesiol Scand 52: 522-529.
-
Holte K, Sharrock NE, Kehlet H (2002) Pathophysiology and clinical implications of perioperative fluid excess. Br J Anaesth 89: 622-632.
-
Weinberg L, Wong D, Karalapillai D, Pearce B2, Tan CO4, et al. (2014) The impact of fluid intervention on complications and length of hospital stay after pancreaticoduodenectomy (Whipple's procedure). BMC Anesthesiol 14: 35.
-
Brandstrup B, Tønnesen H, Beier-Holgersen R, Hjortsø E, Ørding H, et al. (2003) Effects of intravenous fluid restriction on postoperative complications: comparison of two perioperative fluid regimens: a randomized assessor-blinded multicenter trial. Ann Surg 238: 641-648.
-
Futier E, Constantin JM, Petit A, Chanques G, Kwiatkowski F, et al. (2010) Conservative vs restrictive individualized goal-directed fluid replacement strategy in major abdominal surgery: A prospective randomized trial. Arch Surg 145: 1193-1200.
-
Nisanevich V, Felsenstein I, Almogy G, Weissman C, Einav S, et al. (2005) Effect of intraoperative fluid management on outcome after intraabdominal surgery. Anesthesiology 103: 25-32.
-
Kabon B, Akça O, Taguchi A, Nagele A, Jebadurai R, et al. (2005) Supplemental intravenous crystalloid administration does not reduce the risk of surgical wound infection. AnesthAnalg 101: 1546-1553.
-
Brandstrup B, Svendsen PE, Rasmussen M, Belhage B, Rodt SÅ, et al. (2012) Which goal for fluid therapy during colorectal surgery is followed by the best outcome: near-maximal stroke volume or zero fluid balance?. Br J Anaesth 109: 191-199.
-
Tambyraja AL, Sengupta F, MacGregor AB, Bartolo DC, Fearon KC (2004) Patterns and clinical outcomes associated with routine intravenous sodium and fluid administration after colorectal resection. World J Surg 28: 1046-1051.
-
Tatara T, Nagao Y, Tashiro C (2009) The effect of duration of surgery on fluid balance during abdominal surgery: a mathematical model. Anesth Analg 109: 211-216.
-
Holte K (2010) Pathophysiology and clinical implications of peroperative fluid management in elective surgery. Dan Med Bull 57: B4156.
-
Holte K, Jensen P, Kehlet H (2003) Physiologic effects of intravenous fluid administration in healthy volunteers. Anesth Analg 96: 1504-1509, table of contents.
-
Yücel OT (2005) Which type of osteotomy for edema and ecchymosis: external or internal? Ann Plast Surg 55: 587-590.
-
Giacomarra V, Russolo M, Arnez ZM, Tirelli G (2001) External osteotomy in rhinoplasty. Laryngoscope 2001 111: 433-438.
-
Rohrich RJ, Krueger JK, Adams WP Jr, Hollier LH Jr (2001) Achieving consistency in the lateral nasal osteotomy during rhinoplasty: an external perforated technique. Plast Reconstr Surg 108: 2122-2130.
-
Ryu JH, Sohn IS, Do SH (2009) Controlled hypotension for middle ear surgery: a comparison between remifentanil and magnesium sulphate. Br J Anaesth 103: 490-495.
-
Tuncel U, Turan A, Bayraktar MA, Erkorkmaz U, Kostakoglu N (2013) Efficacy of dexamethasone with controlled hypotension on intraoperative bleeding, postoperative oedema and ecchymosis in rhinoplasty. J Craniomaxillofac Surg 41: 124-128.
-
Kosucu M, Omür S, Besir A, Uraloğ lu M, Topbas M, et al. (2014) Effects of perioperative remifentanil with controlled hypotension on intraoperative bleeding and postoperative edema and ecchymosis in open rhinoplasty. J Craniofac Surg 25: 471-475.
s